Case Report
Primary Extradural Osteolytic Meningioma: A Case Report
Sushil Kumar1*, Aparajita Singh2 and Amit Handa1
1Department of Neurosurgery, St. Stepehen’s Hospital, Tis Hazari, Delhi, India
2Department of Radiology, St. Stepehen’s Hospital, Tis Hazari, Delhi, India
*Corresponding author: Sushil Kumar, Department of Neurosurgery, St. Stepehen’s Hospital, Tis Hazari, Delhi
Published: 13 Jul 2017
Cite this article as: Kumar S, Singh A, Handa A. Primary
Extradural Osteolytic Meningioma: A
Case Report. Clin Surg. 2017; 2: 1560.
Abstract
A 35-year-old lady presented with gradually progressive painless swelling in the left frontal region
which was hard anteriorly and soft posteriorly. Computed tomography (CT) showed an osteolytic
expansile lesion, enhancing uniformly on contrast magnetic resonance imaging (MRI). The
lesion was excised with a wide margin of healthy bone and on histology it was confirmed to be a
meningiothelial meningioma.
Keywords: Extradural meningioma; Osteolytic; Subdural extension
Introduction
Meningiomas commonly arise from the arachnoid cap cells located in the external layer of the arachnoid membrane. The extracranial meningiomas are rare, comprising 1-2% of all meningiomas [1,2]. Meningiomas originating outside the dural compartment are variously called ectopic, extradural, calvarial, cutaneous extracranial, extraneuraxial or intraosseous meningiomas. Lang et al. [3] proposed the term “primary extradural meningiomas” for this type of lesion and the term defines the origin of this tumor as being separate from the dural covering of the brain. Meningiomas in such locations may be hyperostotic, osteolytic or mixed. The osteolytic variety is the rarest hence being reported.
Case Presentation
A 35-year-old lady presented with gradually progressive painless swelling in the left frontal
region for the last 2 years. There was no history of trauma or fever. On examination there was a
diffuse swelling with the anterior part being hard and the posterior part being soft. The swelling was
non-tender and the overlying skin could be pinched off the swelling. The swelling was fixed, nonfluctuant
without any cough impulse.
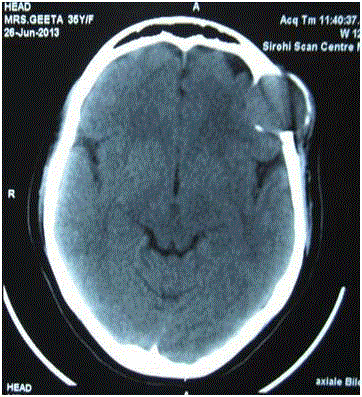
Computed tomography scan revealed a left sided frontal intradiploic mass expanding the
calvaria with prominent bone destruction (Figure 1). The lesion extended through the skull defect
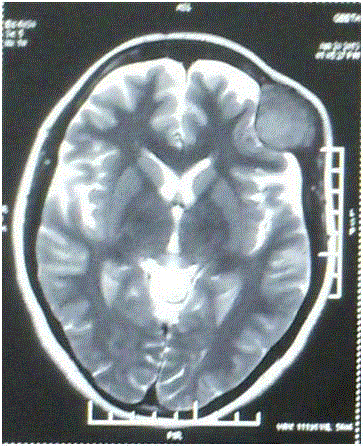
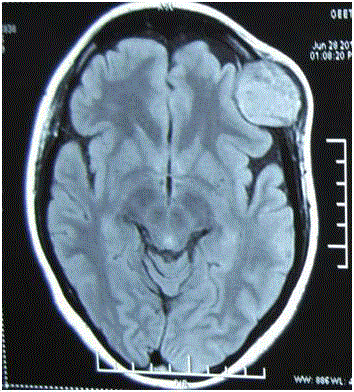
both intra and extracranially. Magnetic resonance imaging revealed the mass to be hyperintense
on T1 weighted images and isointense on T2 weighted images (Figure 2a and 2b). Gadolinium
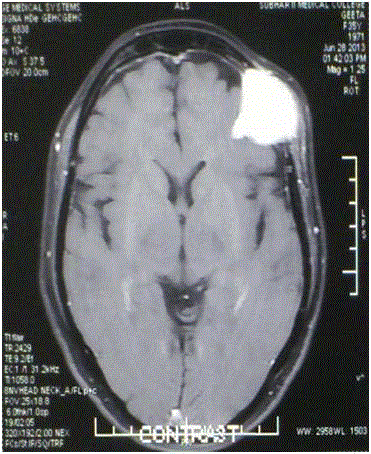
administration showed homogenous enhancement of the lesion (Figure 2c). MRI also revealed the
small subdural extension of the lesion (Figure 2c).
The pre-operative diagnosis was intradiploic meningioma of the osteolytic variety. At surgery
the tumor was solid, well defined, expanded both the inner and outer table of the skull, destroyed
the dinner table at one place and perforated in to the subdural space through a thinned out but
not infiltrated dura (Figure 3). After removal of the tumor along with a wide margin of healthy
bone, cranioplasty was done using methylmethacrylate. Histopathology confirmed the diagnosis of
meningiothelial meningioma without any evidence of malignancy.
Discussion
Intradiploic meningiomas usually present as painless expansile masses without any
neurological symptoms and signs. However symptoms if present are dependent on tumor
location, size and involvement of the neighboring structures. Meningiomas presenting with
scalp swelling and extracranial soft tissue mass are more aggressive in nature than their cranial
counterparts [4]. However our case did not show any sign of malignancy on histologic examination.
