Case Report
Liver Transplantation for Hepatic Epithelioid Hemangioendothelioma Case Report and Review of the Literature
Mihaylov V*, Kostadinov R, Vasilevski I, Takorov I, Simonova M, Katzarov K, Odiseeva E and Vladov N
Department of Transplant Surgery, Military Medical Academy, Bulgaria
*Corresponding author: Vassil Mihaylov, Department of Transplant Surgery, Military Medical Academy, Sofia, Bulgaria
Published: 03 Mar, 2017
Cite this article as: Mihaylov V, Kostadinov R, Vasilevski
I, Takorov I, Simonova M, Katzarov K,
et al. Liver Transplantation for Hepatic
Epithelioid Hemangioendothelioma
Case Report and Review of the
Literature. Clin Surg. 2017; 2: 1322.
Abstract
Hepatic epithelioidhemangioendothelioma (HEHE) is a rare vascular tumor of the liver, with less than 500 cases reported worldwide. It has indolent course and often presents with unspecific symptoms. Unlike other primary liver tumors, it does not arise in the background of chronic liver disease. The definitive diagnosis is difficult and often necessitates percutaneous liver biopsy. Another feature of HEHE is its variable and unpredictable prognosis. Due to the rarity of this condition, currently there is no accepted treatment approach. Excellent results are achieved through the surgical modalities-liver resection (LR) and liver transplantation (LT), with high survival rates and disease free survival (DFS). Other therapeutic options include chemo/radiotherapy regiments and transcatheter arterial chemoembolization (TACE). We present a case report of 33 years old male with multiple bilobar hepatic epithelioid hemangioendothelioma who underwent orthotopic liver transplantation with excellent long-term outcome.
Introduction
Hepatic epithelioidhemangioendothelioma (HEHE) is a rare neoplasm of vascular origin, which has histologic appearance between hemangioma and hemangiosarcoma and unpredictable clinical course [1,2]. Although there is no accepted therapeutic approach, surgical therapy is currently the mainstay of treatment. Liver resection (LR) is a viable option, but it is seldom possible, because of the advanced stage of the tumor at the time of diagnosis [3,4]. The unresectable cases are candidates for liver transplantation with high survival rates and disease free survival (DFS). Other therapeutic options include chemo/radiotherapy regiments and transcatheter arterial chemoembolization (TACE).
Case Presentation
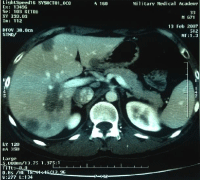
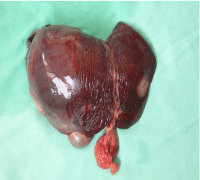
We present a case of 33- year old male, who was referred to the unit with multiple bilobar liver lesions (Figure 1) and no evidence for any primary tumor. The patient had no other comorbidities, apart from ichthyosis vulgaris of the skin. The laboratory results were unremarkable and the tumor markers (AFP, CEA and CA19-9) were within reference values. The histology and immunehistochemistry of percutaneous liver biopsy revealed epithelioidhemangioendothelioma. A diagnostic laparoscopy was performed, showing no extra hepatic disease. The bilobar involvement and the localization of the lesions, classified the case as unresectable. The patient was listed for liver transplantation and within a month he was transplanted with full liver graft from a deceased donor. The post-operative period was uneventful. Two months after the transplantation an anastomotic biliary stricture was identified, that was successfully managed with endoscopic stent placement. No adjuvant chemotherapy was administered. The patient was prospectively followed. Ten years after transplantation the patient is doing well and has no signs of recurrence (Figure 1 and 2).
Discussion
Epithelioidhemangioendothelioma is a rare neoplasm of endothelial origin. It was first described
in soft tissue by Weiss and Enzinger in 1982 [5]. Since then there have been many reports of this
tumor with different localization, including head and neck, brain, bones, lung, spleen, etc. Ishak was
the first to report a series of 32 patients with hepatic epithelioidhemangioendothelioma [1]. HEHE
has low incidence rates, affecting less than 1 per one million people with a male to female ratio of
2:3 [4]. According to the literature review, less than 500 cases are reported worldwide. HEHE can occur at any age, although the tumor is not common in children [4,6].
