Research Article
Reported Opening Limitations as a TMD Symptom: A Clinical Report on Diagnoses and Outcome
Alexandra Carlsson1, Bengt Wenneberg2 and Christina Mejersjö3*
1Centre for Oral Rehabilitation, Public Dental Health, Linköping, Sweden
2Department of Stomatognathic Physiology, Gothenburg University, Sweden
3Clinic of Orofacial Pain, VGRegion Public Dental Health and Sahlgrenska Academy, Sweden
*Corresponding author: Christina Mejersjö, Clinic of Orofacial Pain, VGRegion Public Dental Health and Sahlgrenska Academy Specialisttandvården bettfysiologi, Universitetsklinikerna FTV Västra Götaland, Box 7163, SE-402 33 Gothenburg, Sweden
Published: 24 Jul, 2017
Cite this article as: Carlsson A, Wenneberg B, Mejersjö
C. Reported Opening Limitations as a
TMD Symptom: A Clinical Report on
Diagnoses and Outcome. Clin Surg.
2017; 2: 1572.
Abstract
Objective: To study diagnoses of reported mouth opening limitations and the outcome after
treatment, to better understand the symptom and the prognosis.
Methods: New referrals to an Orofacial Pain & Temporomandibular Disorders (TMD) Clinic with
the symptom of “jaw locking” in the referral were considered for this clinical prospective report.
This referrals constituted 5.8% of all the referrals during a ten month period, and 40 patients were
included. Case history, clinical examination and diagnoses were made according to the RDC/
TMD criteria. MRI and CT examinations of the temporomandibular joint were performed when
indicated. Reported symptoms and clinical signs were compared for different diagnoses. The
treatment was non-invasive and conservative, no patient underwent surgery. At end of treatment,
the clinical examination was repeated, the primary and definite diagnoses were compared, and the
improvement after treatment was evaluated.
Results: The main diagnoses were disc displacement with reduction (DDwR), 23%, disc displacement
without reduction (DDwoR), 30%, and myofascial pain with limited opening (wLO), 45%. General
Hypermobility was significantly more frequent in the disc displacement diagnosis compared with
myofascial pain (p<0.05). After treatment, the mean opening capacity was good, regardless of the
diagnosis.
Conclusion: A report of jaw locking is not indicative of a single diagnosis of TMD. A diagnosis
based on the history and a clinical examination is generally accurate. The symptom of opening
limitations responds well to conservative treatment methods.
Keywords: Jaw locking; Diagnosis; Treatment outcome; Disc displacement; Myofascial pain
Introduction
Opening limitations, catching and locking of the jaw, are common complains of patients
referred to a clinic for orofacial pain and temporomandibular disorders (TMD). TMD is a collective
term including a number of clinical symptoms and diagnoses of the masticatory muscles and/or
the temporomandibular joints (TMJ) [1]. Dentists and physicians often use the word locking in
their referrals and the patient can use the word to describe their condition of opening limitations.
Screening questions for reported symptoms are used; “Does your jaw get stack, locked or get out” [2]
and “Does your jaw lock or become stuck once a week or more” [3] with the intention of identifying
TMJ or disk problems. Also the RDC/TMD Patient History Questionnaire [4] version 2016, ask
“Have you ever had your jaw lock or catch”.
A study among adults found a prevalence of 4% of middle-aged women reporting frequent
locking of the jaw [5]. Another epidemiological study among children and adolescents found that
3.7% reported jaw locking [6], while the prevalence of reported intermittent locking of the jaw of
adolescents 18 years of age was 14% [7]. A meta-analysis on the prevalence of clinical signs of intraarticular
temporomandibular disorders in children and adolescents found a frequency of 2.3% with
locking [8].
