Research Article
Positive Predictive Value of Biopsy of Palpable Masses Following Mastectomy
Brennan SB*, D’Alessio D, Kaplan J, Edelweiss M, Heerdt A and Morris E
Department of Breast Imaging, Memorial Sloan Kettering Cancer Center, NY 10604, USA
*Corresponding author: Sandra Brennan, Department of Breast Imaging, Memorial Sloan Kettering Cancer Center, 500 Westchester Ave, West Harrison, NY 10604, USA
Published: 07 Aug, 2017
Cite this article as: Brennan SB, D’Alessio D, Kaplan
J, Edelweiss M, Heerdt A, Morris E.
Positive Predictive Value of Biopsy
of Palpable Masses Following
Mastectomy. Clin Surg. 2017; 2: 1580.
Abstract
Objective: Determine the positive predictive value (PPV) of biopsy of palpable masses following
mastectomy (MX). Determine if there are patient characteristics, tumor or imaging features more
predictive of cancer.
Materials and Methods: IRB-approved retrospective review of 16396 breast ultrasounds June 2008
- December 2015 identified patients with MX presenting with palpable masses. Medical records
and imaging studies were reviewed. Statistical analysis was performed with Fisher’s exact test. 95%
confidence intervals (CI) were calculated.
Results: 117 patients presented with palpable masses on the MX side. 101/117 patients who had a
palpable mass on physical examination had a true sonographic mass to correlate with the clinical
findings. 91/101 (90%) underwent biopsy: 19/91 (21%, 95% CI; 13-31) biopsies were malignant.
72/91 (79%) were benign. All 19 cancers were on the original cancer side. Recurrences ranged from
0.4 to 4.5 cm maximum diameter, mean 1.3 cm.
Prophylactic versus therapeutic mastectomy was very statistically significant (p=0.01). The use of
tamoxifen or an AI was also statistically significant (p=0.04) Patient age (p=1.0), radiation therapy
(p=1.05), chemotherapy (p=0.2) immediate breast reconstruction (p=0.2) or implant versus flap
(p=0.2) had a statistically significant association with finding cancer on biopsy.
Lesion shape (irregular versus oval/round) was highly statistically significant (p=0.0003) as was nonparallel
orientation on ultrasound (p=0.008). Circumscribed versus non-circumscribed margins
was also statistically significant (p=0.008).
Conclusion: The PPV of biopsy of palpable masses on the side of MX was 21% (95% CI; 13-31). All
recurrences were on the original cancer side and this was very statistically significant.
Keywords: Breast; Mastectomy; Biopsy; Fine-Needle; Cytology; Recurrence
Introduction
Over the past decade, several single-institution studies [1,2] and population-based studies [3,4]
have documented an increase in mastectomy rates in the United States. In conjunction with this
general rise, it has been noted that the rates of bilateral mastectomies—particularly contralateral
prophylactic mastectomies—have also increased [5-7].
In women who undergo breast conserving surgery instead of mastectomy, mammography
has a well-defined role in surveillance of women after breast conserving surgery [8-10]. Even
though mammographic interpretation of the post-treated breast may be challenging, there are
well-described patterns of recurrence such as increased density, architectural distortion or micro
calcifications [11-14]. The accuracy of mammography in detecting recurrence is also improved by
comparing the pre-treated breast to the post-treated breast and understanding the normal postoperative
appearance. However, in women who undergo mastectomy, routine surveillance of the
mastectomy side with mammography remains controversial. Some centers still routinely image
these patients [15] while others feel the yield of finding recurrent cancer in asymptomatic patients is
too low and clinical examination alone in the asymptomatic patient is more beneficial [16]. At our
institution, we do not perform routine mammographic surveillance of the mastectomy side but rely
on clinical breast examination and then image these patients accordingly based on physical findings
such as palpable masses, skin thickening or retraction.
We conducted this study to determine the positive predictive value (PPV) of biopsy of palpable masses on the mastectomy side and to determine if there are patient,
tumor or morphologic imaging features predictive of cancer. As
this is the first study to date looking at the PPV of biopsy following
mastectomy, it has the further potential to help guide radiologists
in the management of palpable masses following mastectomy. We
describe the classic imaging appearance of common benign palpable
masses following mastectomy and reconstruction.