Unlike other primary liver tumors, it does not arise in the background
of chronic liver disease. Although there is no specific cause, some of
the suggested risk factors include oral contraceptives, vinyl chloride,
major liver trauma, thorotrast and others [7-10].
HEHE is a low-grade malignancy with unpredictable clinical
course. It has a propensity for angiocentric growth, obliterating the
lumen of the vessel and spreading centrifugally into the surrounding
tissue, inducing fibrotic response. The distinction between HEHE
and other malignant lesions may be quite challenging [2,11-15].
The definitive diagnosis of this tumor is based on positive immunehistochemical
staining for factor VIII –related antigen (FVIII-RAg)
and specific endothelial markers, such as CD31 and CD34 [4,5,15]. By
the time of diagnosis, the tumor is almost always multinodular and
spread into both liver lobes [3,4]. It has long been debated, whether
this is a result of multiple, synchronously occurring nests of tumor
cells or represents an odd pattern of tumor metastasis from a single
source. Recent advances demonstrate the monoclonal origin of the
lesions, thus proving it is a result of metastatic spread [15,16]. The
presence of extrahepatic disease varies among different series between
17% and 37% [3,4,17,18].
Imaging modalities recognize two distinct patterns of HEHE–
nodular and diffuse. The nodular type can manifest as multiple,
often bilobar nodular masses with subcapsular spread. The diffuse
type represents a more advanced stage of the disease, with formation
of confluent lesions. Common radiological signs of HEHE include
capsular retraction, presence of intralesional calcifications and
specific patterns of perfusion on contrast series -peripheral and
delayed enhancement, and target sign appearance [19,20]. Rarely, this
tumor can manifest as a solitary, often subcapsular node, representing
an early stage of the disease. The progression of a single nodule to
multifocal spread has been documented, during follow-up [2,20,21].
The clinical manifestation ranges from asymptomatic state to
hepatic failure [22-24]. Many cases are discovered accidentally, during
routine examination. The most common symptoms include right
upper quadrant pain, anorexia, weight loss, weakness, hepatomegaly
and jaundice [3,4]. The laboratory findings are unspecific and most
commonly include liver test abnormalities with mildly distorted
values. However, the biochemical analysis may show no deviation.
The commonly assessed tumor markers–CEA, CA19-9 and AFP are
almost always negative, or slightly elevated [4].
Hepatic epithelioidhemangioendothelioma is a tumor with
variable and unpredictable prognosis. The assessment of clinical or
pathological criteria offers no benefit in predicting the outcome. The
clinical course may range from a relatively benign one, with favorable
outcome and prolonged survival, even in the setting of no treatment
[2-4,25], to rapid progression and death [24,26]. It is remarkable that
the disease evolution does not seem to depend on the degree of tumor
spread, with reported long-term survival, in some cases, even in the
presence of metastatic disease – a behavior, which resembles that of
the neuro-endocrine tumors (NETs) [27].
The extremely low incidence of HEHE is a serious setback for
conducting randomized comparative analyzes and determining the
best treatment approach. The inability to predict the disease outcome
is a further impediment to this process. The major portion of the
available publications consists of retrospectively analyzed clinical
cases and reports with small sample sizes. This scattered, non-uniform
data demands careful interpretation of the conclusions reached, due
to the possibility of statistical bias. The demographic characteristics
and results from some of the papers are summarized in Table 1.
In 2006 Mehrabi et al. [4] published a review, encompassing the
reported cases of HEHE for the period 1984-2005. This is the largest
survey on the topic to date and contains data for 402 patients. HEHE
was multifocal in 86% of the 306 cases with sufficient data for the
analysis, and extrahepatic spread was observed in 36%. The most
common treatment approach, used in 128 patients (44.8%), was
liver transplantation (LT), followed by no treatment in 71 patients
(24.8%), chemotherapy or radiotherapy in 60 patients (21%) and
liver resection (LR) in 27 patients (9.4%). In the meta-analysis the
survival data was available for 253 patients. The surgical therapies–
liver resection and liver transplantation were associated with the
best results, with 5-year survival of 75% and 55.8% respectively. The
survival rates decreased markedly in the chemotherapy/radiotherapy
group and in the no treatment group, with 5-year survival of 30%
and 4.5% respectively. It should be noted, that whereas the LR group
had the highest OS, most of the patients weren’t eligible for radical
resection due to the multifocal tumor spread in the liver. Limited
extrahepatic disease was not considered an absolute contraindication
to surgical therapy, due to the reported long survival of patients with
systemically advanced HEHE.
