Research Article
Results of Bone and Soft Tissue Surgery Combined with Arthrodesis of the Talocalcaneal and Calcaneocuboid Joints for Equinovarus Associated with Spina Bifida
Takashi Fukushima*, Cherrelle Jones and Alan Kidon
Department of Foot and Ankle-Orthopedic Surgery, Precision Orthopaedic Specialties, USA
*Corresponding author: Mark J. Mendeszoon, Department of Foot and Ankle Orthopedic Surgery, Precision Orthopaedic Specialties, Inc., 150 Seventh Avenue, Suite 200 Chardon, OH 44024, USA
Published: 07 Feb, 2017
Cite this article as: Mendeszoon MJ, Jones C, Kidon A.
An Early Retrospective Review of the
Arthrosurface Metatarsophalangeal
Joint Implant. Clin Surg. 2017; 2: 1291.
Abstract
Hallux rigidus is a condition, which is defined as degenerative arthritis of the first metatarsophalangeal
joint. Hallux rigidus occurs due to repetitive micro trauma or wear and tear on the first MPJ. The
surgical treatments for the condition are thought of in two ways: joint salvage or joint destruction. The
total implant discussed throughout this paper is a joint salvage technique. Joint salvage procedures
aim to preserve the motion of the first MPJ. This study was conducted using the Arthrosurface Toe
Motion Total Toe System™. The study consisted of using 17 implants in a total of 14 patients. The
Arthrosurface Toe Motion Total Toe System™ is comprised of a poly-metal interface as opposed to
some the earlier designs utilized for first metatarsal phalangeal joint implantation. In considering
treatment implications, it is to be noted that the patients in this study were either a Coughlin stage
3 or 4.
During follow up the patients were assessed clinically and radiographically. All patients were available
for follow up and their outcomes, which were assessed using the AOFAS scores. Throughout the
years there have been numerous total implant designs. The benefits of using the Arthrosurface Toe
Motion Total Toe System™ are that it preserves the length of the first MPJ as opposed to other
techniques, which require resection of bone prior to implantation.
Introduction
Physical exam
When the patient presents with pathology of the 1st MPJ, one of the most common complaints is
pain. During the examination, the physician typically finds that the pain is at the end range of motion
with plantar flexion and dorsiflexion. Occasionally there can be an associated dorsal prominence
over the first MPJ, which usually indicates there is bone spurs associated with the pathomechanics
of the first metatarsal phalangeal joint. Crepitus is another finding of 1st MPJ pathology. Crepitus is
defined as grinding sound or sensation produced by friction between bone and cartilage. In the later
stages of hallux rigidus, there is a complete lack of motion [1].
Radiographic studies
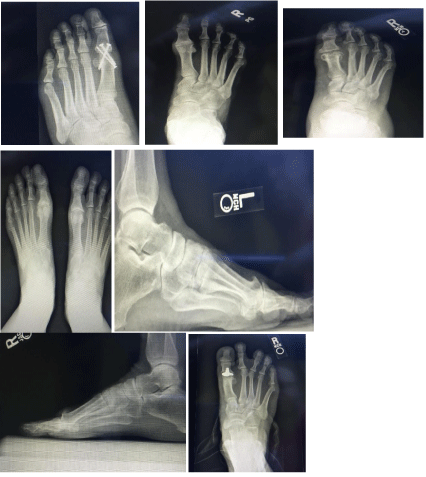
Before any treatments are offered a series of radiographs should be taken to assess the pathology
of the first MPJ. This usually consists of the lateral, anteroposterior, and the medial oblique views of
the affected foot. The AP view allows the practitioner to assess the joint space, while the lateral and
MO views will show any associated spurring around the joint as well as the joint space. Occasionally
loose bodies or sub chondral cysts are seen in any view taken. Sclerosis of the bone may also be
seen on the radiographic studies since this is one of the ways that the bone tries to heal itself. This
is a radiograph of a patient that presented to the clinic with a previous attempt at a 1st MPJ fusion
that has failed. The patient elected to undergo a revisional procedure with the Arthrosurface total
implant
In this radiograph you can see the flattened appearance of the metatarsal head as well as
significant joint space narrowing. This is the radiograph of a patient whose initial surgery consisted
of a hemi implant (Figure 1). The patient was not doing well with this type of implant and decided
to undergo a second procedure and have it converted using the Arthrosurface total implant. In this
radiograph, there are substantial cystic changes occurring in the first metatarsal head. There is also
a significant loss of the joint space [2]. This patient presented as a surgical consult for b/l hallux
rigidus pain and elected to have both 1st MPJ’s reconstructed with the Arthrosurface total implant.
