Research Article
Isolated Sphenoid Sinus Pathology: Retrospective Analysis of 7 Cases
Alper Dilci1*, Omer Bilac2 and Ersem Giritli1
1Department of Otolaryngology, Yunus Emre State Hospital, Eskisehir, Turkey
2Department of Otolaryngology, Sultan Abdulhamid Han Research and Training Hospital, Istanbul, Turkey
*Corresponding author: Alper Dilci, Department of ENT and Head Neck Surgery, Yunus Emre State Hospital, 26190, Eskisehir, Turkey
Published: 24 Apr, 2017
Cite this article as: Dilci A, Bilac O, Giritli E. Isolated
Sphenoid Sinus Pathology:
Retrospective Analysis of 7 Cases. Clin
Surg. 2017; 2: 1420.
Abstract
Objectives: To investigatethe patients who underwent endoscopic sphenoid sinus surgery for isolated sphenoid sinus disease. We also evaluated the clinical characteristics and management skills
of our department in isolated sphenoid pathologies.
Design: Retrospective analysis of case series.
Material and Methods: 7 patients who underwent endoscopic sphenoid sinus surgery for
isolated sphenoid sinus disease. Clinical characteristics and main symptoms of patients, physical
examination, radiologic findings and management aproaches were investigated retrospectively.
Results: We identified 7 cases of isolated sphenoid sinus disease between January 2015 and January
2016. 3 cases with fungal infection of sphenoid sinus, 2 cases with with sphenochoanal polyp and 2
cases with mucocele were treated by endoscopic sphenoidotomy.
Conclusion: Isolated sphenoid sinus pathologies are rare clinical entities. Diagnosis is based on the
history, endoscopic examination and computed tomography findings. Endoscopic sphenoidotomy
is a safe and easy treatment option and represented the gold standard for this disease at the present time.
Keywords: Sphenoid sinus; Sphenoidotomy; Endoscopic
Introduction
The sphenoid sinus was defined as the neglected sinus by van Alyea, in 1941 because of its
isolated position and difficult accessibility [1]. However, sphenoid sinus disease has been reported
increasingly in recent medical literature. Isolated sphenoid sinus pathology is a rare clinical condition
among patients with paranasal sinus disease, reported incidence between 1%-3% [2]. Because of the
location and difficult accessibility of sinus is suggested to make it less accessible to infectious agents.
Isolated sphenoid sinus lesions most commonly present with headache, ophtalmological and
nasal symptoms. Delayed diagnosis may occur due to its nonspecific symptoms [3]. However, there
are many vital structures, including the middle cranial fossa, internal carotid artery, optic nerve and
optic chiasm, cavernous sinus, brain, meninges and cranial nerves adjacent to sphenoid sinus [4].
Improper management of sphenoid sinus disease may lead to serious complications such as orbital
abscess, cavernous sinus thrombosis, meningitis, epidural, subdural, cerebral abscess [5].
The signs and symptoms of isolated sphenoid sinus disease may be unclear and nonspecific, is
difficult to diagnose with history and physical examination due to the location of the sinus [6]. Beside the symptoms and physical examination finding; nasal endoscopy and better imaging technologies
such as CT and MRI allow the early diagnosis of sphenoid sinus disease. Differential diagnosis has
to be made with sphenoid sinusitis, fungal infection, benign neoplasms such as inverted papilloma
and malignant neoplasms for isolated sphenoid sinus pathology [7].
In this study, we present seven patients who underwent endoscopic sphenoid sinus surgery for
isolated sphenoid sinus disease in Eskisehir Yunus Emre State Hospital. The purpose of this study is
to review our experience with lesions located in the sphenoid sinus.
Material and Methods
In this retrospective study, seven patients who underwent endoscopic sphenoid sinus surgery for
isolated sphenoid sinus disease were presented between January 2015 and January 2016 in Eskisehir Yunus Emre State Hospital ENT Department. Data collected from the
archives of patient files and surgical notes of Eskisehir Yunus Emre
State Hospital. Informed consent was taken from all patients who
included in this study. Patient demographics, presenting symptoms,
surgical details and histopathological outcome were evaluated (Table 1).
