Case Report
A Case Report of Orbital Abscess Complicating Ethmoidal Sinusitis in 15 Months Girl
Saif Al Dossari1 and Kamal-Eldin Ahmed Abou-Elhamd2*
1Department of Ophthalmology, King Faisal University, Saudi Arabia
2Department of Surgery, King Faisal University, Saudi Arabia
*Corresponding author: Kamal-Eldin Ahmed Abou-Elhamd, Department of Surgery, College of Medicine, King Faisal University, Al- Ahsa 31982, Box 400, Saudi Arabia
Published: 07 Feb, 2017
Cite this article as: Dossari SA, Ahmed Abou-Elhamd
K-E. A Case Report of Orbital Abscess
Complicating Ethmoidal Sinusitis in 15
Months Girl. Clin Surg. 2017; 2: 1289.
Abstract
Objectives: Our study aimed to present a case of right subperiosteal abscess in a 15 months girl secondary to ethmoidal sinusitis.
Study Design: A case report study.
Methods: A 15- month’s old girl presented to emergency room, Al-Ahsa, Saudi Arabia by her
parents in July 2016 with swelling of the upper and lower lids of the right eye for 3 days duration
and fever.
Results: After failure of medical treatment for orbital cellulitis, a diagnosis of right subperiosteal
abscess due to ethmoidal sinusitis was made followed by surgical drainage and rapid improvement.
Conclusion: Orbital examination complicated by soft tissue oedemain children is not easy even
to efficient clinician to reach a proper diagnosis. Thus, the use of imaging is important to reach a
proper diagnosis.
Keywords: Orbital cellulitis; Subperiosteal abscess; Sinusitis
Case Presentation
A 15-month’s old girl presented to emergency room, Al-Ahsa, Saudi Arabia by her parents in
July 2016 with swelling of the upper and lower lids of the right eye for 3 days duration and fever not
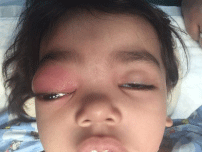
responding to antipyretics (Figure 1). Child is healthy and not known to have any systemic disease
and she received all her immunization as scheduled. There was no history of trauma or surgery.
On examination, the child was febrile and looked ill and not active. Both upper and lower lids on
right eye showed significant signs of inflammation (redness, swelling and hotness) and there was
tenderness mainly on the medial sides of right upper lid. The vision and intraocular pressure could
not be assessed. Extra ocular muscles movement showed decrease right eye elevation, otherwise
full movement in both sides was elicited. Pupil showed sluggish reaction on right eye. The right
eye showed inferior dystopia and mild proptosis. The right eye showed conjunctival injection more
prominent on the superior quadrant of the conjunctiva. Anterior segment and dilated fundus
examination was normal. Left eye exam was within normal limits.
Investigation
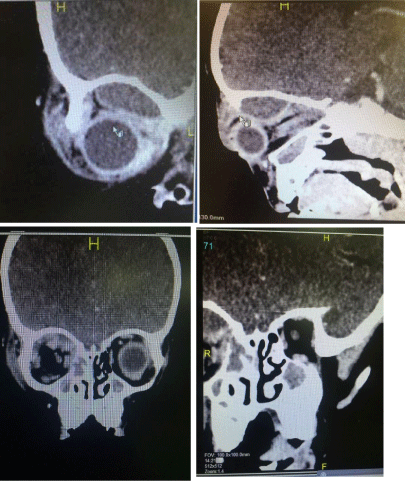
CBC shows leukocytosis and low hemoglobin (Figure 2). CT scan on the orbit and paranasal
sinuses was done and showed in (Figures 3) about 1.9 x 2.6 x 1 cm
localised fluid collection with ring enhancement after administration
of I.V contrast material seen in the superior medial aspect of the right
orbital cavity and pushing the eye globe antero-inferiorly suggestive
of abscess formation and retro-orbital cellulitis with surrounding
marked soft tissue swelling overlying the right eye, mucosal thickening
of both maxillary sinus appears more prominent in the right side with
opacification of the right upper nasal cavity and ethmoidal air cell
suggestive of sinusitis. The left orbital cavity appears within normal.
Both optic nerves appear unremarkable. The extraocular muscles
appear within normal except for the right medial and superior rectus
muscles which appears displaced by the fluid collection described
above. These findings conclude retro-orbital localised collection in the
superior medial right orbital cavity most likely represent abscess with
radiological evidence of sinusitis. A diagnosis of right subperiosteal
abscess was made.
Management
She was admitted and IV antibiotics was given for five days in
the form of Vancomycin 125 mg QID, Ceftazidime 420 mg TID and
Metronidazole 125 mg TID, but there was no improvement. Then
on the fifth day, oculoplasty consultation was requested and patient
taken to OR for urgent drainage of the subperiosteal abscess. Lid
crease approach was done. Patient was kept on the same antibiotics
for one week more including metronidazole.
Post operative
Patient showed significant improvement of the signs of
inflammation including the proptosis. By the first day post operatively
she was a febrile and she was discharged after one week on oral
augmentin for 14 days.
