Research Article
Laparoscopic Lich Gregoir Extravesical Ureteric Reimplantation for Correction of High Grade Vesicoureteric Reflux- Short, Intermediate and Long Term Outcomes with Literature Review
Krishanu Das*, George P Abraham, Krishnamohan Ramaswami, Datson George P, Jisha J Abraham, Thomas Thachill and Thampan OS
Department of Urology, Lakeshore Hospital, India
*Corresponding author: Krishanu Das, Department of urology, Lakeshore Hospital, NH 47 Bye Pass Maradu Nettoor P.O. 682040, Kochi, India
Published: 01 May, 2017
Cite this article as: Das K, Abraham GP, Ramaswami
K, Datson George P, Abraham JJ,
Thachill T, Thampan OS. Laparoscopic
Lich Gregoir Extravesical Ureteric
Reimplantation for Correction of High
Grade Vesicoureteric Reflux- Short,
Intermediate and Long Term Outcomes
with Literature Review. Clin Surg. 2017;
2: 1456.
Abstract
Objective: To assess the efficacy of laparoscopic Lich-Gregoir antireflux surgery in management of
Grade III-V vesicoureteric reflux.
Methods: Patients with bothersome urinary infection and high grade vesicoureteric reflux (grades
III-V) were recruited for the procedure. All patients were worked up in detail. Pre-procedure
cystoscopy was performed with placement of ureteral stent and a perurethral catheter. Ureteric
reimplantation was performed following Lich-Gregoir principle. Voiding cystogram and ultrasound
were evaluated 6 monthly.
Results: From August 2009 till June 2012, 36 patients (68 renal units — 30 bilateral, 4 unilateral and
2 common sheath reimplantations) underwent laparoscopic antireflux surgery. Preoperative reflux
grades were 32 Grade III, 24 Grade IV and Grade V in 12. Mean operation duration was 103.33 min
for unilateral and 154.09 min for bilateral antireflux procedure. A difference in operation duration
between male and female children was perceived (115 min vs. 165 min, p< 0.001). No major
intraoperative events were encountered. Postoperatively 3 patients complained of vague abdominal
pain. Mean hospital stay was 2.5 days. 3 patients complained of voiding dysfunction after catheter
removal. 30 children (60 renal units) attended 3 year follow-up. Complete resolution of VUR was
noted in 30 Grade III (100%), 21 Grade IV (95.45%) and 9 Grade V (75%) units. Overall reflux
resolution rate was 93.75%.
Conclusion: Laparoscopic Lich-Gregoir type of antireflux procedure offers satisfactory outcome in
management of high grade VUR. Children with Grade V VUR may benefit from ureteral tapering
prior to antireflux construction.
Keywords: Vesico; Ureteric reflux; Laparoscopy; Antireflux surgery
Introduction
Vesicoureteric reflux (VUR) is a perplexing urological problem that may culminate in
nephropathy, scarring and ultimately renal failure [1-3]. Definitive treatment of VUR is based on
grades of severity and clinical presentation. Although Grades I and II VUR occasionally resolve
spontaneously on long term antibiotic prophylaxis and expectant management [2], high grade
reflux often requires early intervention to prevent upper tract deterioration [4,5]. Despite the success
of endoscopic treatment [6,7], surgical treatment remains the gold standard treatment option for
managing high grade reflux. Several surgical techniques are available for correction of reflux [8].
Conventionally, these exercises are conducted through open approach. Laparoscopic approach for
antireflux construction is evolving. In the limited citations published till date, this approach has
been appraised to achieve the same feat as incisional techniques with palpable benefits and fewer
shortcomings [9]. We bring forth our experience with this operative exercise in our patient cohort.