Analyzing the data from the ELTR (European Liver Transplant
Registry), in a large multicenter study, Lerut et al. [3] managed to compile detailed information about the long-term follow-up of
59 patients, who had undergone LT for HEHE for the period June
1989 to June 2004. The ELTR report validated the place of liver
transplantation in the treatment of HEHE with 1-, 5- and 10- year
overall survival of 93%, 83% and 72%, respectively. The analysis
showed also, that pre-LT tumor treatment (18 patients), the presence
of lymph node invasion (18 patients) or the presence of extrahepatic
disease (10 patients) did not influence significantly the survival
rates. Only the presence of microvascular, or combined micro-/
macrovascular invasion negatively affected the survival. Lerut et al. [3]
demonstrated excellent 1-, 5- and 10-year disease free survival (DFS)
rates: 90%, 82% and 64%, which were not significantly influenced by
the presence of LN invasion, extrahepatic disease, pre-LT treatment
or vascular invasion. This marker of an advanced neoplastic process
should not be considered an absolute contraindication and warrant
careful preoperative staging and patient evaluation.
However, in 2009 the Pittsburg group identified the presence of
extrahepatic disease, beyond the portal lymph nodes, as a predictor
of poor outcome in their series of 25 patients [18]. In this largest
single-center experience, the patients were divided into four
groups, depending on the therapeutic strategy - 17 underwent LT,
4 –transcatheter arterial chemoembolization (TACE), 2 patients
underwent liver resection and 2 –TACE, followed by LT. Cardinal et
al. [18] concluded that the difference in survival was not statistically
significant between the LT (172 months) and the TACE group (83
months), p=0.98. There was a tendency towards better outcome of the
patients with extrahepatic disease, treated with TACE (83months),
than those, treated with LT or LR (38.8 months), p=0.12. Presence
of angiolymphatic invasion could not be identified as a predictor
of worse prognosis. This study demonstrated the value of TACE in
advanced cases, where LR or LT were not feasible.
Grotz et al. [17] published a paper, analyzing the results of 30
patients, treated for HEHE at Mayo Clinic. The team assessed a
number of pathological and morphological features, including the
disease type – nodular or diffuse, the number of tumor nodules, size
of nodules and the number of hepatic segments involved in attempt to
identify important predictors of favorable prognosis. Those patients
with nodular disease pattern (p=0.01) and largest tumor nodule ≤ 10
cm (p=0.003) had improved DFS. The number of tumor nodules ≤ 10
approached significance (p=0.052) as a predictor of better outcome.
The reports published by Rodriguez [30] and Nudo [29]
summarize the American and Canadian experience with LT for
HEHE with overall results showing no difference as compared to one
another and the European experience [3].
A recent study by Remiszewski et al. [31] described a single institution experience with 1234 liver transplantations, performed
for the period 1989 – 2013 and compared the outcomes in three
separate cohorts–HEHE (10 patients), HCC (155) and LTs for other
indications (1069). The overall survival at the end of the follow-up
period for the HEHE group was 87.5%, which was superior to the
OS of the HCC group (54.3%) and the group with LTs for other
indications (76.3%).
Wang et al. [32] published a report of 33 patients, who underwent
treatment for HEHE, between 2004 and 2011, with various methods.
Seventeen underwent liver resection, 12 had TACE alone, 3 patients
were treated with TACE and LR and 1 patient underwent LT. There
was no significant difference between the overall survival of the TACE
and LR arms. The presence of symptoms was identified as a predictor
of worse prognosis. Older age and elevated CA19-9 were implicated
to have negative effect on the overall survival.
In a recent review, Zhao et al. [33] compared the Western and
Chinese experience in the treatment of HEHE. Fifty patients from
China were identified and included in the report. The most used
treatment approach in the Chinese population was liver resection
(45.7%), followed by palliative treatment (34.3%). TACE and liver
transplantation were utilized in 14.3% and 5.7% of the patients
respectively. The authors did not detect significant difference in the
overall survival between the four treatment groups (p=0.74), although
there was a trend towards better survival with the surgical approaches.
