Case Report
Bilateral Hydrothorax after Left Internal Jugular Venous Catheterization in Infant
Rachid Khemakhem1*,Muhammad Riazulhaq1, Refeat Med Sadok1 and Hamdan Al Ghamdi2
1Department of Pediatric Surgery, King Faycal Medical Complex, KSA
2Department of Pediatric ICU, Children Hospital, KSA
*Corresponding author: Rachid Khemakhem, Department of Pediatric Surgery, King Faycal Medical Complex, Taif, Al Sadad, Shahar Street, 21944,Taif City, Saudi Arabia
Published: 10 Feb, 2017
Cite this article as: Khemakhem R, Riazulhaq M, Sadok
RM, Ghamdi HA. Bilateral Hydrothorax
after Left Internal Jugular Venous
Catheterization in Infant. Clin Surg.
2017; 2: 1301.
Abstract
In intensive care units, central venous catheters are frequently used to resuscitate ill patients by administration of intra-venous fluids, medication, and giving parenteral nutrition. But these
devices are source of complications that can sometimes be life threatening. We describe a case of
pleural effusion that appears many days after internal jugular central line insertion and discuss the
mechanism and management of this serious complication.
Keywords: Central line; Internal jugular vein; Pleural effusion, Infant
Case Presentation
We report the case of a 3 months old female, with history of intrauterine growth restriction, no history of chronic constipation, who was admitted 4 days back for fever and poor feeding. These symptoms have been related to infection and the child was managed by empiric triple antibiotic with an initially improvement... Suddenly, this patient develops huge abdominal distension, bilious vomiting and continuous crying. At the clinical examination the child was lethargic, septic, pale and dehydrated. Abdomen is distended and tender. The nasogastric tube gives fecal fluid. Rectum was empty with only bloody mucus. The abdominal X-ray shows a moderate distension of the small intestine with ascites and air-fluid levels, there is no pneumatocele or pneumoperitoneum. At biology there is anemia with Hb=7.5 gm/dl, platelet was 26 000, hyponatremia at 127 mmol/l and urea is 25 gr/ml. The abdominal ultrasound shows distended bowel loops with a thick wall and moderate amount of turbid intra-peritoneal free fluid. The child was intubated, sedated and placed under mechanical ventilation. After rapid resuscitation and transfusion, an exploratory laparotomy was performed. It shows the appearance of necrotizing enterocolitis of the terminal ileum and right colon without perforation, a proximal ileostomy with peritoneal toilet and drainage was performed. A left internal jugular central venous catheter size 4 fr was inserted surgically with open technic uneventful. In post-operative period, the child remained under mechanical ventilation, triple antibiotic (vancomycin, meropenem, and flagyl), inotropes and parenteral nutrition. Chest radiography (Figure 1) showed a central line in place in the superior vena cava. The evolution was progressively favorable, the stoma starts to run 3rd postoperative day, the nasogastric tube no longer brings bile, and abdomen becomes gradually soft, lax and painless. The child is still under NPO and on parenteral nutrition; he was extubated at day 5 post op. On 7th day post op patient becomes polypneic with inter-costal retraction, hypoxic and febrile. Pulmonary auscultation shows diminution of breath sounds with some crepitation in left hemi-thorax, and chest radiography shows bilateral pleural effusion mainly in the left side. The child was intubated and mechanically ventilated. Pleural puncture brings clear serous fluid rivalta negatif with high level of glucose. A chest tube was than inserted and brings back 90 cc liquid. The central line was closed then withdrawn and two peripheral lines were placed (Figure 2). Evolution was marked by the progressively healing of the pleural effusion and the patient was extubated after three days. One month later closure of the ileostomy was performed after verification of the permeability of the distal ileum and colon.
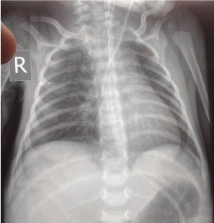
Figure 1
Figure 1
Chest x rays after left jugular CL insertion show CL well placed in the superior veina cava.
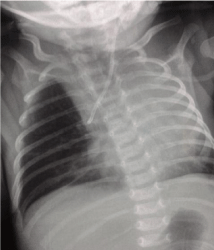
Figure 2
Figure 2
Chest x rays show left pleural effusion and the tip of the central line migrating to the right side.
Discussion
Intra-venous central line is an important devise for the management of severely ill patients in
the ICU for delivering fluids, nutrients, medication and monitoring the volume status. The correct
position of the central line is usually confirmed by perioperative fluoroscopy or postoperative chest
X-ray. But despite the advances made in the design, material of the catheter and the technique of
insertion, still there are many complications that can happen at the time of insertion of this devises
or later on [1].
These complications can be immediate or delayed. Acute
complications are usually mechanical such as pneumothorax,
hemothorax or arterial puncture. They are more frequent and occur in
up to 3% of cases [1]. Delayed complications are mostly infection and
thrombosis of the central line, less frequently pleural and pericardial
effusions or even cardiac tamponade [2,3].
Pleural effusion following central line insertion is rarely reported.
It account for about 0.5% of known complications related to this
procedure and is very uncommon to be bilateral [2]. The incidence
of this complication is much lower with jugular vein than with the
subclavian route and in man than in woman [1,4].