It can be a major challenge for the clinician to determine whether a patient’s symptoms are
caused by disc displacement or due to myofascial pain with limited mouth opening (wLO). Testing
the end feel with a downward force on the mandibular incisors with the fingers, a soft end feel
and increased mouth opening suggests muscle-caused restriction, while a hard and not increased opening may indicate disc displacement without reduction (DDwoR)
[1]. Furthermore, a limited opening capacity of 24 mm - 30 mm
with deflection to the affected side, pain in the affected joint, and
impaired laterotrusion to the contralateral side but normal to the
ipsilateral side, are all signs that could indicate DDwoR. A history
of clicking that resolved with a sudden onset of opening limitations
has been interpreted as the disc being permanently displaced [1].
General Hypermobility has been identified as a risk factor for disc
derangements of the temporomandibular joint [9].
Muscle tissue damage from dental injections (post-injection
trismus), excessive chewing, yawning or dental treatment could
lead to myalgia causing opening limitations and a sensation of jaw
locking. The first muscular response to trauma is often a protective
co-contraction, with the antagonist muscles trying to protect the
injured part [10]. There is no or little pain when the muscle is at
rest, but use of the muscles increases the pain and mouth opening is
impaired. Prolonged muscle contractions may lead to local muscle
soreness and changes to the muscular tissues through the release of
bradykinin, substance p and histamine [11].
Examples of other diagnoses that could result in severe opening
limitations are TMJ arthritis, fibrosis and scarring of the TMJ cartilage,
oral infections, scleroderma, scars, and trismus caused by neoplasm
[12]; however, myofascial pain is the most common diagnosis [13].
A magnetic resonance image (MRI) examination of the TMJ
provides an estimation of the relationship between the joint
components, but does not always identify the cause of the reported
opening limitations [14].
The aims of the study were:
I. To identify the diagnoses of patients referred for “locking”
of the jaw;
II. To estimate how well the initial clinical examination
identified the diagnosis or whether this was changed after additional
examinations
III. To study the features of the different diagnoses and the
outcome after treatment.
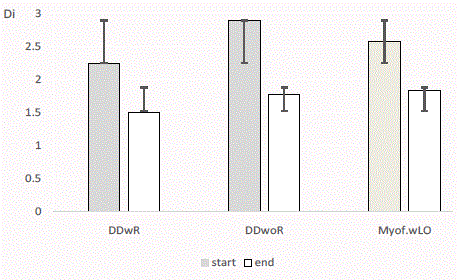
Figure 1
Figure 1
Clinical dysfunction index (Di) and standard deviation for three
diagnoses with opening limitations at start (first examination) and at end
of treatment (DDwR: Disc Displacement with Reduction; DDwoR: Disc
Displacement without Reduction; MP wLO: Myofascial Pain with Limited
Opening).
Materials and Methods
New referrals to the Orofacial Pain & TMD Clinic, Gothenburg,
were screened for “locking of the jaw” as described in the referral
and it was that description in the referral that qualified the patient
for inclusion in the study. The period of recruitment of consecutive
patients for this prospective observation study was ten months.
During this period, 783 patients were referred to the clinic, and 45
patients matched the inclusion criteria (nine males and 36 females,
aged 17-72 years), constituting 5.8% of the referrals. Five patients
postponed their examination and never came to an examination
within the study period, leaving 40 patients who were included in the
study. The patients were given a priority appointment for examination
at the clinic.
At the first visit to the clinic the patients completed a standardized
questionnaire concerning their jaw problems and general health. The
patient history was taken according to the Research Diagnostic Criteria
for TMD (RDC/TMD) [4]. The clinical examination was performed
by the same dentist for all the patients and according to the Axis I
(clinical condition) of RDC/TMD [15], including maximum opening
capacity, with and without pain, and additional “assisted opening”
by the examiner, also called “the end feel” [1]. The lateral movement
capacity was measured towards the affected, ipsilateral, side and to
the contralateral side, and the difference between the directions was
calculated. The patient´s history and the clinical examination resulted
in a primary diagnosis. The examination was extended [16] to allow
for calculation of the clinical dysfunction index evaluating the severity
of the clinical dysfunction [17] (Di 0-III; 0=no clinical signs; Di
I=mild; Di II=moderate; Di III=severe signs of clinical dysfunction).
The patient’s general hypermobility (HMS) was estimated according
to Beighton (0-9 points, >4 being hypermobile) [18].
