Case Report
Amyloıdosıs in Colon Presentıng wıth Rectal Bleedıng in Multıpl Myeloma: A Case Report
Vedat Goral1*, Ragip Ortac2 and Nevin Yılmaz3
1Department of Gastroenterology, Istanbul Medipol University School of Medicine, Istanbul, Turkey
2Department of Pathology, Izmir Medicalpark Hospital, Izmir, Turkey
3Department of Gastroenterology, Mugla Sitki Kocman University School of Medicine, Mugla, Turkey
*Corresponding author: Vedat Goral, Department of Gastroenterology, Istanbul Medipol University School of Medicine, Istanbul, Turkey
Published: 07 Aug, 2017
Cite this article as: Goral V, Ortac R, Yılmaz N.
Amyloıdosıs in Colon Presentıng wıth
Rectal Bleedıng in Multıpl Myeloma: A
Case Report. Clin Surg. 2017; 2: 1581.
Abstract
Multiple myeloma (MM) is a malignant proliferation of plasma cells that secrete monoclonal
immunglobin (M protein). It accounts for 1% of all cancers and 10% of hematological malignancies.
Mean age at diagnosis is 66 years. The most common findings are bone pain, pathological fractures,
anemia, bone marrow failure, Infections triggered by neutropenia and immunodeficiency, and
kidney failure and rarely can cause acute hypercalcaemia, symptomatic hyperviscosity, neuropathy,
amyloidosis and coagulopathy. Amyloidosis is a rare disease characterized by nonspecific symptoms
and signs. It can be seen anywhere in the gastrointestinal tract. In this case, a colonoscopy was
performed on the patient who was directed to gastroenterology clinic with rectal bleeding and
amyloidosis was detected in the biopsy from tumoral lesions seen in the colonoscopy.
Keywords: Multipl myeloma; Amyloidosis; Rectal bleeding
Introduction
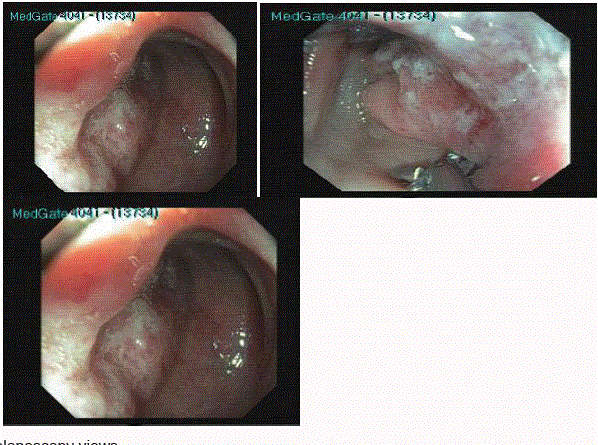
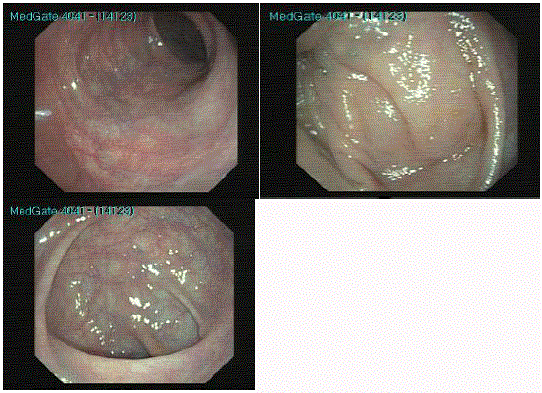
A 76-year-old female patient with multiple myeloma was directed to gastroenterology with rectal bleeding while hospitalized with acute renal failure and hypercalcemia. The patient underwent colonoscopy. and lumen-narrowing, vegetan, erosional, moderately hard, pseudotumor-like, mucopleural lesions were detected at approximately between 50 cm - 60 cm on colonoscopy. There was partial narrowing and pseudotumor in the colon. Six different biopsies were taken from different places on lesions. Homogenous, amorphous material accumulation in the submucosa and around the veins were detected in the biopsy specimens stained with hematoxylin and eosin dye and Congo red. Colonoscopic images are shown in Figure 1, and images of pathological specimens are shown in Figure 2a and 2b. The patient underwent a second colonoscopy 1 month later for control. The lesions detected in the first colonoscopy were not found (Figure 3). On the second colonoscopy, biopsy was taken again from the rectosigmoid region, but it has been observed that the amyloidosis continues in biopsy.
