Research Article
Obesity in Patients after Liver Transplantation
Mariana Arruda Silva1*, Alceu Afonso Jordão Júnior2 and Orlando de Castro e Silva Júnior1
1Department of Surgery and Anatomy, Sao Paulo University, Brazil
2Department of Internal Medicine, Sao Paulo University, Brazil
*Corresponding author: Mariana Arruda Silva, Department of Surgery and Anatomy, School of Medicine of Ribeirao Preto, Sao Paulo University, Avenida Caramuru, 2450, ap. 97, torre 02. Postal Code: 14030- 000. Ribeirao Preto, Sao Paulo, Brazil
Published: 14 Apr, 2017
Cite this article as: Silva MA, Júnior AAJ, de Castro e Silva
Júnior O. Obesity in Patients after Liver
Transplantation. Clin Surg. 2017; 2:
1403.
Abstract
The aim of the present study was to evaluate the nutritional status of post-liver transplant patients.
The sample consisted of a group of patients submitted to liver transplantation and a control
group of patients without liver disease. Nutritional status was assessed by body composition
and anthropometric methods. Body mass index indicating overweight and obesity was observed
regardless of the post-liver transplantation period. Waist circumference was greater than the value
recommended by the World Health Organization in the majority of post-transplant patients.
Patients with a longer post-transplant period had a mean phase angle similar to that of the control
group, while patients with a shorter post-transplant period had a lower mean phase angle. These
results suggest a full recovery from surgery and a health improvement after transplantation since
the phase angle is a measure related to nutritional status and prognosis. In conclusion, although the
post-liver transplantation population studied may have had a full recovery and health improvement
after surgery, obesity and excessive body fat mass are prevalent and may be deleterious in the long
term in view of the associated risk of cardiovascular events.
Keywords: Liver transplantation; Obesity; Fat body mass; Phase angle
Introduction
In recent decades, overweight and obesity have become a global public health issue. Overweight
and obesity are associated with increased risks of all-cause mortality, cancer, non-alcoholic fatty
liver disease, hypertension, type 2 diabetes, and metabolic syndrome [1]. The major impact of
obesity on the liver is the association with non-alcoholic steatohepatitis (NASH). Indeed, NASH
has emerged as one of the fastest growing indications for liver transplantation [2].
Clinical observations in long-term survivors after liver transplantation have revealed a considerable gain in body weight and an increasing prevalence of obesity [1,3]. Most of the excessive
weight gain occurs in the first year of transplantation and among the causes include recovery of the
appetite followed by health improvement and hyperphagia associated to the corticosteroid use and a
sedentary life style [4]. At the end of the first year after liver transplantation, patients fail to replenish their total body protein, while fat mass approximates predicted values [3]. Immunosuppressive medication is often cited as a risk factor for weight gain [1].
Recently, post-transplant obesity has received interest as part of the metabolic syndrome evolving
after transplantation, jeopardizing the gain in patient prognosis achieved by transplantation [2,3].
Obesity is associated with metabolic disorders and comorbidities such as coronary artery disease
[2]. Moreover, cardiovascular events have been reported as a leading cause of mortality after solid
organ transplantation [1].
Considering this scenario and the importance of preventing obesity in liver graft survivors,
nutritional status should be monitored in all post-transplant patients, leading to appropriate
nutritional treatment. The aim of the present study was to evaluate the nutritional status of postliver
transplant patients.
Table 1
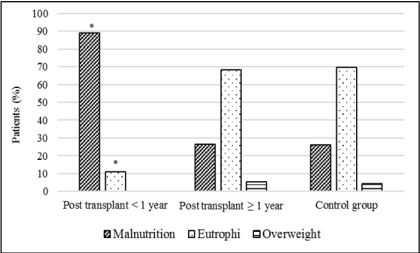
Figure 1
Figure 1
Nutritional status of the post-transplant and control groups
according to muscle arm circumference. *p=0.002 for malnutrition between
groups and p=0.0059 for normal weight between groups.