Generally, catheterization via the left internal jugular vein results
in more malposition and vascular perforation than a catheter placed
from the right internal jugular vein. This is because the right internal
jugular vein runs into the right brachiocephalic vein in a fairly
straight course whereas the left internal jugular vein forms a greater
bend when it becomes in the left brachiocephalic vein [1,5,6]. In this
way, the catheter is lying against the right lateral wall of the superior
vena cava at 45 degrees. This close contact of the catheter tip with
the vein wall leads to endothelial cell damage and then adherence
of platelets and activation of the coagulation cascade. The resulting
thrombus fosters attachment of the catheter tip to the vein wall,
causing irritation of the endothelial cell and osmotic injury. Through
the damaged lining, fluid can diffuses into the pleural cavity forming
an effusion [7,8].
Bilateral effusion is due to passage of the liquid from a displaced
catheter into the mediastinum and then into both pleural cavities via
anatomical communications between them [5].
An important differential diagnosis in this situation is chylothorax,
due to direct injury of the thoracic canal during central line insertion.
Biochemical analysis of the pleural fluid must be done to compare
the electrolyte and glucose profile with the infused fluid. Chylothorax
can be confirmed by the presence of chylomicrons with high levels
of triglycerides and the absence of large quantities of glucose or
electrolytes. A ratio of pleural fluid glucose to serum glucose of >1
suggests that the effusion may be caused by the infusion fluid [6].
Other reviews confirmed the hazards of delayed diagnosis of
hydrothorax from jugular vein canulation. The patients typically
presented with symptoms of breathlessness or chest discomfort at
about 2.9±0.8 days (ranging from 1 to 7 days) after catheter insertion.
The pleural fluid aspirated appeared transudative with variable
glucose concentrations [1,7,8].
Many factors have been advocated to explain vein wall erosion
- The fixation of the catheter to the skin allow the back and forth movement of the tip against the venous wall combined with head and neck motion.
- A stiff catheter in the left internal jugular vein takes a curved course to the SVC bringing the catheter tip into close proximity of the wall of SVC.
- High acidity, alkalinity and osmolality of the infused liquids may contribute to the erosion, e.g., total parenteral nutrition, antibiotics infusion (vancomycin) and sodium bicarbonate.
- Poor nutritional state of this sick patients resulting in poor tissue condition.
- Female patients have higher incidence may be due to a smaller veins [1].
The incidence of this complication can be reduced to minimum
by using soft tissue line with length and size adapted at the newborn.
If there is no free back flow, the cannula tip may be in closed
contact with the vessel wall. In this situation, the cannula should
be repositioned till blood can be easily aspirated. If this cannot be
achieved the cannula should be removed because movement of the
cannula tip against the vessel wall may result in devascularisation,
erosion, and perforation. The cannula should be firmly secured to the
skin to prevent movement of its tip against the vessel wall [2].
Management of pleural effusion involves stopping of all infusions
through the CVC followed by aspiration from the catheter, drainage
of the pleural cavity, maintaining the patient’s hemodynamics, and
adequate oxygenation. Removal of the improperly placed catheter is
firmly indicated [3,7].
Conclusion
In recent years, catheterization of the superior vena cava via
the sub-clavian or the internal jugular vein became a routinely
procedure in ICU to facilitate management of these critical patients.
Pleural effusion related to central line malposition is a rare but
serious complication. Its incidence can be reduced to minimum by
performing ultra-sound guided canulation and the use of the smallest
and soft lines. The need for such lines should be constantly reviewed
and as soon as they accomplish their role they should be removed [2].
This case report aims to sensitize the physicians to this
complication and emphasize the importance of ensuring a good
position of the catheter by aspiration of venous blood, immediate
post insertion X-ray with contrast injection confirming the correct
position and the use of ultra-sonographic guidance whenever
available especially in difficult cases.
References
- Lee EK. An Unexpected Left Hydrothorax after Left Internal Jugular Venous Catheterization for Total Parental Nutrition and Antibiotics. Ann Acad Med Singapore. 2006; 35: 742-745.
- Henderson AM, Sumner E. Late perforation by central venous cannulation. Arch Dis Child. 1984; 59: 776-789.
- Omar HR, Fathy A, Elghonemy M, Rashad R, Helal E, Mangar D. Massive hydrothorax following subclavian vein catheterization. Int Arch Med. 2010; 3: 32.
- Beardsall K, White DK, Pinto EM, Kelsall AW. Pericardial effusion and cardiac tamponade as complications of neonatal long lines: are they really a problem? Arch Dis Child Fetal Neonatal. 2003; 88: 292–295.
- Paw HGW. Bilateral pleural effusions: unexpected complication after left internal jugular venous catheterization for total parenteral nutrition. Br J Anaesth. 2002; 89: 647-650.
- Flannigan C, Bourke T, Keown K, Terris M. Bilateral total parenteral nutrition pleural effusions in a 5-week-old male infant. BMJ Case Reports. 2012.
- Burrah R, Sonig A, Patel R, Devi U. An unusual complication of internal jugular vein catheterization. Indian J Crit Care Med. 2013; 17: 265-266.
- Colón R, Frazier OH. Right Hydrothorax after Left Subclavian and Internal Jugular Vein Catheterization: A Delayed Complication. Tex Heart Inst J. 1985; 12: 389-392.