Treatments
For the early stages of hallux limitus/ rigidus, it may be appropriate to treat the patient
conservatively. This usually entails non-surgical treatments. Shoe
modification is one of these modalities. Extra depth shoes can be
utilized to accommodate spurring of the 1st MPJ. Shoes with a rocker
sole in the ball of the foot can also be used so that there is less need for
the joint to flex, which prevents painful motion of the 1st MPJ. Another
non-surgical treatment option is the use of NSAIDs to decrease the
amount of inflammation in the area. Functional orthotics is another
treatment modality that may be utilized in mild 1st MPJ arthritis
[3]. One of the most common orthotic devices used is a Morton’s
extension. The way this device works is that if prevents motion in
the first MPJ by decreasing the ROM needed for function. Since the
device is rigid, there is less movement in the joint, which results in
less pain for the patient since the arthritic surfaces are not gliding
against each other as much as it would without the device in place.
Joint preservative procedure
Cheilectomy: Cheilectomy is the removal of the osteophytic
proliferation about the metatarsal head or the proximal phalangeal
base. In some cases, the dorsal ¼ to 1/3 of the metatarsal head is
transected to increase the motion of the first metatarsal phalangeal
joint.
Hemi and total implants: Implant arthroplasty has played a
major role in the advancement of surgery for painful arthritic joints.
Implants for the first metatarsophalangeal joint have provided
thousands of patients with the opportunity to ambulate with a painfree
functional first ray. Some authors have applauded the versatility
and effectiveness of implants for hallux rigidus. The two types are the
total and the hemi implant. The total implant has segments for both
the first metatarsal and the proximal phalanx, while the hemi may
only have a segment for the proximal phalanx. The Arthrosurface
implant consists of a metatarsal component and a phalangeal
component designed for resurfacing the 1st metatarsal head and
the base of the proximal phalanx. These two implants replace the
metatarsophalangeal joint by complete functional preservation of the
joint and maintaining of the sesamoid complex.
Joint destructive procedures
Keller Arthroplasty: The Keller arthroplasty is a procedure
indicated for a reduction of joint pain and has been a mainstay of
hallux limitus and rigidus surgery for many years. The procedure
is still useful and effective in selected patients, particularly as an
alternative to an implant. The Keller arthroplasty may be considered
as a salvage procedure for iatrogenic complications or arthritic joints.
In the Keller arthroplasty, the proximal 1/3 of the proximal phalanx
is resected while the first metatarsal head is left intact, although any
osteophytes may be removed.
First MPJ Arthrodesis: For many, first MPJ arthrodesis is thought
of as the gold standard for treatment of hallux limitus/ rigidus.
Arthrodesis of the first metatarsophalangeal has been considered
for significant degenerative changes at the first metatarsophalangeal
joint and evidence of instability at the first metatarsophalangeal joint.
This is done by resecting portions of the 1st metatarsal head and the
proximal phalanx then bringing those surfaces together and fixating
them with screws or a combination of screws with a plate.
Surgical procedure
The patient is placed supine on the operating table, with the
operative extremity in a well-padded position. The procedure can
be done with either general anesthesia or monitored anesthesia care.
