Research Article
Absorbable Suture as a Preferred Option for Lateral Ankle Instability Repair
Adebola Tee Adeleke1*, Nathan Judd1, Zflan Swayzee1, J Joseph Anderson2 and Dallin Greene3
1Department of Podiatric Surgery, American Foundation of Lower Extremity Surgery and Research, USA
2Department of Podiatric Surgery, New Mexico Bone and Joint Institute, USA
3Department of Podiatric Surgery, Third Year Resident, United Health Services, USA
*Corresponding author: Adebola T Adeleke, Department of Podiatric Surgery, American Foundation of Lower Extremity Surgery and Research, 2301 Indian Wells Dr. Suite A, Alamogordo, NM, 88310 USA
Published: 15 Jun, 2017
Cite this article as: Adeleke AT, Judd N, Swayzee Z,
Anderson JJ, Greene D. Absorbable
Suture as a Preferred Option for Lateral
Ankle Instability Repair. Clin Surg.
2017; 2: 1516.
Abstract
Lateral ankle instability is most commonly caused by inversion ankle sprains as these disrupt the soft tissue constraints of the ankle. Of the patients who suffer from an inversion ankle sprain, 50% will develop ankle pathology and up to 20% will develop chronic lateral ankle instability. Surgical intervention is necessary in those who do develop chronic ankle instability, usually utilizing the modified Brostrom procedure. This is a well-documented procedure that has historically relied primarily on the characteristics of suture material. It is shown, however, that non-absorbable sutures are used and that it can affect complication rates of the procedure. In this study we examine the use of absorbable suture for the modified Brostrom procedure and compare it to expected outcomes of the procedure. A total of 352 patients that underwent the Brostrom procedure were reviewed with an age range of 18-76, mean of 39.58 and a split of 202 males and 150 females. Visual analog scale pain scores and American College of Foot and Ankle Surgeons hindfoot and ankle scores were taken preoperatively and postoperatively at 3, 12 and 24 months. The decrease in pain and increase in foot function values were deemed significant in improvement (p< 0.01). Only 6 patients (1.7%) required revision due to re-injury. The results indicate that the use of absorbable suture is a viable means of performing the Brostrom procedure with a low complication rate which leads to long-term patient satisfaction.
Introduction
The ankle is a complex joint that primarily exhibits sagittal plane motion along with secondary
frontal plane excursion. The joint has multiple ligamentous attachments that aid in its stabilization,
in fact, 70% of ankle joint stability is soft tissue derived [1]. This stability is most commonly
disrupted through an inversion injury on a plantar flexed foot. The majority of the injuries was
treated conservatively and healed uneventfully [2]. Research has shown that as much as 50% of
patients with ankle sprains develop some kind of long-term sequelae and up to 20% will suffer from
chronic symptomatic ankle instability [1,3].
Lateral ankle instability can be classified into two separate groups, functional and mechanical.
Functional instability refers to a subjective feeling or sensation that the ankle is about to give way,
while mechanical instability is used when patients show excessive ankle ROM, this would include a
positive anterior drawer and talar tilt test with radiographs or telos used for confirmation [4].
Chronic lateral ankle instability, regardless of classification, that does not improve conservatively
may go on to surgical intervention. Currently, over 80 procedures have been described for
lateral ankle stability repair [5]. These procedures usually attempt to restore stability by primary
ligamentous repair with or without augmentation, grafting techniques or tendon transfer [6-10].
An example of primary ligamentous repair of the lateral ankle is the Brostrom procedure, which
has extensively been analyzed and described in literature [1,5,7,11-14]. The Brostrom procedure
has been shown to have well to excellent results 86% to 95% of the time in both short and long
term follow up [15-19]. The Brostrom procedure was initially described using a fine synthetic nonabsorbable
suture [6]. Today, surgeons continue to recommend using non-absorbable suture for
lateral ankle repair [20]. Conversely, the use of absorbable suture as well as a combination of both
are well-supported in literature [11,13,18,21].
Although shown to be superior in strength, the use of non-absorbable suture in ligamentous
repair has demonstrated well-documented complications throughout the body. There have been case reports that describe retained infection secondary to a nonabsorbable
suture implanted in tissue as well as scar formation and
tissue erosion [22-24].
This type of encapsulation isn’t as rare as it has been with other
non-absorbable sutures thereby igniting an inflammatory cascade
involving histiocytes, giant cells and lymphocytes [24]. Among
other non-absorbable sutures this reaction was found especially in
polyester suture, which is commonly used for the modified Brostrom
procedure.
