Surgical Technique
Novel Surgical Approach to Reducible Hammertoe Repair: Plantar Incisional PIPJ Arthroplasty
Raymond Lopez*, Brian Asencio and Jacqueline Brill
Department of Foot & Ankle Surgery, Mt. Sinai Medical Center, USA
*Corresponding author: Raymond Lopez, Department of Foot & Ankle Surgery, Mt. Sinai Medical Center, USA
Published: 25 Apr, 2017
Cite this article as: Lopez R, Asencio B, Brill J. Novel
Surgical Approach to Reducible
Hammertoe Repair: Plantar Incisional
PIPJ Arthroplasty. Clin Surg. 2017; 2:
1433.
Abstract
The surgical correction of hammertoe deformities has been conventionally approached through a longitudinal or elliptical incision located just proximal to the affected proximal interphalangeal joint (PIPJ) on the dorsal aspect of the affected digit. While this has proven to be a safe and effective surgical approach, common complications including painful, deforming scar contracture and poor cosmesis, promoted the authors to investigate this novel plantar incisional approach. In addition, the increasing patient interest towards minimally invasive procedures and cosmetically conscious outcomes necessitates other options. For example, the lateral approach has been outlined with good results however; by the nature of the location of the lateral incision have inherent higher risk of compromising to the neurovascular supply to the digit, increasing the risk of ischemia or paresthesias. Although other alternative approaches have been attempted to address these issue, the plantar approach as described by the authors has never been presented in the literature. This novel approach not only allows the surgeon to address the physiological deformity, but also minimizes the common complications associated with the more traditional procedures. Additionally, the authors feel that this approach will satisfy the ever-growing trend towards patients seeking the most cosmetic and aesthetically pleasing outcome.
Introduction
Hammertoe deformities are a common pathology of patients presenting with forefoot pain.
Perhaps because of cosmetic and shoe wearing issues, the deformity is reportedly more common
in women than men. Hammertoe deformities are found in men as well, especially in those with
certain pre disposing factors; such as an associated elongated metatarsal, metatarsal phalangeal
(MTP) synovitis and instability, inflammatory arthropathies, neuromuscular conditions, and illfitting
shoe gear [1-3]. The biomechanical influences that disrupt the intrinsic balance of muscle
insertions into metatarsals and phalanges which lead to the deforming forces contributing to
digital contracture has been well established in the literature [4,5]. To review, there are three main
biomechanical mechanisms of development for hammertoe contracture. The most common etiology
is “Flexor Stabilization.” This type of hammertoe contracture results from abnormal excessive
pronation during the stance phase of gait. The posterior leg muscles contract earlier and longer than
normal, creating a mechanical disadvantage of the normally stabilizing interossi muscles leading
to pathological contracture. In addition with the long flexors gaining a mechanical advantage
over the intrinsic musculature, the quadratus plantae muscle also loses its ability to straighten the
oblique course of the long flexor tendon, which results in the classic finding of the adductovarus
contracture of the fourth and fifth digit. The next most commonly encountered digital contracture
is described as “Extensor Substitution” This type of contracture is associated with an equinus type
of gait in which the gastrocnemius and soleus muscles are contracted leading to a tight heel cord.
As a result, the anterior leg muscles must assist the ankle in dorsiflexion to oppose the contracted
Achilles tendon leading to a mechanical advantage over the lumbrical muscles of the foot, resulting
in excessive metatarsal phalangeal joint (MPJ) hyperextension during the swing phase of gait and
eventual metatarsal plantarflexion and digital contracture. The least encountered type of digital
contracture is termed “Flexor Substitution.” This type of contracture is observed when the patient
has a weakened gastrocnemius or soleus muscle, which leads to a calcaneus style of gait. The flexor
muscles of the deep posterior compartment of the leg substitute for the weakened gastrocnemius
and soleus muscles. The decreased plantarflexory force of the ankle is achieved with the flexor
digitorum longus muscle, allowing it to achieve a mechanical advantage over the interossei muscles
leading to a sagittal plane contracture of the all the digits.