Depending on the patient, a regional block may also be utilized in
the form of a popliteal or ankle block. Generally, an ankle tourniquet
is also utilized along with the use of an Esmarch bandage wrapped
around the foot carried to the ankle, prior to tourniquet inflation. A
dorsal incision is then made with a #15 blade over the first metatarsal
phalangeal joint, slightly medial to the extensor hallucis longus
tendon. To expose the joint capsule a combination of sharp and
blunt dissection is used through the subcutaneous tissues. Care is
taken to protect the neurovascular structures and electrocautery is
used as needed. The extensor hallucis longus tendon is freed from the
capsule and retracted laterally to keep the tendon within its sheath. A
longitudinal arthrotomy is made along the medial border of the joint,
and the capsule is elevated off the bone. A complete release of the
collateral ligaments, sesamoidal suspension ligaments, and capsule
should be made so that the entire joint, including the sesamoids, is
easily visualized. It is very important to visualize the articular edge of
the sesamoid crista on the metatarsal head because this is the landmark
for placement and sizing of the implant. In advanced hallux rigidus,
the sesamoids and flexor hallucis brevis will have fibrotic adhesions
to the metatarsal head that will limit dorsiflexion postoperatively.
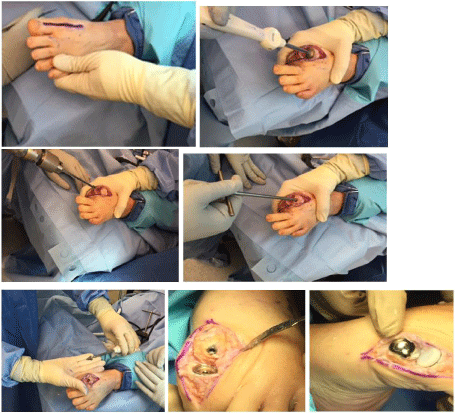
A curved osteotome, freer or McGlammary elevator can be used to
release these plantar adhesions (Figure 2). Care should be taken to
avoid damage to the metatarsal-sesamoid articulation. A cheilectomy
is not performed at this time to avoid over resection of bone.
Surgical technique: First metatarsal preparation
1. Use the Drill Guide to locate the axis normal to the articular surface and central to the defect. The plantar foot of the Drill Guide should be seated at or just below the crista. Place the Guide Pin into a cannulated pin driver and secure at the etch marking on the Guide Pin. Advance the Guide Pin into the bone. Confirm correct Guide Pin placement radiographically before proceeding. Place the Step Drill over the Guide Pin and drill until the proximal shoulder of the Step Drill is flush to the articular surface. Should the Guide Pin loosen, use the Step Drill to re-center the Guide Pin in the pilot hole and advance into the bone.
2. Tap the hole to the etched depth mark on the Tap. Based on the resistance felt during tapping, a decision can be reached as to whether or not bone cement will be needed.
3. Place the Driver into the Taper Post and advance the Taper Post until the line on the Driver is flush with the cartilage surface making sure that it is central to the defect.
4. Clean the taper in the Taper Post with the Taper Cleaner. Place the Trial Cap into the Taper Post to confirm correct depth of the Taper Post. The height of the Trial Cap must be flush or slightly below the existing articular cartilage surface to avoid the HemiCAP DF Articular Component from being placed proud or above the surface of the defect. Adjust depth if needed using the Driver to rotate the Taper Post. Remove the Trial Cap.
5. Place the Centering Shaft into the taper of the Taper Post. Place the Contact Probe over the Centering Shaft and rotate around the Centering Shaft. Use light pressure on the Contact Probe to ensure proper contact with the articular surface. Read the Contact Probe to obtain offsets at four indexing points and mark each of the identified offsets on the appropriate Sizing Card. The plantar offsets are best determined by placing the Contact Probe on either side of the crista within the sesamoid grooves. Select the appropriate DF Articular Component using the Sizing Card.
6. Choose the appropriate Surface Reamer based on the offsets. Confirm selection by matching the color code on the DF Articular Component package with the colored band on the Surface Reamer shaft. Drive the Surface Reamer over the Guide Pin until it contacts the top surface on the Taper Post.
7. Place the appropriately sized Dorsal Reamer Guide into the taper of the Taper Post. The Guide should be oriented such that the Dorsal Reamer is at the 12 o’clock position. Advance the Dorsal Reamer to the depth stop. Once the Dorsal Reamer has advanced to the handle, immediately stop the cannulated powered drill and remove the Dorsal Reamer Guide.