The patient´s diagnosis refers to the side of the current symptoms
and the reason for the referral. Intramuscular local anaesthetic was
used as a diagnostic tool to block muscle pain. Manipulation of the
TMJ disc was performed when DDwoR was clinically suspected.
Computed tomography (CT) and MRI of the TMJs were
performed when clinically indicated. The indication for CT was
a suspicion of degenerative changes of the TMJ, and for MRI,
a suspicion of TMJ disc displacement. The examinations were
performed at the Department of Oral and Maxillofacial Radiology,
Institute of Odontology, Gothenburg. The preliminary diagnosis of
the disc position (RDC group II a or II b) was according to the clinical
examination.
The treatment followed the routines at the clinic for the condition
and was individually designed, including counselling and information,
awareness training and mobilization, local physical training and
relaxation, acupuncture and pharmacological management, and
stabilization splint [1,19]. No patient had a surgical intervention.
The same clinical examination as at start was repeated at the end
of treatment by the same examiner. The patient charts were later
looked into and narrowly observed, and reported symptoms, clinical
signs at the first examination and at the end of treatment, X-rays and
MRI examinations were compared for the different diagnoses. From
the patients´ chart, information was collected about the treatment
outcome as classified by the patients (impaired, unaltered, improved,
obviously improved, and symptom-free) and about any changes of
the preliminary diagnosis to the final diagnosis at end of treatment.
The questionnaire and the examination of the patients followed
the routines at the clinic. Informed consent to participate in the study
was obtained from each patient and the guideline of the Helsinki
Declaration has been followed in this investigation. The study was
discussed at the Ethical Committee at the University of Gothenburg,and according to their written policy for such studies, no more ethical
approval was required
The SPSS software version 22 was used for statistical processing.
Differences in frequency and severity of signs and symptoms between
groups were analyzed with the Chi-square and Mann-Whitney
U-tests. For analyzing differences of the mandibular moving capacity,
the Students t-test was used. The level for statistical significance
was set at p < 0.05. The agreement between the preliminary and the
definite diagnosis was calculated as a percentage of the agreement and
with the Cohen’s Kappa [20].
Table 1
Table 1
Diagnoses of 40 patients with reported mouth opening limitations, preliminary after the first clinical examination and definite for 33 patients after treatment (n:
Number of Patients; DDwR: Disc Displacement with Reduction, DDwoR: Disc Displacement without Reduction; wLO: with Limited Opening).
Results
The main diagnoses of the patients reporting a symptom of
“locking” were, disc displacement with reduction (DDwR) 23%, disc
displacement without reduction (DDwoR) 30%, and myofascial pain
with limited opening (wLO) 45%. The proportion of females was the
same for the diagnoses. The duration of symptoms was longer for
DDwR and the experienced locking was often intermittent. The mean
age for both DDwR and DDwoR was 35 years, while it was 45 years
for the myofascial pain wLO patients, the difference between DDwR
and myofascial pain wLO being statistically significant (p < 0.05).
The diagnoses at the first examination and at the end of treatment
are shown in Table 1. The seven patients with only one appointment
at the clinic only received a preliminary diagnosis. Comparing the
diagnoses at the start and at the end of treatment for 33 patients, an
agreement was found in 80 % and with κ=0.731 (good agreement
[18]). The primary diagnosis was changed in six patients, with the
greatest change for DDwoR, where 25% (three patients) had their
diagnosis changed; two to myofascial pain wLO and one to arthritis.
Of the 40 patients in the study, eleven patients had a MRI and
17 aCT examination. All DDwoRs were confirmed by MRI, but the
examination also revealed DDwoR in the opposite joints in 67%
of the patients examined. From the MRI, it was noticed that most
joints with DDwoR had an indication of degenerative TMJ changes.
Degenerative changes were frequently found by CT in the affected
joint but also in the opposite TMJ.
Analyzing features of the different diagnoses, a report of TMJ
clicking prior to the experienced locking was common in all three
diagnoses, 73% – 89%. Hypermobility was observed in 75% of the
patients with DDwR, in 33% of the DDwoR patients and in 20%
of the myofascial pain wLO patients. Both the DD diagnoses had
significantly more general hypermobility compared with myofascial
pain wLO (p< 0.05).