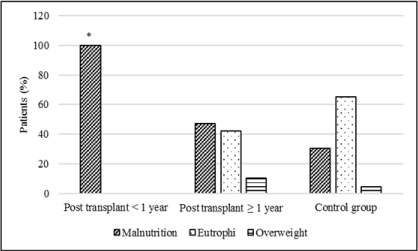
Figure 2
Figure 2
Nutritional status of the post-transplant and control groups
according to muscle arm area. *p=0.0019 for malnutrition between groups.
Method
The present study reports partial data from a major unpublished study of liver transplantation
from our group conducted at Hospital das Clínicas, Ribeirao Preto Medical School, Sao Paulo
University (HC-FMRP/USP) between March 2012 and December 2013. Nutritional status was
assessed by body composition and anthropometric methods. The sample consisted of a group of
post-liver transplantation patients (n=28) and a control group of patients without liver disease
(n=23).
The post-transplant group consisted of patients aged ≥18
years with a post-liver transplantation period >30 days. Exclusion
criteria were chronic kidney disease, acute or chronic respiratory
failure, infectious pulmonary disease, untreated hyperthyroidism or
hypothyroidism, and locomotor disability. Patients with diagnosis of
graft rejection were excluded from the sample. The post-transplant
group was divided into two subgroups according to post-transplant
period, i.e., <1 year and ≥1 year.
The control group consisted of outpatients aged ≥18 years
seen at the Urology Clinic of HCFMRP-USP, matched to the posttransplant
patients for gender, age and body mass index (BMI).
Eligibility criteria included absence of alcohol consumption and
of acute or chronic liver disease, renal failure, pulmonary disease,
cancer, hyperthyroidism, hypothyroidism, and locomotor disability.
Biochemical analyses of albumin, aminotransferases, total protein,
cholinesterase, lactate dehydrogenase, bilirubin, alkaline phosphatase
and glutamyl transferase were carried out according to standard
methodologies [5-12] at the Laboratory of the Surgery Department,
HCFMRP-USP, in order to determine liver function.
Anthropometric measurements of weight, height, arm and
abdominal circumferences and skinfold thickness were performed for nutritional assessment. Measurements were made according to
standard methods using calibrated equipment. BMI was classified
according to standard references for adults [13] and elderly subjects
[14]. Arm muscle circumference, arm muscle area and arm fat area
were assessed by equations and considered to represent malnutrition,
normal weight and obesity according to reference values for gender
and age [15-18].
Body composition was assessed by 50 kHz single frequency electric
bioimpedance using a Biodynamic Analyzer 310 model (Biodynamics
Corporation, Seattle, WA, USA) for the tetrapolar method and using
an Ironman Segmental Compositor BC-558 (Tanita Corporation,
Toquio, Japan) for the segmental method, according to standard
methods and with the patient fasted for at least 4 h.
Food consumption was assessed by a trained dietitian using a
habitual food record.
Statistical analyses were performed using the Prism GraphPad
4.0 software (San diego, CA, USA). Data are reported as mean and
standard deviation for continuous quantitative variables. The Student
t test and ANOVA (with Bonferroni’s post-test) were used to compare
two or more independent groups. The chi-square test was applied to
categorical variables. The level of significance was set at 5% in all tests.
The study was approved by the Ethics Committee o HCFMRPUSP
and all subjects gave written informed consent to participate.
Results
Sample consisted of 5 women and 23 men. Main causes of liver transplantation were by alcoholic cirrhosis (29%), followed by
cryptogenic cirrhosis (21%), alcoholic cirrhosis associated to virus C
hepatitis (14%), virus C hepatitis cirrhosis (14%) and other causes as
virus B hepatitis (n=1), virus B associated to virus D hepatitis (n=1),
autoimmune hepatitis cirrhosis (n=1), familiar paramyloidosis (n=1),
alfa-1 antitrypsin deficiency (n=1), and primary biliary cirrhosis
(n=1). Immunosuppressive medication consisted most of tacrolimus
(50%), followed by tacrolimus associated to mofetil micofenolate
(43%), mofetil micofenolate (4%) and sirulimus (4%).
