Case Report
An Interesting Periferic Artery Disease: Case Report
Haydar Yasa1*, Füruzan Aktuğ2 and Talat Tavlı3
1Department Cardiovascular Surgery, Batı Anadolu Central Hospital, Turkey
2Department of Anestesiology, Batı Anadolu Central Hospital, Turkey
3Department Anjiology and Cardiology, Batı Anadolu Central Hospital, Turkey
*Corresponding author: Haydar Yasa, Department Cardiovascular Surgery, Batı Anadolu Central Hospital Bayraklı-İzmir/Turkey
Published: 10 May, 2017
Cite this article as: Yasa H, Aktuğ F, Tavlı T. An Interesting
Periferic Artery Disease: Case Report.
Clin Surg. 2017; 2: 1468.
Abstract
A 56-year-old male patient with Fontaine stage II b, aortoiliac TASC II: Type B, the distal popliteal
lesions TASC II was considered Type C lesions. Ankle pressure of 60 mmHg and 40 mmHg great toe
pressure, transcutaneous oxygen partial pressure was 40 mmHg. Left lower extremities pulses those
manually (-). Ankle-brachial index ( ABI ) measurement; left to right, were found to be 0.9 to 0.4.
Peripheral angiography; Left E II – IIA's output was monitored over 90% plaque. In the proximal
third of the left popliteal artery segment is 100% occluded. Left common iliac arteries – common
femoral artery bypass was performed synthetic graft. Supragenual popliteal arteries infragenual
popliteal artery saphenous vein bypass was performed. Should not be sacrificed for the collateral
artery stenting or hybrid procedures, we believe that similar results can be obtained from open
surgery to perfectly.
Keywords: Stent; Hybrid; Arter; Open surgery
Introduction
Atherosclerotic peripheral artery disease most commonly involves superficial femoral arteries. However, their involvement in other regions is also monitored. Interestingly, superficial femoral artery was normal but only external iliac artery, popliteal artery and distal stenosis were observed in this study. This phenomenon is thought to be rare and it would be beneficial to be presented for the sake of success.
Case Presentation
A 56-year-old male patient was treated with DM Type 2 (+) for 10 years, 1 packet/day for 20
years and 50 m to 100 m. Intermittent cladication and cold and pallor complaints were present in
left lower extremities. Fontaine clasification was evaluated as Stage II b. Aortoiliac level TASC II:
Type B Popliteal distal lesion level was accepted as TASC II: Type C lesion. Absolute ankle pressure
was 60 mmHg, absolute large toe finger pressure was 40 mmHg, transcutaneous partial oxygen
pressure was 40 mmHg. Left lower limb pulses are manual (-).
Measurement of the ankle-brachial index (ABi); 0.9 for the right and 0.6 for the left. Peripheral
arterial lower extremity doppler: abdominal aorta calibration is normal. Right lower extremity
examination; main iliav artery, external iliac, superficial femoral, intimal thickening in popliteal
arteries and occasional plaque formation.
Left lower extremity doppler: The normal triphasic flow form has disappeared and a low speed
monophasic flow has occurred. There are similar changes in the proximal and middle segments of
the anterior and posterior tibial arteries as described above. Dorsalis pedis at the level of the ankle,
no flow in the anterior and posterior tibial arteries (complete occlusion). Coronary and aortic bifemoral
peripheral angiography was performed with these findings. LAD mid 40%, diagonal 2 40%
lesions were detected on coronary angiography. Coronary angiography was recommended.
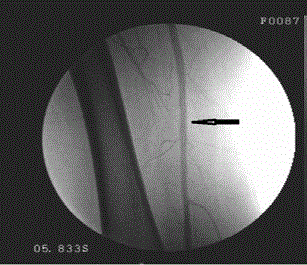
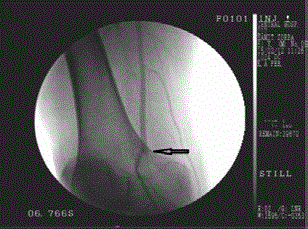
Distal abdominal aorta, right and left common iliac arteries (CIA) are atheromatous. Right
internal iliac artery (RİİA) and external iliac (EIA) are right EIA plate. In the left EIA, 90% of the
atheromatous plaque was observed at the exit of the IIA. Right and left common femoral artery
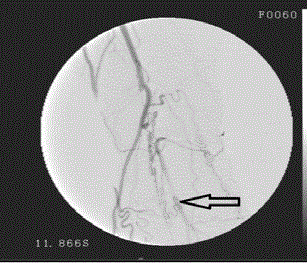
(CFA), arterial profunda femoris are atheromatous. Proximal 1/3 of the left popliteal arteries present
at 100% of the distal popliteal artery at the distal third of the occipital occlusion. (Figures 1-4).