Materials and Methods
A retrospective analysis was conducted including patients who were treated by our team
between August 2009 and June 2012. Study was approved by institutional review board. Children
were recruited from both emergency department and outpatient clinics. All children attending with pyrexia and a documented urinary infection were evaluated in detail, including complete blood exam, renal function, urinalysis, ultrasound
scan (US) to check for renal anatomy and scars, and a voiding
cystourethrogram (VCUG) to check for VUR. Children with VUR
underwent further assessment to rule out coexisting malformations
or secondary pathologies contributing to reflux. Symptomatic
children with low grade reflux (Grade I and II) were offered Deflux
injections. Patients with high grade reflux and renal scarring in US
underwent dimercaptosuccinic acid (DMSA) renogram to assess
renal function. Symptomatic patients with recurrent UTI (≥ 1
episode of documented urinary infection despite being on antibiotic
prophylaxis), Grade III-V VUR, with or without renal scars and
with salvageable renal unit were offered antireflux surgery and those
consenting to laparoscopic approach comprised the study cohort. All
procedures were performed under general anaesthesia with single
dose of parenteral antibiotic at induction. First, urethrocystoscopy
was performed to define trigonal anatomy and location of the ureteric
orifice, the appearance of the orifice, the submucous length of the
intravesical ureter and rule out any secondary pathology contributory
to reflux. Unilateral or bilateral double J ureteral stents (Rusch;
Germany, 3F in children ≤ 5 years age and 4.8F in children >5 years)
were inserted depending on laterality of reflux. Per urethral cathere
was inserted and children were positioned 45 degree Trendelenberg
with shoulder support and padding of pressure points. In unilateral
procedures the pathological side was tilted upwards by 20 degrees.
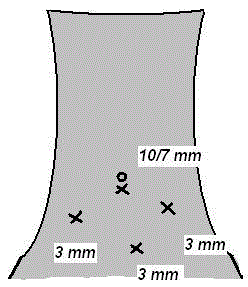
Four ports were employed, a 7 mm camera port, and three, 3 mm
working ports (two ports at left and right iliac fossa along midclavicular
line for dissection and suturing and one at midline suprapubic level
for retraction) (Figure 1). Pneumoperitoneum was created using
Hassan technique. A transperitoneal approach was employed in all
cases. After familiarising with the anatomy, the pathological ureter
was identified at the level of pelvic brim and dissected till the level of
ureterovesical junction using blunt and sharp dissection. The presence
of stent facilitated the identification of the ureter especially when
grossly dilated. During ureteral mobilisation use of electrocautery
was restricted strictly and 4 mm to 5 mm of periureteral adventitia
was preserved. Subsequently, urinary bladder was filled through
the preinserted per-urethral catheter with 100 mm to 200 mm of
normal saline depending on age and bladder capacity of the child
(0.91% weight/volume, 300 mM/L, Fresenius Kabi, Germany).
The peritoneum overlying the bladder was incised followed by
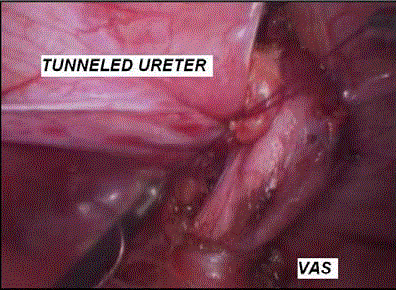
seromuscular cystotomy. The most important structure encountered
in the vicinity during this step was the vas deferens in males and
uterine artery and adnexal structures in females. These structures
were meticlously mobilised and preserved. Thereafter, extramucosal
detrusor trough was created by suburothelial undermining (Figure
2). A wide trough of 4 cm to 5 cm length was created using hook
electrocautery. Any accidental breach of the bladder mucosa during
this step was sutured. At the level of ureterovesical junction, the
myotomy was extended on either side of the ureteric insertion
in an inverted Y fashion. The ureter was thereafter directed in the
trough and detrusor approximation undertaken with 3-0 polyglactin
sutures (Vicryl; Ethicon, Johnson and Johnson) on a 30 mm 3/8 circle
needle. We usually employed three equidistant sutures taking care
not to overangulate or overcompress the ureter (Figure 3). Adequate
tension was maintained during detrusorraphy. In duplex moiety
with lower moiety ureterocele, the ureterocele was incised during
cystoscopy; ureteral stents were inserted in each moiety, followed
by laparoscopic common sheath reimplantation. In all patients an
abdomanl drain was placed after completion of antireflux and drain
was kept without suction. Post surgery oral intake was resumed when
children were comfortable. Catheter was removed next postoperative
day. Children were sent home once fully ambulatory with adequate
oral intake and satisfactory voiding. Paracetamol as analgesic was
advised only on demand. The ureteral stents were removed after six
weeks. All patients were reassessed three monthly with complete
clinical evaluation, renal parameters, urinalysis and ultrasound scan.
