Case Report
Case Report: A Nodule on the Scalp with Exogenous Pigment
Nallayici EG1*, Kroft2, Hogenes3 and Schreurs1
1Department of Plas1Department of Surgery, Ziekenhuisgroep Twente (ZGT), Almelo, Netherlands
2Department of Dermatology, Ziekenhuisgroep Twente (ZGT), Almelo, Netherlands
3Department of Pathology, Laboratorium Pathologie Oost-Nederland (LABPON), Hengelo, Netherlands
*Corresponding author: Erol Gökhan Nallayici, Department of Surgery, Ziekenhuisgroep Twente, Zilvermeeuw 1, 7609 PP, Almelo, Netherlands
Published: 24 Apr, 2017
Cite this article as: Nallayici EG, Kroft, Hogenes, Schreurs.
Case Report: A Nodule on the Scalp
with Exogenous Pigment. Clin Surg.
2017; 2: 1423.
Abstract
Background: Modifying hair colour is a common fashion statement in the modern society. Allergy
and/or contact dermatitis on p-Phenylenediamine (PPD) and possible carcinogenetic effects of hair
colouringare described side effects of hair colour dye, but longstanding cutaneous deposition of the
dye pigment has never been described before in current literature.
Observation: We present a 41-year-old Caucasian woman who was referred to our department of
surgery with a nodule on her scalp. The nodule was slowly growing and was first noticed a couple
of months ago. The nodule gave her cosmetic problems. She had no history of scalp trauma, dermal
tattoos, infection or previous skin problems and no family history for dermal malignancies. With
physical examination an elastic bluish nodule of 10 mm, without an opening in the centre was
seen. The nodule was excised and histological analyses demonstrated an extensive granulomatous
inflammatory reaction. These granulomas were associated with an excessive deposition of
intracellular blue-black pigment of exogenously origin and double breaking foreign body materials.
Conclusion: Recurrent use of hair colour dye may induce pigment deposition in rare cases.
Keywords: Exogenous pigment; Blue-black pigment; Nodule; Hair coloring; Hair dye
Introduction
Modifying your hairstyle and hair colour is a fashion statement that reaches out from ancient history to modern society. Hair is an indicator of attractiveness, health and beauty, hair dyeing has become popular among men and women pursing such value or fashion trends. Nowadays, the use of hair dye has been estimated between 50-80% of woman [1]. Several different hair cosmetics with different materials are available and new techniques and dyes are continuously developed to improve the desired effects. Due to close contact of these materials to the skin, different side effects are known ranging from allergy to contact dermatitis (para-phenylenediamine) [2,3] and from poisoning [4,5] till possible carcinogenetic effects [6,7]. Nagata “et al.” [8] suggests that long-term use of hair dyes also may be associated with an increase in circulating testosterone levels.
Case Presentation
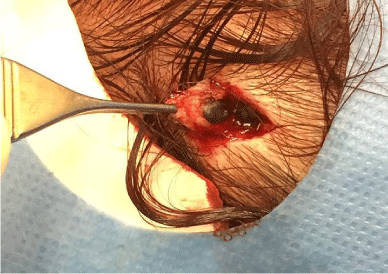
A 41-year-old Caucasian woman was referred to our department of surgery with a nodule on herscalp. The nodule was slowly growing and was first noticed a couple of months prior to her referral. There was only a single nodule present, causing cosmetic but no physical complaints. Her medical history showed hypertension, a laparoscopic cholecystectomy, a mild aortic valve stenosis and an unguis incarnatus of the hallux. The patient used oral anticonception, but no other medications. The patient had any history of head trauma, dermal tattoos, infection, allergies or previous skin problems. There was no family history for dermal malignancies, especially not for melanoma.
Examination
With physical examination an elastic blueish nodule of 10 × 10 × 5 mm, without an opening in
the centre was seen at the occipital scalp region with some hair loss on the skin surface immediately
above the nodule. During total body inspection no clinical atypical melanocytic lesions were seen.
The nodule was not painful during palpation. Its appearance was felt to be suspicious for malignancy.
Differential diagnosis
- sebaceas cyst/pilar cyst/hidrocystoma
-blue naevus
-foreign body granuloma
-nodular melanoma
-pigmented dermatofibroma
-pilomatricoma
-lymphadenosis cutis benigna
Excision
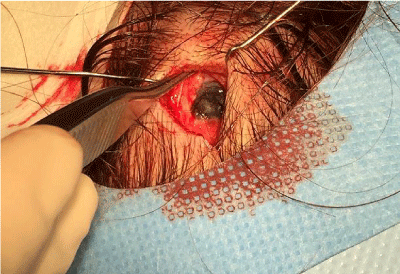
Complete resection of the lesion was advised with margins of 2
mm. During this procedure, the nodule appeared to expand from
the dermis through the subcutaneously to be closely adherent to the
periost. In order to gain more information we changed our procedure
to a diagnostic incision biopsy instead of complete resection.
Microscopic examination
Biopsy showed an extensive granulomatous inflammatory
reaction, similar to sarcoid-granuloma deposits as found in
sarcoidosis. These granulomas were associated with an excessive
precipitation of intracellular blue-black pigment of exogenously
origin and double breaking foreign body materials (Figures 2a and
2b). There were no malignant features.
Diagnosis
Foreign body granulomatous (GIANT) cell reaction, in the
absence of known hair dye substances.
Follow-up
Due to the benign aspect of this lesion further resection was not
performed after shared decision making with the patient. After one
year follow-up, our patient did not develop other complaints, new
lesions or nodules. Further follow-up was discontinued due to lack of
further indication.