Material and Methods
Following IRB approval, we performed a HIPAA-compliant
retrospective review of 16396 consecutive diagnostic breast
ultrasounds performed at our institution, a tertiary care cancer
hospital, from June 2008 to December 2015. The need for informed
consent was waived. Patients who presented for ultrasound because
of a palpable mass on physical examination of the mastectomy side
were identified and included in our study. The physical examination
was performed by either the surgeon or breast oncologist who then
referred the patient for ultrasound. Our cohort of patients included
women who initially palpated a lump themselves which was then
confirmed by their doctor or the lump was felt on clinical examination
by the surgeon, medical oncologist or survivorship NP. The patients
were then referred to radiology for imaging. We included patients
with reconstructed and non-reconstructed breasts. Patients who had
prophylactic mastectomy after breast cancer was diagnosed in the
contralateral breast were also included.
The medical records and all imaging studies for the patients
included in the study were reviewed by SB with 11 years experience.
All patients had ultrasound performed (Acuson S2000, Siemens)
with a linear probe and frequency range of 9-16MHz. Additional
mammographic views were performed as needed at the discretion
of the radiologist interpreting the study at the time of presentation.
Some patients were also referred for MRI. The age of the patient,
menopausal status and BRCA status if known were recorded. The side
of the palpable lesion and whether the mastectomy was therapeutic
or prophylactic were noted. A note was also made of whether the
patient had nipple sparing or skin sparing mastectomy, immediate
breast reconstruction or none and whether they had an implant or
autologous flap reconstruction. The histology of the primary tumor
including grade and hormone receptor status was recorded and
adjuvant therapy with chemotherapy, radiation therapy or hormonal
therapy was also noted.
On ultrasound examinations, all palpable lesions that had
a sonographic correlate considered a true mass had size, shape
(round, oval, irregular), margins (indistinct, angular, circumscribed,
spiculated, micro-lobulated), presence of shadowing and orientation
(parallel, anti-parallel) on sonography documented. Based on the
BI-RADS lexicon 5th edition for ultrasound, indistinct, angular,
micro-lobulated and spiculated were considered non-circumscribed.
Palpable masses that were considered not to be true masses
included surgical clips, implant fold, implant valve and dystrophic
calcifications. These patients did not undergo biopsy and were not
included in analysis.
If biopsy was performed of the palpable lesion then histology
was recorded and if no biopsy was performed then follow-up if any
was noted. Percutaneous biopsy, FNA or core, was done by a breast
Radiologist under ultrasound guidance. No cytopathologist or
cytotechnologist was available on site for immediate assessment of
adequacy at the time of FNA. The FNA passes were immediately rinsed
in CytoLyt® solution by the radiologist and transported to pathology
for slide preparation where they were then evaluated for adequacy
and diagnosis at a later time. Statistical analysis was performed with
Fisher’s exact test. 95% confidence intervals (CI) were calculated. A p
value < 0.05 was considered statistically significant.
Results
Patients
Patients of 117 are presented for targeted ultrasound of palpable
masses on the side of a mastectomy (MX). These patients ranged in age
from 25-82 years with a mean of 52 years. Patients of 101/117 who had
a palpable mass on physical examination had a true sonographic mass
to correlate with the clinical findings. The 16/117 had no sonographic
mass and the palpable lesion was found to be related to the implant
itself in 7 with the patient feeling the implant valve (Figure 1), folds
(Figure 2) or implant edge. Four patients were feeling a surgical clip,
calcification (Figure 3) or suture material, and one patient was feeling
her rib. These patients did not undergo biopsy. Four patients had a
palpable mass on clinical examination and no sonographic correlate
to account for the physical findings. The 91/101 (90%) patients
with a palpable sonographic mass ultimately underwent biopsy of
the mass. 78/91 patients had fine needle aspirations (FNA), 8/91
had core biopsies and 5/91 had surgical biopsies. The 66/78 (85%)
patients had FNAs which were deemed diagnostic or satisfactory for
evaluation and 12/77 (15%) patients had FNAs which were deemed
non-diagnostic or acellular. The 5 out of these 12 cases had either
a follow up core biopsy, FNA or excision with benign results. 5/12
of these lesions resolved with the FNA and could no longer be seen
on subsequent imaging. Only 2 out of the 12 lesions deemed nondiagnostic/
acellular were unchanged after FNA and had no follow
up surgical procedure. Specifically, these 2 lesions had an initial low
suspicion on imaging and no imaging change or recurrence after a follow up of 52 and 31 months. The 10/101 (10%) patients did not
undergo biopsy and had follow-up imaging (range of follow-up was
6-83, with a mean of 34 months) with no cancer found on follow-up.