Antropometric data are shown in Table 1. Mean muscle arm
circumference and mean muscle arm area differed statistically
between groups. A higher frequency of muscle mass deficit (Figures
1 and 2) was observed in the <1 year post-transplant group regarding
muscle arm circumference and muscle arm area. Sub-scapular
skinfold thickness differed significantly between groups.
Tetrapolar bioelectrical impedance data are presented in Table 2
and segmental bioelectrical impedance data are presented in Table 3.
There was no significant difference in body fat mass or body fat-free
mass between groups according to both the tetrapolar and segmental
methods. Phase angle was significantly lower in the <1 year posttransplant
group. Energy and macronutrient intake did not differ
significantly between groups.
Waist circumference was greater than the value recommended by
the WHO [19], of 94 cm for men and 80 cm for women, in 78% of <1
year post-transplant patients and in 79% of ≥1 year post-transplant
patients.
Table 2
Table 3
Discussion
The present study contributed important results to the literature
by corroborating with recent findings about the nutritional status of
liver transplant recipients.
Body mass index values indicating overweight and obesity
were observed in liver transplant patients regardless of post-liver
transplantation period. Waist circumference demonstrated higher
severe risks of cardiovascular events in the majority of patients.
Excessive weight gain (more than 10 kg) during the first year after
liver transplantation has been reported [1], with a 40% incidence of
obesity in this population in the first post-transplant year [20] and
an incidence of about 70% three years after transplantation [21,22].
Studies have described an increased prevalence of dyslipidemia,
hypertension and diabetes mellitus in liver transplant recipients.
Together with the excessive body weight, these conditions contribute
to the occurrence of metabolic syndrome and the increasing risk
of cardiovascular events, which are the main cause of death after
transplantation [23,24].
Although the difference was not significant, fat body mass was
greater in patients with ≥1 year of liver transplantation, while lean
body mass was similar for the two groups. It is possible that the
recovery of body mass does not occur proportionally between fat and
lean mass in post-liver transplanted patients.
Increased food intake, physical inactivity and immunosuppressive
therapy have been described as possible causes of obesity in liver
transplant patients [7].
Phase angle, a measure of bioimpedance analysis, was similar
between patients with a longer post-transplant period and controls,
while patients with a shorter post-transplant period had a lower mean
phase angle. These results suggest a full recovery from surgery and
improved health after transplantation since phase angle is a measure
associated with nutritional status and prognosis [25].
In conclusion, although the post-liver transplantation population
studied here may have had a full recovery and health improvement
after surgery, obesity and excessive fat body mass are prevalent and
may be deleterious in the long term considering the associated risk of
cardiovascular events.
Acknowledgment
The author’s responsibilities were as follows –Silva MA:
accountable for research execution and manuscript preparation.
Jordão AA: accountable for research supervision and revision of the
manuscript. Castro e Silva O: mentor of the research, accountable for
research supervision and revision of the manuscript.
This work was supported financially by a Capes Federal grant.
References
- Beckmann S, Ivanovic N, Drent G, Ruppar T, De Geest S. Weight gain, overweight and obesity in solid organ transplantation—a study protocol for a systematic literature review. Syst Ver. 2015;4:1-8.
- Saab S, Lalezari D, Pruthi P, Alper T, Tong MJ. The impact of obesity on patient survival in liver transplant recipients: a meta-analysis. Liver Int. 2015;35(1):164-70.
- Schütz T, Hudjetz H, Roske AE, Katzorke C, Kreymann G, Budde K, et al. Weight gain in long-term survivors of kidney or liver transplantation--another paradigm of sarcopenic obesity? Nutrition. 2012;28(4):378-83.
- Parolin MB, Zaina FE, Lopes RW. [Nutritional therapy in liver transplantation]. Arq Gastroenterol. 2002;39(2):114-22.
- SIMS FH, HORN C. Some observations on Powell's method for the determination of serum bilirubin. Am J Clin Pathol. 1958;29(5):412-7.