Intradiploic meningiomas are typically either osteoblastic or osteolytic or at times mixed types. Osteolytic type appears as radiolucent on plain X-Rays. The osteolytic lesion may appear as hypodense on plain computed tomography
with thinning, expansion and discontinuity of the inner and outer
cortical layers. Tumor enhances on contrast administration [5].
All these features were typically seen in our patient. On magnetic
resonance imaging (MRI), T1 weighted images show hypointense or
isointense signal while T2 weighted images are usually hyperintense.
Homogenous enhancement after gadolinium administration is typical
and was observed in our case as well. The intradiploic osteolytic
subtype is extremely rare and only 17 cases have been reported in the
literature [6,7]. The only curative treatment is wide surgical resection
accompanied by cranioplasty in the same sitting. If the resection is
subtotal as is usual in the basal region, the tumor should be followed
up radiologically and irradiated if progression is there [8].
Lang classified intraosseous meningiomas as purely extracalvarial
(Type I), purely calvarial (Type II) or calvarial with extracalvarial
extension (Type III). The latter two are further divided as convexity(C)
or skull base (B) forms. In our case as the epicenter of the tumor was
in extracalvarial space, it was believed to have arisen away from the
dura with later impingement, thinning and perforation of a small
nubbin, through the dura into the subdural space. Only 8 cases
with intradural component of this type have been reported in the
literature [9,10]. Our case is of primary extradural type as the dura
was displaced inwards from the dinner table of the skull, a finding
thought to be consistent with an extradural growth. Som et al. [11]
reported that direction of the bone displacement and subsequent
bone remodeling caused by tumor growth is suitably accurate in
ascertaining the presumed site of origin.
Many hypotheses have been formed to explain the origin of
primary extradural meningiomas. Azar K et al. [12] postulated their
origin from meningiocytes trapped in the cranial sutures during
head molding at birth. Zulch et al. [13] postulated their origin to
entrapment of arachnoid within the site of fractures. Lopez et al. [14]
postulated arachnoid cells along the peripheral portion of the cranial
nerves to be responsible for primary extradural meningioma in PNS,
orbit and neck.
Shuangshoti et al. [15] proposed that primary extradural
meningioma arise directly from multipotential mesenchymal
cells or from metaplasia of mesenchymal cell types, e.g. fibroblasts
and Schwann cells. By the foregoing postulations it seems primary
extradural meningiomas have a multifactorial etiology.
Figure 1
Figure 1
Computerized tomography scan axial view showing expansion and
destruction of the left frontal bone.
Figure 2a
Figure 2b
Figure 2c
Figure 2c
MRI axial sections-Homogenously enhancing after contrast
administration on T1 weighted image.
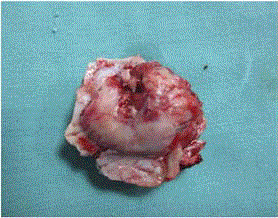
Figure 3
Figure 3
Photograph of excised specimen showing well delineated tumor on
the inner aspect of the bone.
References
- Mazumdar DP, Vengsarkar US, Bhatjiwale MG, Goel A. Diffuse calvarial meningioma: a case report. J Postgrad Med. 2001;47(2):116-8.
- Whicker JH, devine KD, McCarty CS. Giagnostic and therapeutic problems in extracranial meningiomas. Am J Surg. 1973;126(4):452-7.
- Lang FF, MacDonald OK, Fuller GN, DeMonte F. Primary extradural meningioma: a report of nine cases and review of literature from the era of computerized tomography scanning. J Neurosurg. 2000;93(6):940-50.
- Muthukumar N. Primary calvarial meningiomas. Br J neurosurg. 1997;11(5):388-92.
- Agrawal V, Ludwig N, Agrawal A, Bulsars KR. Intraosseous intracranial meningioma. AJNR Am J Neuroradiol. 2007;28(2):314-5.
- Rosahl SK, Mirzayan MJ, Samii M. Osteolytic intraosseous meningiomas: illustrated review. Acta Neurochir (Wein). 2004;146(11):1245-9.
- Sheikhrezaie A, Meybodi AT, Hashemi M, Shafiee S. Primary intraosseous osteolytic meningioma of the skull: a case report. Cases J. 2009;2:7413.
- Crawford TS, Kleinschmidt-DeMasters BK, Lillehei KO. Primary intraosseous meningioma. Case report. J Neurosurg. 1995;83(5):912-5.
- Oka K, Hirakawa K, Yoshida S. Primary calvarial meningiomas. Surg Neurol. 1989;32(4):304-10.
- Arana E, Menor F, Lloret RM. Intraosseous meningioma. J Neurosurg. 1996;85(2):362-3.
- Som PM, Sachdev VP, Sacher MM. Intrafrontal sinus primary meningioma. Neurodiology. 1991;33(3):251-2.
- Azar-Kia B, Sarwar M, Marc JA. Intraosseous meningioma. Neuroradiology. 1974;6(5):246-53.
- Zulch KJ. Brain tumors: Their biology and pathology. 3rd Ed. Berlin: Springer-Verlag. 1986:72-77.
- Lopez DA, Silvers DN, Helwig EB. Cutaneous meningiomas-a clinicopathological study. Cancer. 1974;34(3):728-44.
- Shuangshoti S, Netsky MG, Fitz-Hugh GS. Parapharyngeal meningioma with special reference to cell of origin. Ann Otol Rhinol Laryngol. 1971;80(3):464-73.