The 19/91 (PPV: 21%, 95% CI; 13-31) of those who underwent biopsy
had cancer (age 35-68, mean 48 years) and 72/91 (79%) were benign.
15/19 cancers were diagnosed by FNA and 4/19 by core biopsy. All
19 cancers were on the original cancer side not the prophylactic
contralateral MX side (p=0.01). The range of follow-up for patients
with a benign biopsy result was 19-77 months, mean 45 months,
with no cancer found on follow-up. 20/91 (22%) patients underwent
biopsy of a lesion on the prophylactic mastectomy side and these
were all benign. So 19/71 (PPV: 27%, 95% CI; 17-39) who underwent
biopsy of a palpable mass on the side of a therapeutic mastectomy had
cancer. Cancer recurrences ranged from 0.4 to 4.5 cm in maximum
diameter mean 1.3 cm.
No cancer was found on the prophylactic mastectomy side and
this was very statistically significant (p=0.01). Recurrences was more
likely in patients who did not receive anti-estrogen therapy and this
was statistically significant (p=0.04). Neither patient age < 50 years
versus ≥50 years (p=1.0), chemotherapy (p=0.2), or radiation therapy
(p=1.0) had a statistically significant association with finding cancer on
biopsy. The 106/117 (91%) patients had reconstruction. The 103/117
(88%) patients had immediate breast reconstruction (IBR), three had
delayed reconstruction and eleven patients declined reconstruction.
The 90/106 (85%) had implant reconstructions and 16/106 (15%) had
autologous flap reconstruction. Only 9 patients had nipple sparing
mastectomies and 107/117 (91%) had skin sparing mastectomies.
The surgical technique and timing of reconstructive surgery had
no statistical significance on cancer recurrence [Immediate breast
reconstruction (p=0.2), nipple sparing mastectomy (p=0.7. Of the
patients with cancer recurrences, 6/19 (32%) had received prior
radiation, 12/19 (63%) hormonal therapy with anti-estrogens and
15/19 (79%) chemotherapy. The 18/19 recurrences were in patients
with implant reconstructions (p=0.2 for implant versus flap only
and p=0.3 reconstructed versus not reconstructed breasts). Patient
characteristics in cancer and benign patients who underwent biopsy
are shown in Table 1.
The 101/117 patients who had a palpable mass on physical
examination had a true sonographic mass to correlate with the clinical
findings. The 16/117 had no sonographic mass and the palpable lesion
was found to be related to the implant itself in 7 with the patient
feeling the implant valve (Figure 1), folds (Figure 2) or implant edge.
Four patients were feeling a surgical clip, calcification (Figure 3) or
suture material, and one patient was feeling her rib. These patients
did not undergo biopsy. Four patients had a palpable mass on clinical
examination and no sonographic correlate to account for the physical
findings. Only 8/117 patients had mammography in the evaluation of
the palpable mass. This included routine MLO, CC views and a cone
compression view in some cases. In one patient the mammogram
showed that the palpable mass was a dystrophic calcification, 2
patients demonstrated an oil cyst/fat necrosis, one patient a mass or
density which was ultimately benign. The remainder had no findings
on mammography. Only 16 patients had MRI performed and 7
patients had mammographic views performed.
On ultrasound, lesion shape (irregular versus oval/round)
was highly statistically significant (p=0.0003) as was non-parallel
orientation on ultrasound (p=0.008). Circumscribed versus notcircumscribed
margins was also statistically significant (p=0.008).
Lesion size and presence of shadowing were not statistically significant (p=1.0). Imaging features on ultrasound in cancer and
benign patients who underwent biopsy are shown in Table 2.
Genetic status was unknown for many patients (48/117, 41%).