Diagnosis of isolated sphenoid sinus disease was based on the
history, physical examination, nasal endoscopy and radiological
evaluation. At the time of the diagnosis, there was no involvement
of the other sinuses. Patients were evaluated by objective ear, nose,
throat examination including flexible nasal sinus endoscopy.
The diagnosis was confirmed by paranasal sinus CT in axial and
coronal sections. This serie also included patients whose disease was
detected incidentally by other departments especially neurology and
neurosurgery. MRI was performed in patients suspected for fungal
infection and malignancy; also performed in patients whose disease
was detected in neurology and neurosurgery.
Surgical technique
The endoscopic sphenoid sinus surgery was performed in antitrendelenburg
position under general anesthesia. Nasal decongestion
is obtained by applying a lidocaine and adrenaline soaked cotton
pledgets in nasal cavity before the surgery. After the decongestion,
cotton pledgets are removed and local anesthetic infiltration are
applied. Middle turbinate are gently displaced laterally. The sphenoid
sinus rostrum are approached between the middle and superior
turbinates laterally and the septum medially. The sphenoid sinus
ostium was identified 1.5 cm above the choana. Superior concha are
visualized by 0 or 30 degree endoscope and the inferior portion of
superior concha was resected. Sphenoidotomy is performed in an
inferomedial direction. Sphenoid sinus ostium was widened and
pathology was removed. The whole mucosa is never excised. At the
end of the intervention, nasal cavity is irrigated and nasal packs are
placed. Tampons are removed between first and second postoperative
days. After the intervention, patients were treated with antibiotic
therapy. Every patient has been followed in 3 months intervals in a
year.
Results
7 patients who underwent endoscopic sphenoidotomy for
isolated sphenoid sinus pathology were included in this study. There
were 5 female and 2 male patients ranging from 22 to 65 years.
Sphenoid sinus involvement was unilateral in 3 patients. 2 patients
with sphenochoanal polyps and 2 patients with sphenoidal mucocele
had unilateral sphenoidal disease. Patients were stratified into groups
based on the pathological condition. Fungal infection, polyps and
mucoceles are the main groups of isolated sphenoid disease in this
study.
Five patients presented with headache that did not respond
to simple analgesia. Headache was either occipital, retroorbital,
bifrontal and vertex; was nonspesific in quality. Nasal symptoms
were the second most common presenting symptoms. These included
nasal obstruction in three patients, postnasal drip and nasal discharge
in two patients. Nasal obstruction was major complaint in the
sphenoidal polyp cases due to the size of the polyp. Nasal symptoms
was resistant to main medical treatment.
Endoscopic examination was performed in all patients. Four
patients had positive findings in the endoscopic examination. Polypoid
tissue in the sphenoethmoidal recess in two patients, mucopurulent
discharge in the sphenoid ostium in a patient and swelling, congestion
and edema in a patient. All patients were investigated with CT scan
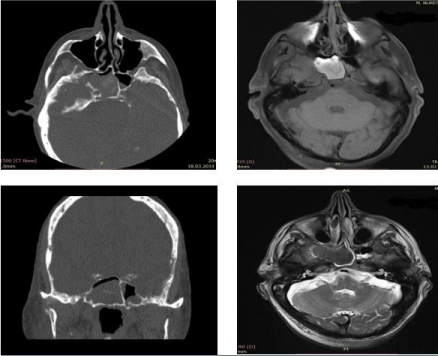
of the paranasal sinuses. If there was a suspicion of sphenoidal mass,
contrast enhancement was utilized and MRI was performed (Figure
1). Four patients was underwent MRI evaluation and fungal infection
was diagnosed in three of them and mucocele was diagnosed in the
other.
Endocsopic sphenoidotomy was performed for all patients.
