Case Report
Surgical Management of Orbital Subperiosteal Abscess Caused by Chronic Rhinosinusitis in an Adult Patient
Seok-Chan Hong* and Donghyuk Im
Department of Otorhinolaryngology-Head & Neck Surgery, Konkuk University School of Medicine, South Korea
*Corresponding author: Seok-Chan Hong, Department of Otorhinolaryngology-Head & Neck Surgery, Konkuk University School of Medicine, Seoul, South Korea
Published: 13 Feb, 2017
Cite this article as: Seok-Chan Hong, Donghyuk Im.
Surgical Management of Orbital
Subperiosteal Abscess Caused by
Chronic Rhinosinusitis in an Adult
Patient. Clin Surg. 2017; 2: 1307.
Abstract
Orbital subperiosteal abscess caused by chronic rhinosinusitis is less common in adults than in children. The patient whom we treated suffered from right periorbital pain, periorbital swelling and diplopia. He underwent functional endoscopic sinus surgery (FESS) after 2 weeks of antibiotics treatment. After operation, the patient recovered well and shows no symptom of visual disturbance and periorbital pain.
Introduction
Orbital subperiosteal abscess is known as a complication of chronic rhinosinusitis more commonly in children. It can result in the dangerous complications such as meningitis, cavernous sinus thrombosis, subdural empyema, brain abscess, blindness, and death [1]. We report a rare case of orbital subperiosteal abscess in 44 year old male patient.
Case Presentation
A 44 year old male visited the outpatient department of Otorhinolaryngology suffering from right periorbital pain for 2 months. He also had diplopia (Figure 1a). The patient had no known medical history, and complained of diplopia and periorbital pain on the right side. Physical examination showed the erythematous swelling on right upper eyelid associated with frontal area swelling with tenderness (Figure 1b). Further evaluation through CT and MRI revealed near total opacification of right frontoethmoid sinuses with the peripheral rim-enhancing hypodense lesion, containing air bubbles, suspicious bone thinning and destruction of posterior wall of right frontal sinus and adjacent focal parenchymal enhancement in the basal frontal lobe. Subperiosteal abscess in right orbital and medial canthal area was also detected (Figure 2). Under the impression of right chronic rhinosinusitis with orbital subperiosteal abscess, the patient was admitted and treated with antibiotics, the combination of a third-generation cephalosporin, clindamycin and metronidazole. After administration of intravenous antibiotics, the patient’s condition improved. On the 15th day of hospitalization, the patient underwent surgical treatment of right functional endoscopic sinus surgery (FESS) including middle meatal antrostomy, intranasal ethmoidectomy, frontal sinusotomy, sphenoidotomy and incision and drainage I of subperiosteal abscess. During the operation, a great amount of pus discharge in ethmoid sinus was detected and removed (Figure 3a). There were no perioperative complications and hospital stay was 18 days. At 6 days after operation, his diplolpia symptom disappeared (Figure 3b). No suspicious signs of recurrence appeared during the 1 month follow up.
Figure 1
Figure 1
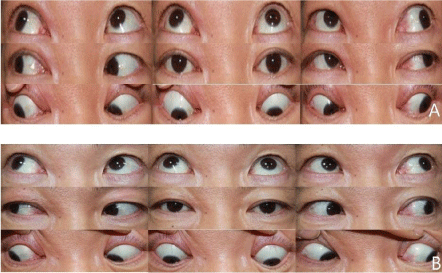
Figure 1a: Photograph of 9-gazeon the 11th day of hospitalization, right trochlear nerve palsy associated with chronic rhinosinusitis was identified.
Figure 1b: Photograph of 9-gaze after 6 days of operation. Eye movement of all directions was normal.
Figure 2
Figure 2
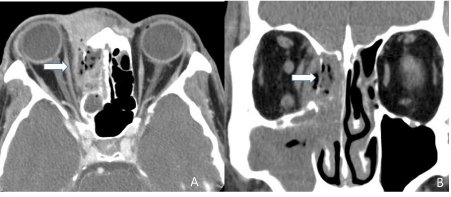
Enhanced orbital CT image. Near total opacification of right frontoethmoid sinuses with the peripheral rim-enhancing hypodense lesion, containing air bubbles (white arrow). A: axial view, B: coronal view.
Figure 3
Figure 3
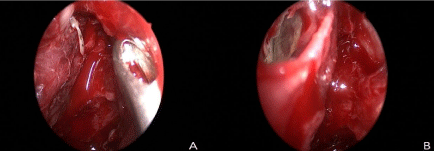
Figure 3a: Intra operative image. Whitish pus discharge was drained from right orbital subperiosteal abscess pocket to nasal cavity.
Figure 3b: After incision and drainage of right orbital subperiosteal abscess, empty space was shown in the periorbital area.
Discussion
The orbit is vulnerable to adjacent spread of infection from the
sinuses where it is surrounded on three sides. Rhinosinusit is causes
about 75% of orbital infections including subperiosteal abscess [2].
Inflammation may spread to the orbit through dehiscence of its bony
walls or by means of interference with venous drainage of the orbital
contents. The many direct networks between the orbital veins and the
paranasal veins facilitate this spread [3]. In a case of orbital infection,
clinical examination, consultation with ophthalmology department
and prompt treatment should be applied. Since any delay can result
in serious complications, such as cavernous sinus thrombosis, partial
or complete visual loss, frontal abscess, meningitis, osteomyelitis, or
even death.
Orbital complications such as orbital subperiosteal abscess are
more frequent in children than in adults. It is directly related to the
close anatomical relations between the paranasal sinuses and orbital contents [4]. The nasal cavity of children is narrower and its mucosa
is tenderer than that of adults; thus, the sinuses are easily blocked by
edematous mucosa during an acute infection, and the infection can
spread from sinuses to the orbit [5].
In this case, the adult patient underwent FESS, because the
antibiotics were not enough to treat the disease. In conclusion, the
clinician should always be aware that adult patient with chronic
rhinosinusitis might be accompanied by orbital subperiosteal abscess.
When medical treatment alone cannot cure the orbital subperiosteal
abscess completely, surgical intervention should be considered.
References
- Smith JM, Bratton EM, Dewitt P, Davies BW, Hink EM, Durairaj VD. Predicting the need for surgical intervention in pediatric orbital cellulitis. Am J Ophthalmol. 2015; 158: 387-394.
- Schramm VL Jr, Curtin HD, Kennerdell JS. Evaluation of orbital cellulitis and results of treatment. Laryngoscope. 1982; 92: 732-738.
- Chandler JR, Langenbrunner DJ, Stevens ER. The pathogenesis of orbital complications in acute sinusitis, Laryngoscope. 1970; 80: 1414-1428.
- Dewan MA, Meyer DR, Wladis EJ. Orbital cellulitis with subperiosteal abscess: demographics and management outcomes. Ophthal Plast Reconstr Surg. 2011; 27: 330-332.
- Sultesz M, Csakanyi Z, Magoros T, Farkas Z, Katona G. Acute bacterial rhinosinusitis and its complications in our pediatric otolaryngolgical department between 1997 and 2006. Int J Pediatr Otorhinolaryngol. 2009; 73: 1507-1512.