Deflection of the mouth-opening path was not an appropriate
description of any of the diagnoses studied, nor did the estimation of
the end feel differ significantly for any of the diagnoses. Tenderness
on palpation of the TMJ was found in all three diagnoses and was not
descriptive of any of them.
TMJ pain on mouth opening was significantly more often
found in DDwoR (p< 0.01), as was pain on lateral excursion both
from and towards the affected side (p< 0.05). The lateral excursion
towards the contralateral side, compared with towards the affected
side, was impaired in DDwoR and the mean difference between the
movements was -3 mm (-9 mm – 0 mm). For myofascial pain wLO,
the laterotrusion difference ranged from -6 mm to +6 mm (mean
+ 1.4 mm); however, the difference between the diagnoses was not
statistically significant.
The outcome after treatment was good for all diagnoses; for
DDwoR, 78% were improved and 22% were symptom-free, for
DDwR, 75% were improved but no symptom-free, and for myofascial
pain wLO, 66% were improved and 13% symptom-free. The clinical
dysfunction index was significantly reduced after treatment for all
three diagnoses (Figure 1), and the mouth opening capacity was
significantly improved, reaching a mean of 45 mm for DDwoR and
myofascial pain wLO (p < 0.001), and 46 mm for DDwR (p< 0.05).
On average, the patients had a treatment period of ten months (2-16
months) and five visits (2-11) to the clinic.
Discussion
The main findings of the study were that myofascial pain wLO
was a more frequent diagnosis underlying the patient’s report of jaw
locking than DDwoR. A TMJ disc with a closed lock is sometimes
regarded as identical with a sensation of locking, but severely limited
mouth opening can be due to either muscle or joint problems, and
sometimes there is also a displaced disc in a patient with myofacisal
pain. Differentiating between muscle and joint symptoms may be
difficult, and a rather similar status was found for both muscle and
joint causes.
The primary diagnoses determined after only history-taking and
a clinical examination were often accurate, but the features of the
different diagnoses were not as clear as described [1,15]. A history
of clicking before the opening limitations appeared was frequently
reported for all three diagnoses studied, and the end feel [1] failed in
our study to disclose clear differences.
The impairment of lateral movement was more elusive.
Impaired lateral mandibular movement to the contralateral side
was descriptive of DDwoR. Hypermobility is a known risk factor for
TMJ disc disorders [9] and was also in this study associated with disc
displacement.
The MRI examination confirmed DDwoR in the patients with
that clinical diagnosis, but also frequently revealed disc derangement
of the opposite joint, although asymptomatic. Probably, some disc displacements were present among those not examined with MRI,
however, not the current problem. The DDwoR noticed on MRI
could also be a consequence of an impaired mouth opening due to
muscle pain and no reduction of the disc occurred at the time of
the examination. One of the shortcomings of the study is that not
all patients had a MRI examination showing the disc position of the
side of the patient´s symptoms, but the study focus on the patient´s
current symptoms which is not always explained by the MRI picture.
The finding of the study of frequent degenerative changes in joints
with DD is in accordance with other studies, like Cortes et al. [21],
who found a significant association between disc displacement and
degenerative changes.
There has been some discussion concerning whether the term
disc derangement would better describe the status of a TMJ with disc
displacement [22]. Epidemiologically, disc displacement is frequently
found, often without any pain or impaired mouth opening. In some
cases the development of a new pseudo disc has also been described
[23].
For most of the patients, hyperactivity and overloading of the
muscles and the TMJs were recognized as the cause of the symptoms.
The treatment focused on measures to unload and relax the system,
to promote a varied functional pattern and improved mouth opening
with or without the disc in its original place [1,19]. According to
the dysfunction index, the outcome after treatment was good, but
numerically better for DD than for myofascial pain wLO, which was
also noticed by Takahara [24].