The 10 patients were BRCA 1 positive, 7 were BRCA 2 positive and
one patient had a CHEK 2 mutation. 51 patients tested negative for
a genetic mutation. Two patients who were BRCA 2 positive had a
recurrence, 9 recurrences were in the tested negative patients and 8
were in the unknown group. The majority of the original primary
cancers were invasive ductal carcinomas (88/117, 75%). Twelve
patients had prior invasive lobular carcinoma, 11 DCIS, 4 DCIS
with microinvasion, 2 had no primary and had undergone bilateral
prophylactic mastectomies. The 86/117 (74%) of the original primary
tumors were ER positive, 21/117 (18%) were ER negative. The 72/117 (62%) were PR positive and 35/117(30%) were PR negative. The
21/117(18%) were HER-2 positive and 86/117 (74%) were HER-2
negative. In total, 16 patients had Triple Negative primary cancers
and 2 of these patients developed a recurrence (p=1.0). Having an
ER negative primary cancer had no statistical significance (p=0.7)
because most of the recurrences were in ER positive patients and the
majority of patients were ER positive. The remainders are unknown
or not available. The histology, grade and hormone receptor profiles
of the original primaries in the patients who developed recurrences
are listed in Table 3. The 16/19 (84%) of the patients who developed
a recurrence originally had an invasive ductal carcinoma, 2 patients
had microinvasive DCIS and one DCIS.
Figure 1
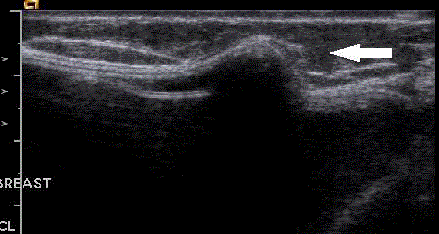
Figure 2
Figure 2
Sonogram of an intact implant with fold or bulge (arrow) which was
felt by the patient as a mass.
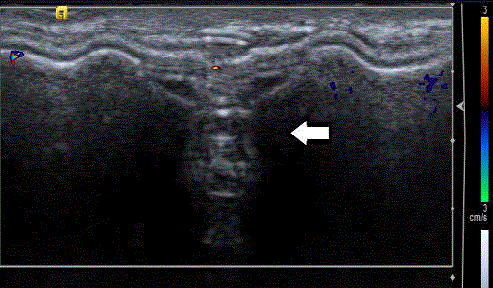
Figure 3
Figure 3
Patient status post-mastectomy with implant reconstruction.
Palpable mass which on ultrasound (Figure 3a) was anechoic with no
vascularity and dense posterior shadowing (arrow). Cone mammographic
view (Figure 3b) confirmed this was a calcification.
Table 1
Table 1
Patient characteristics in cancer and benign patients who underwent
biopsy of palpable masses on the side of a mastectomy.
Table 2
Table 2
Imaging features on ultrasound in cancer and benign patients who
underwent targeted ultrasound of palpable masses on the side of a mastectomy.
Table 3
Table 3
Histology, grade and hormone receptor profiles of the original primaries in 19 patients who developed recurrences.
