Case Report
Huge Liposarcoma of the Thigh with Decubitus Ulcers: Report of a Case
Dutta Gautam1*, Sagar Poonam2, Kala Sanjay1, Sonkar Manoj1 and Singh Raj Kumar1
1Department of Surgery, GSVM Medical College, Kanpur, India
2Department of ENT, Maulana Azad Medical College, New Delhi, India
*Corresponding author: Gautam Dutta, Department of Surgery, GSVM Medical College, Kanpur, UP- 208002, India
Published: 18 Jul, 2017
Cite this article as: Gautam D, Poonam S, Sanjay K, Manoj
S, Kumar SR. Huge Liposarcoma of the
Thigh with Decubitus Ulcers: Report of
a Case. Clin Surg. 2017; 2: 1569.
Abstract
We are presenting a case of huge liposarcoma of the left thigh with decubitus ulcers in a patient
aged 60 years. The tumor was overlooked and the patient came to us due to increasing difficulty in
walking due to the progressively increasing size and weight of the said tumor. We are discussing the
presentation, clinical findings, the relevant investigations and the operative management of the case.
The large dimensions with decubitus ulcers, heavy weight and the infiltration of the tumor in the
muscle planes were some of the interesting findings of this case.
Keywords: Lipoma-like; Liposarcoma; Surgery; Soft tissue tumor
Introduction
Virchow was the first to describe liposarcoma in 1860s. The liposarcomas are the malignancies of the fat cells of the body, which usually appear as a slowly enlarging painless mass, though some may show rapid enlargement with ulcerations of the overlying skin. They are overall the most common soft tissue tumors, with an annual incidence of 2.5 cases per million populations. The trunk and lower extremities are the most common sites affected, followed by head and neck region. Oral involvement may occur, although very rare. They mostly arise from the deep-seated stroma rather than the subcutaneous or submucosal fat. Most cases arise de novo, sarcomatous changes of a pre-existing lipoma is rare.
Case Presentation
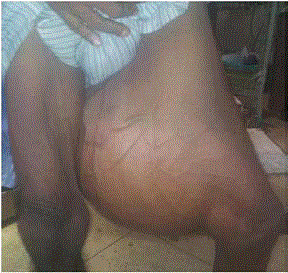
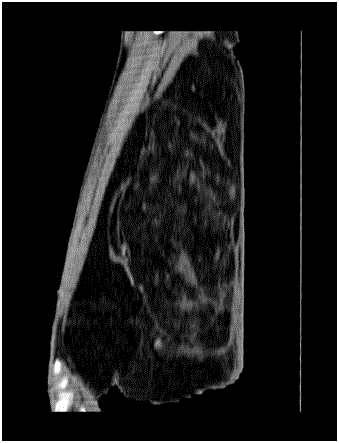
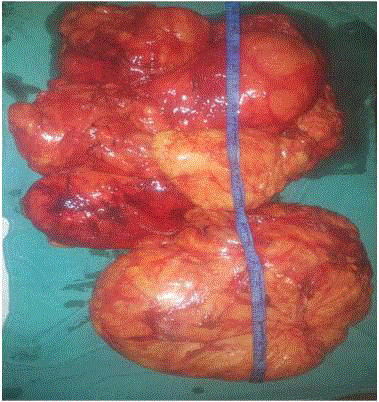
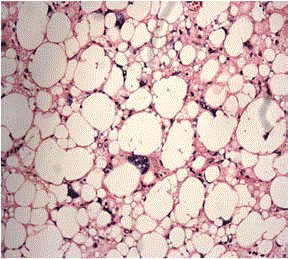
A 60-yr old male came to our OPD with gradually progressive swelling over the posterior aspect of his left thigh from past 5 years. The progression was very insidious and painless. However, the patient complained that the rate of growth of the lump had been faster from past one year, with ulcerations on the overlying skin and progressively increasing difficulty in walking due to increasing weight of the tumor. The local examination demonstrated a 50X35 cms tumor, firm in consistency with reduced mobility. There was no tenderness on both superficial and deep palpation. There were two ulcers over the mass (5 cm × 4 cm and 3 cm × 3 cm each) which bled on touch (Figure 1) The overlying veins were prominent (Figure 2). There was no inguinal lymphadenopathy. Blood investigations were essentially normal. Helical CT of the involved thigh revealed a large (345 mm × 181 mm × 256 mm) fibrofatty space occupying lesion in posterior aspect of the left thigh with multiple septations. Within the septations, large quantity of fat tissue with increased attenuating fibrous and vascular bundles were seen. No involvement of bony cortex of left femur or any vascular bundle was seen. Inguinal lymph nodes were within normal limits (Figure 3). Excision of the tumor was done under regional anaesthesia. During surgery, a large, well-encapsulated tumor (weight 15 kg, dimensions 50 cm × 35 cm) was found, situated between the adductor and large muscles that pushed the muscles aside (Figure 4). Post-op was uneventful, drain removed on 6th POD and stitches removed on 10th POD, the stitch-line was healthy. On pathological examination, lipoblasts were seen with abundant clear multi-vacuolated cytoplasm and eccentric darkly stained nucleus indented by the vacuoles (Figure 5). Final diagnosis of well-differentiated lipoma-like liposarcoma was made. The patient recovered well and no signs of local or systemic relapse were seen 6 months of follow-up. The patient did not receive adjuvant or neoadjuvent chemotherapy or radiotherapy.