The study found a good result of conservative treatment
methods of reported limited mouth opening. Surgical treatment
of disc displacement has produced varied results. Lavage gave an
effect equivalent to that of local anesthetics [25], and another study
found lavage to be an effective method when the effect of previous
conservative treatment was poor [26]. In a follow-up after 24 and 60
months, Schiffmann et al. [27] found no difference in treatment effect
between four different strategies for closed lock. Manipulation of the
TMJ disc seldom gives a lasting result, and a review [28] concludes
that DDwoR should be treated by the simplest and least invasive
method.
After treatment the dysfunction was significantly reduced and the
maximum mouth opening reached about the same mean capacity,
regardless of the diagnosis. This reassuring information is important
to give to the patient, who often finds the symptom very unpleasant.
The proportion of 5.8% of the referrals expressing symptoms of
jaw locking is close to the report of 6% by Dahlström [29], and he
concluded that there is often a combination of myalgia and disc
displacement. Reported locking has been identified as one predictor
of the onset of TMD symptoms [30], which indicates the importance
of paying attention to the symptom.
To conclude, the sensation of jaw locking is not a defined
dental symptom and is not an expression of a single diagnosis but
of many diagnoses with the symptom of mouth opening limitations.
The patient’s history and the clinical examination often provide
sufficient information for the diagnosis; the symptom responds
well to conservative treatment and has a good prognosis. Impaired
lateral movement from the affected side and TMJ pain on mandibular
movement was descriptive of DDwoR.
References
- Okeson JP, editor. Management of temporomandibular disorders and occlusion. 7th ed. Mosby: Elsevier Inc. 2013;129-69,222-90.
- American Academy of Orofacial Pain. General assessment of the orofacial pain patient. De Leeuw R, Klasser GD, editors. Orofacial pain – guidelines for assessment, diagnosis and management. 5th ed. Chicago:Quintessence. 2013:25-46.
- Lövgren A, Visscher CM, Häggman-Henrikson B, Lobbezoo F, Marklund S. Validity of three screening questions (3Q/TMD) in relation to the DC/TMD. J Oral Rehabil. 2016;43(10):729-36.
- Schiffman EL, Truelove E, Ohrbach R, Andersson G, John MT, List T, et al. The Research Diagnostic Criteria for Temporomandibular Disorders. I: overview and methodology for assessment of validity. J Orofac Pain. 2010;24:7-24.
- Yekkalam N, Wänman A. Prevalence of signs and symptoms indicative of temporomandibular disorders and headaches in 35-, 50-, 65- and 75-year-olds living in Västerbotten, Sweden. Acta Odontol Scand. 2014;72(6):458-65.
- Hirsch C, Hoffmann J, Turp JC. Are temporomandibular disorder symptoms and diagnosis associated with pubertal development in adolescents? An epidemiological study. J Orofac Orthop. 2012;73:6-8,10-18.
- Mejersjö C, Ovesson D, Mossberg B. Oral parafunctions, piercing and signs and symptoms of temporomandibular disorders in high school students. Acta Odontol Scand. 2016;74(4):279-84.
- da Silva CG, Pachêco-Pereira C, Porporatti AL, Savi MG, Peres MA, Flores-Mir C. Prevalence of clinical signs of intra-articular temporomandibular disorders in children and adolescents: A systematic review and meta-analysis. J Am Dent Assoc. 2016;147:10-18.
- Chang TH, Yuh DY, Wu YT, Cheng WC, Lin FG, Shieh YS, et al. The association between temporomandibular disorders and joint hypermobility syndrome: a nationwide population-based study. Clin Oral Investig. 2015;19:2123-32.
- Okesson JP. Bell´s Orofacial Pains. The clinical Management of Orofacial Pain. 6th edition, Chicago, Quintessence Publishing. 2005:287-328.
- Tegeder L, Zimmermann J, Meller ST, Geisslinger G. Release of algesic substances in human experimental muscle pain. Inflamm Res. 2002;51(8):393-402.
- Stern D. Benign and Malignant Tumors. In: Laskin DM, Green CS, Hylander WL (editors). Temporomandibular Disorders: an evidence-based approach to diagnosis and treatment. Quintessence Publishing Co, Inc. 2006:319-33.