Discussion
Despite advances in surgical technique, radiotherapy and chemotherapy, locoregional recurrences after mastectomy are still a concern. The rate of local recurrence following mastectomy is reported to be between 5% and 27% [16-18]. Despite this, routine surveillance of the mastectomy side with mammographic screening is not advocated as most recurrences are clinically evident. Fajardo found that mammographic imaging of the mastectomy site did not increase the detection of locally recurrent breast cancer and found mammography to be useful in only 2/20 patients. At our institution, routine surveillance mammography for patients with breast cancer treated with mastectomy is only done on the contralateral intact breast. We rely on physical examination for asymptomatic mastectomy patients and refer those with suspicious clinical findings for imaging. As mastectomy rates are rising, it is likely to expect more of these patients presenting for imaging. Local recurrence after mastectomy has a negative impact on survival so the threshold to biopsy mastectomy patients is low. In the work-up of mastectomy patients with palpable masses ultrasound is the imaging test of choice. In some cases however mammography may be helpful to confirm the palpable is an oil cyst, dystrophic calcification or part of the implant itself for example the implant valve. In an effort to better select patients for biopsy and know what our positive predictive value of biopsy is in this patient cohort, we reviewed the data at out institution. Studies to date looking at the supplemental benefit of screening breast ultrasound show higher PPV of biopsy if lesions are characterized and classified correctly [19-22]. And while certain lesion characteristics such as irregular lesion shape, non-parallel orientation and noncircumscribed margins were more likely to be malignant (Figure 4) we found some overlap in sonographic features between benign and malignant lesions in our patient population. Some biopsy-proven recurrences had benign imaging features. In keeping with the literature and the variable appearance of fat necrosis, some had classic imaging appearance (Figure 5) while others were more indeterminate (Figure 6). Also, one of the biopsy-proven cases of recurrence appeared echogenic on ultrasound a feature we associate often with fat necrosis. Yoo et al. evaluated local recurrence of breast cancer in reconstructed breasts using TRAM flaps and similarly found that imaging findings may mimic benign lesions and advised caution and pathological confirmation even in benign-appearing lesions [23]. Our data shows significant P values for lesion characteristics in keeping with the BI RADS lexicon in so far as lesions with irregular shape, not-circumscribed margins and anti-parallel orientation on ultrasound were more likely to be malignant. Biopsy of lesions with any or all of these morphologic descriptors is advised. We also found a very significant P value for prophylactic mastectomy versus not. No cancers were found on the prophylactic mastectomy side. In the setting of a mass with benign morphologic features on the prophylactic mastectomy side we suggest short term follow up rather than biopsy in conjunction with clinical follow up. In all women, palpable findings with or without imaging correlates should be managed clinically with perhaps a higher level of suspicion in patients who have undergone mastectomy for cancer rather than a prophylactic mastectomy. While the BI-RADS lexicon provides guidance for characterizing the morphologic features of a mass and the associated risk of malignancy, our results show that caution should be taken in evaluating palpable lesions in patients who have undergone mastectomy for breast cancer. In these patients, the palpable finding may be so small that accurate assessment of morphologic imaging features may be precluded. With regards to palpable findings, lesions that may typically be considered to have predominately benign imaging characteristics according to BI-RADS must be considered in the context of the patient's history including symptoms, risk for primary or recurrent breast cancer, prior cancer histology and prior adjuvant therapy. We felt it was important to include prophylactic mastectomy patients because they may also present with a palpable mass and there is little if no data in the literature on the work-up and management of these lesions. Our data showed a very significant P value when the palpable lesion was on the prophylactic mastectomy side and all of the masses biopsied on the prophylactic mastectomy side were benign. So assuming the morphologic features of the palpable lesion imply benignity and the clinical suspicion is low we suggest short term imaging and clinical follow up of these patients. The majority