The success of the Brostrom procedure using sutures or anchors
has been well-documented; however, literature base remains sparse
when looking at the outcome of absorbable suture specifically for
the repair of ligamentous structures in lateral ankle stabilization
[21,25,26]. The purpose of this research manuscript will be to present
the outcomes of subjects who underwent lateral ankle stabilization
using absorbable suture while also adding to a sparse literature
database on the topic.
Table 1
Table 1
There were 352 patients in the cohort that were reviewed. The cohort was divided into 202 males and 150 females and the average age was 39.6 years.
Table 1
Patients and Methods
Patients were seen and treated between 2005 and 2009 for lateral
ankle instability secondary to an ankle sprain. All Patients failed
conservative care prior to surgical intervention: immobilization,
ankle bracing and physical therapy. Patients were excluded from the
study if they met the criteria of diagnosis of a fracture secondary to
the ankle sprain, osteochondral defect, previous surgery, inadequate
fibular groove, anterior lateral ankle impingement, perineal tendon
pathology, patients with connective tissue disease or anyone with a
neurologic disease.
Following failure of conservative treatment patients were given
the option of surgery. Of those who opted for surgery, 94.6% had
confirmed damage to the lateral ankle ligamentous complex on MRI.
The surgeries were performed by the same surgeon (JJA) and were
done at two outpatient surgery centers and one outpatient hospital.
Just prior to surgery a Visual Analog Score (VAS) and modified
American College of Foot and Ankle Surgeons (ACFAS) hind foot
ankle score was used to obtain preoperative subjective scores.
The patients were transported to the operating room and placed
on the operating table in a supine position. General anesthesia was
delivered and the extremity was prepped and draped in the usual
sterile manner. A standard ankle distractor under standard tension
was then placed on the patients’ ankle with distal distraction. Gravity
pressure was used in order to help maintain joint distraction. A full
diagnostic ankle arthroscopy was performed with debridement of
synovitic tissue and hypertrophic synovium. Pre and post debridement
photos were taken and a portal sweep exchange was performed. The
medial portal was then closed with 4-0 non-absorbable synthetic
monofilament suture.
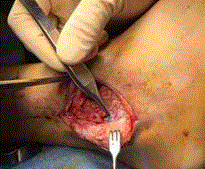
The lateral portal incision was then extended distally to curving
around the distal tip of the fibula in a curvilinear fashion. Care
was taken to avoid contact with neurovascular structures. #0, #1
polygalactin 90-10 braided absorbable suture were used to reapproximate
the anatomic alignment of the anterior talofibular and
calcaneofibular ligaments and perform a pants–over–vest reefing of
the lateral aspect of the extensor retinaculum (Gould modification).
Deep closure was performed using #2-0 polygalactin 90-10 braided
absorbable suture and subcutaneous closure with #3-0 polygalactin
90-10 braided absorbable suture. Cutaneous closure was then
performed using #4-0 non-absorbable, synthetic monofilament
suture (Figure 1).
A dry sterile dressing was then applied and the patient’s lower
extremity was splinted while the foot was held in a dorsiflexed and
everted position. At two weeks, the patient was placed in an equalizer
boot with passive range of motion and continued to stay non-weight
bearing. At four weeks full weight bearing and physical therapy
began. Patients were allowed to return to full activities at 12 weeks.
At three months, 12 months and 24 months following the
procedure the patients were re-evaluated. The patients were assigned results based on ACFAS scores and visual analog scale (VAS) scores.
Figure 1
Results
There were 352 patients in the cohort that were reviewed. The
cohort was divided into 202 males and 150 females and the average
age was 39.6 years (Table 1).
Patients had a pre - operative VAS score of 6.28 and 1.09 postoperatively
(Table 2).
ACFAS scores improved significantly from pre= operative to 3
months, 12 months and 24 months respective (Table 2).
Patients underwent physical therapy pre-operatively for 6.61
weeks while post-operative sessions lasted for 5.19 weeks, a difference
that exhibited statistical significance (Table 1).
A total complication rate of 4.55 % was seen, most of which
being nerve entrapment. Other complications included two patients
with superficial dehiscence, one with CRPS and one with superficial
cellulitis. This study’s low complication rate of 4.55% supports current
literature in regards to the modified Brostrom procedure as well as
supports the use of absorbable suture as an effective, reproducible and
safe means of performing the Brostrom procedure.
Discussion
The main finding in the study is that the Brostrom procedure is an
effective lateral ankle stabilizer and that the use of absorbable suture
is viable, safe and just as effective when compared to historical data
using non-absorbable suture.