The development of hammertoes is known to be progressive with
stages of treatment corresponding to the severity and reducibility
of the contracture. Many hammertoes begin as flexible or reducible
interphalangeal joint contractures and over time progress to more
rigid, non-reducible deformities. While conservative treatments
options are available, surgical intervention has proven to provide the
best long-term outcome [6].
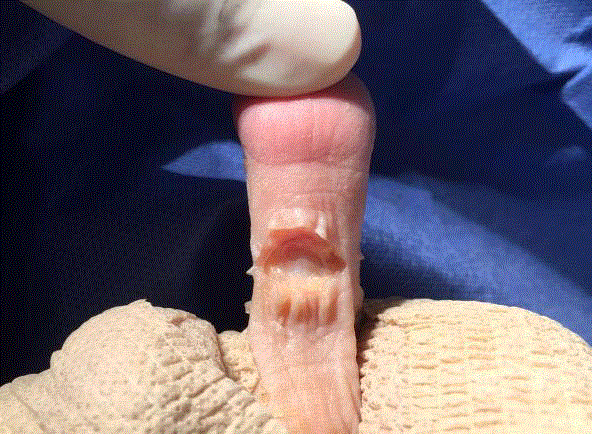
Figure 1
Figure 1
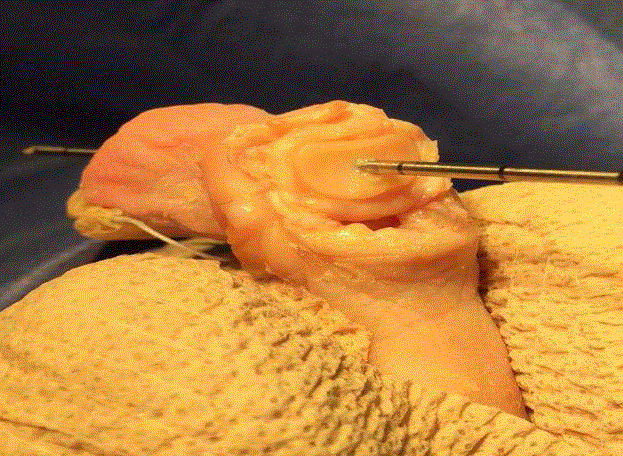
Transverse incision an the platar aspect of the 2nd PIPJ, followed
by blunt dissection to the flexor tendon sheath.
Figure 2
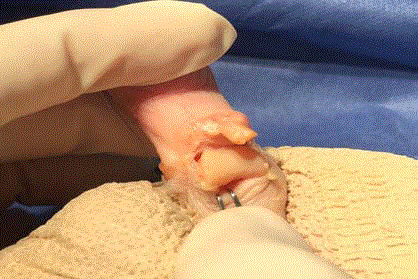
Figure 3
Figure 3
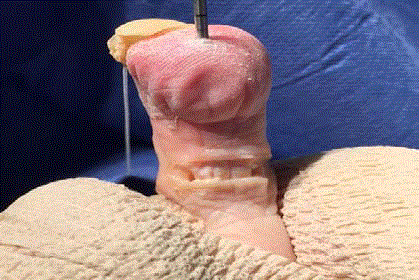
Transected FDL, and FDB tendons visible. Joint capsule is entered
with a transverse incision. The medial and lateral collateral ligaments are
then cut, freeing the proximal phalanx and allowing it to be exposed plantarly
through the incision site. At this point the EDL tendon is also visible dorsally
and can be accessed if required.
