Research Article
Evolution of Hair Transplantation
Kayiran O*
Department Plastic and Reconstructive Surgery Clinic, Ankara Research and Training Hospital, Turkey
*Corresponding author: Oguz Kayiran, Department Plastic and Reconstructive Surgery Clinic, Ankara Research and Training Hospital, Ankara, Turkey
Published: 06 Feb, 2017
Cite this article as: Kayiran O. Evolution of Hair
Transplantation. Clin Surg. 2017; 2:
1287.
Abstract
Background: Numerous non-surgical methods and surgical options are available for the solution
of baldness in the practice. Technology gives mighty weapons in this field. Thus, individualized
solutions are best carried out with well-trained and qualified practitioners. Here, a modification
of follicular unit extraction, direct hair implantation is introduced with previously licensed unique
pens.
Materials and Methods: Follicular unit extraction and direct hair implantation methods were
carried out in 207 hair transplantations between January and December of 2014. The nests for the
grafts were created via pieces of hand-cut razor blade in follicular unit extraction. In addition, a
new modification of follicular unit extraction, direct hair implantation, is done via pens that are
produced for this purpose.
Results: Thirty eight direct hair implantations were performed in addition with 169 follicular
unit extractions. An average number of 2973 grafts were transplanted. Mean operation time was
calculated as 385 minutes.
Conclusion: Hair transplantation is still the best solution for hair loss. In conjunction with the
surgery, the addition of non-surgical interventions may give a better result to the patient. On the
other hand, the promising results in the field of regenerative medicine with cell-based solutions may
alter hair transplantation and change the options solely into this field.
Keywords: Hair transplantation; Direct implantation; Razor; Nest
Introduction
Hair transplantation has gone a big revolution with the pioneers in this field [1-7]. However, it
is still controversial for the practitioners which transplantation method is the best so far. To achieve
a good cosmetic result in hair transplantation, a natural-looking hairline with adequate density shall
be established. There are numerous modifications of defined techniques with each one explaining
and suggesting verified solutions. Hair follicle harvesting techniques are either hand-held or robotic
methods. The practitioner-dependent methods are comprised of direct excision of the donor area
and extraction of the follicles by punches; whereas SAFE (Surgically Advanced Follicular Extraction)
and ARTAS are the robotic systems [8-12]. After harvesting of the follicles, the transplantation can
be carried out by punches, needles or scalpels [13-16]. Overall success is attributable to meticulous
handling of the follicles as well as gentle transplantation. Regarding the graft survival (hair, cartilage,
etc), the main concern is the “take” [17]. Appropriate preparation of the recipient bed is crucial to
enhance the take.
This note describes the available options in hair loss surgery, the concepts of non-surgical
approaches and an experience share with a few patients grafted via direct hair implantation (DHI)
method. In addition, we describe a new method by using sliced razor blades to create comfortable
nests for the follicles that are to be transplanted. Thus, the evolution of hair transplantation is
summarized as well.
Material and Methods
This retrospective study consisted of 207 patients who had hair transplantation between
January and December 2014. The patients with scar tissue on the scalp and side-burn, beard and/or
moustache transplantation, multisession transplantations and female patients were excluded. The
harvested grafts out of the scalp were also not evaluated. Moreover, the patients with type III, IV
and V in Norwood classification were included in the study. On the other hand, the patients getting
medications, injections or having administrations to enhance hair density were excluded.
All the procedures were carried out under local anesthesia. The
hair was cut 1-2 mm in length. Micromotor system was used in the
harvesting of the hair follicles [13]. This system consists of punches
attached to the hand-piece of the micromotor system (1500-3000
rpm). Punches were chosen according to the diameter of the follicles
ranging between 0.8 and 1.2 mm. Harvesting of the follicles was
handled in supine position. With the aid of the sharp punch attached
to the motorized system, the follicle is detached from the surrounding
tissue (approximately 3-4 mm in depth=deep dermis layer). Later on,
it is released manually with fine-curved microforceps produced for
this purpose. Temporo-occipital region was used as donor site.
The harvested grafts were aligned in Petri dishes with cooled
saline (4°C). A dressing is made with sterile saline coated gauze to the
donor area and the patient was turned to the supine position.
In follicular unit extraction (FUE) technique, razor blades that
was cut into pieces was used to open the nests in vertically-oriented
fashion that are to be grafted (Figure 1). With this, we aimed to
diminish the incarceration of the implanted follicles. However, in
DHI technique, the grafts were loaded to the DHI pens with one
charged staff for this purpose (Video 1). The implantation of the
follicles was carried out in accordance with the natural hair angles by
the author under loupe magnification (Video 2 and 3).
