Research Article
Relapse Prevention of Lichen Slerosus in the Pediatric Phimosis Treated by Surgery
Bolla G* and Sartore G
Department of Pediatric Urology, O.C. Dolo, Italy
*Corresponding author: Bolla G, Department of Pediatric Urology, O.C. Dolo, Venice, Italy
Published: 03 Mar, 2017
Cite this article as: Bolla G, Sartore G. Relapse Prevention
of Lichen Slerosus in the Pediatric
Phimosis Treated by Surgery. Clin Surg.
2017; 2: 1326.
Abstract
Lichen sclerosus (LS) is a chronic inflammatory and progressive disease, usually located in the anogenital
area; spontaneous remission is rare. The disease is more common in females than males
(3-10F:1M) but it can also be seen in children and middle-aged men.
Objective: The paper aims to investigate the possibility to lower the relapse rate incidence in boys
surgically treated because of phimosis produced by LS.
Method: Two groups–established according to temporal succession–of 176 boys suffering
from phimosis (63.6% with lichen sclerosus in the histologic specimen) were treated by partial
circumcision and post-operative topical corticosteroid treatment. For the second group the topical
treatment was prolonged.
Results: In the second group the incidence rate of relapse of lichen on the residual prepuce was
significantly lower (1.6% vs. 5.6%).
Conclusion: The topical prolonged corticosteroid treatment appears a good therapeutic choice.
Keywords: Phimosis; Lichen sclerosus; Topical corticosteroid treatment
Introduction
Lichen sclerosus at atrophicus is a chronic inflammatory sclerotic and atrophic disease of
unknown cause that predominantly affects male and female genital skin. LS (Lichen Sclerosus) in
females may be an autoimmune disorder, in which the body’s immune system mistakenly attacks
and injures the skin. People with LS are at greater risk of developing other autoimmune disorders,
such as some types of thyroid disease, anemia, diabetes, alopecia areata and vitiligo. Malignant
degeneration has been recorded in up to 5.8% of penile LS, being controversial for such degeneration
a putative role of HPV infection; HPV has also been found in a significant number of penile LS. In
males, LS is considered to be a disease of the uncircumcised individual, although it can also persist
after circumcision. In females, the vulvar-perineal area is mainly affected, especially in middle
aged and elderly women. It was demonstrated that lichen appears as the main cause of phimosis in
childhood, much more than balanitis or iatrogenic causes.
The Authors investigated into a possible modality of relapse prevention of LS, after surgery, for
the residual foreskin.
Methods
From July 2008 to June 2016 we have treated by preputial plasty with resection of the scar
foreskin (partial circumcision) 176 boys suffering from phimosis–where the foreskin cannot be
fully retracted over the gland penis. Study occurred after having previously obtained the informed
consent from the parents and the ethics approval according to Helsinki Declaration.
Mean age at surgery was 9.2 y. and average follow-up has been 39 m. and 12 d. In the former
group of children (from July 2008 to April 2011) –53–the topical steroid treatment was remaining
five days postoperatively (once a day); in the latter (from May 2011 to June 2016) –123 children, not
only for the boys with a whitish foreskin and clear little blood-vessels- macroscopic indication on
the existence of lichen–the topical steroid treatment was extending for fifteen days (always once a
day) postoperatively. We used a gel with Fluocinolone (0.025 grams in 100 grams of product).
The statistical analysis was performing by χ-square Test.
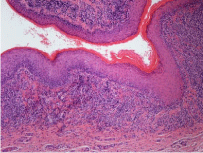
Figure 1
Figure 1
Dense lymphocytic band-like infiltrate of LS is located at the
epidermal-dermal interface, associated with basal epidermal alteration and
upward migration of inflammatory cells within epidermis. Haematoxylin and
Eosin 10x.
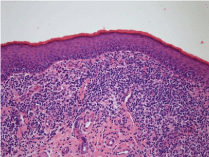
Figure 2
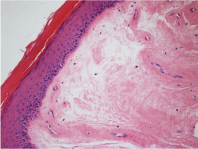
Figure 3
Figure 3
A more detailed view of edema and sclerosing late modifications
of dermis in LS. Haematoxylin and Eosin 20x.
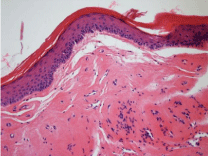
Figure 4
Results
112 boys (63.6%) showed the existence of lichen sclerosus in
the histologic specimen. For five children – 2.8% -the condition of
phimosis was coming back on the residual prepuce. In the first group
of boys –53, treated with steroid gel on the suture for 5 days only,
the relapses of phimosis were three (5.6%). In the second group of
boys–123, treated with steroid gel for fifteen days on the suture, two
were the relapses of phimosis (1.6%).
All boys with relapse (5-4.4%) have suffered from lichen sclerosus
on the foreskin. These five boys were treated by a total prepuce
resection–circumcision - ; for a child we have added a meatoplasty
because the relapse was involving the outer urethral meatus. The
lichen has been the cause of all relapses.
We have confirmed a statistically significant difference in relation
to the incidence rate of relapse between the two groups - p≤ 0.05.
Discussion
In our experience we wanted to understand the chances of relapse
prevention in boys surgically treated for phimosis caused by lichen
sclerosus. These relapses were happening exclusively in children who
showed the existence of lichen on the removed prepuce. All relapses
(2.8%) had appeared within the first three months after surgery. It’s
therefore an early condition.