In three of the patients extended unilateral sphenoidotomy was
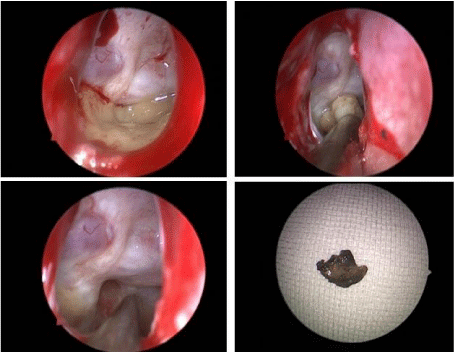
performed for fungus ball. Internal carotid artery dehissence was seen
in a patient with fungal infection (Figure 2). There was not any major
complications during the surgeries. All patients reported improvement
in symptoms postoperatively. Hospital stay ranged form a minimum
number of a day to a maximum of 3 days. Routine postoperative CT
or MRI scanning were not conducted; nasoendoscopy was applied in
the follow up period. Patients are followed up in 3 months intervals
during a year and there was not any recurrences was reported.
Table 1
Figure 1
Figure 2
Figure 2
Intraoperative images of fungal infection of sphenoid sinus.
Dehissence was detected on the wall of carotid canal and calcified material
resulted from fungal infection sphenoid sinus.
Discussion
Isolated sphenoid sinus disease is an uncommon disease that affects
1%-3% of patients. Compared to the other sinuses, presents several
diagnostic and therapeutic challenges. Inflammatory etiologies were
responsible for 61%-82% of isolated sphenoid pathologies, followed
by benign or malignant neoplasm [8]. Malignancy of sphenoid sinus
could also be reported unless in our series we could not diagnose
any of it. Fulminant headaches, visual disturbances, CSF rhinorrhea,
cranial nerves deficits can be seen in malignant cases of this region
[9]. It is usually insidious in onset and may present with nonspesific
symptoms like headache and nasal obstruction. The most common
symptom of sphenoid sinus disease is headache. In the majority of
previous reports, headache was nonspesific in location, quality and
intensity [10]. Headache was presenting and major symptom in
71% of cases in our series. Nasal symptoms was the second most
commonly complaint in our case series. Two patients had a huge
polypoid mass arising form sphenoid sinus blocking the nasal airway.
Visual disturbances are oftenly the second most common symptoms
for sphenoid pathology in other series, but in our study we could
not meet it. Maybe it is due to there is not any neoplastic mass in
sphenoid sinus in this study.
The diagnosis of isolated sphenoid sinus disease is based on
history, physical examination including nasoendocopy and radiologic
studies. Sphenoethmoidal recess can be identified by endoscopic
nasal examination [11]. However; 57% patients in our series present
endoscopic findings. Normal looking sphenoethmoidal recess on
nasoendoscopy does not exclude sphenoid pathology so radiologic
studies must be used [12]. In isolated sphenoid sinus pathologies; CT
imaging may reveal a spectrum of pathology ranging from mucosal
thickening to opacifications of sinus. It is valuable in showing the
bone details with the ability of differentiating the sinus wall expansion
and destruction. Fungal infections of the sphenoid sinus require more
special attention. It is occasionally not distinguishable from benign or
malignant tumors. All susupected mass lesions within the sphenoid
sinus should be evaluated with MRI as it provides more information
about the soft tissues [13].
There are many surgical techniques are used to access the
sphenoid sinus including subfrontal, frontotemporal, subtemporal
transcranial, transfacial, transseptal. These techniques require surgical violation to the other structer for sphenoid sinus. The transnasal
surgical approaches to isolated sphenoid sinus diseases include the
endoscopic transnasal, endoscopic transethmoid, transseptal and
endoscopic pterygoid fossa [14]. If necessary each of these can be
used in conjunction with an extracranial approach. In cases involving
inflammatory process like in this case series; endoscopic transnasal
sphenoidotomy has been reported to be safe and effective. The key
point in approaching the sphenoid sinus was adequate exposure of
the sphenoethmoidal recess to identify the sphenoid sinus ostium
endoscopically. Once the sphenoid ostium was sufficiently enlarged,
surgery can be performed with caring to optic and carotid canal. Like
in our series, dehissense can be seen in optic or carotid canals and
harmful maneuvers to these structures can cause major complications
during the surgery. This technique offers several advantages: better
view of anatomic structures, no visible scars, lesser traumatisim, small
postopeative morbidity, preservation of physiological mucociliary
drainage and shorter hospitalization. Unfortunately, difficult
management of intraoperative bleeding and any other complications
in surgery, long and difficult learning curve for the operator and need
for special instruments are the major disadvantages.
