Case Report
Endoscopic Ultrasound - Guided Ethanol Injection for Pancreatic Insulinoma
Rita Yuk-Kwan Cheung, Kai-Pun Wong* and Brian Lang
Department of Surgery, Division of Endocrine Surgery, University of Hong Kong, Queen Mary Hospital, Hong Kong
SAR, China
*Corresponding author: Kai Pun Wong, Department of Surgery, Division of Endocrine Surgery, University of Hong Kong, Queen Mary Hospital, 102 Pokfulam Road, Pokfulam, Hong Kong, China
Published: 11 Aug, 2017
Cite this article as:
Abstract
Pancreatic insulinoma is the most common neuroendocrine tumor of pancreas expressing hormonal manifestation. While majority of insulinoma is benign, complete resection of tumor with enucleation already provided potential cure. Ff tumor is located at head of pancreas and close proximity to main pancreatic or common bile duct, enucleation often lead to pancreatic leakage and morbidity. However, major pancreatectomy including Whipple operation is also major undertaking. Endoscopic ultrasound guided alcohol injection with ablative effect offers an alternative for treatment of pancreatic insulinoma with low morbidity. In this report, we will share our experience and review the current literature on EUS-guided alcohol ablation for pancreatic fistula.
Case Presentation
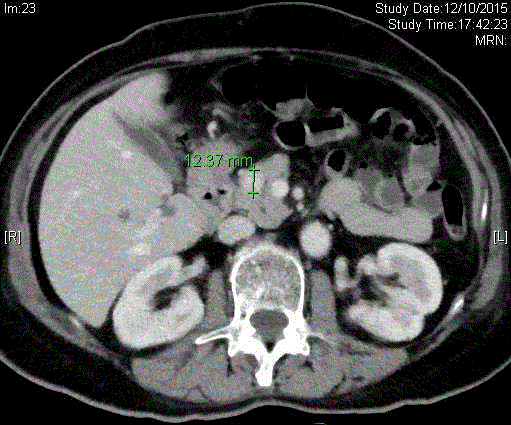
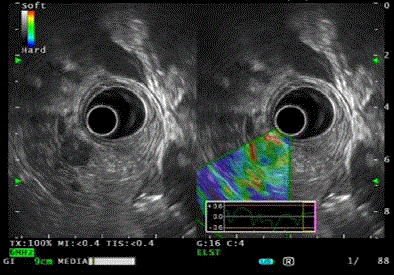
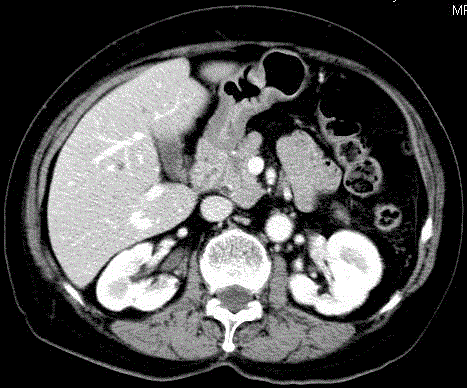
A 75-year old woman was admitted to hospital through causality because of dizziness and syncope. She was found to be hypoglycemic with Histix of 2.7. She had hypertension for 20 years, and follicular thyroid carcinoma with bone metastasis, treated with total thyroidectomy and radioablative iodine 6 months ago. There was no history of diabetes. She was on anti-hypertensive agents and thyroxine replacement. After admission, she was found to have multiple hypoglycemic attacks. Blood tests during her inpatient hypoglycemic attack showed random glucose 2.1 mmol/L, insulin 122 mIU/L (5-10 mIU/L) and C-peptide 3.49 nmol/L (0.27 - 1.27 nmol/L). The results were compatible with endogenous hyperinsulinemia. Diazoxide 50 mg daily per oral was prescribed, with control of hypoglycemic episodes. Contrast computer tomography (CT) of the abdomen revealed a 1.2 cm enhancing pancreatic head nodule (Figure 1). The main differential diagnoses included pancreatic neuroendocrine tumor and hypervascular metastasis from known thyroid cancer. Arterial stimulation with venous sampling (ASVS) was performed: 10% calcium gluconate was injected at common hepatic, gastroduodenal, superior mesenteric and splenic arteries sequentially, and blood was sampled from bilateral hepatic veins after each injection. Serum insulin was elevated when calcium was injected in GDA and thus the pancreatic head lesion was likely insulinoma. Endoscopic ultrasound (EUS) was performed confirming the 1.2 cm × 1 cm circumscribed heterogeneous mass over pancreatic head, with close proximity to common bile duct (CBD) and main pancreatic duct (MPD) although tissue planes were preserved (Figure 2). Both CBD and MPD were not dilated. EUSguided fine needle aspiration cytology (FNAC) was performed. FNAC result later confirmed welldifferentiated neuroendocrine tumour. In view of patient’s age and underlying metastatic thyroid malignancy, pancreatic head insulinoma enucleation with possibility of pancreatodudenectomy (Whipple operation) due to close proximity to CBD and MPD was deemed high risk for her. EUSguided ethanol injection was offered. During the procedure, 1.5 ml 95% ethanol was injected into the lesion under EUS guidance. The procedure was uneventful and well tolerated. Soon after EUS with ethanol injection, diazoxide was stopped and there were no more hypoglycemic episodes. Blood glucose monitoring remained from 5 to 7. She was discharged on day 4. CT scan 4 months after the procedure showed that the previously seen pancreatic head tumour had resolved, with residual hypoenhancement (Figure 3). The patient was latest seen 1 year after ethanol injection and she remains asymptomatic and no hypoglycemic attacks were noted.