Figure 1a
Figure 1b
Figure 2a
Figure 2a
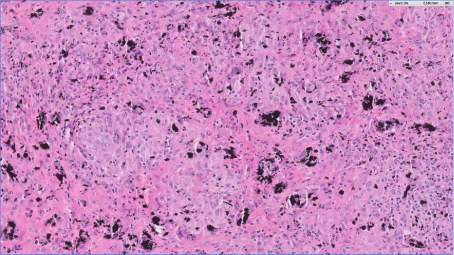
Histology overview (HE, 1x) of the cutaneous excision with
epidermis, dermis and subcutaneous fat including inked resection margins,
showing the depth of the granulomatous lesion.
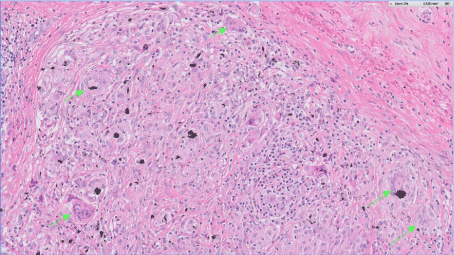
Figure 2b
Figure 2b
Histology detail (HE, 20x) showing in more detail the presence of
giant cells (arrows), histiocytes and lymphocytes. The presence of the black
pigment can easily be appreciated in this picture.
Discussion
During last decades, several different hair cosmetics have been introduced into the market. Our patient was not able to remember the different brands and hair dye substances she used over time. She did use different types; some of them contained natural and some chemical dyes. The most common types of hair dyes are temporary, semi-permanent and permanent hair dyes [9,10]. The hair consists of the root and the shaft, the shaft has three layers: the cuticle, the cortex and the medulla. The temporary dyes have large molecules which are unable to penetrate into the cortex, temporary dyes are easily washed out in one shampoo. The small molecules of the semi-permanent hair dyes easily penetrate through the cuticle into the cortex and are there for also washable, the dye is removed in 4-15 shampoos [9,10]. The smaller particles of the permanent dyes do reach the cortex, in the cortex they form larger molecules and are therefore not washable [10]. Temporary and semi-permanent dyes are direct dyes which do not require chemical reaction to impact colour [10]. Permanent dyes are colourless and contain oxidizing and alkaline agents, which induce a chemical reaction to form the colour [10]. The most common permanent pigments are para-phenylenediamine (PPD), para-toluenediamine (PTD) and para-aminophenol (PAP) [9]. Paraphenylenediamine is present in more than 70% of the hair dyes, but it can also be found in coloring products like other cosmetics, textile dyes, temporary tattoos, printing inks, photocopying, black rubber, oils and gasoline [10]. The correct use of the hair dyes is essential; misuse may result in hair damage and hair loss [9]. Paraphenylenediamine in direct dermal contact, may cause adverse side effects like skin irritation or allergy [2,3] and systemic effects like cancer [6,7]. However our knowledge about these side effects is still very limited and most side-effects are very rare. The dermal deposition of hair dyes has not been described previously. To our speculation, hair dye deposition might occur after dermal contact of the dye through the hair shaft toward the hair root (Figure 1). Due to excessive deposition of hair dye, the nodule might expand toward the periost like in our case. The dermal deposition of the pigment from hair dyes after colouring was our case only explanation for the clinical and pathological findings.
Conclusion
To our knowledge, this is the first report of long standing dermal pigment deposition after the use of hair colouring dye. It is important to realize that using hair colouring dye may have more side effects then currently known in literature.
References
- Nohynek GJ, Skare JA, Meuling WJ, Wehmeyer KR, de Bie AT, Vaes WH, et al. Human systemic exposure to [14C]-paraphenylenediamine-containing oxidative hair dyes: Absorption, kinetics, metabolism, excretion and safety assessment. Food Chem Toxicol. 2015;81:71-80.
- Søsted H, Rustmeyer T, Gonçalo M, Bruze M, Goossens A, Giménez-Arnau AM, et al. Contact allergy to common ingredients in hair dyes. Contact Dermatitis. 2013;69(1):32-9.
- Diepgen TL, Naldi L, Bruze M, Cazzaniga S, Schuttelaar ML, Elsner P, et al. Prevalence of Contact Allergy to p-Phenylenediamine in the European General Population. J Invest Dermatol. 2016;136(2):409-15.
- Patra AP, Shaha KK, Rayamane AP, Dash SK, Mohanty MK, Mohanty S. Paraphenylenediamine containing hair dye: an emerging household poisoning. Am j Forensic Med Pathol. 2015;36(3):167-71.
- Sanchez L, Harish H, Shanmugamari K, Siddalingeswara, Alvarez-Uria G, Laura G, et.al. Hair dye poisoning: Retrospective analyses of patients admitted to ICU at a rural hospital in India. Indian J Med Res. 2016;144(1):134-7.
- Heikkinen S, Pitkäniemi J, Sarkeala T, Malila N, Koskenuvo M. Does Hair Dye Use Increase the Risk of Breast Cancer? A Population-Based Case-Control Study of Finnish Women. PloS one. 2015;10(8):e0135190.
- Takkouche B, Mahyar E, Montes-Martínez A. Personal use of hair dyes and risk of cancer: a meta-analysis. Jama. 2005;293(20):2516-25.
- Nagata C, Wada K, Tsuji M, hayashi M, Takeda N, Yasuda K. Association of hair dye use with circulating levels of sex hormones in premenopausal Japanese women. Euro J Public Health. 2015;25(5):895-9.
- Gavazzoni Dias MF. Hair cosmetics: an overview. Int J Trichology. 2015;7(1):2-15.
- Kim KH, Kabir E, Jahan SA. The use of personal hair dye and its implications for human health. Environ Int. 2016;89-90:222-7.