- Henry JR, Chiamori N, Golub OJ, Berkman S. Revised spectrophotometric methods for the determinatioon of glutamic-oxalacetic transaminase, glutamic-pyruvic transaminase, and lactic acid dehydrogenase. Am J Clin Pathol. 1960;34:381-98.
- Bessey OA, Lowry OH, Brock MJ. A method for the rapid determination of alkaline phosphates with five cubic millimeters of serum. J Biol Chem. 1946;164:321-9.
- Ellman GL, Courtney KD, Andres Júnior V, Featherstone RM. A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem. Pharmacol. 1961;7: 88-95.
- Gornall AG, Bardawill CJ, David MM. Determination of serum proteins by means of the biuret reaction. J Biol Chem. 1949;177(2):751-66.
- Doumas BT, Watson WA, Biggs HG. Albumin standard and the measurement of serum albumin with bromocresol green. Clin Chim Acta. 1971;31(1):87-96.
- Kaplan MM. Laboratory Tests. In: Schiff L, Schiff ER. Diseases of the Liver, Philadelphia: Lippincott IB. 1987;219-60.
- Porter CJ, Curnow DH. International Union of Pure and Applied Chemistry and International Federation of Clinical Chemistry. IUPAC section ON Clinical Chemistry. Commission on Teaching of Clinical Chemistry and IFCC Committee on Education Provisional Recommendation (1979) on a scheme for a two year postgraduate course in clinical chemistry. Clin Chim Acta. 1980;103(2):239F-247F.
- World Health Organization. Obesity: preventing and managing the global epidemic. Report of a WHO Consulation. Geneva: World Health Organization, Technical Report Series, n. 894. 1998.
- Lipschitz DA. Screening for nutritional status in the elderly. Prim Care. 1994;21(1):55-67.
- Blackburn GL, Thornton PA. Nutritional assessment of the hospitalized patient. Med Clin North Am. 1979;63(5):11103-15.
- Frisancho AR. New norms of upper limb fat and muscle areas for assessment of nutritional status. Am J Clin Nutr. 1981; 349(11): 2540-5.
- Frisancho AR. Anthropometric standards for the assessment of growth and nutritional status. Ann Arbor: The University of Michigan Press, USA.1990.
- US Department of Health and Human Services; Centers for Disease Control and Prevention; National Center for Health Statistics. Anthropometric reference data for children and adults: United States, 1988-1994.Vital and Health Statistics, series 11, n. 249. 2009.
- Nishida C, Ko GT, Kumanyika S. Body fat distribution and noncommunicable diseases in populations: overview of the 2008 WHO Expert Consultation on Waist Circumference and Waist-Hip Ratio. Eur J Clin Nutr. 2010;64(1):2-5.
- Stegall MD, Everson G, Schroter G, Bilir B, Karrer F, Kam I. Metabolic complications after liver transplantation. Diabetes, hypercholesterolemia, hypertension, and obesity. Transplantation. 1995;60:1057-60.
- Richards J, Gunson B, Johnson J, Neuberger J. Weight gain and obesity after liver transplantation. Transpl Int. 2005;18(4):461-6.
- Anastácio LR, Pereira MC, Vilela EG, Lima AS, Correia MI. Overweight in liver transplant recipients. Rev Col Bras Cir. 2013;40(6):502-7.
- Reichman TW, Therapondos G, Serrano MS, Seal J, Evers-Meltzer R, Bohorquez H, et al. "Weighing the risk": Obesity and outcomes following liver transplantation. World J Hepatol. 2015;7(11):1484-93.
- Da Silva Alves V, Hack Mendes R, Pinto Kruel CD. Nutritional status, lipid profile and HOMA-IR in post-liver transplant patients. Nutr Hosp. 2014;29(5):1154-62.
- Llames L, Baldomero V, Iglesias ML, Rodota LP. Values of the phase angle by bioelectrical impedance; nutritional status and prognostic value. Nutr Hosp. 2013;28(2):286-95.