Surgical Tecnique
In the presence of these findings, the patient was prepared for surgery. Routine blood tests were done. One gram of cefazolin sodium was administered as IV
for antibiotic prophylaxis before the procedure. The operation area
was disinfected with iodine and covered with sterile drape. Right
external iliac artery retroperitoneal oblique midi j incision was
reached. Other incisions were performed classically to achieve CFA,
superficial femoral artery, infragenual popliteal artery. At the same
time, about 15 cm long vena saffena magna was removed from the
right lower extremity. Grafts were passed through the tunnels. The
arterial structures were returned with vascular tape and all patients
before the cross clamping were administered IV 5000 units heparin
bolus. Polypropylene suture of 5-6/0 was used for anastomoses. Left
common iliac artery – common femoral artery was bypassed with 8
mm ring graft. Superficial femoral artery was evaluated as normal.
Supragenital popliteal artery – infragenital popliteal artery bypass
bypass was performed.
After completion of the anastomoses, the x-clamp was removed
and air was removed from the graft, and the operation was terminated
by closing the grafts appropriately.
There is a cladicatio intermittant repair near the postoperative 3rd
month follow-up and manual distal trauma can be taken. ABI 0.9,
absolute ankle pressure 90 mmHg, absolute large head finger pressure
80 mmHg.
Figure 1
Figure 2
Figure 3
Figure 4
Discussion
Atherosclerotic peripheral arterial disease affects approximately 10% of men over 65 years of age. This rate is up to 20% in women and men over 75 years of age [1]. Peripheral artery disease continues to be an important health problem with the cause of this occurrence. It is the most common and most important cause of mortality and morbidity in the community. There have been significant increases in percutaneous stenting procedures in recent years. There are authors in the TASC classification who recommend percutaneous stents even in Type A, B, C or even D group [2-4]. However, one of the most important points to be considered in the stenting procedure is the risk of stenosis of the collateral arteries. As in this case, although the lesion in the proximal to the EIA is TASC Type A, percutaneous stenting is not preferred due to the risk of internal iliac artery occlusion (Figure 1). The occlusion in the distal popliteal artery was close to perfection with the use of a stent on the same side as the stent was not preferred due to the correspondence to the knee joint (Figure 3). Again, hybridization is not preferred for the same reasons. Open surgery was performed at the first postoperative month and the results were close to normal in the distal intermittent manual (+), ABI 0.9 and absolute ankle and absolute toe thumb systolic pressures. Another debate concerns the use of autogenous grafts. In infragenic bypass, autologous safen ven- tine has higher rates of short- and long-term patency [5]. The benefits of safen ven graft include foldability, resistance to infection, less thrombogenicity, suitability for manipulation, long-term viability, diffusion feeding, ease of use, and more economical [5,6]. At the same time, we believe the use of autologous grafts would be appropriate. Incisions are made for arterial access and autogenous grafts can be prepared with very short additional incisions. In this respect, contralateral extremity injuries are avoided postoperatively and the possibility of limb use emerges. The most frequent site of atherosclerotic obstruction was the superficial femoral arterial segment. The incidence was 25.8% in femoral, 22.1% in Peroneal, 10.1% in Post Tibial, 16.1% in Anteriortibial, 19.8% in Popliteal, 5.4.2% in Iliac arteries. Superficial femoral arterial involvement SFA was normal and stenosis in the popliteal artery and external iliac artery was observed in this case. Hybrid interventions and percutaneous stenting procedures in peripheral arterial disease are increasingly in the midst of treatment. However, in cases where stent or hybrid intervention is not possible, surgery can be performed very successfully. As a result, we think that collateral arteries should not be sacrificed for stenting or hybrid intervention, and that open surgery may achieve close results.
References
- Criqui MH, Fronek A, Barrett-Conner E, Klauber MR, Gabriel S, Goodman D. The prevalance of peripheral arterial disease in a defined population. Circulation. 1985; 71: 510-515.
- TransAtlantic Intersociety Consensus (TASC) Worcing Group: Management of peripheral arterial disease. Vasc Surg. 2000; 31: 1-296.
- Rooke TW, Hirsch AT, MisraS, Sidawy AN, Beckman JA, Findeiss LK, et al. 2011ACCF/AHA Focused Update of the Guideline for the Management of Patients With Peripheral Artery Disease(updating the 2005guideline): a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2011; 58: 2020-2045.
- Jeffrey LA, Jonathan LH, Nancy A, Biykem B, Ralph GB, Lesley HC. Management of patients with peripheral artery disease (Compilation of 2005 and 2011 ACCF/AHA Guideline Recommendations): A report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Am Coll Cardiol. 2013; 61: 1555-1570.
- Klinkert P, Post PN, Breslau PJ, van Bockel JH. Saphenous vein versus PTFE for above-knee femoropopliteal bypass. A review of the literature. Eur J Vasc Endovasc Surg. 2004; 27: 357-362.
- Falco E, Celoria G, Nardini A, Saccomanno G, De Franchi G, Zappia F, et al. Femoro-popliteal bypass with reversed saphenous vein. Experience in a General Surgery Department. Minerva Chir 1995; 50: 883-888.