of the reconstructions were with implants so with little numbers of autologous implants we cannot comment on significance. However the work-up of patients with a palpable mass in an autologous reconstruction is the same as for a palpable mass in any patient. With the exception that Mammography may be more helpful to assess for calcifications and MRI to better characterize fat necrosis. Some institutions perform screening mammography on autologous reconstructions. In the absence of data to support routine screening mammography in these patients at our institution we rely on clinical examination in the routine follow up of these patients. This study shows the specific issue of FNA yielding a non-diagnostic or acellular specimen after MX. The majority of the lesions biopsied were sampled with FNA technique. These lesions are often small and after mastectomy there may be only skin and underlying chest wall or implant making core biopsy difficult. For the same reasons, the yield from FNA is sometimes low with sparse cells present and samples sometimes deemed acellular or non-diagnostic by the cytopathologist. The 12/77 (15%) of our FNAs were deemed non-diagnostic. For these cases we perform careful radiologic correlation and based on our level of suspicion determine if there is a need for surgical biopsy or if these lesions are safe to follow. The 4/12 resolved with the FNA, one lesion was half the original size post aspiration and 3/12 were unchanged after FNA. One patient subsequently had a core biopsy which was benign and one had a surgical excision also benign. None of the lesions which were called non-diagnostic on FNA proved to be malignant on follow-up (range of follow-up was 6-58 months, mean 29 months). An adequate specimen obtained by FNA is one that leads to resolution of a problem presented by a lesion in a particular patient’s breast. There is no specific requirement or national standard for minimum number of ductal cells to be present for specimen adequacy. Therefore, adequacy is determined by the opinion of the aspirator that the cytologic findings based on the report are consistent with the clinical-radiological impression and that the lesion was adequately sampled, and the opinion of the pathologist examining the smears that the described cytologic findings are concordant and slides do not have significant distortion or artifacts, and can be interpreted [24, 25]. While we did not review our overall total rate of reconstructive surgery after mastectomy at our institution, our numbers are in keeping with current trends. Most (88%) of the patients in the group had immediate breast reconstruction (IBR) and most (85%) were with implants [26,27]. IBR has been shown to be safe and not associated with an increased risk of local recurrence [28] and while all recurrences in our group had IBR this was not statistically significant (p=0.2) as most of the patients in the group had IBR. Similarly, reconstruction versus no reconstruction (p=0.3) or the type of reconstruction (implant versus flap) were not significantly associated with recurrence (p=0.2). While our study did have some limitations, in that it was retrospective and not all patients underwent biopsy, it is the first study to date looking at the positive predictive value of biopsy following mastectomy. It is also the only study to address the specific issue of FNA yielding a non-diagnostic or acellular specimen after MX. In conclusion, the positive predictive value of biopsy in mastectomy patients for palpable masses is high, reaching 21% in this study. An irregular shape, non-parallel orientation on sonography and not-circumscribed margins had a statistically significant association with finding cancer. All cancers in our study were on the original cancer side and this was statistically significant (p=0.01). Since we did have some overlap with benign sonographic features in lesions that were malignant, we cannot suggest using only BI-RADS descriptors to avoid biopsy. Since recurrence after mastectomy may mimic benign lesions pathologic confirmation is advised. However if we had spared the 20 patients who underwent biopsy on the prophylactic mastectomy side our PPV would have increased slightly to 27% (19/71). Therefore we suggest that lesions with benign sonographic features and low clinical suspicion on the prophylactic mastectomy side could undergo short-interval follow-up rather than biopsy. However, these numbers were small and future studies are needed.
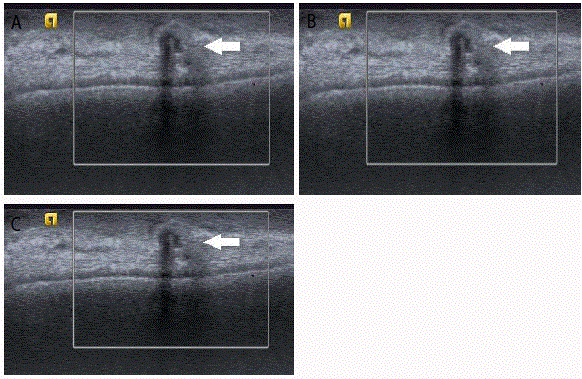
Figure 4
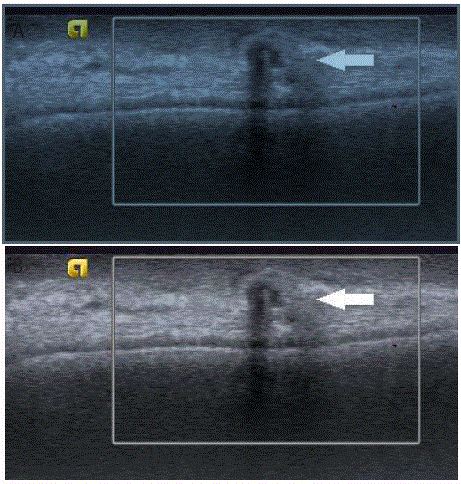
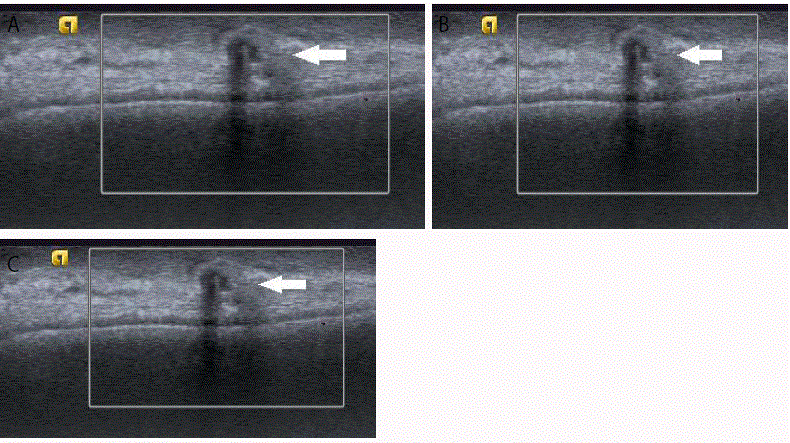
Figure 4
Palpable masses (Figure 4a-4c) in patient’s status post-mastectomy, all with irregular shape and vertical orientation and yielding recurrent invasive ductal
carcinoma on biopsy.