Discussion
Insulinoma is one of the most common types of neuroendocrine tumors with hormonal
manifestion. And it is the most common cause of endogenous hyperinsulinemia [1]. More than
95% of insulin is benign [1,2]. Long-term cure with resolution of symptoms are expected after
complete resection. Cytoreduction with maximal resection of tumor is also indicated for symptom and hormonal control in patient with metastasis [2] because of low possibility that malignant insulinoma, enucleation without margin or
regional lymph node dissecteion is feasible to achieve cure. However
if tumor is large, presence of multiple lesions, or close to/involving
pancreatic duct, major resection, i.e. pancreatectomy will be
required. While the extent of pancreatectomy depends on location of
tumor, major pancreatectomy namely Whipple operation, pyloruspreserving
pancreaticoduodenectomy, subtotal pancreatectomy or
distal pancreatectomy carry high morbidity even in high volume
centers being 10% to 43%, respectively [3]. Contemplating a high
morbitidy operation to cure a benign disease is less than satfiactory.
The situation worsens if this operation were undergone in a patient
with medical comorbidity or advance age. A less invasive ablative
procedure could be beneficial.
EUS is one of the most sensitive localization methods for pancreatic
insulinoma, up to 75%, though sensitivity is operator-dependent
[4]. By localizing the insulinoma, EUS-guided ethanol injection
to pancreatic tumor for ablation can be contemplated. It is a new
minimally invasive therapeutic procedure for small neuroendocrine
tumors with accumulating evidence from the literature [5-19] (Table
1). Up till now, 30 patients have undergone EUS-guided ethanol
ablation for pancreatic insulinoma. Majority of the procedure
(14/18) was performed for pancreatic head lesions. While surgical
resection of pancreatic head lesion lead to high risk of complication,
EUS guided minimal invasive interventation offer an option for
treatment for insulinoma. It reflected by the fact that high proportion
of procedures was undergone for pancreatic head lesion. On the other hand, EUS-guided ethanol ablation was mainly performed in
elderly or poor surgical candidates due to comorbidities, patients who
refused operation but refractory to medical treatment, and persistent
lesions after resection or multiple lesions especially associated with
MEN 1. The response of ethanol ablative treatment was determined
by resolution of recurrent hypoglycemic symptoms. Most of the
studies reported no or minimal adverse effects after procedure. Mild
adverse events included transient abdominal pain and self-limiting
fever. More severe complications, including pancreatitis, pancreas
necrosis or duodenal ulcer have been reported. At the moment, there
are no definite selection criteria for pancreatic insulinoma amenable
by EUS ethanol injection. All lesions in the reported cases are less than
2 cm in size, and have to be localized and being accessible by EUS.
On the other hand, there were no guidelines suggesting the dosage of
alcohol or type of injection needle. Occasionally, repeated injections
of ethanol in different sessions are required. In our patient, 22-gauge
needle with 1.5 ml absolute ethanol was only injected once. Some
advocates that injecting a smaller volume of ethanol than estimated
for the tumor volume could prevent procedure-related adverse
events, such as leakage of ethanol and post-procedural pancreatitis.
In addition to procedure-related complications, the major concern of
local ablation therapy is oncological clearance, i.e. failure in complete
ablation or recurrence. In the literature there are no long-term data
regarding recurrence for pancreatic insulinoma or other neuroendocrine
tumor treated with EUS ethanol injection. For insulinoma,
disease response and recurrence could be monitored by presence of
symptoms and imaging which may show hyper-enhancing features
of the ablated lesion. For persistent or recurrence of NET without
signs of distant metastasis, repeated complementary ethanol ablation
therapy could be applied. Surgical resection should be considered
if repeated ethanol ablation failed to cure the condition. However,
most of these patients who optioned for EUS ethanol ablation were
too fragile for major operation and thus conservative treatment and
monitoring were usually offered.
Figure 1
Figure 1
Contrast CT abdomen showing enhancing lesion over pancreatic
head before ethanol injection.
Figure 2
Figure 3
Figure 3
Contrast CT abdomen showing the previously enhancing lesion in
pancreatic head became hypodense after ethanol injection.
Table 1
Table 1
: Summary of case reports/series about EUS-guided ethanol injection for pancreatic insulinoma.
