Research Article
Patient Age Significantly Influences Post-Esophagectomy Inpatient Mortality, Length of Stay, Hospital Charges, and Discharge Disposition
Esther H Cha, Gregory Burgoyne and Richard F Heitmiller*
Department of Surgery, MedStar Union Memorial Hospital, USA
*Corresponding author: Richard F Heitmiller, Department of Surgery, MedStar Union Memorial Hospital, 3333 N. Calvert Street, JPB Suite 610, Baltimore, Maryland, USA
Published: 06 Jul 2017
Cite this article as: Cha EH, Burgoyne G, Heitmiller RF.
Patient Age Significantly Influences
Post-Esophagectomy Inpatient
Mortality, Length of Stay, Hospital
Charges, and Discharge Disposition.
Clin Surg. 2017; 2: 1539.
Abstract
Background: There are conflicting reports on the merits of surgery in older esophageal cancer
patients. The objective of this study is to track inpatient outcome, hospital charges, and discharge
disposition as a function of age.
Study Design: The Nationwide Inpatient Sample was searched for all patients from 2006 to 2010
with a primary diagnosis of esophageal cancer (ICD-9: 150) and underwent esophagectomy (ICD-9:
424). Cervical and upper third malignancies (ICD-9: 150.0 & 150.3) were excluded. Data recorded
included age, gender, mortality, length of stay (LOS), hospital charges, discharge, disposition, and
diagnosis and procedure codes. Patients were stratified into three age groups: < 55; 55-74; 75 years
and older. Results were analyzed using Chi2 and ANOVA.
Results: 9,970 patients were included in this study. 81.2% were male. Mean age, mortality, LOS and
charges were 63.3 years, 6.1%, 16.9 days and $161,229 respectively. For the age groups < 55, 55-74,
≥75 respectively, mortality was 2.5, 6.3, 10.3% (p<0.01); LOS was 15.3, 16.8, 19.4 days (p<0.01).
There was a significant increase need for post-discharge skilled nursing facility based on age. Home
health care was common for all groups (41.2-46.4%).
Conclusion: Post-esophagectomy in-patient mortality, LOS, inpatient charges and the need for
post-discharge to skilled nursing facility increase significantly with age. Inpatient charges alone
underestimate the overall cost of esophagectomy care. These results should help in selecting
esophageal cancer patients for surgery.
Keywords: Esophagectomy; Esophageal cancer; Age; Nationwide inpatient database;
Esophagectomy; Cancer; Patient age; Mortality; Charges; Discharge; Disposition; Length of
stay; LOS
Abbreviations
ASA: American Society of Anesthesiologist; CGA: Comprehensive Geriatric Assessment; ECOG: Eastern Cooperative Oncology Group; LOS: Length of stay; NIS: National Inpatient Sample; SEER: Surveillance, Epidemiology, and End Results
Introduction
Esophagectomy for patients with esophageal cancer remains a complex surgery, associated with significant morbidity and mortality despite advances in surgical technique and post-operative care. The number of elderly patients with esophageal cancer that present for surgical evaluation is increasing [1]. The purpose of this study is to assess the function of age with respect to outcomes and hospital charges of esophageal cancer patients undergoing surgery. This data will allow improved patient selection as well as provide reasonable expectations regarding outcomes and discharge disposition following surgery.
Methods
A retrospective cohort study was designed to evaluate patients following esophagectomy for
esophageal cancer. Data were gathered from the National Inpatient Sample (NIS), Healthcare Cost
and Utilization Project (HCUP), Agency for Healthcare Research and Quality from 2006 to 2010
[2]. The study was exempt from formal review by the Institutional Review Board as the NIS data
lacks discrete patient identifiers.
ICD-9-CM diagnosis and procedure codes were used to select
patients with a primary diagnosis of esophageal cancer (ICD-9-CM
diagnosis code 150.X) and who underwent esophageal resection (ICD-
9-CM procedure code 42.4X). Cervical and upper third malignancies
(ICD-9-CM diagnosis code 150.0 and 150.3 respectively) were
excluded to limit potential confounding variables, such as head and
neck malignancies.