8. Place the Sizing Trial into the defect that matches the offset profile of the chosen DF Articular Component. Confirm the fit of the Sizing Trial so that it is congruent with the edge of the surrounding articular surface or slightly recessed. It is critical to ensure that the toe can be articulated to 90 degrees dorsiflexion. Removal of all osteophytes and non-essential bone on the metatarsal head with adequate soft tissue and sesamoid releases will increase ROM.
9. If using the DF Articular Component as hemi- arthroplasty, all osteophytes should be removed from the dorsal phalanx to maximize ROM. The Phalangeal Reamer can be utilized or a standard cheilectomy cut can be performed. If using the DF Articular Component and Phalangeal Component as a total joint replacement, defer osteophyte removal until Phalangeal Component is positioned.
10. Before placing the DF Articular Component on the Implant Holder, make sure that sufficient suction is present to hold the device on the distal suction cup. Align the DF Articular Component on the Implant Holder. Orient the etch marks on the back of the DF Articular Component with the etch mark on the handle of the Implant Holder. Align the DF Articular Component with the appropriate offsets. nsert into taper of the Taper Post.
11. Use a slight tap on the Impact or to seat the DF Articular Component. Progressively tap the Impact or until the Articular Component is firmly seated on the bone and into the Taper Post.
Surgical technique: Proximal phalanx preparation
1. Using the Pin Drill Guide, place the 1.5 mm Guide Pin cen>tral to the phalangeal surface, in line with the axis of the bone. Confirm 1.5 mm Guide Pin placement radiographically before proceeding.
2. Introduce the Reamer over the 1.5 mm Guide Pin and advance under power until the Reamer depth indicator is flush to the medial, lateral, and plantar phalangeal articular surfaces. Do not use the dorsal surface as a reference as the Reamer may cut beyond its margin making proper depth determination difficult.
3. Introduce the Tap over the 1.5 mm Guide Pin and advance by hand until the Tap depth indicator is flush to the level of the original (before reaming) phalangeal articular surface.
4. Place the 2 loops of the Suture from the Delivery Tool around the proximal end of the Fixation Post. Apply tension to the proximal end of the suture to mount the Fixation Post onto the Delivery Tool. Introduce over the 1.5 mm Guide Pin, and advance using the Hex Driver until the distal surface of the Fixation Post is fully seated in the prepared bone socket. Remove the Hex Driver and 1.5 mm Guide Pin. Draw the Delivery Tool away from the joint, allowing access to the seated Fixation Post. Use care to not damage or tangle the suture strands.
5. Use the Insert Trials to determine the most appropriate Phalangeal Insert for seating into the Fixation Component. The medial lateral offset dimensions of the Trial and Phalangeal Insert should match the medial lateral offset dimensions of the DF Articular Component. Perform range of motion evaluation before proceeding.
6. Pass the proximal knotted end of the Suture from the Delivery Tool through the slot in the Hex Driver shaft. Rotate the Hex Driver to tension the sutures and apply force through the Delivery Tool to seat the Phalangeal Insert. Perform final range of motion evaluation.
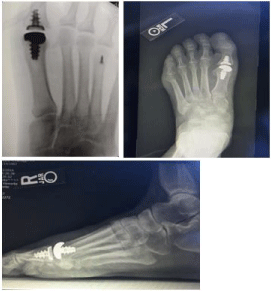
Figure 1
h2 id="anch5" class="text-left article-page-title">Figure 2Figure 3
Table 1
Table 2
Table 3
Results
There were 14 patients involved, (eight females and six males), 3 patients had bilateral implants placed, while 11 had a single implant placed, for a total of 17 implants. The average age of the patient was 60.8 years with the range being from 54-69, and the median age being 56 years old. Radiographs were taken pre and post operatively to assess each patient’s affected joint. Following surgical intervention, the patient’s progress was reassessed in the clinic at each postoperative appointment. The postoperative appointments were scheduled for 1 week, 2 weeks, 6 weeks, 3 months, and 6 months. The patient’s were then categorized into two groups: primary procedures and secondary procedures. A person undergoing a primary procedure meant that this was their first surgical intervention for addressing their hallux limitus/ rigidus. A person in the secondary group meant that they had previous surgical intervention. A scoring system similar to that of the AOFAS scoring system for rear foot was used, but tailored to the first metatarsal phalangeal joint (Figure 3). The three main categories of the scoring system were pain, function, and alignment. The higher the patient’s score total, the better the outcome of the procedure [4].