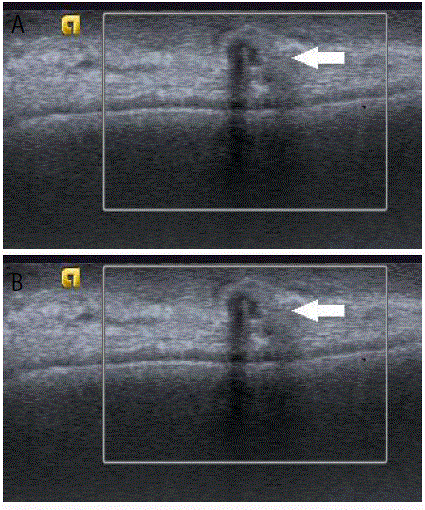
Figure 5
Figure 5
Patient status post-mastectomy with TRAM flap reconstruction and a palpable mass in the reconstructed left breast. On ultrasound (Figure 5a) it
appeared as an oval parallel isoechoic mass with central anechoic component (arrow). Cone mammographic (Figure 5b) view over the palpable mass shows an
area of increased density and central fat (arrow) consistent with fat necrosis.
Figure 5
Figure 6
Patient status post right mastectomy with TRAM flap reconstruction and palpable mass in the medial right breast. On ultrasound (Figure 6a) it was oval,
parallel and is to hyperechoic with no vascularity (arrow). MRI (Figure 6b and 6c) show a heterogeneously enhancing mass in the medial reconstructed breast.
References
- McGuire KP, Santillan AA, Kaur P, Meade T, Parbhoo J, Mathias M, et al. Are mastectomies on the rise? A 13-year trend analysis of the selection of mastectomy versus breast conservation therapy in 5865 patients. Ann Surg Oncol. 2009;16(10):2682-90.
- Katipamula R, Degnim AC, Hoskin T, Boughey JC, Loprinzi C, Grant CS, et al. Trends in mastectomy rates at the Mayo Clinic Rochester: effect of surgical year and preoperative magnetic resonance imaging. J Clin Oncol. 2009;27(25):4082-8.
- Mahmood U, Hanlon AL, Koshy M, Buras R, Chumsri S, Tkaczuk KH, et al. Increasing national mastectomy rates for the treatment of early stage breast cancer. Ann Surg Oncol. 2013;20(5):1436-43.
- Habermann EB, Abbott A, Parsons HM, Virnig BA, Al-Refaie WB, Tuttle TM. Are mastectomy rates really increasing in the United States? J Clin Oncol. 2010;28(21):3437-41.
- Veronesi U, Cascinelli N, Mariani L, Greco M, Saccozzi R, Luini A, et al. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med. 2002;347(16):1227-32.
- Tuttle TM, Habermann EB, Grund EH, Morris TJ, Virnig BA. Increasing use of contralateral prophylactic mastectomy for breast cancer patients: a trend toward more aggressive surgical treatment. J Clin Oncol. 2007;25(33):5203-9.
- Tuttle TM, Jarosek S, Habermann EB, Arrington A, Abraham A, Morris TJ, et al. Increasing rates of contralateral prophylactic mastectomy among patients with ductal carcinoma in situ. J Clin Oncol. 2009;27(9):1362-7.
- Orel SG, Troupin RH, Patterson EA, Fowble BL. Breast cancer recurrence after lumpectomy and irradiation: role of mammography in detection. Radiology. 1992;183(1):201-6.
- Paszat L, Sutradhar R, Grunfeld E, Gainford C, Benk V, Bondy S, et al. Outcomes of surveillance mammography after treatment of primary breast cancer: a population-based case series. Breast Cancer Res Treat. 2009;114(1):169-78.