Patients were stratified to three groups based upon age: Group
1: Age < 55 years-old; Group 2: Age 55 - 74 years old; Group 3: Age
≥75 years-old. Analysis of these three groups was performed to
determine mean mortality, mean LOS and percentage distribution
across the discharge options. Furthermore, patients were stratified by
age (in decades) to determine distribution of disease by age as well as
mortality.
Our hypothesis is that outcomes and hospital charges after
esophageal resection for the three patient age groups would be
significantly different. Continuous and categorical data were
evaluated with uni-variate analysis of variance (ANOVA) and chisquared
analysis, respectively, using Microsoft Office Excel 2007®
(Microsoft, Redmond, WA, USA). Significance was determined with
a p-value less than α: 0.05.
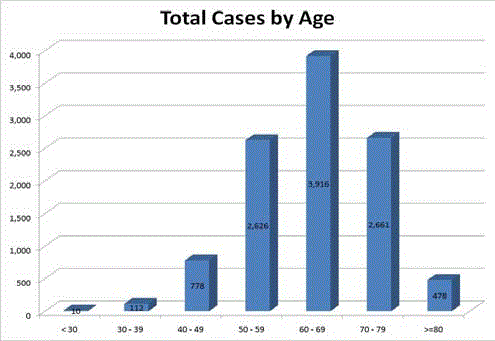
Figure 1
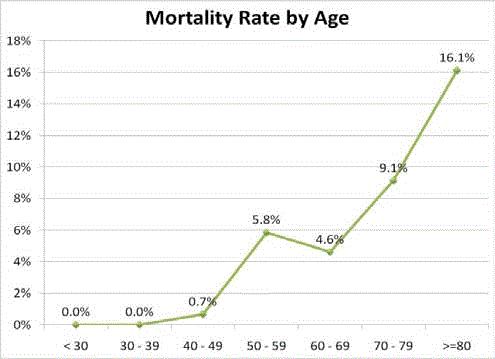
Figure 2
Results
A total of 9,971 patients undergoing esophagectomy for cancer
of the middle and lower esophagus from 2006 to 2010. Data for
mortality rate, age, gender distribution, LOS and hospital charges are
summarized by year in (Table 1). For this 5 year period, there were
an average of 1,994 cases per year (1,720-2,234) and a total of 613
deaths with a mean mortality rate of 6.1% (4.1% - 8.2%). The mean
overall age was 63.3 years (62.7-63.7) and the majority of the patients
were male (81.2%) compared to female patients (18.8%). The mean
overall LOS was 16.9 days (16.1-17.8) with mean hospital charges of
$161,229. Results for the three age groups (< 55 year; 55 - 74 years;
≥75) including mean mortality rate, LOS, discharge disposition
and hospital charges are summarized in Table 2. Statistical analysis
showed a significant difference in mortality (2.5%; 6.3%; 10.3%), LOS
(15.3; 16.8; 19.4) and hospital charges ($146,605; $157,612; $198,639)
between the three age groups (p<0.01).
Significant differences (p< 0.01) were also noted between the
age groups of patients of who underwent routine discharge (45.2%;
32.8%; 15.8%), were discharged home with home health (46.4%;
45.4%; 41.2%) or were transferred to a skilled nursing facility (5.1%;
14.5%; 31.6%).Transfer to another hospital showed no significant
difference (p: 0.74). Figure 1 shows the distribution of esophagectomy
cases for esophageal cancer across age by decade with the majority
of cases between the ages of 50 and 80 years old (Figure 2) displays
the mortality rate for the same cases across age by decade with the mortality increasing from 0.7% in the 40 - 49 range to 16.1% in the
age ≥ 80 range.
Table 1
Table 2
Discussion
Esophagectomy for patients with esophageal cancer remains
a complex surgery with significant morbidity, mortality despite
advancements in surgical technique and post-operative care [1].
Although the prevalence of esophageal cancer in the United States has
remained static over the last decade, the Surveillance, Epidemiology,
and End Results (SEER) website projects 16,910 new cases for the year
2016 [3]. At the same time, the United States population is aging. As a
result, an increasing number of senior esophageal cancer patients are
presenting for consideration of surgery [4]. Is it reasonable to offer
surgery to esophageal cancer patients regardless of age, or is there
a point at which the risk-benefit odds are tipped against operative
treatment? The purpose of this study was to assess cost, risks, and
discharge disposition of esophageal cancer patients undergoing
surgery as a function of age. Armed with this information, patient
selection for surgery will be enhanced, and patients better informed
about what they can expect for both surgery and early recovery.