Discussion
Liposarcomas represent 10% - 35% of all soft tissue sarcomas, making them the second most common type after malignant fibrous tumors. The WHO classification of soft tissue tumors (2002) divided liposarcomas into five distinct histological subtypes: well differentiated, dedifferentiated, myxoid, pleomorphic and mixed. The diversity of these lesions is reflected by their clinical and biological behaviour, which ranges from non-metastatic tumors (well-differentiated liposarcoma) to tumors with high metastatic potential (pleomorphic liposarcoma) [1]. Because of this behaviour, pathological and radiological evaluation is critical for establishing an appropriate therapy [2]. Malignant transformation of lipomas has been rarely reported, but, as a rule, well-differentiated liposarcomas are not derived from lipoma [3,4]. The image on CT or MRI exams and the morphological relationship between the areas of fat and non-fat components allows the identification of the histological subtype of liposarcomas. Thick connective septa (> 2 mm) inside of a poorly vascularized fat tumor are suggestive of the diagnosis of welldifferentiated liposarcoma [5]. Well-differentiated liposarcoma most frequently affects the deep soft tissues of extremities (65% - 75% of cases); over 50% of these are located in the lower limbs, especially the thigh [6] and have no metastatic potential unless de-differentiation, but they may have local recurrences [7]. Prognosis and treatment of these tumors is strongly related to their anatomical location. For subcutaneously located lesions, surgical excision with wide resection margins is sufficient; in such cases, local recurrence is minimal to nonexistent. For well-differentiated liposarcoma, which are located deeper in the body, the local recurrence risk is high. Studies have shown that local recurrence rate is of 43% for lesions located in the extremities, 70% for groin tumors and 91% for retroperitoneal lesion [8]. In these instances, radiotherapy may be used as adjunctive therapy to decrease local recurrence rate. Mortality associated with multiple complications or local recurrence is significant when well differentiated liposarcomas are located in the retroperitoneal (33%) or inguinal (14%) areas and is insignificant for extremities lesions if de-differentiation does not appear [9]. Concerning our patient, there was no muscle, vascular or bone tumor invasion, therefore, despite its huge size, a large excision allowed an R0 resection (negative surgical margins). Subsequent follow-up did not identify any local recurrence. The absence of local invasion and a lower degree of aggressiveness of the tumor correlates with a favourable prognosis.
Figure 1
Figure 2
Figure 3
Figure 3
Helical CT of the thigh revealed a large (345 mm × 181 mm × 256
mm) fibrofatty space occupying lesion in posterior aspect of the left thigh with
multiple septations.
Figure 4
Figure 5
Figure 5
Lipoblasts with abundant clear multi-vacuolated cytoplasm and
eccentric darkly stained nucleus indented by the vacuoles.
Conclusion
Adipocyte tumors represent the largest single group of mesenchymal neoplasms, due to the high prevalence of lipomas and their variants. Liposarcoma represents the single most common sarcoma in adults. Surgical excision is the main treatment for most liposarcomas. As such, every possible effort should be made to completely remove the tumor. These tumors usually have a low metastatic potential, especially if located in extremities. Well differentiated liposarcomas located on the extremities do not require any adjuvant chemotherapy or radiotherapy. The overall survival and prognosis is favourable.
References
- Murphey MD, Arcara LK, Fanburg-Smith J. From the archives of the AFIP: Imaging of musculoskeletal liposarcoma with radiologic-pathologic correlation. Radiographics. 2005;25:1371-95.
- Chang HR, Hajdu SI, Collin C, Brennan MF. The prognostic value of histologic subtypes in primary extremity liposarcoma. Cancer. 1989;64:1514-20.
- Sampson CC, Saunders EH, Green WE, Laurey JR. Liposarcoma developing in a lipoma. Arch Pathol. 1960;69:506-10.
- Sternberg SS. Liposarcoma arising within a subcutaneous lipoma. Cancer. 1952;5:975-8.
- Hosono M, Kobayashi H, Fujimoto R, Kotoura Y, Tsuboyama T, Matsusue Y, et al. Septum-like structures in lipoma and liposarcoma: MR imaging and pathologic correlation. Skeletal Radiol. 1997;26:150-4.
- Enzinger FM, Winslow DJ. Liposarcoma. A study of 103 cases. Virchows Arch Pathol Anat Physiol Klin Med. 1962;335:367-88.
- Forus A, Larramendy ML, Meza-Zepeda LA, Bjerkehagen B, Godager LH, Dahlberg AB, et al. Dedifferentiation of a well-differentiated liposarcoma to a highly malignant metastatic osteosarcoma: amplification of 12q14 at all stages and gain of 1q22-q24 associated with metastases. Cancer Genet Cytogenet. 2001;125:100-11.
- Chung PW, Deheshi BM, Ferguson PC, Wunder JS, Griffin AM, Catton CN, et al. Radiosensitivity translates into excellent local control in extremity myxoid liposarcoma: A comparison with other soft tissue sarcomas. Cancer. 2009;115:3254-61.
- Kindblom LG, Angervall L, Svendsen P. Liposarcoma a clinicopathologic, radiographic and prognostic study. Acta Pathol Microbiol Scand Suppl. 1975;253:1-71.