Case Report
A Rare Complication of Nasogastric Tube Insertion: Bronchopleural Fistula
Tevfik Ilker Akcam*, Ali Ozdil, Ahmet Kayahan Tekneci and Ufuk Cagirici
Department of Thoracic Surgery, Ege University Faculty of Medicine, Izmir, Turkey
*Corresponding author: Tevfik Ilker Akcam, Department of Thoracic Surgery, Ege University, Faculty of Medicine, 35100, Bornova, Izmir, Turkey
Published: 13 Jun, 2017
Cite this article as: Akcam TI, Ozdil A, Tekneci AK, Cagirici
U. A Rare Complication of Nasogastric
Tube Insertion: Bronchopleural Fistula.
Clin Surg. 2017; 2: 1510.
Abstract
A nasogastric tube (NGT) had been inserted due to the complaints of refusal of oral nutrition and aglutition to a sixty-one years old female with schizophrenia. Disturbance in general status,
hypotension, dispnea and tachicardia were observed after the initiation of enteral feeding. Chest
X-ray revealed left hydropneumothorax therewith tube thoracostomy was performed. Enteral
feeding fluid drainage was observed. Thorax computed tomography showed NGT to be in the left
pleural space. The patient was followed up after the removal of NGT and the tube thoracostomy
was ended on the sixteenth day. The patient was discharged from the hospital without any sequela.
Although insertion of NGT is a simple procedure it can result in serious complications like epistaxis,
pharyngeal perforation, osephagial rupture and pneumothorax. The localization of the tube must be
corrected after insertion in order to avoid and detect these serious complications.
Keywords: Bronchopleural fistula; Hydropneumothorax; Nasogastric tube
Introduction
Nasogactric tube (NGT) insertion is one of the most common procedures for gastro-intestinal system evaluation [1]. It can be used with the aim of aspiration of gastric content, evaluation and treatment of recurrent vomiting, evaluation of organ injury in trauma patients, enteral feeding etc [1]. Complications like epistaxis, intracranial or bronchial localization, pharyngeal or alveolar perforation, esophageal or gastric or duodenal rupture and pneumothorax can be seen due to the malposition of NGT [2,3]. Bronchial rupture is also one of the rare complications. We report a case of hydro-pneumothorax due to the bronchopleural fistula after the insertion of NGT for enteral feeding.
Case Presentation
A sixty-one years old female patient with schizophrenia underwent coronary angiography
with cardiac complaints. After the angiography treatment of the patient was rearranged due to the
increase of the psychiatric findings. In the follow-up, NGT was inserted because of the refusal of
oral nutrition, disphagia and aglutition. In a short time interval after the initiation of enteral feeding
from NGT disturbance in general status, hypotension, dispnea and tachicardia were observed.
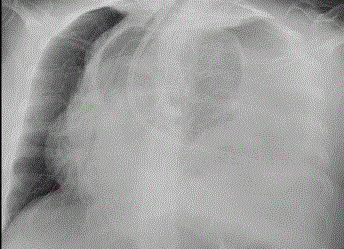
Breath sounds were reduced on the left hemithorax in physical examination. Chest X-ray revealed
left hydro-pneumothorax (Figure 1). Enteral feeding solution drainage was observed after the
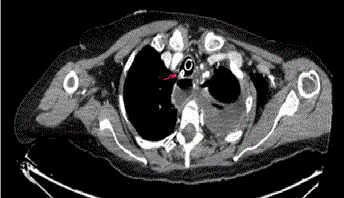
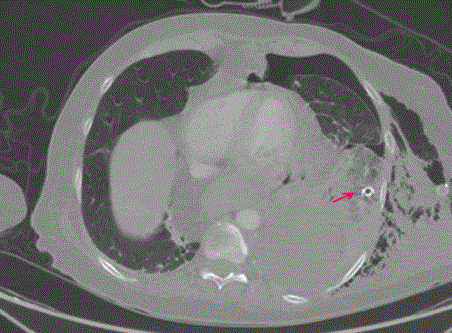
implementation of left tube thoracostomy. Thorax computed tomography showed NGT passing
through trachea to the left main bronchus (Figure 2), going on to the lower lobe lateral basal
segment parenchyma and ending in the left pleural space causing parenchymal laceration. NGT
was ended with the guidance of endoscopy and stent was placed to the narrowed segment of the
esophagus by Gastroenterology Clinic. Bronchopleural fistula localization could not be detected on
bronchoscopy.
The patient was followed up with pleural lavage two times per day with effective antibiotics and
antiseptics until the pleural fluid culture results had been negative. Tube thoracostomy was ended
on day 16 after the lasting of air and fluid drainage. The patient is under follow up for six months
without any recurrence.
