Mini Review
Deep Intramuscular Left Anterior Descending (LAD) Artery: Implications for a Young Surgeon Performing Coronary Artery Bypass Surgery
Venkat R Machiraju* and Dhaval M Trivedi
Department of Cardiothoracic Surgery, University of Pittsburgh Medical Center, Pittsburgh, PA 15237, USA
*Corresponding author: Venkat R. Machiraju, Department of Cardiothoracic Surgery, University of Pittsburgh Medical Center, Pittsburgh, PA 15237, USA
Published: 07 Jun, 2017
Cite this article as: Machiraju VR, Trivedi DM. Deep
Intramuscular Left Anterior Descending
(LAD) Artery: Implications for a Young
Surgeon Performing Coronary Artery
Bypass Surgery. Clin Surg. 2017; 2:
1495.
Abstract
Dissecting out a deep intramuscular Left anterior descending coronary artery (DIMLAD) is one of the most difficult aspects of coronary artery bypass surgery. About 17-20% of the patients presenting for surgical revascularization have a deep lying LAD in the interventricular septum. Coronary artery bypass surgery (CABG) is the most commonly performed operation by the adult cardiac surgeon and is also generally performed by the junior most cardiac surgeon as they start their surgical practice. It is of concern that surgeons who do not have the surgical skill to dissect out a DIMLAD will perform their anastomosis in the distal segment of the LAD where it comes to the surface. In this location it can be of small caliber, be affected by atherosclerotic disease and pose technical difficulties due to its small size to perform a durable anastomosis.
Introduction
The LAD is the most common vessel bypassed at the time of CABG. The LAD, in the majority
of patients, lies deep in the epicardial fat and muscle in its proximal one third to one half and
courses to the epicardial surface thereafter. This more visible course in the distal one half to one
third is where most surgeons perform their anastomosis. The vessel here is of smaller caliber thereby
increasing the technical challenge of the anastomosis. Bypass is most commonly performed by
placing the distal left internal mammary artery to the LAD. The LAD is the most important blood
vessel that is commonly bypassed during surgical revascularization for ischemic coronary artery
disease. Sudden occlusion of LAD leading to acute myocardial infarction has a higher mortality than
occlusion of any other coronary artery branch in the setting of surgical revascularization. Similarly
acute occlusion or dissection of the proximal left anterior descending coronary artery during
percutaneous interventions can lead to major morbidity or mortality if not intervened immediately.
Survival benefit as well angina free life has been documented by Loop [1] in patients who have a
well functioning patent graft to the LAD. When such an artery is bypassed it is very essential to
perform the anastomosis at a place where the patency of the graft is assured consistently. Adams
et al. [2] described 21/169 patients in their study who required percutaneous intervention after
Coronary artery bypass surgery in the immediate post operative period in which 6 patients needed
intervention to the LAD.
Coronary arteries are generally in the subepicardial surface of the heart and so are easy to
see and perform a satisfactory anastomosis with a bypass conduit using either an artery or a vein
graft. However, patient’s general body habitus and female gender can predispose to excessive fatty
deposition on the heart making it difficult to identify the coronary artery branches. In addition,
pathologic studies have shown that some coronary artery branches are deeply embedded in the
muscular wall making it even more difficult to identify these branches during bypass surgery. Of
these vessels, the LAD is described to be located in a deep intramuscular location in about 21.7%
[3] of the cases either in the proximal or middle third of its course. The ramus intermedius, first
and second obtuse marginal branches are also commonly embedded in the lateral muscular
wall. At times, in their entire course without coming on to the surface. Similarly the distal right
coronary artery or the posterior descending coronary artery branch can be deeply embedded in
the atrioventricular groove or assume an intracavitary position making the search for these blood
vessels difficult. Surgeons on occasion cannot identify these vessels and left them non-revascularized
despite the known coronary stenosis.
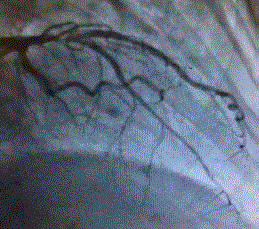
Figure 1
Figure 2
Anatomy of the Intramuscular LAD
The LAD can come directly from the left coronary sinus as a separate ostium or divide from left main trunk under the pulmonary artery along with the left circumflex artery. As it curves around the pulmonary artery it gives the first septal branch and it is at this location it starts diving into the interventricular septum and runs its course by giving additional branches into the septum and diagonal branches to the anterolateral wall. The intramuscular portion is generally straight instead of tortuous as we commonly see in the angiogram (Figure 1) and also varies in length between 0.5 cm to 3.7 cm and at a depth of 0.3 cm to 0.8 cm in the septum. Ferreira described superficial and deep varieties of intramuscular LAD. Superficial intramuscular LAD arteries are crossed by oblique muscle fibers while the deep type is crossed by transverse muscle fibers. In addition, a right ventricular type intramuscular LAD has been described which is very close to the endocardium and separated by a thin layer of endocardium from the right ventricular cavity. Surgeons have described getting into the right ventricular cavity while dissecting the intramuscular LAD because of close proximity. The myocardial bridge as it was described in the beginning was seen on the angiogram during systole as squeezing or milking a segment of the artery that is lying under the muscle.