Figure 1
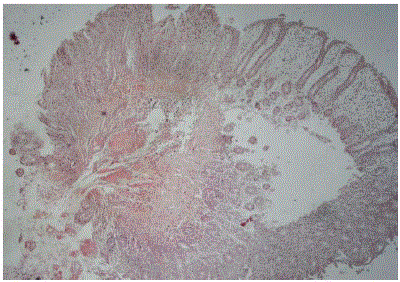
Figure 2a
Figure 2a
Congo red positive amyloid deposits on submucosal vessel walls
in colon biopsy (x40; Congo red, photo 7394).
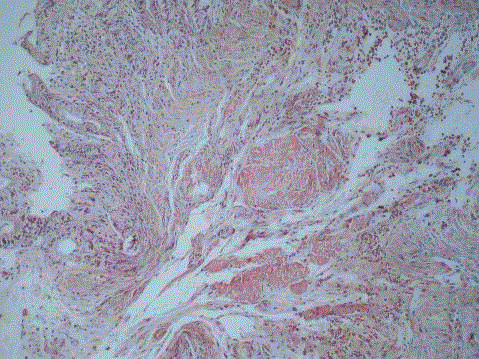
Figure 2b
Figure 2b
Thickening of the walls of the submucosa due to congo redpositive
amyloid deposits (x100; Congo red, photo 7396).
Figure 3
Discussion
Multiple myeloma (MM) is a malignant proliferation of plasma
cells that secrete monoclonal immunglobin (M protein) [1-5]. It
accounts for 1% of all cancers and 10% of hematological malignancies.
Mean age at diagnosis is 66 years. Radiation, genetics such as t (11;
14), t (14; 18), t (8; 14), 13q deletion, familial predisposition, IL-6
and IL1-β are implicated in etiology. The disease is characterized
by lytic lesions in the bones, (humoral) immunodeficiency, renal,
and neurological symptoms. In addition to the clinical features of
myeloma; anemia and roll formation, serum M protein concentration
>3g/dl, elevation of sedimentation rate, >30% plasma cell in bone
marrow, and immunophenotype such as (+) staining with CD38,
CD56, and CD138 were also detected. As clinically heterogeneous
disease, MM can be classified into two types, usually untreated, silent
myeloma (SMM) and MM (active) requiring treatment. The diagnostic
criteria for MM were revised in 2014 by the International Myeloma
Working Group (IMWG)[2,4]. The most common findings are bone
pain, pathological fractures, anemia, bone marrow failure, Infections
triggered by neutropenia and immunodeficiency, and kidney
failure and rarely can cause acute hypercalcaemia, symptomatic
hyperviscosity, neuropathy, amyloidosis and coagulopathy.
In amyloidosis, amyloid, the abnormal protein, is deposited in the
tissues as an extracellular deposit [6-9]. Amyloid deposits are found
in the vascular veins and in the intestinal system in the mucosa,
submucosa, muscularis mucosa layer [10-12]. Similar amyloid
deposits were present in our case. Amyloid deposits in the intestines
are seen as pseudotumor or ulceration. Amyloid protein accumulates
irreversibly in the colon. However, in some publications it is reported
that amyloid deposition can be reversible with chemotherapy
treatment, especially with melphalan and steroid therapy, in the
early stages [13-15]. AL amyloidosis is characterized by plasma cell
dyscrasia and monoclonal light chain in in serum and/or urine; and
this type of amyloidosis largely seen in the gastrointestinal system. AL
amyloidosis is characterized by multiple myelomas in 15% of the cases.
It is a rare disease characterized by nonspecific symptoms and signs.
It can be seen anywhere in the gastrointestinal tract. Amyloidosis
can mimic other diseases of the gastrointestinal tract, such as
inflammatory bowel diseases, ischemic colitis, collagenous colitis,
and malignancies. Due to non-specific symptoms, diagnosis can
easily be missed in patients who have not been diagnosed previously
with amyloidosis or a related disease. The prognosis of MM involving
the GI tract is unfavorable. Stomach and duodenal involvement is
rare, and asymptomatic, or can cause nausea, vomiting, pain and
sometimes hematemesis. Diarrhea, protein loosing enteropathy,
ulcers, masses, gastric ulcer, hypotonia and dilatation may be
present in small bowel involvement. The endoscopic detection of a
submucosal petechial hematomas and polypoid lesions in the setting
of gastrointestinal bleeding should raise suspicion of the disease.