After the entire implantation was established, the patient was
dressed with antibiotic coated, moisturized gauze to both donor
and recipient areas that were removed three days later at which
the first hair washing would also be carried out. The patients were
recommended to have their first hair-cut 15 days later.
At the end of the first postoperative year, patients were asked to
evaluate their satisfactions as bad, good and excellent.
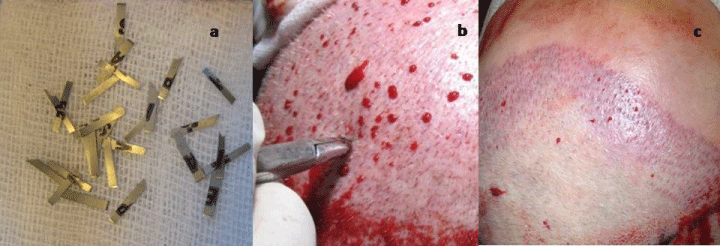
Figure 1
Figure 1
a) The razor blade is cut into pieces with 1-2 mm sharp edges b) Perforation is carried out with these pieces held by clamps c) These nests are in a
vertically-oriented fashion that are ready now for grafting.
Video 1
Video 2
Video 3
Results
A total number of 615400 grafts were transplanted in 207 patients.
Of these, 38 were DHI (19%) and 169 had FUE (81%).
Patients were classified as Norwood III, IV and V in 1 (0.5%), 30
(14.5%) and 176 (85%) patients, respectively. The main reason of hair
loss was androgenetic alopecia in our patients.
An average number of 2973 grafts were transplanted. Mean graft
numbers transplanted in FUE and DHI methods were 2982 and 2934,
respectively. The mean density was observed around 75 units/cm2 for
DHI technique and 50 units/cm2 for FUE method.
Mean operation time was noted as 385 minutes in which mean
FUE and DHI times were calculated as 373 and 437 minutes,
respectively. The patients were followed-up between 1 and 5 years.
Table 1 describes the distribution of the patients.
None of the patients had infection. Inclusion cyst formation was
observed in 4 patients who were treated successfully.
A few results with DHI technique are presented in (Figure 2 and
3).
The transaction rates were found as 2% which was attributable
to the literature percentages (2-8%) [13,18,19]. No graft loss was
documented in transplanted areas. Regarding satisfaction, excellent
scores were noted in 193 patients (93.2%) and 13 patients (6.3%)
gave good scores. One patient could not decide to give a score. We
regarded his score as bad (0.5%).
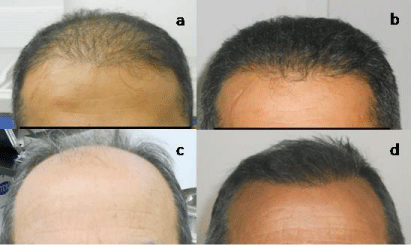
Figure 2
Figure 2
A 44-year-old male patient with Norwood type III patient. a) Preoperative appearance b) Postoperative 1-year appearance. A 51-year-old with Norwood
type IV patient. c) Preoperative appearance d) Postoperative 1-year appearance.
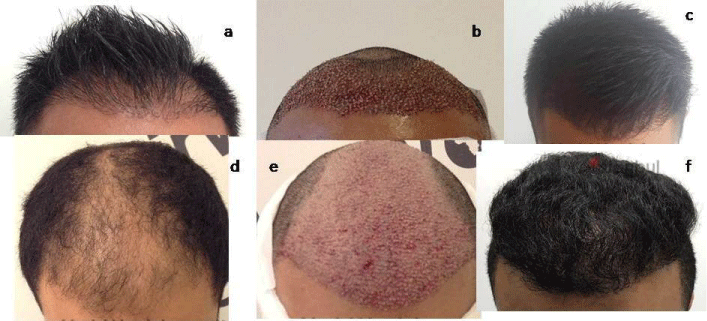
Figure 3
Figure 3
A 32-year-old male patient with Norwood type III patient. a) Preoperative appearance b) Immediate appearance of the patient after transplantation
c) Postoperative 1-year appearance. A 38-year-old with Norwood type V patient. d) Preoperative appearance. e) Immediate appearance of the patient after
transplantation f) Postoperative 1-year appearance.