Discussion
Numerous characteristics were taken into consideration while carrying out this study. The first category that we broke the patient’s into was whether this was a primary or secondary procedure. A primary procedure means that this was the first surgical intervention to treat hallux rigidus, while secondary means that they had had prior intervention [5]. For those that fell into the secondary category the previous interventions consisted of a silicone implant, hemi implant, and non-union of 1st MPJ fusion. When patient chooses to undergo surgery, there is inherent risk associated with doing so, in which every precaution is used to ensure that complications do not arise. The most common complications associated with correction of hallux limitus/ rigidus are infection, non-union, mal union, improper function or complete loss of function [6]. It is necessary to point out that the scale used to assess patient’s outcomes in the postoperative period were more subjective than objective [7,8]. While radiographs were analyzed to prove that joint space was preserved and clinical evaluations were done to prove that joint range of motion was increased, overall success of the surgery was based on how patient’s felt in regards to how they felt prior to surgical intervention.
Conclusion
All patients were available for follow up and most were satisfied with their outcomes, with only one patient seeking to have the implant removed. The Arthrosurface Toe Motion Total Toe System™ preserves the length of the first MPJ, re-approximates anatomy, and conserves bone and soft tissue by using the Metatarsal based HemiCAP DF and an inlay, screw-based Phalangeal component. This creates an environment for the first MPJ to be mobile while other types of implants are fixed at one component. As this is a relatively new product, we look forward to seeing the long term follow up results. However, after analyzing the results thus far, they appear promising, and we will continue to use this product. The future goal of this study is to eventually have a large enough population size to illustrate more statistically significant results.
References
- Sung W, Weil L Jr, Weil LS Sr, Stark T. Total First Metatarsophalangeal Joint Implant Arthroplasty: A 30-year Retrospective. Clin Podiatr Med Surg. 2011; 28: 755-761.
- Baumhauer JF, Nawoczenski DA, DiGiovanni BF, Wilding GE. Reliability nd validity of the American Orthopedic Foot and Ankle Society Clinical Rating Scale: a pilot study for the hallux and lesser toes. Foot Ankle Int. 2006; 27: 1014-1019.
- Ibrahim T, Beiri A, Azzabi M, Best AJ, Taylor GJ, Menon DK. Reliability and validity of the subjective component of the American Orthopedic Foot and Ankle Society clinical rating scales. J Foot Ankle Surg. 2007; 46: 65-74.
- Cook E, Cook J, Rosenblum B, Landsman A, Giurini J, Basile P. Metaanalysis of first metatarsophalangeal joint implant arthroplasty. J Foot Ankle Surg. 2009; 48: 180-190.
- Kissel CG, Husain ZS, Wooley PH, Kruger M, Schumaker MA, Sullivan M, et al. A Prospective Investigation of the BioproHemi-Arthroplasty for the First Metatarsophalangeal Joint. J Foot Ankle Surg. 2008; 47: 505-509.
- Kim PJ, Hatch D, Didomenico LA, Lee MS, Kaczander B, Count G, et al. A multicenter retrospective review of outcomes for arthrodesis, hemi-metallic joint implant, and resectional arthroplasty in the surgical treatment of end-stage hallux rigidus. J Foot Ankle Surg. 2012; 51: 50-56.
- Warren S. Taranow, DO and Judson R. Moore, PA-C, JD. Hallux Rigidus: A Treatment Algorithm. Tech Foot & Ankle. 2012; 11: 65–73.
- Cook JJ, Cook EA, Rosenblum BI, Landsman AS, Roukis TS. Validation of the American College of Foot and Ankle Surgeons Scoring Scales. J Foot Ankle Surg. 2011; 50: 420-429.