Rarely, colonic amyloidosis can be the first sign of multiple myeloma
[7,11,12,16]. Sometimes it can also cause upper gastrointestinal
bleeding in cases of jejunal involvement [17]. The development of
amyloidosis in multiple myeloma negatively affects the disease and
shortens the survival. Amyloid is most commonly located in the
sigmoid colon and rectosigmoid region in the gastrointestinal tract.
There is rectal bleeding in 25% - 45% of cases, caused by ischemia,
infarction, or ulceration in cases with amyloidosis involvement in
the colon, Amyloid involvement in the colon and gastrointestinal
bleeding linked to multiple myeloma cases have been reported in
the literature. In our case, the case of amyloidosis in the colon with
rectal bleeding is very rare. The disease treatment and supportive
care were applied to the patient; surgical intervention or endoscopic
intervention (such as APC, selective micro-coil remobilization
therapy, or injection therapy) were not done. It was seen that the
lesions completely disappeared in the control colonoscopy 1 month
after. This case demonstrates that although it is rare, amyloidosis can
be seen in colon in patients with multiple myeloma and this patients
can be presented with rectal bleeding.
References
- Kazandjian D. Multiple myeloma epidemiology and survival: A unique malignancy. Semin Oncol. 2016;43(6):676-681.
- Pratt G, Morris TC. Review of the NICE guidelines for multiple myeloma. Int J Lab Hematol. 2017;39(1):3-13.
- Smith D, Yong K. Advances in understanding prognosis in myeloma. Br J Haematol. 2016;175(3):367-380.
- Fonseca R, Monge J, Dimopoulos MA. Staging and prognostication of multiple myeloma. Expert Rev Hematol. 2014;7(1):21-31.
- Fonseca R, Monge J. Myeloma: classification and risk assessment. Semin Oncol. 2013;40(5):554-66.
- Ebert EC, Nagar M. Gastrointestinal manifestations of amyloidosis. Am J Gastroenterol. 2008;103(3):776-87.
- Hurlston DP. Iron-deficiency anemia complicating AL amyloidosis with recurrent small bowel pseudo-obstruction and hindgut sparing. J Gastroenterol Hepatol. 2002;17(5):623-4.
- Matsui H, Kato T, Inoue G, Onjie E. Amyloidosis localized in the sigmoid colon. J Gastroenterol. 1996;31(4):4607-11.
- Harada K, Ichikawa D, Konishi H, Komatsu S, Atsuhi S, Hitoshi F, et al. Perforation of the sigmoid colon and massive ischemia of the small intestine caused by amyloidosis associated with multiple myeloma: a case report. Int Surg. 2014;99(6):685-90.
- Garay M, Bollo J, Balague C, Targarona E, Trias M. Gastrointestinal bleeding as a first symptom of a focal jejunal amyloidosis. Cir Esp. 2014;92(10):696-8.
- Kon T, Nakagawa N, Yoshikawa F, Haba K, Kitagawa N, Michihiro I, et al. Systemic immunoglobulin light-chain amyloidosis presenting hematochezia as the initial symptom. Clin J Gastroenterol. 2016;9(4):243-51.
- Maza I, Vlodavsky E, Eliakim RA. Rectal bleeding as a presenting symptom of AL amyloidosis and multiple myeloma. World J Gastrointest Endosc. 2010;2(1):44-6.
- Lim AY, Lee Jh, Jung KS, Gwag HB, Kim DH, Kim SJ, et al. Clinical features and outcomes of systemic amyloidosis with gastrointestinal involvement: a single-center experience. Korean J Intern Med. 2015:30(4);496-505.
- Oqasawara N, Kitagawa W, Obayashi K, Itoh Y, Noda H, Funaki Y, et al. Solitary amyloidosis of the sigmoid colon featuring submucosal tumor caused hematochezia. Intern Med. 2013;52(22):2523-7.
- Audemard A, Lepennec V, Riffaut N, Ficheux M, Macro M, Galateau-Salle F. Pseudo-tumoral intestinal amyloidosis. QJM. 2013;106(12):1139.
- Kwon YH, Kim JY, Kim JH, Park HW, Yang HM, Jeon SW, et al. [A case of primary colon amyloidosis presenting as hematochezia]. Korean J Gastroenterol. 2012;59(1):44-7.
- Yau AH, Cornell IS, Cheung J. Jejunal amyloidosis: a rare cause of severe gastrointestinal bleeding. Can J Gastroenterol. 2012;26(6):320-1.