Conclusion
Isolated sphenoid sinus diseases occurs relatively infrequent and presenting symptoms are often nonspesific. Headaches, nasal symptoms, visual disturbances, cranial nerve findings can be reported. Inflammatory diseases are the most of the reasons of isolated sphenoid sinus disease presented with unlocalized headache and nasal findings. Diagnosis and management of sphenoid sinus can be challenging in some cases. History, physical examination including nasoendoscopy and radiologic studies must be necessary for appropriate diagnosis. Especially, for inflammatory lesions of sphenoid sinus; minimally invasive endoscopic transnasal sphenoidotomy is safe and effective method. Anatomic relations of major structures in sphenoid sinus and skull base should always keep in mind during the management.
References
- Van Alyea OE. Sphenoid sinus: anatomic study, with consideration of the clinical significance of the structural characteristics of the sphenoid sinus. Arch Otolaryngol. 1941;34(2):225–53.
- Lawson W, Reino AJ. Isolated sphenoid sinus disease: an analysis of 132 cases. Laryngoscope. 1997;107(12 Pt 1):1590-5.
- Nour YA, Al-Madani A, El-Daly A, Gaafar A. Isolated sphenoid sinus pathology: Spectrum of diagnostic and treatment modalities. Auris Nasus Larynx. 2008;35(4):500–8.
- Wang ZM, Kanoh N, Dai CF, Kutler DI, Xu R, Chi FL, et al. Isolated sphenoid sinus disease: an analysis of 122 cases. Ann Otol Rhinol Laryngol. 2002;111(4):323-7.
- Goldman A. Complications of sphenoid sinusitis. Oper Techn Otolaryngol. 2003:14:216–8.
- Ng YH, Sethi DS. Isolated sphenoid sinus disease: differential diagnosis and management. Curr Opin Otolaryngol Head Neck Surg. 2011;19(1):16-20.
- Grillone GA, Kasznica P. Isolated sphenoid sinus disease. Otolaryngol Clin North Am. 2004;37(2):435-51.
- Cakmak O, Shohet MR, Kern EB. Isolated sphenoid sinus lesions. Am J Rhinol. 2000;14(1):13-9.
- Ghosh R, Dubal PM, Chin OY, Patel TD, Echanique KA, Baredes S, et al. Sphenoid sinus malignancies: a population - based comprehensive analysis. Int Forum Allergy Rhinol. 2016; 6(7):752–9.
- Ruoppi P, Seppä J, Pukkila M, Nuutinen J. Isolated sphenoid sinus diseases: report of 39 cases. Arch Otolaryngol Head Neck Surg. 2000;126(6):777-81.
- Gibbons MD, Sillers MJ. Minimally invasive approaches to the sphenoid sinus. Otolaryngol Head Neck Surg. 2002;126(6):635-41.
- Sethi DS. Isolated sphenoid lesions: diagnosis and management. Otolaryngol Head Neck Surg. 1999;120(5):730-6.
- Branstetter BF, Weissman JL. Role of MR and CT in the paranasal sinuses. Otolaryngol Clin North Am. 2005;38(6):1279-99, x.
- Martin TJ, Smith TL, Smith MM, Loehrl TA. Evaluation and surgical management of isolated sphenoid sinus disease. Arch Otolaryngol Head Neck Surg. 2002;128(12):1413-9.