The Brostrom procedure was initially shared in literature by Dr.
Lennart Brostrom in 1966 by using a non-absorbable synthetic thread
[6]. Since his published paper, many surgeons have tried everything
from other types of non-absorbable suture, absorbable suture and
anchors. Regardless of the type of suture or anchor used, research
still finds that each technique yields favorable outcomes even though
some studies share that using anchors increases the stability of the
correction.
Suture characteristics come into play when deciding which would
be a viable option for surgery. Strength is an important characteristic
when performing a lateral ankle stabilizing procedure since you are
repairing the ligament that is responsible for restraining anterior
displacement of the talus in relation to the tibia and fibula. For the
most part non-absorbable suture is stronger than absorbable suture
but, a study performed in 2010 by Najibi et al. [27] indicated that
polygalactin 90 -10 braided absorbable suture failed at a higher
maximum load than polyester braided suture of an equivalent size.
In fact, the paper concluded that #1 polygalactin 90 -10 braided
absorbable suture has equivalent strength to #2 polyester braided
suture and the polygalactin 90 -10 braided absorbable suture material
is less stiff, making it easier to work with Human tissue reactions
have also been observed secondary to implantation of different
suture types. Braided polyester suture showed to be surrounded by
a fibrous tissue capsule lined with histiocytes and giant cells and
another study showed the same type of suture to have significantly
more suture granulomas present than other sutures studied [24,28].
Another important characteristic is not security, which the optimal
suture would allow a strong knot security with minimal number
of square knots thrown that would reduce operation time, reduce
tissue reaction and less risk of infection. Polygalactin 90 -10 braided
absorbable sutures has been shown to have the advantage of keeping a
strong knot with minimal amount of square knots thrown [29].
In conclusion, the bioabsorbability, knot security and patient
outcomes have shown that polygalactin 90 -10 braided absorbable
suture would be a more advantageous suture than the braided
polyester material for the Brostrom procedure. Absorbable suture
has been shown to have similar results and excellent outcomes as
compared to the historic literature. We have had excellent results
with statistically significant improvement as illustrated by VAS and
ACFAS scores. We believe that our recurrence and complication
rates are better than those explained literature, 2.6% to 17%, when
compared to different suture types and different techniques [3,30,31].
We understand the limitations of this study include the lack
of a control group, using non-absorbable suture, thereby calling
into question the study’s effectiveness as derived from the use of
absorbable suture rather than from the Brostrom procedure itself.
Despite the limitation, the use of absorbable suture as a viable, lowrisk
and long-term successful means for performing the Brostrom
procedure can’t be ignored. Further comparative studies are needed.
References
- Berlet G, Landis G, Hyer C, Philbin T. Anatomic Repair of Lateral Ankle Instability. Operative Techniques in Foot and Ankle Surgery. 2011;99:834-41.
- Kerkhoffs G. Acute Lateral Ankle Ligament Ruptures in the Athletes. Foot Ankle Clin N Am. 2013;18:215-18.
- Giannini S, Ruffilli A, Pagliazzi G, Mazzotti A, Evangelisti G, Buda R, et al. Treatment Algorithm for Chronic Lateral Ankle Instability. Muscl, Lig Tend. 2014;4:455-60.
- Baravarian B, Ben-Ad R. Exploring Surgical Options for Lateral Ankle Instability. Pod Tod. 2014;27:5.
- Bauer G. New Method for Reconstruction in Lateral Ankle Instability. Am Podiat Med Assoc. 1995;85:459-63.
- Brostrom L. Sprained Ankles IV. Surgical Treatment of “Chronic” Ligament Ruptures. Acta Chir Scand. 1966;132:551-65.
- Keller M, Grossman J, Caron M, Mendicino RW. Lateral Ankle Instability and the Brostrom-Gould Procedure. Foot Ankle Surg. 1996;35:513-20.
- Visser HJ, Oloff M, Jacobs AM. Lateral Ankle Stabilization Procedures: Criteria and Classification. Foot Surg. 1980;19:74-89.
- Yu GV, Lynn JA, Thornton D, Choos JN. The Split Peroneus Longus Lateral Ankle Stabilization Procedure. Foot Ankle Surg. 1994;33:298-313.
- Janis LR, Kittleson RS, Cox DG. Chronic Lateral Ankle Instability: Assessment of Subjective Outcomes Following Delayed Primary Repair and a New Secondary Reconstruction. Foot Ankle Surg. 1998;37:369-75.