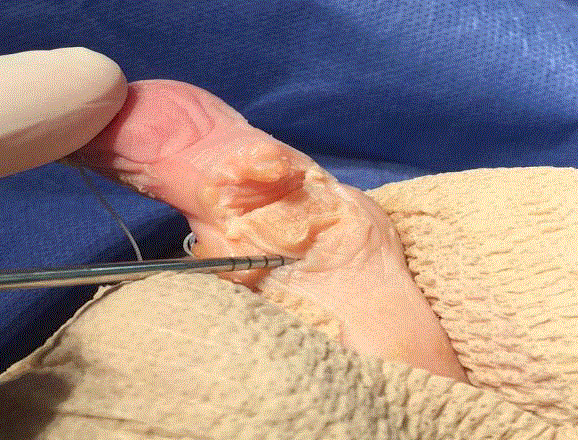
Figure 4
Figure 4
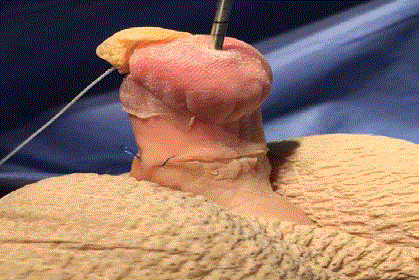
With the proximal phalanx exposed plantarly through the incision
site the arthroplasty of the proximal phalanx head is performed.
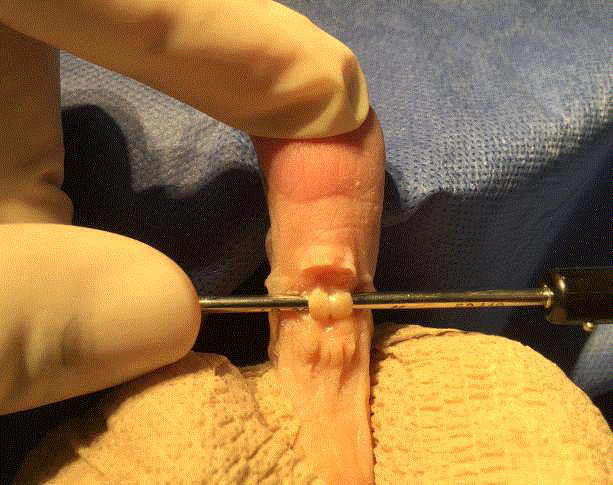
Figure 5
Figure 5
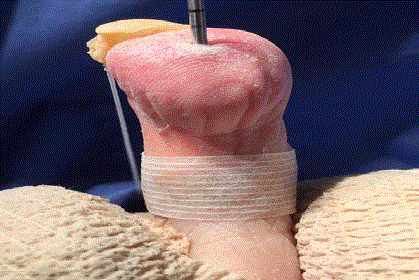
K-wire is advanced distally into the base of the middle phalanx
then proximally into the proximal phalanx when the digit is in the corrected
position.
Figure 6
Figure 6
Once the phalanges are in an acceptable position, the flexor
tendons are re-approximated with 4/0 Vicryl absorbable sutures.
Surgical Technique
The following is a detailed description of our proposed plantar incisional approach for PIPJ arthroplasty. The patient is prepped and the extremity draped in a sterile fashion. A typical V block of local anesthetic is administered with 3-5cc of 0.5% bupivacaine to the effected digit. A number 15 blade is used to make a 1cm transverse incision just proximal to the PIPJ using the proximal crease line as the parallel guide (Figure 1). Blunt dissection then follows to the flexor tendon sheath (Figure 2). The flexor tendons are then split transversely as far distally as possible allowing for the possibility of a flexor tendon transfer if required. Plantar PIPJ joint capsulotomy is performed, and the medial and lateral collateral ligaments are then released (Figure 3). The blade is then passed between the extensor tendon and the proximal phalanx releasing the extensor hood. The head of the proximal phalanx is now free and delivered into the field through the elliptical portal. A bone saw or double action bone cutter is used to transect the proximal phalanx at the neck or at whatever level the surgeon deems as necessary (Figure 4). It should be noted that cartilaginous resection at apposing joint surfaces could also be performed if joint fusion is necessary. The free bone is removed and any rough edges are smoothed with a rasp. If a flexor tendon transfer is to be performed the remaining flexor tendon is split longitudinally and inserted on the dorsal aspect of the proximal phalanx. If necessary a K-wire is then inserted into the base of the middle phalanx and advanced, exiting the distal aspect of the digit. Joint contracture is reduced and the K-wire is then retrograded proximally into the proximal phalanx base (Figure 5). The surgical site is then irrigated with normal saline, flexor tendon re-approximated with 4-0 vicryl and primary closure of incision is performed (Figure 6 and 7). Suture strips are placed over incision and a loose splint with Betadine bandage and gauze is placed over the toe (Figure 8). Patient is given surgical shoe with sutures to be removed in two weeks.
