Research Article
Choices of Food after Total Laryngectomy
Cheerasook Chongkolwattana1*, CDR Pachrin Chanpresit2 and Preyanuj Yamwong3
1Department of Otorhinolaryngology, Mahidol University, Thailand
2Somdech Phra Pinklao Hospital, Thailand
3Department of Medicine, Mahidol University, Thailand
*Corresponding author: Cheerasook Chongkolwattana, Department of Otorhinolaryngology, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok 10700, Thailand
Published: 26 Apr, 2017
Cite this article as: Chongkolwattana C, Pachrin Chanpresit
CDR, Yamwong P. Choices of Food
after Total Laryngectomy. Clin Surg.
2017; 2: 1438.
Abstract
Background: Management of laryngeal cancer by total laryngectomy resulted in alteration of
pharyngeal anatomy and physiology and with combined radiation makes it more difficult for food
bolus to pass through pharynx and upper esophagus. The purpose of this study is to identify the
choice of Thai food, which has variety of texture that laryngectomies could eat at different period of
treatment. Ability to eat chili hot food is also studied.
Method: Prospective comparison choice of food types is done from preoperative and to 1,3 and 6
months post-operative period using questionnaire. Thai food were classified by texture into 7 types
as clear liquid, thick liquid, soft, semisolid, sticky, hard, and hard and dry food. Ability to eat chili
hot food is compared between preoperative period and at 6 months after operation.
Results: Seventeen patients with uncomplicated total laryngectomy were enrolled. The patients
could eat type 1-3 food (clear liquid, thick liquid and soft food) well at all time. For the rest of food
types, the laryngectomies had more difficulty eating them. Sticky food is the most difficult to eat
after total laryngectomy and radiation. Both hard food and hard and dry food were difficult for the
patients but less than sticky food. The worst time of eating difficulty was at 3 months. At 6 months
after surgery, 76.5% of patients who could eat semisolid food, which is the common food in daily life,
without difficulties. This was the same as before treatment. Patients who could not eat sticky food,
hard food and hard and dry food at all were 52.95%, 29.4% and 41.2% respectively. Approximately
half of the patients (9/17) could eat hot food at 6 months after the operation although all of them
could eat it before having cancer.
Conclusion: The result can be used for preoperative counseling on possible types of food at different
period of treatment. To improve the eating satisfaction and life quality, the patients should be
instructed to try all types of food, especially after complete healing from surgery and radiation.
Keywords: Thai food types; Choices of food; Total laryngectomy
Introduction
Management of laryngeal cancer by total laryngectomy although successful in curing the
diseases but the alteration of pharyngeal and laryngeal anatomy can affect eating and swallowing
physiology of the patients. Eating is not only bringing energy sources for lives, but also giving people
the pleasure of living. Questions about swallowing and eating ability have been part of many quality
of life assessments. The purpose of this study is to evaluate the reality of eating status after total
laryngectomy especially with Thai food.
In normal pharyngeal phase of swallowing, the tongue pushes backward and downward.
Constrictor muscles start contraction. The larynx is closed and pulled upward and forward by many
muscles connected to hyoid bone. Laryngeal closure not only prevents aspiration but also create
subglottic pressure to help driving food. Upward and forward laryngeal movement create retroflex
movement of epiglottis, protecting the airway while food sliding from vallecular to pyriform sinus
and then esophagus. This movement also increases a space between cricoid and vertebrae, creating
slight negative pressure and also help pulling open the cricopharyngeaus muscle or upper esophageal
sphincter. With all these mechanisms together, the food will easily pass pharynx to esophagus. The
esophagus moves in peristalsis manner to move the food downward. It also needs to expand and
contract when the food passing through it.