Discussion
Nasogastric tube insertions are a common procedure in the treatment and follow up of patients [1]. The insertion, evaluation of localization and convenience of NGT can be performed by medical
doctors and educated nurses [4]. Although it seems to be a simple procedure, it can cause mortal complications due to the malposition [2,3,5]. Delayed detection of
the complications worsens the situation. In the literature, different
methods and techniques are defined to avoid and decrease the
complications. The main methods offered are insufflation test, gastric
aspiration, capnometer, capnography and magnetic guidance [2,3].
Verification of the localization is very important after the
insertion NGT. The fastest and simplest method of this verification is
‘insufflation test’ which is composed of air insufflation and epigastric
auscultation [2,3]. pH level of gastric aspirate from the NGT is a
more accurate method [2]. Furthermore, chest X-ray is accepted as
‘gold standart’ to determine complications due to airway or thoracic
malposition [6]. Roubenoff and Ravich offered this two staged
method for insertion of NGT. Firstly, they push forward the NGT
30 cm blindly, then they improve the localization of the NGT in the
esophagus radiographically, finally they further insert the tube to
the optimal length of 50 cm and confirmed the localization with a
second X-ray [7]. Marderstein et al. [8] and coworkers performed this
method and reported that the incidence of pneumothorax after NGT
insertion was decreased from 0.38% to 0.09%. A few new methods
are described to avoid the malposition even so the performance of
traditional methods. Young and coworkers notified that in addition
to endoscopic and fluoroscopic based methods, a device with an
external sensor which produce real time signal for localization can
increase the success of NGT insertion [9]. Capnometer is another
confirmation method which has the highest sensitivity and specificity.
It can determine NGT malposition with the detection of CO2 [2,3].
In a study comparing NGT insertion methods, the success
of endoscopic methods used during insertion was reported as
95%. On the other side the success of blindly NGT insertion was
decreased through the level of 25% [10]. Rassias et al. [11] reported
the tracheopulmonary complication rate as 2% and mortality rate as
0.3% due to this complication in their prospective study including
740 intensive care unit patients undergone NGT insertion.
In conclusion, however NGT insertion is thought and seemed to
be a simple approach, by the consideration of its complications it must
not be accepted as so innocent. As the serious complications keep in
view, NGT insertion by well-experienced clinicians and confirmation
of localization is important for the avoidance of complications.
Figure 1
Figure 2
Figure3
References
- Hooker EA. Complications of gastrointestinal devices. In: Tintinalli JE, Kelen GD, Stapczynski JS, editors. Emergency Medicine: A Comprehensive Study Guide. New York, McGraw Hill. 2000:599.
- Pillai J B, Vegas A, Brister S. Thoracic complications of nasogastric tube: review of safe practice. Interact Cardiovasc Thorac Surg. 2005;4:429-33.
- Al Saif N, Hammodi A, Al-Azem MA, Al-Hubail R. Tension Pneumothorax and Subcutaneous Emphysema Complicating Insertion of Nasogastric Tube. Case Rep Crit Care. 2015;2015:690742.
- Boeykens K, Steeman E, Duysburgh I. Reliability of pH measurement and the auscultatory method to confirm the position of a nasogastric tube. Int J Nurs Stud. 2014;51(11):1427-33.
- Prabhakaran S, Doraiswamy VA, Nagaraja V, Cipolla J, Ofurum U, Evans DC, et al. Nasoenteric tube complications. Scand J Surg. 2012;101(3):147-55.
- Metheny N. Measures to test placement of nasogastric and nasointestinal feeding tubes: a review. Nurs Res. 1988;37(6):324-9.
- Roubenoff R, Ravich W. J. Pneumothorax due to nasogastric feeding tubes: report of four cases, review of the literature, and recommendations for prevention. Arch Intern Med. 1989;149:184–188.
- Marderstein EL, Simmons RL, Ochoa JB. Patient safety: effect of institutional protocols on adverse events related to feeding tube placement in the critically ill. J Am Coll Surg. 2004;199:39-47.
- Young RJ, Chapman MJ, Fraser R, Vozzo R, Chorley DP, Creed S. A novel technique for post-pyloric feeding tube placement in critically ill patients: a pilot study. Anaesth Intensive Care. 2005;33(2):229-34.
- Hernandez-Socorro CR, Marin J, Ruiz-Santana S, Santana L, Manzano JL. Bed side sonographic-guided versus blind nasoenteric feeding tube placement in critically ill patients. Crit Care Med 1996;24:1690-4.
- Rassias J, Ball PA, Corwin HL. A prospective study of tracheopulmonary complications associated with the placement of narrow-bore enteral feeding tubes. Crit Care. 1998;2:25-28.