Extrahepatic spread of the disease was not associated with worse
outcome, but the presence of symptoms (p=0.076), elevated tumor
markers (p=0.027) and the diffuse type HEHE (RR=12.17, p=0.016)
were identified as risk factors for poorer outcome.
Hepatic epithelioidhemangioendothelioma is a rare vascular
tumor. Nevertheless, a wide variety of treatment approaches are
described in the literature. Chemotherapy and radiotherapy are
conservative modalities, which are mainly used as a means of
palliation or supplementary treatment in the adjuvant or the neoadjuvant
setting. Many agents have been described in the literature,
mostly chosen for their anti-angiogenic properties, including
thalidomide, doxorubicin, epirubicin, gemcitabine, interferon, etc.
[4]. The effectiveness of these modalities in improving survival is still
not clear. Given the indolent course of the tumor, associated with
long survival, even in systemically advanced cases, comparative trials
need to be designed to elucidate the place of chemo/radiotherapy
in treatment of HEHE. Transcatheter arterial chemoembolization
(TACE) is a perspective method, which, according to some reports
offers comparable survival to the surgical modalities [18,32,33].
Cardinal et al. [18] suggested that it leads to improved survival, with
less treatment-related complications, compared to LT and LR, in the
case of HEHE with extrahepatic spread.
The surgical therapy has consistently provided satisfactory
results and is currently the method of choice. Liver transplantation
and radical liver resection offer comparable results [4,17,33-35] with
excellent long-term outcome. Many authors agree, that whenever
possible, radical liver resection should be attempted [2,4,6,35,36].
However, others disagree with that statement, because of the
observed more aggressive behavior of the tumor after liver resection
[37,38]. According to Ben-Haim [38] at the time of resection the
tumor has already spread microscopic seedings across the liver, not
visible on imaging studies. Liver regeneration after resection is largely
dependent on angiogenesis. The promotion of vascular proliferation
thus may stimulate the neoplastic growth and result in quick
deterioration and death.
It should be noted, that by the time of diagnosis HEHE is
most often bilobar and not suitable for radical liver resection [2,3].
Liver transplantation has proven an effective treatment of HEHE
with similar or even superior survival to LT for other indications
[31,39,40]. Some authors state that limited extrahepatic disease is
no contraindication to liver transplantation [2-4,27,38]. Due to the
protracted course of the disease, long-term survival can be expected
even in the event of disease recurrence. On that basis, Lerut et al. [3]
advocate an aggressive approach in such cases.
Figure 1
Figure 2
Table 1
Conclusion
Hepatic epithelioidhemangioendothelioma is a treatable disease. Good results can be achieved when an early diagnosis is made, followed by complex assessment of the tumor and patient characteristics by a multidisciplinary team and selection of the most appropriate treatment modality. Liver transplantation and radical liver resection offer the best chance for long-term survival; however the latter is seldom possible due to bilobar hepatic involvement. Patient follow-up and aggressive approach toward disease recurrence are key factors for long-term survival.
References
- Ishak KG, Sesterhenn IA, Goodman ZD, Rabin L, Stromeyer FW. Epithelioid hemangioendothelioma of the liver: a clinicopathologic and follow-up study of 32 cases. Hum Pathol. 1984; 15: 839-852.
- Makhlouf HR, Ishak KG, Goodman ZD. Epithelioid hemangioendothelioma of the liver: a clinicopathologic study of 137 cases. Cancer. 1999; 85: 562-582.
- Lerut JP, Orlando G, Adam R, Schiavo M, Klempnauer J, Mirza D, et al. The place of liver transplantation in the treatment of hepatic epitheloid hemangioendothelioma: report of the European liver transplant registry. Ann Surg. 2007; 246: 949-957.
- Mehrabi A, Kashfi A, Fonouni H, Schemmer P, Schmied BM, Hallscheidt P, et al. Primary malignant hepatic epithelioid hemangioendothelioma: a comprehensive review of the literature with emphasis on the surgical therapy. Cancer. 2006; 107: 2108-2121.