In total laryngectomy (TLG), the trachea is anteriorly fixed and opened to the neck and the
positive pressure at subglottis is loss. Larynx and hyoid are removed which resulted in absence of hyolaryngeal elevation and the mechanism to pull open the cricopharyngeus [1,2]. The negative pressure to pull the food into
esophagus is also lost. McConnel [3] found that higher tongue base to
posterior pharyngeal wall pressures are required after laryngectomy to
propel a bolus through the collapsed pharynx. Choi “et al.” [4] Studied
upper esophageal sphincter (UES) in post TLG patients comparing to
normal and found decreasing resting pressure, maximum contracting
pressure, degree of relaxation and coordination of sphincter
movement and length of sphincter had reduced. The proximal part
of esophageal body had decreased maximum contraction pressure,
contraction time and peristaltic wave propagation with statistical
significance. There is no different of lower esophageal function
between post TLG and normal. Duranceu “et al.” [5] found functional
change of upper esophageal sphincter and body of esophagus in all 10
TLG patients in their study, 5 of which complained dysphagia. Both
Choi and Duranceu found normal function of lower sphincter.
TLG can be used as a primary or secondary surgical treatment for
laryngeal cancer. When indicated for a primary, untreated tumor, it
is usually for advanced stage of cancer. It is almost always follows by
postoperative radiation. Radiation can damaged salivary and mucous
gland and also cause fibrosis. These reduce and thicken saliva, limit
muscle contraction and limit esophageal expansion. Combination of
Surgery and radiation makes it more difficult for food bolus to pass
through pharynx and upper esophagus. Sense of smell which was
reduced by redirection of inspiratory airflow not passing the nose
and some effect of chemotherapy can cause alteration of taste. The
patients tend to have swallowing difficulty, taste alteration and less
apatite.
Thai food is worldwide popular for its balance combination of
taste including sour, sweet, salty, bitter and also its hotness. Many
kinds of spices give “heat” or hotness to Thai food, but the most
prominent is from chili which contains capsaicin. Although capsaicin
can reduce appetite and energy intake in non-users [6], it adds food
flavor to regular users and tend to increase appetite.
There are also many kinds of Thai foods, with not only variety of
taste but also texture. Variation of Thai food’s taste and texture can be
used as representative of many Asian foods. Some people, also health
care personnel’s still believe that hot food or hard food is not suitable
for sick people, cancer patients or post radiation and try to restrict
types of food for patients. Long term intake of bland and soft diet
tends to decrease appetite which may result in decrease food intake
and quality of life.
It is our purpose to study the choices of food and eating ability of
laryngectomees on different types of common food in Thailand and
also on chilli hot food. The type of food that the patients choose during
the different postoperative periods and what final type of food that
patients were comfortable to eat at the end of 6 months after surgery
comparing to their preoperative food. We also study the ability to eat
chili hot food. The result can help surgeons and care team for realistic
preoperative counseling and also help patients and families to prepare
better food to fit the patients’ ability and satisfaction.
Study design
The design is a prospective comparison of pre- and post-surgery
eating ability, using questionnaire on choices of food. The study had
been approved by Siriraj Institutional Review Board (SIRB), Faculty
of Medicine Siriraj Hospital, Mahidol University.
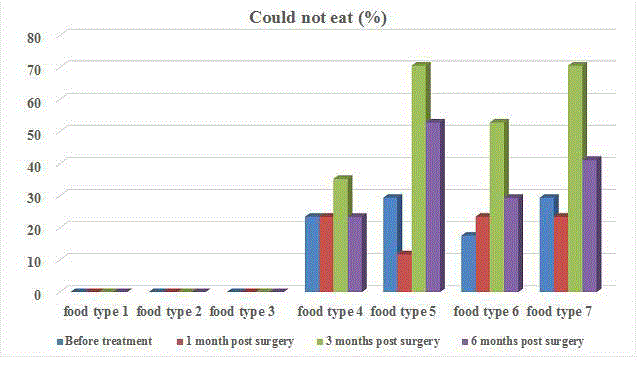
Figure 1
Figure 1
Percentage of patients who could not eat comparing 7 types of
food and timing from before operation to 1, 3 and 6 months after surgery.
Table 1
Materials and Methods
Questionnaire on choice of food and eating ability had been done
on TLG patients at Dept. of Otorhinolaryngology, Siriraj Hospital,
Mahidol University, and Bangkok, Thailand from July 2003-
September 2004. The patients complete the questionnaire before
surgery and at 1, 3 and 6 months after completion of Surgery. Patients
with flap reconstruction, recurrence diseases after treatment, history
of pharyngocutaneous fistula, and medical condition that affect
swallowing such as cerebrovascular diseases were excluded from
the study. In our hospital, the mucosa of hypopharynx is preserved
in all cases of laryngeal cancer. In case of hypopharyngeal cancer
primary closure is done if one side of pyriform mucosa is preserved
and pharyngeal mucosal is wider than 5 cm relaxed. Pharyngeal
closure is usually done in T-shaped closure or transverse if there is
minimal tension. The cricopharyngeus muscle is usually not sutured
approximation on the front of the mucosal suture.