The choice of extending for all boys the postoperative topical
steroid treatment on the preputial suture after the first series (5.6%
of relapse) was found to reduce the incidence rate of relapses
(1.6%). This choice was leaving apart from consideration of the wait
pertinent to histologic report. In adulthood the medical treatment with
corticosteroids for the penile lichen is accepted, also outside of the
surgical treatment [1-3].
Now it’s confirmed the main list of lichen sclerosus for causing
the scar preputial fibrosis in children [4-8]. Then it’s quite clear that
the question regards which wideness we can achieve with reference
to excision of the foreskin. We know the significance of the foreskin
in order to the immunocompetence and the peripheral sensitivity
[9,10]. For this reason we prefer a conservative treatment, with the
exclusive excision of the scar foreskin. Of course, in consequence of
the partial preservation of the prepuce, we can expect a reappearance
of phimosis. Then we have resolved, in the course of our experience,
that the extension of topical steroid treatment on the residual prepuce
finds an effective application for the sake of reducing the relapse
incidence rate.
The clinical attitude has to abide by the histopathologic pattern.
The etiology of LS is poorly understood. In females, studies
have demonstrated a link with autoimmune diseases and various
autoantibodies, whereas local factors seem to play a major pathogenetic
role in males, especially the exposure of the sensitive epithelium of
glans and prepuce to urine, particularly in uncircumcised individuals
[11]. A possible role of Borrelia infection in the development of LS
remains to be elucidated [12].
Concerning the pathological features of LS, macroscopically the
disease starts as flat, ivory to white papules that coalesce to form
plaques of varying size and shape, followed by progressive atrophy (LS
atrophicus) leading to a wrinkled, flat or depressed scar. Vulvar lesions
may have secondary lichenification due to pruritus-related scratching
and coexist with hypertrophic areas, the so-called “mixed vulvar
dystrophy”. The glans, prepuce or external meatus of prepubertal
or adolescent males may be involved by LS, resulting in phimosis or
meatal stenosis (balanitis xerotica obliterans). Histologically, in LS
there are numerous epidermotropic and dermal lymphocites CD8+
CD57+ as well as significant alteration of the extracellular matrix
such as increased hyaluronate accumulation in the broad hyalinized
dermal zone that is observed in well-established lesions.
In early ones (Figure 1) the inflammatory infiltrate is quite
heavy, superficial and band-like, mimicking lichen planus (interface
or junctional dermatitis). Other early histologic features include
basal vacuolization of the epithelium or the epidermis, followed by
fragmentation of basal membrane, epidermal atrophy, and loss of
dermal papillary elastic fibers and a broad expanding zone of subepidermal
edema (Figure 2). Later, extensive hyalinization of dermis
and subepithelial connective tissue occurs, that in later stages becomes
densely sclerotic. In these stages basement membrane thickening
becomes evident whereas inflammatory cells become more dispersed
(Figure 3 and 4). A spectrum of vascular changes occurs in LS, chiefly
represented by lymphocytic vasculitis, ranging from concentric
lymphohistiocytic infiltrate with lamination of the adventitial layer (a
feature typical of penile lesions) to a dense perivascular lymphocytic
cuff with occasional fibrin deposition in vessel walls.
Conclusion
The choice of prolonging for two weeks the topical corticosteroid treatment on the residual foreskin, after surgical treatment, in our experience appears a good behavior for relapse prevention in boys with phimosis caused by lichen sclerosus.
References
- Clouston D, Hall A, Lawrentschuk N. Penile lichen sclerosus (balanitis xerotica obliterans). BJU Int. 2011; 108: 14-19.
- Cooper SM, Arnold SJ. Patient education: Lichen sclerosus (Beyond the Basics). Up To Date. 2016.
- Depasquale I, Park AJ, Bracka A. The treatment of balanitis xerotica obliterans. BJU International. 2000; 86: 459-465.
- Bolla G, Sartore G, Longo L, Rossi C. The sclero-atrophic lichen as principal cause of acquired phimosis in pediatric age. Pediatr Med Chir. 2005; 27: 91-93.
- Mattioli G, Repetto P, Carlini C, Granata C, Gambini C, Jasonni V. Lichen sclerosus et atrophicus in children with phimosis and hypospadias. Pediatr Surg Int. 2002; 18: 273-275.
- Rossi E, Pavanello P, Franchella A. Lichen sclerosus in children with phimosis. Minerva Pediatr. 2007; 59: 761-765.
- Jasaitiene D, Valiukeviciene S, Vaitkiene D, Jievaltas M, Barduskas V, Gudinaviciene I, et al. Lichen sclerosus et atrophicus in pediatric and adult male patients with congenital and acquired phimosis. Medicina (Kaunas). 2008; 44: 460-466.
- Chalmers RJ, Burton PA, Bennett RF, Goring CC, Smith PJ. Lichen sclerosus et atrophicus. A common and distinctive cause of phimosis in boys. Arch Dermatol. 1984; 120: 1025-1027.
- Van Rossum MM, van der Avoort IA, de Hoop D, Dukel L, van der Vleuten CJ, de Hullu JA. Lichen sclerosus. Ned Tijdschr Geneeskd. 2007; 151: 1225-1231.
- Becker K. Lichen sclerosus in boys. Dtsch Arztebl Int. 2011; 108: 53-58.
- Kantere D, Alvergren G, Gillstedt M, Pujol-Calderon F, Tunback P. Preview (Epub ahead of print Sep 27, 2016) 2017, Clinical features, complications and autoimmunity in male lichen sclerosus. Acta Derm Venereol. 2016; 97.
- Weedon D. In: Weedon’s skin pathology. Churchill Livingstone Elsevier. 2010; 313-316.