- Weiss SW, Enzinger FM. Epithelioid hemangioendothelioma: a vascular tumor often mistaken for a carcinoma. Cancer. 1982; 50: 970-981.
- Lauffer JM, Zimmermann A, Krähenbühl L, Triller J, Baer HU. Epithelioid hemangioendothelioma of the liver. A rare hepatic tumor. Cancer. 1996; 78: 2318-2327.
- Dean PJ, Haggitt RC, O'Hara CJ. Malignant epithelioid hemangioendothelioma of the liver in young women. Relationship to oral contraceptive use. Am J Surg Pathol. 1985; 9: 695-704.
- Darras T, Moisse R, Colette JM. Epithelioid hemangioendothelioma of the liver. J Belge Radiol. 1988; 71: 722-723.
- Banerjee B, Rennison A. Epitheloid haemangioendothelioma of liver: a vascular tumour easily mistaken for metastatic carcinoma on ultrasound imaging. Br J Radiol. 1992; 65: 611-613.
- Soslow RA, Yin P, Steinberg CR, Yang GC. Cytopathologic features of hepatic epithelioid hemangio-endothelioma. Diagn Cytopathol. 1997; 17: 50-53.
- Neofytou K, Andreas Chrysochos, Nikolas Charalambous, Menelaos Dietis, Christos Petridis, Charalampos Andreou, et al. Hepatic epithelioid hemangioendothelioma and the danger of misdiagnosis: report of a case. Case Rep Oncol Med. 2013; 2013: 243939.
- Bismuth B, Castel H, Boleslawski E, Buob D, Lambert M, Declerck N, et al. Primary sarcoma of the liver and transplantation: a case study and literature review. Rare Tumors. 2009; 1: e31.
- Cacciatore M, Dei Tos AP. Challenging epithelioid mesenchymal neoplasms: mimics and traps. Pathology. 2014; 46: 126-134.
- Gupta R, Mathur SR, Gupta SD, Durgapal P, Iyer VK, Das CJ, et al. Hepatic epithelioid hemangioendothelioma: A diagnostic pitfall in aspiration cytology. Cytojournal. 2010; 6: 25.
- Antonescu C. Malignant vascular tumors--an update. Mod Pathol. 2014; 27: S30-S38.
- Errani C, Yun Shao Sung, Lei Zhang, John H Healey, Cristina R Antonescu. Monoclonality of multifocal epithelioid hemangioendothelioma of the liver by analysis of WWTR1-CAMTA1 breakpoints. Cancer Genet. 2012; 205: 12-17.
- Grotz TE, David Nagorney, John Donohue, Florencia Que, Michael Kendrick, Michael Farnell, et al. Hepatic epithelioid haemangioendothelioma: is transplantation the only treatment option? HPB (Oxford). 2010; 12: 546-553.
- Cardinal J, de Vera ME, Marsh JW, Steel JL, Geller DA, Fontes P, et al. Treatment of hepatic epithelioid hemangioendothelioma: a single-institution experience with 25 cases. Arch Surg. 2009; 144: 1035-1039.
- Bruegel M, Muenzel D, Waldt S, Specht K, Rummeny EJ. Hepatic epithelioid hemangioendothelioma: findings at CT and MRI including preliminary observations at diffusion-weighted echo-planar imaging. Abdom Imaging. 2011; 36: 415-424.
- Kim EH, Rha SE, Lee YJ, Yoo IeR, Jung ES, Byun JY. CT and MR imaging findings of hepatic epithelioid hemangioendotheliomas: emphasis on single nodular type. Abdom Imaging. 2015; 40: 500-509.
- Chen Y, Yu RS, Qiu LL, Jiang DY, Tan YB, Fu YB, et al. Contrast-enhanced multiple-phase imaging features in hepatic epithelioid hemangioendothelioma. World J Gastroenterol. 2011; 17: 3544-3553.
- Demir L, Can A, Oztop R, Dirican A, Bayoglu V, Akyol M, et al. Malignant epithelioid hemangioendothelioma progressing after chemotherapy and Interferon treatment: a case presentation and a brief review of the literature. J Cancer Res Ther. 2013; 9: 125-127.
- Dietze O, Davies SE, Williams R, Portmann B. Malignant epithelioid haemangioendothelioma of the liver: a clinicopathological and histochemical study of 12 cases. Histopathology. 1989; 15: 225-237.