Conclusion
In conclusion, EUS-guided ethanol ablation for insulinoma is a promising options but not yet a standard alternative to surgical resection, with lack of long-term results and technical standardization. However, it is a useful alternative for patients who have small tumor, and are not fit for operation. We postulated that even in insulinoma with metastatic disease, EUS-guided ethanol could be considered for symptoms and hormonal control. For persistent or recurrent disease, repeated sessions of ethanol injection is possible. Although procedure-related adverse events are not common and usually mild, severe complications such as pancreatitis or necrosis could occur and thus careful injection technique and close monitoring after procedure are advocated.
References
- Kittah NE, Vella A. Management of endocrine disease: Pathogenesis and management of hypoglycemia. Eur J Endocrinol. 2017;177(1):R37-R47.
- Doi R. Determinants of surgical resection for pancreatic neuroendocrine tumors. J Hepatobiliary Pancreat Sci. 2015;22(8):610-7.
- Briggs CD, Mann CD, Irving GR, Neal CP, Peterson M, Cameron IC, et al. Systematic review of minimally invasive pancreatic resection. J Gastrointest Surg. 2009;13(6):1129-37.
- Puli SR, Kalva N, Bechtold ML, Pamulaparthy SR, Cashman MD, Estes NC, et al. Diagnostic accuracy of endoscopic ultrasound in pancreatic neuroendocrine tumors: a systematic review and meta analysis. World J Gastroenterol. 2013;19(23):3678-84.
- Paik WH, Seo DW, Dhir V, Wang HP. Safety and Efficacy of EUS-Guided Ethanol Ablation for Treating Small Solid Pancreatic Neoplasm. Medicine (Baltimore). 2016;95(4):e2538.
- Deprez PH, Claessens A, Borbath I, Gigot JF, Maiter D. Successful endoscopic ultrasound-guided ethanol ablation of a sporadic insulinoma. Acta Gastroenterol Belg. 2008;71(3):333-7.
- Schnack C, Hansen CØ, Beck-Nielsen H, Mortensen PM. [Treatment of insulinomas with alcoholic ablation]. Ugeskr Laeger. 2012;174(8):501-2.
- Muscatiello N, Salcuni A, Macarini L, Cignarelli M, Prencipe S, di Maso M, et al. Treatment of a pancreatic endocrine tumor by ethanol injection guided by endoscopic ultrasound. Endoscopy. 2008;40(2):E258-9.
- Levy MJ, Thompson GB, Topazian MD, Callstrom MR, Grant CS, Vella A. US-guided ethanol ablation of insulinomas: a new treatment option. Gastrointest Endosc. 2012;75(1):200-6.
- Jürgensen C, Schuppan D, Neser F, Ernstberger J, Junghans U, Stölzel U. EUS-guided alcohol ablation of an insulinoma. Gastrointest Endosc. 2006;63(7):1059-62.
- Vleggaar FP, Bij de Vaate EA, Valk GD, Leguit RJ, Siersema PD. Endoscopic ultrasound-guided ethanol ablation of a symptomatic sporadic insulinoma. Endoscopy. 2011;43(2):E328-9.
- Lee MJ, Jung CH, Jang JE, Hwang JY, Park DH, Park TS, et al. Successful endoscopic ultrasound-guided ethanol ablation of multiple insulinomas accompanied with multiple endocrine neoplasia type 1. Intern Med J. 2013;43(8):948-50.
- Bor R, Farkas K, Balint A, Molnar T, Nagy F, Valkusz Z, et al. [Endoscopic ultrasound-guided ethanol ablation: an alternative option for the treatment of pancreatic insulinoma]. Orv Hetil. 2014;155(41):1647-51.
- Qin SY, Lu XP, Jiang HX. EUS-guided ethanol ablation of insulinomas: case series and literature review. Medicine (Baltimore). 2014;93(14):e85.
- Yang D, Inabnet WB, 3rd, Sarpel U, DiMaio CJ. EUS-guided ethanol ablation of symptomatic pancreatic insulinomas. Gastrointest Endosc. 2015;82(6):1127.
- Trikudanathan G, Mallery SJ, Amateau SK. Successful Endoscopic Ultrasound-Guided Alcohol Ablation of Sporadic Insulinoma Using Three-Dimensional Targeting (with Video). Clin Endosc. 2016;49(4):399-401.
- de Sousa Lages A, Paiva I, Oliveira P, Portela F, Carrilho F. Endoscopic ultrasound-guided ethanol ablation therapy for pancreatic insulinoma: an unusual strategy. Endocrinol Diabetes Metab Case Rep. 2017;2017.
- Mittal M, Yip B, Lee JG. Endoscopic Ultrasound-Guided Ethanol Ablation for Control of Local-Regional Metastatic Insulinoma. Pancreas. 2017;46(3):e17-e8.
- Luo Y, Li J, Yang A, Yang H, Li F. 68Ga-Exendin-4 PET/CT in Evaluation of Endoscopic Ultrasound-Guided Ethanol Ablation of an Insulinoma. Clin Nucl Med. 2017;42(4):310-311.