Estimated GFR (EGFR) was calculated using Schwartz formula [10].
Preoperative and postoperative EGFR values were compared. A
repeat VCUG was interpreted at six months following the procedure.
Complete resolution of reflux in follow-up VCUG and improvement
in pelvicaliceal dilatation in US was remarked as treatment success.
Downgrading or persistence of same grade of VUR was inferred as
unsatisfactory outcome and symptomatic patients were rendered
alternative corrective options. Those with successful reflux resolution
were re-evaluated at three years and five years. Statistical analysis was
conducted using descriptive statistics, T test and Wilcoxon signedrank
test. A p value < 0.05 was considered statistically significant.
Table 1
Figure 1
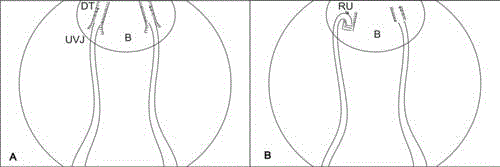
Figure 2
Figure 2
Sketch of surgical principle.
B: Urinary Bladder; DT: Detrusor Trough; RU: Reimplanted Ureter; UVJ:
Ureterovesical Junction
Figure 3
Results
Thirtysix children (30 bilateral, four unilateral and two common sheath reimplantations, total 68 renal units) with primary VUR underwent laparoscopic reflux correction. The severity of reflux was Grade III VUR in 32 units, Grade IV VUR in 24 units and Grade V VUR in 12 units. Three children underwent antireflux correction in solitary functioning renal unit. The contralateral unit was dysplastic (n=2) or nonfunctioning secondary to high grade reflux (n=1) and laparoscopic nephrouereterctomy was performed for the contralateral unit. All other children had bilateral functioning renal units. Table 1 projects the statistical analysis of our patient cohort. Mean age was 6.1 years. Twenty one children were male and 15 were females. The average number of UTIs experienced prior to study recruitment were 4.2 and all children had at least one febrile UTI. All children were on antibiotics. No children in this cohort received endoscopic injections prior to laparoscopic surgery. Preoperative renal function was normal in all children. Mean surgical duration was 103.3 min for unilateral and 154.1 min for bilateral antireflux procedure. The operation duration was longer in female children (165 min in female and 115 min in males, p< 0.001). In two patients, minimal breach of the bladder mucosa occurred during suburothelial undermining of the detrusor. However, antireflux surgery could be completed using laparoscopy approach. In the post-operative period, three children complained of vague abdominal pain that settled with anticholinergic medications. All patients had per urethral catheter removed on first postoperative day. No children experienced any urine leak postoperatively. Three children experienced transient voiding dysfunction after catheter removal that was managed by short period of reinsertion of per urethral catheter (one week) and anticholinergics. One child presented with persistent hydronephrosis after stent removal and was managed by reinsertion of ureteric stent. Three months later this stent was removed after resolution of the hydronephrosis. All children complied with the first year follow-up schedule. Symptomatic improvement was appraised in all but two children. Both continued to experience recurrent urinary infections post surgery. No children reported decline in renal function. Improvement was observed in the mean follow-up serum creatinine, albeit not statistically significant (preoperative 0.94 mg/ dl vs. postoperative 0.76 mg/dl, p=1.012). There was significant improvement in the mean follow-up EGFR values (preoperative 65.3 ml/min/1.73 m2 vs. postoperative 74.87 ml/min/1.73 m2, p< 0.001). At one year, complete resolution of VUR was noted in 32 children (60 renal units, 30 units with Grade III VUR (100%), 21 units with Grade IV VUR (95.5%) and 9 units with Grade V VUR (75%). Overall reflux resolution rate was 93.8%. Amongst the four units with persistent VUR, downgrading of VUR was noted in all. One unit showed Grade I VUR and three units Grade II VUR. All these children had bilateral VUR at presentation and underwent simultaneous bilateral reconstructions. Two children were stable clinically during followups and were observed. In other two children with Grade II reflux and urinary tract infection, symptoms resolved after Deflux injection. Thirty children (29 bilateral and 2 unilateral VUR, 60 renal units, 26 Grade III, 22 Grade IV and 12 Grade V) attended three year follow-up. Twenty one children (40 units, 25 children with Grade III, 12 children with Grade IV and three children with Grade V VUR) attended five year follow-up. Clinical and radiological parameters were stable in all of them with no further episodes of UTI and no recurrence of VUR.