Figure 7
Figure 7
Running sub-q technique with 4/0 Prolene is used to is used to
further minimize post operative scarring.
Figure 8
Figure 8
Incision site and suture is then covered with steri-strips for
additional reinforcement and protection. Post-operative dressing and orders
remain the same as tradition digit arthroplasty.
Discussion
The traditional surgical approach for hammertoe correction is to
utilize a longitudinally oriented dorsal incision, allowing access of the
underlying soft tissue and osseous components necessary to complete
the interphalangeal joint release. Due to the transverse orientation
of this type of incision to the underlying resting skin tension lines,
scar contracture is not uncommon. Additionally, the large dorsal
incisions are easily visible and not aesthetically pleasing to the patient
postoperatively [7]. Modifications to this procedure have since been
made and more recently laterally located incisions have been gaining
popularity [8]. While this approach minimizes the visibility of the
incision site, it does so at the cost of increasing possible complications,
namely digital ischemia, avascular necrosis (AVN), and digital nerve
trauma [9,10]. It is for these reasons that this region of the digit has
historically been avoided when considering surgical portals [11,12].
It is the viewpoint of this paper that the plantar aspect of the digit
may be the key in providing a safe and effective portal for the surgical
correction of hammertoes that also satisfies the patient’s aesthetic
concerns.
As previously noted, the sensitive neurovascular structures
located medially and laterally along the digits have deterred access
in those regions, however the anatomical makeup on the plantar
aspect of the digit is free of concerning structures. Interestingly, the
plantar level of the PIPJ mirrors the dorsal aspect, minimizing any
learning curve to those familiar with the traditional dorsal approach.
Traditionally longitudinal incisions on the plantar aspect of the digits
are avoided, due to possibility of painful scar of the weight bearing surface of the foot. Incision sites on weight bearing surfaces have been
shown to lead to increased fibrosis and the possibility of a secondary
contracture [13]. It must be noted however that fat pad allocation at
the metatarsal phalangeal joint and unique curvature of the lesser
digits significantly minimize contact forces experienced on the plantar
proximal interphalangeal joint cleft of the digits during gait, rather
allocating ambulatory pressures to the distal tuft which are further
increased in hammertoe deformities [14]. Furthermore, successful
use of a plantar longitudinal incision for the tendon release in the
treatment of claw toes has been previously outlined [15,16]. While
a plantar longitudinal incision has shown to be a viable option for
accessing the lesser digits, a smaller, less invasive transverse incision
provides sufficient space for dissection while further minimizing
complications [17,18].
Considerations for a new surgical technique should be made
in instances where sufficient correction can be obtained through a
superior approach, which provides for a more favorable outcome.
When considering various surgical options, specifically in the
instance of cosmetically oriented procedures, one must consider
the prospective outcomes as well as the possible complications. This
plantar incisional approach to reducible hammertoe repair is clearly
less invasive than the traditional dorsal longitudinal incision; providing
for equally sufficient access to the joint and surrounding structures
and yields an exponentially favorable aesthetic outcome. While some
choose to avoid plantar incisions believing the pressure will increase
fibrous and adhesions; the short transverse incision described, due
to its unique placement located in the non-weight-bearing portion
of the PIPJ fold, as well as its orientation to the resting skin tension
lines (RSTL), the authors feel the risk are minimal. The transverse
plantar approach also avoids the susceptible neurovascular bundles
locate on the lateral and medial aspects of the digit, therefore avoiding
the common complication of de-vascularization and necrosis. The
transverse plantar approach delivers the expected correction common
with the traditional approach however with absolutely no scar visible
on the patients standing foot, and an incision hidden in the plantar
PIPJ fold. We believe this is an excellent alternative to the traditional
procedure for patients seeking optimal correction with a cosmetically
appealing outcome, and we feel further research is warranted to assess
its applicability in surgical practice.