- Palli D, Russo A, Saieva C, Ciatto S, Rosselli Del, Turco M, et al. Intensive vs clinical follow-up after treatment of primary breast cancer: 10-year update of a randomized trial. National Research Council Project on Breast Cancer Follow-up. JAMA. 1999;281(17):1586.
- Dershaw DD. Mammography in patients with breast cancer treated by breast conservation (lumpectomy with or without radiation) AJR Am J Roentgenol. 1995;164(2):309-16.
- Lee KA, Jochelson MS. Post breast conservation therapy imaging and local recurrence. Q J Nucl Med Mol Imaging. 2013;57(4):332-9.
- Liberman L, Van Zee KJ, Dershaw DD, Morris EA, Abramson AF, Samli B. Mammographic features of local recurrence in women who have undergone breast-conserving therapy for ductal carcinoma in situ. AJR Am J Roentgenol. 1997;168(2):489-93.
- Dershaw DD, McCormick B, Osborne MP. Detection of local recurrence after conservative therapy for breast carcinoma. Cancer. 1992;70(2):493-6.
- Destounis S, Morgan R, Arieno A, Seifert P, Somerville P, Murphy P. A review of breast imaging following mastectomy with or without reconstruction in an outpatient community center. Breast Cancer. 2011;18(4):259-67.
- Fajardo LL, Roberts CC, Hunt KR. Mammographic surveillance of breast cancer patients: should the mastectomy site be imaged? AJR Am J Roentgenol. 1993;161(5):953-5.
- Valagussa P, Bonadonna G, Veronesi U. Patterns of relapse and survival following radical mastectomy. Analysis of 716 consecutive patients. Cancer. 1978;41(3):1170-8.
- Zimmerman KW, Montague ED, Fletcher GH. Frequency, anatomical distribution and management of local recurrences after definitive therapy for breast cancer. Cancer. 1966;19(1):67-74.
- Crystal P, Strano SD, Shcharynski S, Koretz MJ. Using sonography to screen women with mammographically dense breasts. AJR Am J Roentgenol. 2003;181(1):177-82.
- Corsetti V, Houssami N, Ghirardi M, Ferrari A, Speziani M, Bellarosa S, et al. Evidence of the effect of adjunct ultrasound screening in women with mammography-negative dense breasts: interval breast cancers at 1 year follow-up. Eur J Cancer. 2011;47(7):1021-6.
- Buchberger W, Niehoff A, Obrist P, DeKoekkoek-Doll P, Dunser M. Clinically and mammographically occult breast lesions: detection and classification with high-resolution sonography. Semin Ultrasound CT MR. 2000;21(4):325-36.
- Kolb TM, Lichy J, Newhouse JH. Occult cancer in women with dense breasts: detection with screening US--diagnostic yield and tumor characteristics. Radiology. 1998;207(1):191-9.
- Yoo H, Kim BH, Kim HH, Cha JH, Shin HJ, Lee TJ. Local recurrence of breast cancer in reconstructed breasts using TRAM flap after skin-sparing mastectomy: clinical and imaging features. Eur Radiol. 2014;24(9):2220-6.
- Abati A, Simsir A. Breast fine needle aspiration biopsy: prevailing recommendations and contemporary practices. Clin Lab Med. 2005;25(4):631-54.
- [No authors listed]. The uniform approach to breast fine-needle aspiration biopsy. NIH Consensus Development Conference. Am J Surg. 1997;174(4):371-85.
- Albornoz CR, Bach PB, Mehrara BJ, Disa JJ, Pusic AL, McCarthy CM, et al. A paradigm shift in U.S. Breast reconstruction: increasing implant rates. Plast Reconstr Surg. 2013;131(1):15-23.
- Cemal Y, Albornoz CR, Disa JJ, McCarthy CM, Mehrara BJ, Pusic AL, et al. A paradigm shift in U.S. breast reconstruction: Part 2. The influence of changing mastectomy patterns on reconstructive rate and method. Plast Reconstr Surg. 2013;131(3):320e-6.
- Nedumpara T, Jonker L, Williams MR. Impact of immediate breast reconstruction on breast cancer recurrence and survival. Breast. 2011;20(5):437-43.