Discussion
VUR is a common problem in childhood, affecting about 1% of all children and up to 25% to 40% of those presenting with acute pyelonephritis [11]. Secondary VUR mandates treatment of the contributory pathology, whereas primary reflux requires correction of the dysfunctional vesicoureteric junction. Endoscopic injections are often utilized for managing low grade reflux that is non-respondent to observation (Grade I and II). But their efficacy in managing Grade III-V reflux is not yet convincing [4-6]. Surgical management remains the most preferred approach for addressing these cases. An armamentarium of surgical techniques has been in vogue for reflux correction, both through transvesical and extravesical routes [12-15]. The basic principles of all these techniques is adequate mobilisation of the ureter preserving its vascularity, creating a trough in the bladder wall that is wide enough to accommodate an optimal length of the lower ureter and buttressing the implanted ureter with generous detrusor muscle support. Conventionally, these surgeries have been performed with open approach. With increasing expertise in laparoscopic surgery, many of these techniques have been successfully replicated laparoscopically [16,17]. Although the preference lies with the treating surgeon’s expertise and experience, extravesical approaches are reportedly associated with lower morbidity and shorter hospital stay than intravesical techniques [18]. This is attributed to minimal handling of the ureter and preservation of bladder mucosal integrity. Laparoscopy additionally benefits the surgeon due to magnification achieved and surgical exercise can be conducted with precision. In our cohort, all procedures could be successfully accomplished via laparoscopic approach. The morbidity profile associated with laparoscopy is appealing. The morbidity profile experienced in our group was minimal and confer to the published standards [9,16,17]. Laparoscopic approach for correction of reflux can be technically challenging [9,19,20]. The operator needs to be versed with advanced laparoscopic techniques, have a thorough knowledge of pelvic anatomy, the skill to operate in the limited pelvic space in children along with expertise in intracorporeal suturing. Adhering to the principles of reconstruction, we created a wide detrusor trough in all cases, thereby maintaining the ureteral diameter to the detrusor trough length ratio. Additionally, full thickness of detrusor muscle was preserved to enable buttressing with adequate tension on the implanted ureter. These can be considerably demanding to achieve in grossly dilated ureters in cases of Grade V reflux. Buttressing with excessive tension has the potential to jeopardize antegrade ureteric peristalsis and pelvicaliceal drainage whereas suboptimal tension runs the risk of persistent reflux along the tunneled ureter. Another point of caution with the extravesical approach is the possibility of iatrogenic injury to the vas deferens in males or adnexal structures in females during mobilization of the lower ureter near the vesicoureteric junction. These structures are encountered in the immediate vicinity of the vesicoureteric junction and were meticulously preserved in all. In our series, the procedure was easier to perform in males. The vas deferens is less bulkier than the adnexal structures and uterine vessels in female children, and was easier to mobilize and preserve. This could explain the observed difference in the operative duration between male and female children. A success rate of 90% to 99% has quoted for open extravesical repairs [21-24]. Proponents of laparoscopic approach also claim good results in these cases [9]. We observed an overall success rate of 94% in our cohort. Scrutinizing our results, we found that children with delayed presentation to surgery from onset of symptoms (mean interval of 48 months) and high grade reflux with grossly dilated ureters at presentation (Grade V VUR) had suboptimal outcome. Additionally, the failed cases belonged to the early part of the series. It is probable that lack of sufficient experience with the technique in the initial part of the series and suboptimal tension in the suture line may be contributory. We strongly believe there is a learning curve in this technique. Also when faced with grossly dilated ureters, tapering the ureteral circumference by tailoring prior to reimplantation may be worthy. A concern with extravesical approaches, especially in bilateral pathologies is postoperative voiding inefficiency [21-25]. We encountered this problem in the initial 3 cases which was managed with short period of recatheterisation. A nerve sparing approach has also been described to overcome this problem [26]. However we did not practice such technique in any of our patients. Some authors have highlighted the importance of an inverted Y shaped detrusor myotomy for creation of detrusor trough [9,27]. We also support this concept and consider it crucial for success. The bifurcating limbs of the Y should be wide enough to allow placement of the ureter in the trough without causing overangulation and thereby preventing subsequent impairment of upper tract drainage. Laparoscopic extravesical antireflux is considered less technically exacting than other laparoscopic transvesical techniques with comparable results [26]. We did not practice transvesical approach in any of our patients and hence unable to comment on the relative merits of our technique over the transvesical approach. A significant proportion of children in our study benefitted from laparoscopic antireflux procedure. This approach should certainly be utilized widely for addressing high grade reflux.