References
- Atinga M, Dodd L, Foote J, Palmer S. "Prospective Review of Medium Term Outcomes following Interpositional Arthroplasty for Hammer Toe Deformity Correction". Foot Ankle Surg. 2011;17(4):256-8.
- Kwon JY, De Asla RJ, De Asla. "The Use of Flexor to Extensor Transfers for the Correction of the Flexible Hammer Toe Deformity." Foot Ankle Clin. 2011;16(4):573-82.
- Roukis TS, Schade VL. “Minimum incision metatarsal osteotomies.” Clin Podiatr Med Surg. 2008;25(4):587–607.
- Bade H, Tsikaras P, Koebke J. “Pathomorphology of the hammer toe.” Foot and Ankle Surgery. 1998;4(3):139-43.
- Schuberth, John M. “Hammer toe syndrome.” The Journal of Foot and Ankle Surgery. 1999:166-78.
- Good J, Fiala K. “Digital Surgery: Current Trends and Techniques”. Clin Podiatr Med Surg. 2010;27(4): 583-99.
- Van Enoo RE, Cane EM. “Minimal incision surgery: a plastic technique or acover-up?” Clin Podiatr Med Surg. 1986;3(2):321–35.
- DeBello John A, DeCoteau KI, Beatty E. “Taking A Novel Approach to Hammertoe Surgery”. Podiatry Today. 2006;19(1).
- Scheck M. “Degenerative changes in the metatarsophalangeal joints after surgical correction of severe hammer-toe deformities. A complication associated with avascular necrosis in three cases”. J Bone Joint Surg Am. 1968;50(4):727-37.
- Scheck M. “Etiology of acquired hammer toe deformity”. Clin Orthop Relat Res. 1997;123:63-9.
- Dhukaram V, Prasthofer CA, Kumar UP. “Minimally invasive forefoot surgery: a cadaveric study”. Foot Ankle Int. 2012;33(12):1139-44.
- Gilheany M, Baarini O, Samaras D. "Minimally Invasive Surgery for Pedal Digital Deformity: An Audit of Complications Using National Benchmark Indicators." J Foot Ankle Research J Foot Ankle. 2015;8(1):17.
- Maffulli Nicola, Mark E. Easley. Minimally Invasive Surgery of the Foot and Ankle. London: Springer Verlag. 2011.
- Mueller MJ, Hastings M, Commean PK, Smith KE, Pilgram TK, Robertson D, et al. "Forefoot Structural Predictors of Plantar Pressures during Walking in People with Diabetes and Peripheral Neuropathy." J Biomech. 2003;36(7):1009-17.
- Bouche RT, Heit EJ. “Combined plantar plate and hammertoe repair with flexor digitorum longus tendon transfer for chronic, severe, sagittal plane instability of the lesser metatarsophalangeal joints: preliminary observations.” J Foot Ankle Surg. 2008;47(2):125–37.
- Kernbach KJ. "Hammertoe Surgery: Arthroplasty, Arthrodesis, or Plantar Plate Repair." Clin Podiatr Med Surg. 2012;29(3):355-66.
- Mark MD, Mizel S. “Correction of hammertoe and mallet deformities.” Operative Techniques in Orthopaedics. 1992;2(3);188-94.
- Prado, Mariano De, Pedro Luis. Ripoll and Pau Golanó. Minimally Invasive Foot Surgery Surgical Techniques, Indications, Anatomical Basis. Barcelona: About Your Health, 2009.