In our study the NIS database was searched to identify all patients
undergoing esophagectomy for cancer for the period 2006 through
2010. The search excluded upper thoracic and cervical esophageal
cancers to ensure patients with primary head and neck malignancies
were not included. This period was selected as it gave complete date
over a five year period. The overall patient characteristics, by year,
are shown in (Table 1). The number of surgery patients remains
relatively constant at approximately 2000 per year consistent with
the SEER esophageal cancer prevalence data. Patient characteristics
are consistent with published data and show a mean age is 63.3
years, and a male predominance (81.2%), Mean LOS and mortality
was 16.9 days and 6.1% (4.1% - 8.2%) respectively. The cost of care
increased each year. (Figure 1) shows the age distribution of the entire
cohort of patients. Twenty-nine percent of patients were 70 years of
age or older (Table 2) summarizes post surgical outcome by age. By
far the 55 - 74 year group was the largest as expected, and patients
who were >75 years represented 13% of the total cohort. Operative
mortality increased significantly, almost exponentially, by age (Figure
2). Mortality for patients 80 years of age or older was a remarkable
16.1%. Both LOS and hospital cost rose significantly by age, but less
dramatically than mortality. One of the most interesting findings in
this review was data on post-discharge disposition. For the purposes of
this study, we defined a routine discharge as one in which there was no
need for skilled nursing facility or home health support. Remarkably,
even for the < 55 years group, less than half of patients (45.2%) had a
routine discharge. This fell to only 15.8% for patients over 75 years of
age. Only 5.1% of < 55 group needed transfer to skilled nursing facility
compared with almost a third (31.6%) for patients over 75 years of
age. All of these results were significant. Transfer to another acute
care facility was uncommon for all age groups. Furthermore, the cost
of all of post-discharge care was not included in the cost data listed
which was for acute care hospital charges only. This means that the
cost of care listed in this database greatly underestimated the overall
cost of care especially for older patients.
Currently many factors come into play when considering surgery
for esophageal cancer patients including surgical morbidity and
mortality, LOS, cost of care, post-discharge disposition, and time to
return to independent activity, quality of life, and survival. All of this
must be further weighted against non-operative treatment options.
Assessing surgical risk, especially when it becomes prohibitive,
can be difficult and controversial. Boyd and Jackson emphasize that
surgical risk varies according to the observer such as patient, family,
nurse, surgeon, anesthesiologist, intensivist, and administrator. They
propose a clinical definition of high risk as >5% mortality, or 2x the
mortality for the general population. Extremely high risk would be
a surgical mortality of >20% [5]. Our results (Figure 2) show that
patients age 70-79 would therefore be considered high risk with
surgical mortality of 9.1%, and patients over 80 years (mortality
16.1%) are close to being “extremely” high risk.
In our study, age was the only variable compared with outcome.
This was a fortuitous variable to track as age, either alone or indirectly,
is central to most published methods of pre-operative risk assessment.
The American Society of Anesthesiologist (ASA) class system has
long been a useful clinical tool. It is based not on age but on clinical
status and co-morbidities. However, the probability of accumulating
co-morbidities and developing declining clinical performance rises
with age. Therefore, ASA class is indirectly related to age.
Fuchs et al. [6] developed a risk assessment scoring system
specifically for esophagectomy patients. The scoring system assigns
points to patient factors including age, co-morbidities, tumor cell
type, hospital volume, and surgical approach. The Society of Thoracic
Surgeons database identified congestive failure, functional status,
smoking (current or former history), three incision esophagectomy,
squamous cell pathology, and age >65 years as factors increasing
patient risk for esophagectomy [7]. Park et al.[8] reported emergency
surgery and increased frailty index increased risk. The frailty index
is a method used to determine a patient’s biologic age as opposed to
chronologic age. Fischer et al. [9] identified co-morbidities, ECOG performance status, and ASA class as risk factors for esophagectomy.