The Thai therapeutic food are classified into food type no 1- 5
(Table 1) [7] The food type no 5-7 are classified by authors in order to
separate into more detail of hard and sticky food. Totally there 7 types
of Thai food depending on texture and examples of real food in each
type are shown in (Table 1).
The laryngeal cancer patients were instructed about food types
and examples of them. They were persuaded to eat all types of food
that they felt comfortable. For types 4-7, we suggested the patients to
start with small amount, chew properly, eat slowly and sip enough
water. They are instructed that they can eat chili hot food when they
felt stable after treatment and no radiation mucositis. They should started with less hot and increase hotness later to the extent that they
were comfortable and satisfied.
The questionnaire was designed by authors to evaluate whether
patients can eat each type of food or not and is there any difficulty
during eating. The questionnaire also gave the real names of food in
each type to make sure that the patients understand the exact type of
food.
Table 2
Results
Initially, there were 25 patients enrolled in the study. During the
follow up period, 2 had local recurrence, 2 had distant metastasis, 1
died of other disease and 3 were lost to follow up. Only 17 patients
had complete data and inclusion criteria for analysis. They were all
male, age range from 38 to 76 years (mean 68.28 years). One patient
did not smoked, while the rest smoke more than 10 packs year (Figure
1).
Among 17 patients, 13 patients (76.5%) has tranglottic cancer,
1 (5.9%) had primary subglottic cancer and 3 (17.6%) has pyriform
sinus cancer. Twenty nine point five percent had stage III and 70.6
% had stage VI cancer. Type of operation is shows in (Table 2). All
the patients in this study had primary total laryngectomy as those
who had secondary or salvage surgery in the same study period had
either fistula or flap reconstruction and were excluded from the study.
All patients did not need NG tube feeding before the operation and
NG was able to be removed before 1 month. All patients received
postoperative radiation of 6000 cGy after the operation except 2
patients who received 4000cGY and 5000cGy due to complications.
The radiation started at 4-6 weeks after the operation and finished
before 3 months. At 6 months after the operation, all wounds heal
well, there was no effect of radiation such as mucositis and all patients
were in stable conditions.
Discussion
We studied the effect of total laryngectomy on eating ability
especially in detail of Thai food. In the preoperative period, patients
already had cancer either in the larynx or hypopharynx and only
76.5% could eat semisolid food without any difficulty. For sticky food,
hard food and hard and dry food patients could not eat were 29.4%,
17.6% and 29.4% respectively.
All of patients could eat types 1-3 food (clear liquid, thick liquid
and soft food) at all time from preoperative to 1,3 and 6 months after
surgery although with some difficulties at first. There was no more
difficulty after 6 months. These food types contain lot of water and its
softness made them easy for swallowing and should be recommended
to patients to eat at all period.
After 1 month, there was effect of surgery and adaptation
requirement to new physiology, the patients had more problems
with type’s 4-6 food. At 3 months postoperative, most people had
mucositis from radiation and had more difficulty eating semisolid,
sticky, hard and hard and dry food. By 6 months, the wound healing
and eating ability had settled. All patients can eat clear liquid, thick
liquid and soft food without any difficulty which may be due to soft consistency and the fact that pharynx was no longer connected to the
airway and there was no more aspiration. Patients can eat semisolid,
which is the common food in daily life at 76.5%, but 35.3% had some
difficulties.
At the end of 6 months, wound healed well and the acute side
effect of radiation had diminished. Only the permanent change from
both total laryngectomy operation and radiation were left. They could
eat semisolid food at the same percentage as before the operation.