- Komatsu Y, Koizumi T, Yasuo M, Urushihata K, Yamamoto H, Hanaoka M, et al. Malignant hepatic epithelioid hemangioendothelioma with rapid progression and fatal outcome. Intern Med. 2010; 49: 1149-1153.
- Otrock ZK, Al-Kutoubi A, Kattar MM, Zaatari G, Soweid A. Spontaneous complete regression of hepatic epithelioid haemangioendothelioma. Lancet Oncol. 2006; 7: 439-441.
- Harada J, Yoshida H, Ueda J, Mamada Y, Taniai N, Mineta S, et al. Malignant hepatic epithelioid hemangioendothelioma with abdominal pain due to rapid progression. J Nippon Med Sch. 2011; 78: 246-251.
- Marino IR, Satoru Todo, Andreas G. Tzakis, Goran Klintmalm, Michael Kelleher, Shunzaburo Iwatsuki, et al. Treatment of hepatic epithelioid hemangioendothelioma with liver transplantation. Cancer. 1988; 62: 2079-2084.
- Madariaga, JR, Marino IR, Karavias DD, Nalesnik MA, Doyle HR, Iwatsuki S, et al. Long-term results after liver transplantation for primary hepatic epithelioid hemangioendothelioma. Ann Surg Oncol. 1995; 2: 483-487.
- Nudo CG, Yoshida EM, Bain VG, Marleau D, Wong P, Marotta PJ, et al. Liver transplantation for hepatic epithelioid hemangioendothelioma: the Canadian multicentre experience. Can J Gastroenterol. 2008; 22: 821-824.
- Rodriguez JA, Becker NS, O'Mahony CA, Goss JA, Aloia TA. Long-term outcomes following liver transplantation for hepatic hemangioendothelioma: the UNOS experience from 1987 to 2005. J Gastrointest Surg. 2008; 12: 110-116.
- Remiszewski P, Szczerba E, Kalinowski P, Gierej B, Dudek K, Grodzicki M, et al. Epithelioid hemangioendothelioma of the liver as a rare indication for liver transplantation. World J Gastroenterol. 2014; 20: 11333-11339.
- Wang LR, Zhou JM, Zhao YM, He HW, Chai ZT, Wang M, et al. Clinical experience with primary hepatic epithelioid hemangioendothelioma: retrospective study of 33 patients. World J Surg. 2012; 36: 2677-2683.
- Zhao XY, Rakhda MI, Habib S, Bihi A, Muhammad A, Wang TL, et al. Hepatic epithelioid hemangioendothelioma: A comparison of Western and Chinese methods with respect to diagnosis, treatment and outcome. Oncol Lett. 2014; 7: 977-983.
- Oshima N, Terajima H, Hosotani R. Surgical Therapy for a Solitary Form of Hepatic Epithelioid Hemangioendothelioma: A Long-Term Survival Case. Case Rep Gastroenterol. 2009; 3: 214-221.
- Langrehr JM, Petersen I, Pfitzmann R, Lopez-Hänninen E. [Malignant epithelioid hemangioendothelioma of the liver. Results of surgical treatment strategies]. Chirurg. 2005; 76: 1161-1167.
- Mosoia L, Mabrut JY, Adham M, Boillot O, Ducerf C, Partensky C, et al. Hepatic epithelioid hemangioendothelioma: long-term results of surgical management. J Surg Oncol. 2008; 98: 432-437.
- Penn I. Hepatic transplantation for primary and metastatic cancers of the liver. Surgery. 1991; 110: 726-734.
- Ben-Haim M, , Roayaie S, Ye MQ, Thung SN, Emre S, Fishbein TA, et al. Hepatic epithelioid hemangioendothelioma: resection or transplantation, which and when? Liver Transpl Surg. 1999; 5: 526-531.
- Hoti E, Adam R. Liver transplantation for primary and metastatic liver cancers. Transpl Int. 2008; 21: 1107-1117.
- Yokoyama I, Todo S, Iwatsuki S, Starzl TE. Liver Transplantation in the Treatment of Primary Liver Cancer. Hepatogastroenterology. 1990; 37: 188-193.