- Xinning Li, Timothy J Lin, Brian D Busconi. Treatment of Chronic Lateral Ankle Instability: A Modified Brostrom Technique Using Three Suture Anchors. J Orthop Surg Res. 2009;4:41.
- Byung-Ki Cho, Yong-Min Kim, Dong-Soo Kim, Eui-Sung Choi, Hyun-Chul Shon, Kyoung-Jin Park. Outcomes of the Modified Brostrom Procedure Using Suture Anchors for Chronic Lateral Ankle Instability-A Prospective, Randomized Comparison between Single and Double Suture Anchors. Foot Ankle Surg. 2013;52:9-15.
- Rockett M, Lateral Ankle Stabilization: The Modified Brostrom-Gould Procedure. Master Techniques in Podiatric Surgery: Foot Ankle. 2005;37:481-90.
- Hardy M, Hild G. Acute Ankle Conditions. McGlamry’s Comprehensive Textbook of Foot and Ankle Surgery. 2013;702-9.
- Liu SH, Jason WJ. Lateral Ankle Sprains and Instability Problems. Clin Sports Med. 1994;13:793-809.
- Karlsson J, Bergsten T, Lansinger O, Peterson L. Reconstruction of the Lateral Ligaments of the Ankle for Chronic Lateral Instability. Bone Joint Surg.1988;70:581-8.
- Bell SJ, Monogne TS, Sitler DF, Cox JS. Twenty-Six-Year Results After Brostrom Procedure for Chronic Lateral Ankle Instability. Am J Sport Med. 2006;34:975-8.
- Maffulli N, Del Buono A, Maffulli G, Oliva F, Testa V, Capasso G, et al. Isolated Anterior Talofibular Ligament Brostrom Repair for Chronic Lateral Ankle Instability: 9-Year Follow-up. Am J Sport Med. 2013;41:858-64.
- Sjolin SU, Dons-Jensen H, Simonsen O. Reinforced Anatomical Reconstruction of the Anterior Talofibular Ligament in Chronic Anterolateral Instability Using a Periosteal Flap. Foot Ankle. 1991;12:15-8.
- Ryan J. Principles and Techniques of Tendon and Ligament Repair. PodiatInstit Update. 2010;52.
- Vitale TD, Fallat LM. Lateral Ankle Sprains: Evaluation and Treatment. Foot Surg.1988;27:248-57.
- Yeo C, Russell N, Sharpe T. Nonabsorbable-Suture-Induced Osteomylitis: A Case Report and Review of the Literature. Case Reports in Orthopedics. 2012;2012:3.
- Rhee YG, Ha JH. Knot-induced Glenoid Erosion after Arthroscopic Fixation for Unstable Superior Labrum Anterior-Posterior lesion: A Case Report. Shoulder Elbow Surg. 2006;15:391-3.
- Postlethatwait RW, Willigan DA, Ulin AW. Human Tissue Reaction to Sutures. Annals of Surg. 1975;181:144-50.
- Kocoaglu B, Ulku TK, Gereli A, Karahan M, Turkmen M. Evaluation of Absorbable and Nonabsorbable Sutures for Repair of Achilles Tendon Rupture with a Suture-Guiding Device. Foot Ankle Int. 2015;36:691-5.
- Montiero G, Ejnisman B, Andreoli CV, Pochini AC, Cohen M. Absorbable Versus Non-absorbable Sutures for the Arthroscopic Treatment of Anterior Shoulder Instability in Athletes: A Prospective Randomized Study. Arthroscopy. 2008;24:697-703.
- Najibi S, Banglmeier R, Matta JM, Tannast M. Material Properties of Common Suture Materials in Orthopaedic Surgery. Iowa Orthop. 2010;30:84-8.
- LoCicero J, Robbins J, Webb W. Complications Following Abdominal Fascial Closures Using Various Nonabsorbable Sutures. Surg Gynec Obstet. 1983;157:25-7.
- Rodeheaver G, Thacker J, Edlich R. Mechanical Performance of Polyglycolic Acid and Polyglactin 910 Synthetic Absorbable Sutures. Surg Gynec Obstet. 1981;153:835-41.
- Li X, Killie H, Guerro P, Busconi BD. Anatomical Reconstruction for Chronic Lateral Ankle Instability in the High-Demand Athlete: Functional outcomes after the Modified Brostrom Repair Using Suture Anchors. Am J Sports Med. 2009;37:488-94.
- Eung SK, Kyung TL, Jun SP, Young KL. Arthroscopic Anterior Talofibular Ligament Repair for Chronic Ankle Instability with a Suture Anchor. Orthop. 2011;34:273.