Again, both ECOG functional status and ASA class are indirectly
related to age. In a cohort of elderly cancer patients (>75 years old)
undergoing esophagectomy, Yamamoto et al. [10] observed post
operative delirium in 26%. Delirium was associated with other
complications and increased LOS. The likelihood of delirium could
be predicted by pre-surgery comprehensive geriatric assessment
(CGA). The CGA is composed of 5 test elements that would each be
adversely affected by age.
Furthermore, similar to our study, the incidence of being
discharged to a rehabilitation facility for patients with and without
delirium was 30.4% vs. 13.6% respectively. Several authors have
documented the consequences and costs associated with operating
on high risk patients and recommend careful consideration when
evaluating such patients for surgery [11-13]. Our study has several
limitations. It is a retrospective study that dates back to 2006. It uses
a broad national database and does not reflect individual surgeon,
institution, or patient results. Only a single variable (age) is tracked.
However, it does not change the fact that this data, and supporting
literature, clearly show that advancing age is a well documented
risk factor for esophageal cancer patients considering surgery.
Furthermore, age ≥75 years of age is associated with significantly
increased risk. This fact, and the high likelihood of need for postdischarge
home or skilled nursing care in elderly patients, should be
part of the discussion of any esophagectomy surgical consent.
Conclusion
Post-esophagectomy in-patient mortality, LOS, inpatient charges and the need for post-discharge to skilled nursing facility increase significantly with age. Inpatient charges alone underestimate the overall cost of esophagectomy care. These results should help in selecting esophageal cancer patients for surgery and communicating post-operative expectations.
References
- Raymond DP, Seder CW, Wright CD, Magee MJ, Kosinski AS, Cassivi SD, et al. Predictors of major morbidity or mortality after resection for esophageal cancer: A Society of Thoracic Surgeons General Thoracic Surgery database risk adjustment model. Ann Thorac Surg. 2016;102(1):207-14.
- Rockville. Healthcare Cost and Utilization Project (HCUP). 2006-2009. Agency for Healthcare Research and Quality. 2006.
- SEER Databases. Surveillance, Epidemiology, and End Results (SEER) Program Research Data (1973-2013), National Cancer Institute.
- Finlayson E, Fan Z, Birkmeyer J. Outcomes in octogenarians undergoing high-risk cancer operation: a national study. J Am Coll Surg. 2007;205(6):729-34.
- Boyd O, Jackson N. Clinical review: How is risk defined in high-risk surgical patient management? Crit Care. 2005;9(4):390-96.
- Fuchs HF, Harnsberger CR, Broderick RC, Chang DC, Sandler BJ, Jacobsen GR, et al. Simple preoperative risk scale accurately predicts perioperative mortality following esophagectomy for malignancy. Dis Esophagus. 2016;30(1):1-6.
- Society of Thoracic Surgery General Thoracic Surgery Database guidelines. Accessed on. 2016;1.
- Park KU, Rubinfeld I, Hodari A, Hammoud Z. Prolonged length of stay after esophageal resection: Identifying drivers of increased length of stay using the NSQIP database. J Am Coll Surg. 2016;223(2): 286-90.
- Fischer C, Lingsma H, Hardwick R, Cromwell DA, Steyerberg E, Groene O. Risk adjustment models for short-term outcomes after surgical resection for oesophagogastric cancer. BJS. 2016;103(1):105-16.
- Yamamoto M, Yamasaki M, Sugimoto K, Maekawa Y, Miyazaki Y, Makino T, et al. Risk evaluation of postoperative delirium using comprehensive geriatric assessment in the elderly patients with esophageal cancer. World J Surg. 2016;40(11):2705-12.
- Dimick JB, Pronovost PJ, Cowan JA, Lipsett PA. Complications and costs after high-rick surgery: where should we focus quality improvement initiatives? J Am Coll Surg 2003;196(5):671-8.
- Gaitonde SG, Hanseman DJ, Wima K. Resource utilization in esophagectomy: when higher costs are associated with worse outcomes. J Surg Oncol. 2015;112(1):51-55.
- Stahl CC, Hanseman DJ, Wima K, Sutton JM, Wilson GC, Hohmann SF, et al. Increasing age is a predictor of short-term outcomes in esophagectomy: a propensity score adjusted analysis. J Gastrointest Surg. 2014;18(8):1423-28.