- Manfredini D, Guarda Nardini L. TMD classification and epidemiology. In: Manfredini D (ed). Current concepts on temporomandibular disorders. Quintessence Publishing Co, Ltd. 2010:32-5.
- Emshoff R, Rudisch A, Innerhofer K, Brandlmaier I, Moschen I, Bertram S. Magnetic resonance imaging findings of internal derangement in temporomandibular joints without a clinical diagnosis of temporomandibular disorder. J Oral Rehabil. 2002;29:516-22.
- Look JO, Schiffman EL, Truelove EL, Ahmad M. Reliability and validity of Axis I of the Research Diagnositc Criteris for temporomandibular disorders (RDC/TMD) and proposed revisions. J Oral Rehabil. 2010;37:744-59.
- Carlsson GE, Magnusson T. Management of temporomandibular disorders in the general dental practise. Chicago: Quintessence; 1999:67-78.
- Helkimo M. Studies on function and dysfunction of the masticatory system. II. Index for anamnestic and clinical dysfunction and occlusal state. Sv Tandlak Tidskr.1974;67:101–21.
- Horan FT, Beighton PH. Recessive inheritance of generalized joint hypermobility. Rheumatol Rehabil. 1973;12(1):47-9.
- Cortés D, Exss E, Marholz C, Millas R, Moncada G. Association between disk position and degenerative bone changes of the temporomandibular joints: an imaging study in subjects with TMD. Cranio. 2011;29(2):117-26.
- Practical statistics for medical research. Altman DG, editor. London: Chapman and Hall. 1991;406-8.
- Cortes D, Exss E, Marholz C, Millas R, Moncada G. Association between disk position and degenerative bone changes of the temporomandibular joints: an imaging study in subjects with TMD. Cranio. 2011;29:117-26.
- Stegenga B, de Bont LGM. TMJ disc derangements. In: Laskin DM, Green CS, Hylander WL, editors. Temporomandibular Disorders: an evidence-based approach to diagnosis and treatment. Quintessence Publishing Co, Inc. 2006:125-36.
- Bristela M, Schmid-Schwap M, Eder J, Reichenberg G, Kundi M, Piehslinger E, et al. Magnetic resonance imaging of temporomandibular joint with anterior disk dislocation without reposition – long-term results. Clin Oral Invest. 2016;16.
- Abboud W, Yahalom R, Givol N. Treatment of Intermittent Locking of the Jaw in Wilkes Stage II Derangement by Arthroscopic Lysis and Lavage. J Oral Maxillofac Surg. 2015;73(8):1466-72.
- Schiffman EL, Velly AM, Look JO, Hodges JS, Swift JQ, Decker KL, et al. Effects of four treatment strategies for temporomandibular joint closed lock. Int J Oral Maxillofac Surg. 2014;43(2):217-26.
- Abboud W, Yahalom R, Givol N. Treatment of Intermittent Locking of the Jaw in Wilkes Stage II Derangement by Arthroscopic Lysis and Lavage. J Oral Maxillofac Surg. 2015;73(8):1466-72.
- Schiffman EL, Velly AM, Look JO, Hodges JS, Swift JQ, Decker KL, et al. Effects of four treatment strategies for temporomandibular joint closed lock. Int J Oral Maxillofac Surg. 2014;43(2):217-26.
- Al-Baghdadi M, Durham J, Araujo-Soares V, Robalino S, Errington L, Steele J. TMJ disc displacement without reduction management: A systematic review. J Dent Res. 2014;93(7 Suppl):37S-51S.
- Dahlström L. Diagnoses among referrals to a Swedish clinic specialized in temporomandibular disorders. Acta Odontol Scand. 1998;56(3):143-7.
- Ohrbach R, Bair E, Fillingim RB, Gonzalez Y, Gordon SM, Lim PF, et al. Clinical orofacial characteristics associated with risk of first-onset TMA: the OPPERA prospective cohort study. J Pain 2013;14(12 Suppl) T33-50.