Identifying the Intramuscular LAD
Surgeons have recognized that the segment of the LAD under the muscle is generally free of atherosclerosis and is of much larger caliber. Secondly as it comes to the surface distally, it is of much smaller caliber and is technically difficult to bypass. Graft patency is always better when the site of anastomosis is free of atherosclerosis and is of a larger caliber. As the LAD is deeply embedded in the septum surgeons have used different techniques to locate the vessel. It can take 20-30 mins to dissect out a DIMLAD, prolonging the cross clamp time. There is bleeding from the epicardial veins or the muscle itself. This bleeding may not be apparent while the aortic cross clamp is on but can become bothersome when the heart is reperfused and beating. Controlling the bleeding on a beating heart close to the graft anastomosis can create distortion of the graft and stricture at the anastomotic site. Secondly the vessel is so deep that performing an anastomosis with the internal thoracic artery was a surgical challenge that was only executed by experienced surgeons. Coronary artery bypass surgery is the most common operative procedure a young surgeon is allowed to perform in any surgical practice. Various techniques have been described by surgeons to identify the deep intramuscular LAD. These include retrograde dissection of the LAD from a distal visible portion, from a diagonal branch or passing a probe in the LAD retrograde [4]. Paruchuri and colleagues [5] described the technique of marsupialization of the DIMLAD using in 176 patients. Inadvertent entry into the right ventricle was described in two patients with this technique. More recent techniques involve intraoperative fluorescence angiography [6] and intraoperative cineangiography [7]. As valuable as it is to identify the segment of the LAD underneath the muscle for a better surgical anastomosis, it is not easy to learn the technique by looking at a video or see one or two cases during training. Surgeons typically follow a ‘groove sign’ (an epicardial groove seen directly in the pericardial fat over the LAD) and a ‘Vein sign’ (where the anterior cardiac vein lies directly over the DIMLAD). While these anatomic signs may bring the surgeon close to the LAD site, splitting the septal muscle over the LAD must be meticulous and in small segments (Figure 2). After locating the artery, the dissection of the septal muscle should be directly over the anterior and midline of the LAD that is visualized. Inadvertent entry into the right ventricle during OFF pump bypass while searching for the DIMLAD immediately forces the surgeon to initiate cardiopulmonary bypass to secure hemostasis. On occasion surgeons have had to take the LAD into the suture to control bleeding and subsequently performed the bypass distally. These anecdotal episodes keep young surgeons away from dissecting a DIMLAD and perform the anastomosis in the distal LAD. Surgeons, who hesitated to dissect out a DIMLAD, have anastomosed the LIMA graft to the distal LAD where they could identify it on the surface. Sometimes a vein graft extension was used as the mammary graft did not reach the distal LAD site of anastomosis. It is always ideal to bring the mammary pedicle through a slit in the pericardium as immediately gives additional length that is required. For fear of struggling to dissect out a DIMLAD, some surgeons routinely opted out to do a bypass distally on the LAD. Surgeons who developed the comfort of dissecting out the LAD from the intramuscular location have consistently provided better revascularization as this segment will provide good blood supply to a larger part of the myocardium including septum, anterior and anterolateral segments of the left ventricle.
Conclusion
Performing over 200 coronary artery bypasses each year over a thirty year period, I have encountered DIMLAD several times and recognized the value of dissecting and performing the anastomosis of the graft in the soft, non- atherosclerotic segment with a large caliber rather than a small distal vessel with atherosclerosis. One of the most difficult parts of coronary artery bypass surgery is to dissect out a deeply embedded intramuscular LAD without creating any technical mishaps. A surgeon who can do that not only prolongs the life of the patient but also gives the patient freedom from repeat cardiac interventions. The LIMA is most commonly used to bypass the LAD. 17%-20% of patients have an intramuscular course of the LAD raising significant technical challenges to performing a durable distal anastomosis, particularly using the LIMA which also diminishes in caliber in its distal portion. Lack of experience in dissecting the intramuscular LAD can lead to complications of right or left ventricular perforation during dissection while performing the anastomosis on a smaller caliber distal LAD can lead to graft failure due to technical complications.
References
- Loop FD. Internal-thoracic-artery grafts. Biologically better coronary arteries. N Engl J Med. 1996;334(4):263-5.
- Adams MR, Orford JL, Blake GJ, Wainstein MV, Byrne JG, Selwyn AP. Rescue Percutaneous Intervention Following Coronary Artery Bypass Graft- A Descriptive analysis of the changing Interface between Interventional cardiologist and Cardiac surgeon. Clin Cardiol. 2002;25(6):280-6.
- Vanker EA, Ajayi NO, Lazarus I, Satyapal KS. The Intramyocardial left anterior descending artery: prevalence and surgical considerations in Coronary artery bypass grafting. S Afr J Surg. 2014;52(1):18-21.
- Gandjbakhch I, Cabrol C. Technics for discovery of a masked interventricular artery in coronary surgery. Nouv Presse Med. 1976;5:2713-4.
- Paruchuri RV, Chattuparambil B, Hasabettu PK, Punnen J. Marsupialization of Intramyocardial Left anterior Descending Artery: A Novel Approach for Easy access During Revascualrization. Ann Thorac Surg. 2005;80(6):2390-2.
- Singh SK, Ihnken KA. Intraoperative fluorescence angiography to identify and confirm repair of intramyocardial left anterior descending coronary artery aneurysm. Ann Thorac Surg. 2010;90(4):e62.
- Aydin U, Kocogullari CU. A method for locating embedded left anterior descending coronary arteries. Ann Thorac Surg. 2013;95(1):360-1.