Follow up
She was seen in the outpatient clinic active and a febrile and there
were no signs of inflammation or proptosis (Figure 4). CT follow
up orbit and paranasal sinuses was done and showed persistent
opacification of the right bulla ethmoidalis and adjacent ethmoidal
cells with otherwise well-pneumatized right anterior frontal
recess cells and right maxillary antrum. There was also satisfactory
mineralization of the right lamina papyracea with practically complete
resolution of the adjacent intra-orbital extraconal inflammatory
changes. There was noticeable regression in the size of previously
identified right orbital roof based subperiosteal abscess reduced to
a small-thickness ring of granulation tissue surrounded by a regular
rim of incorporated periosteal reaction.
Figure 1
Figure 2
Figure 3
Figure 4
Figure 4
Outpatient clinic active and a febrile and there were no signs of inflammation or proptosis.
Discussion
Orbital cellulitis is a common complication of ethmoidal sinusitis
in children [1,2]. It is an acute suppurative inflammation of orbital soft
tissue. It is characterized by acute onset with rapid progression and is
accompanied by fever. If it is treated ineffectively, complications may
develop including cavernous sinus thrombosis, meningitis, frontal
abscess, and osteomyelitis, loss of vision and death. Intracranial and
intraorbital complications occur in children more frequently than
in adults with an incidence of 3 % [15,16]. The potential devastating
complications with regards to vision and/or intracranial extension
are thankfully rare. Anatomically, the orbit is a quadrilateral pyramid
surrounding the eye and its soft tissues. The orbital septum which is
a layer of fascia forms a barrier between the deep orbital soft tissue
and the superficial structures. Inflammation anterior to the septum
causes preseptal cellulitis which accounts for 84- 87% of cases [3] and
posterior to the septum causes orbital cellulitis.
At birth only the ethmoidal sinuses are well developed. The
maxillary sinus develops within the first two years. The frontal
sinuses only start developing in the 6th year of life. The ostia of
the sinuses are relatively large compared to the size of the sinuses
during early development [3]. The rich venous plexus in the orbit
communicates with the facial veins anteriorly. The orbital veins are
without valves facilitating a two-way spread of infections. Preseptal
cellulitis (first group in Chandler’s classification) is characterized
by erythema and swelling of the eyelids. The visual acuity, ocular
movements are normal. In young children the intense oedema of
the lidsmay sometimes make examination of the eye difficult and the
distinction between orbital cellulitis (second group) and it is difficult.
Orbital cellulitis is characterized by lid oedema and erythema,
chemosis of the conjunctiva, restricted ocular motility and proptosis.
Impaired ocular motility and proptosis might be pathognomonic for
diagnosis of subperiosteal abscess which is the third group [17-19].
Patients are more likely to present with leukocytosis, fever, and/or
a history of upper respiratory symptoms and generalized malaise
[8]. Orbital abscess and cavernous sinus thrombosis are the fourth
and fifth groups of Chandler’s classification [4]. Preseptal cellulitis
as a complication to acute sinusitis involves 50-72% of orbital cases
while orbital cellulitis involves 19-50%, and 9–15 % associated with
subperiosteal abscesses [9-11]. Orbital examination complicated by
soft tissue oedemain children is not easy even to efficient clinician
to reach a proper diagnosis. The differentiation between preseptal
and deep orbital cellulitis is difficult based on clinical observation
and clinical presentation may not always reflect underlying disease
severity [7]. Thus, the use of imaging is important to reach a
proper diagnosis. Radiation exposure can lead to increased risks
of malignancy; leukaemia and primary brain tumours especially in
the pediatric population [5,6]. So, decision for ordering CT scan
should be under joint ENT & Ophthalmology consultation. Contrastenhanced
CT scanning is the imaging modality of choice as it can
identify soft tissue changes while also providing bony detail [8,12,13]
A complete blood count (CBC), CRP and sedimentation rate, should
be included in the initial investigations [13]. An elevated white blood
cell count may occur in either preseptal or orbital cellulitis, but is
more common in orbital cellulitis. The erythrocyte sedimentation
rate is often elevated in patients with orbital cellulitis [14]. Patients
with orbital complications due to an acute sinusitis have a higher
body temperature and white blood cell counts, and elevated values
for CRP in peripheral blood when compared to patients with orbital
inflammation and swelling due to other causes [17]. The main
organisms in orbital infection in affected children are Streptococcus
(two-thirds of cases) and Haemophilus (almost half of cases) and
antibiotic choices should reflect this [3]. The treatment of preseptal
and orbital cellulitis requires a coordination of a paediatrician, an
ophthalmologist and otorhinolaryngologist, with further advice
from the neurosurgical and neurology teams if necessary. Frequent
evaluation of the child is necessary to check the response to treatment.