For types 5-7 food, they could eat less than before surgery with
more difficulty with sticky food and hard and dry food. The worst
food was sticky food which only 47.2 % of the patients could eat it,
while 58.9% of patients could eat the hard and dry food (Table 3). The
choice of food types correlate well with altered functions of pharynx,
upper esophageal sphincter and upper esophagus [1-3] which make
propagation of food more difficult and slower. The sticky and dry food
would be more difficult to pass through the pharynx and esophagus.
Approximately half of the patients (9/17) could eat chili hot food at 6
months after the operation, although 3/9 had to reduce the hotness.
In the preoperative cancer counseling, most doctors and patients
tend to discuss and explain more on diseases, treatment and treatment
outcome. For total laryngectomy, there is also specific concern on how
to communicate with other people. The anatomical and physiological
changes that affect eating ability should also be informed to them.
They should understand the type of food patient can eat. Although
liquid and soft food are good for all stage of postoperative period as
well as during radiation also. Patients should be instructed to try all
type of Thai food that they were familiar before having cancer, even
chili hot food. Even if they could not eat some food types during
early postoperative and during radiation, they still can try it after the
wound heals and effect of radiation is stable. Chili hot food is not
prohibited for cancer patients but only half can go back to eat it Table
4. In this study, only uncomplicated cases of TLG were included.
Although Hui (1996) [8] suggested that stretch pharyngeal mucosal
larger than 2.5 cm is sufficient for swallowing function after primary
closure, we keep larger mucosal width of 5 cm or more. And the
swallowing result is relative good in our study. In complicated cases like pharyngeal fistula, flap reconstruction, the patients are likely to
have more swallowing problems and the eating ability could be worse
than in this study. Any how they should be instructed to try as many
types of food as possible. The essence of eating is to bring energy to
life, but enjoyable food brings happiness and liveliness to people.
Table 3
Table 3
Comparing the type of food that the patients eat before and after treatment completion at 1,3 and 6 month among 17 patients. Detail of each number of food
types are shown in table 1.
Table 4
Limitation
There were limit number of patients in this study and the eating satisfaction was not studied.
Conclusion
After uncomplicated total laryngectomy with or without partial pharyngectomy and post operative radiation, patients were still able to eat all 7 types of Thai food, classified by consistency. All patients could eat clear liquid, thick liquid and soft food at all period of study. At 6 months after surgery, 13/17 (76.5%) had no difficulty eating semisolid food, which is the daily life food. Although sticky food, hard food and hard and dry food type are more difficult, high percentage of patients could eat them. Half of the patients could also eat chili hot food compare to before having cancer, although some with reduced hotness. Laryngectomees should be persuaded to try all kind of food even chili hot food to improve eating satisfaction and life quality.
Acknowledgement
We would like to thank Ms. Bungon Pinkeaw and Mr. Suthipol Udompanturak for statistical assistance, Ms. Jeerapa Kerdnoppakhun on manuscript preparation, and to thank Prof. Chaweewan Bunnag and Assoc. Prof. Pongsakorn Tantilipikorn for their support.
References
- Sullivan PA, Hartig GK. Dysphagia after laryngectomy. Curr Opin in Otolaryngol Head Neck Surg. 2001;9:139-146.
- Landera MA, Lundy DS, Sullivan PA. Dysphagia after total laryngectomy.. 2010;19:39-44.
- McConnel FM, Cerenko D, Mendelsohn MS. Dysphagia after total laryngectomy. Otolaryngol Clin North Am. 1988;21(4):721-6.
- Duranceau A, Jamieson G, Hurwitz AL, Jones RS, Postlethwait RW. Alteration in esophageal motility after laryngectomy. Am J Surg. 1976;131(1):30-5.
- Choi EC, Hong WP, Kim CB, Yoon HC, Nam JI, Son EJ, et al. Changes of esophageal motility after total laryngectomy. Otolaryngol Head Neck Surg. 2003;128(5):691-9.
- Yoshioka M, St-Pierre S, Drapeau V, Dionne I, Doucet E, Suzuki M, et al. Effects of red pepper on appetite and energy intake. Br J Nutr. 1999;82(2):115-23.
- Summasut R. Therapeutic diet. Malnutrition and Treatment by Society of Parenteral and Enteral Nutrition of Thailand. 1st ed. Bangkok: Machalongkhun; 1993;73-7.