Conclusion
Laparoscopic extravesical ureteric reimplantation is an effective surgical option for management of high grade vesicoureteric reflux, with minimal morbidity and comparable outcome to other surgical approaches for this pathology. Children with Grade V reflux may benefit from tapering of the ureter prior to antireflux creation.
Acknowledgements
Mr. Sooraj Rajsekharan for the statistics used in the study.
References
- Olbing H, Claësson I, Ebel KD, Seppänen U, Smellie JM, Tamminen-Möbius T, et al. Renal scars and parenchymal thinning in children with vesicoureteral reflux: a 5-year report of the International Reflux Study in Children (European branch). J Urol. 1992;148(5):1653-6.
- Decter RM. Update on vesicoureteral reflux: pathogenesis, nephropathy, and management. Rev Urol. 2001;3(4):172-8.
- Bernstein J, Arant BS Jr. Morphological characteristics of segmental renal scarring in vesicoureteral reflux. J Urol. 1992;148:1712-4.
- Medical versus surgical treatment of primary vesicoureteral reflux. Report of the International Reflux Study Committee. Pediatrics. 1981;67(3):392-400.
- Weiss R, Duckett J, Spitzer A. Results of a randomized clinical trial of medical versus surgical management of infants and children with grades III and IV primary vesicoureteral reflux (United States). The International Reflux Study in children. J Urol. 1992;148:1667-73.
- Mevorach RA, Hulbert WC, Rabinowitz R, Kennedy WA, Kogan BA, Kryger JV, et al. Results of a 2-year multicenter trial of endoscopic treatment of vesicoureteral reflux with synthetic calcium hydroxyapatite. J Urol. 2006;175(1):288-91.
- Läckgren G. Endoscopic treatment of vesicoureteral reflux: Current status. Indian J Urol. 2009;25(1):34-9.
- Greenfield SP. Vesicoureteral reflux--current treatment options. Expert Opin Pharmacother. 2003;4(11):1959-66.
- Yegappan L, Leo CTF. Laparoscopic Extravesicular Ureteral Reimplantation for Vesicoureteral Reflux: Recent Technical Advances. J Endourology. 2000;14(7):589-94.
- Schwartz GJ, Haycock GB, Edelmann CM Jr, Spitzer A. A simple estimate of glomerular filtration rate in children derived from body length and plasma creatinine. Pediatrics. 1976;58(2):259-63.
- Walker RD, Duckett JW, Bartone FF, McLin PH, Richard GA. Screening schoolchildren for urologic disease. Birth Defects Orig Artic Ser. 1977;13(5):399-407.
- Politano VA, Leadbetter WF. An operative technique for the correction of vesicoureteral reflux. J Urol. 1958;79(6):932-41.
- Cohen SJ. Ureterocystostomy: A new antireflux technique. Akt Urol. 1975;6:1-5.
- Glenn JF, Anderson EE. Distal tunnel ureteral reimplantation. J Urol. 1967;97(4):623-6.
- Zaontz MR, Maisels M, Sugar EC, Firlit CF. Detrusorrhaphy: extravesical ureteral advancement to correct vesicoureteral reflux in children. J Urol. 1987;138:947-9.
- Chen HW, Lin GJ, Lai CH, Chu SH, Chuang CK. Minimally invasive extravesical ureteral reimplantation for vesicoureteral reflux. J Urol. 2002;167(4):1821-3.
- Gill IS, Ponsky LE, Desai M, Kay R, Ross JH. Laparoscopic cross-trigonal Cohen ureteroneocystostomy: novel technique. J Urol. 2001;166(5):1811-4.
- Chen HW, Yuan SSF, Lin CJ. Ureteral reimplantation for Vesicoureteral Reflux: Comparison of Minimally Invasive Extravesical with Transvesical and Conventional Extravesical Techniques. Urology. 2004;63(2):364-7.