Examiner should consider conditions that may simulate orbital
infections. They are neuroblastoma, rhabdomyo sarcoma, fungal
infections, orbital myositis, lymphangioma, Graves’s disease, dermoid
cyst rupture or inflammation, trauma, or systemic conditions such as
sickle cell disease [14]. Preseptal cellulitis may be treated with oral
antibiotics and nonsteroidal anti-inflammatory drugs with regular
daily clinic review. Orbital cellulitis needs hospital admission and
treatment with a combination of intravenous antibiotics covering
for both aerobic and anaerobic organisms for 2 weeks followed by
oral antibiotics for 1 week. The presence of an abscess needs surgical
intervention. Indications for an operative intervention include a
visible abscess formation in CT or MRI scan, vision loss, impaired
ocular motility, or a clinical progression after 24 h of therapy [17].
A third generation cephalosporin (ceftriaxone or cefotaxime)covers
both gram positive and gram negative organisms, however the
additional use of flucloxacillin to cover Staphylococcus aureus is
fruitful. Metronidazole is also used to cover for anaerobic bacteria.
The use of clindamycin is recommended in the presence of infections
that involve the bone with osteomyelitis or those individuals who are
allergic to cephalosporins and penicillins.
References
- Sobol SE, Marchand J, Tewfik TL, Manoukian JJ, Schloss MD. Orbital complications of sinusitis inchildren, J. Otolaryngol. 2002; 31: 131-136.
- Rahbar R, Robson CD, Petersen RA, DiCanzio J, Rosbe KW, McGill TJ, et al. Management of orbital subperiosteal abscess in children, Arch. Otolaryngol Head Neck Surg. 2001; 127: 281-286.
- P Watts. Preseptal and orbital cellulitis in children in Symposium: eyes and ENT chapter Paediatrics and child health. 2015; 26: 1.
- Chandler JR, Langenbrunner DJ, Stevens ER. The pathogenesis of orbital complications in acute sinusitis, Laryngoscope. 1970; 80: 1414-1428.
- Pearce MS, Salotti JA, Little MP, McHugh K, Lee C, Kim KP, et al. Radiation exposurefrom CT scans in childhood and subsequent risk of leukaemia and brain tumours: a retrospective cohort study. Lancet. 2012; 380: 499-505.
- Miglioretti DL, Johnson E, Williams A, Greenlee RT, Weinmann S, Solberg LI, et al. Paediatric computed tomography and associated radiation exposure andestimated cancer risk, JAMA Pediatr. 2013; 167: 700-707.
- Crosbie RA, Nairn J, Kubba H. Management of paediatric periorbital cellulitis: Our experience of 243children managed according to a standardized protocol 2012-2015. Int J Pediatr Otorhinolaryngol. 2016; 87: 134-138.
- Bedwell J, Bauman NM. Management of pediatric orbital cellulitis and abscess. Curr Opin Otolaryngol Head Neck Surg. 2011; 19: 467-473.
- Sobol SE, Marchand J, Tewfik TL, Manoukian JJ, Schloss MD. Orbital complications of sinusitis inchildren, J. Otolaryngol. 2002; 31: 131-136.
- Al-Madani MV, Khatatbeh AE, Rawashdeh RZ, Al-Khtoum NF, Shawagfeh NR. The prevalence of orbital complications among children and adults with acute rhinosinusitis. Braz J Otorhinolaryngol. 2013; 79: 716-719.
- Ryan JT, Preciado DA, Bauman N, Pena M, Bose S, Zalzal GH, et al. Management of pediatric orbital cellulitis in patients with radiographic findings of subperiosteal abscess. Otolaryngol Head Neck Surg. 2009; 140: 907-911.
- Soon VT. Pediatric subperiosteal orbital abscess secondary to acutesinusitis: a 5-year review. Am J Otolaryngol. 2011; 32: 62-68.
- DMeara DJ. Sinonasal disease and orbital cellulitis in children. Oral Maxillofac Surg Clin North Am. 2012; 24: 487-496.
- Jain A, Rubin PA. Orbital cellulitis in children. Int Ophthalmol Clin. 2001; 41: 71-86.
- Hicks CW, Weber JG, Reid JR, Moodley M. Identifying and managing intracranial complications of sinusitis in children:a retrospective series. Pediatr Infect Dis J. 2011; 30: 222-226.
- Giusan AO, Kubanova AA, Uzdenova RKh. Rhinosinusogenic complications: the prevalence and principles of treatment.Vestn Otorinolaringol. 2010; 4: 64-67.
- Welkoborsky H-J, Graß S, Deichmuller G, Bertram O, Hinni ML. Orbital complications in children: differential diagnosis of a challenging disease. Eur Arch Otorhinolaryngol. 2015; 272: 1157-1163.
- Khalifa BC. Extent of resection of the lamina papyracea in medial subperiosteal abscess. Otolaryngol Head Neck Surg. 2011; 145: 161-164.
- Ketenci I, Unlu¨ Y, Vural A, Dogan H, Sahin MI, Tuncer E. Approaches to subperiostal orbital abscesses. Eur Arch Otorhinolaryngol. 2012; 270: 1317-1327.