Discussion
Male type baldness may cause a negative effect on individual’s
self-esteem. Hair transplantation gives a unique permanent solution
for those patients.
Non-surgical therapies for hair loss can be used mainly in early
phases. On the contrary, these options will be the first-line therapy
when the donor supply is limited or adjunctive after a surgical hair
modality is carried out [20]. Minoxidil, finasteride, dutasteride,
spironolactone or cyproterone acetate can be prescribed in selected
patients with temporary actions [20-25]. Moreover, low-level light
or laser therapy can be utilized in patients with early-phase hair loss
where the practitioner may choose home-use and/or in-office systems.
It is known that prostaglandin analogues such as prostaglandin F2a
and prostaglandin E2 promote hair growth in both mice and human
follicles [26]. In practice, latanoprost (a prostaglandin F2a analogue)
is a solution that provides a significant increase in hair growth [27].
Mesotherapy and platelet-rich plasma can be utilized in patients
needing additional therapies in the enhancement of hair growth.
Mesotherapy consists of superficial injections of pharmaceuticals and
vitamin compounds to the follicles. Platelet-rich plasma (PRP) is used
in almost every section of the medicine and includes several plateletderived
factors [28]. It is proven that PRP injections enhance hair
growth in transplanted follicles [29-31]. Nevertheless, more studies
are needed to evaluate PRP as a hair loss therapy.
Since the concept of “donor dominance” in male pattern hair loss
was first published in 1959, it is still not clear why the occipital hair is
spared [4]. The most accepted reason seems that occipital scalp is not
androgen dependent [23]. Whatever the reason is, it is the feature that
occipital hairs have permanent serves for hair transplantation in both
female and male pattern hair loss [4].
The permanent solution for hair loss can be achieved with
hair transplantation. The grafts harvested from the donor area are
transplanted to the recipient area in qualified, well-trained hands
and at optimum conditions. Nevertheless, graft viability depends
on several factors determined by the hair type, delicate technique,
physical trauma, vascular factors, biochemical injury, infection,
patient disruption and idiopathic reasons [32].
Hair transplantation is comprised of consecutive steps:
planning, preparation and anesthesia, graft harvesting, secure of
the harvested grafts, graft transplantation, and dressing. Each step
may be individualized in practice. Planning of the patient consists
of some blood tests, a thorough history of medical situation and
marking. After shortening of the hair if needed and preparation with
antiseptic solutions, anesthesia is carried out. Mostly, local anesthesia
is preferred; however, regional anesthesia or local anesthesia with
sedation can be chosen. When an entire anesthesia is established, a
tumescent solution is injected both to the donor and recipient area.
This enables an expansion to harvest the follicles in donor area and
graft them easily. The survival of the harvested graft is dependable on
temperature, hydration, infection and trauma [33]. The surgeon and
staff shall not transect or crush and dehydrate the follicles during the
procedure. This meticulous technique will ensure the best outcome.
It is also advised to maintain the follicles that are to be transferred
in a cold solution in order to reduce the ischemia and reperfusion
injury. Some holding solutions exist such as intravenous holding
solutions (eg: normal saline, lactated Ringer), cell culture media (eg:
Dulbecco’s Modified Eagle Medium, Williams E) and hypothermic
holding solutions (eg: HypoThermosol, BioLife Solutions, Bothell,
WA) [32]. Nevertheless, stored grafts are mostly kept cold in ice
blocks or cold solutions with the temperature rate between 4°C
and 10°C Harvesting of the follicles can be done via manually or
motorized systems. The practitioner can choose sharp or dull tipped
punches with a wide variety of diameter and bevel type. Eventually,
the follicles are transplanted delicately into the recipient area with
appropriate angle to establish similar grow pattern with the normal
hair. Nests for the grafts that are to be implanted can be created via
a sharp-punch and needles or scalpels in selected sizes [13-16]. On
the front line, we prefer to make the transplantations in a zig-zag
fashion to achieve a natural-looking frontal hairline design [14]. The
number of hair units required for the recipient size can be calculated
by the formulas defined for both frontal and vertex regions [23,34-
38]. The normal hair density is around 100 units/cm2 [39]. In general,
the density achieved with hair transplantation is approximately 30-40
units/cm2. Higher density called as dense packing (up to 60 units/
cm2) can be achieved with high viability rates [16,23,40].
Follicular unit transplantation (FUT) is a widely accepted
technique in hair transplantation [41]. In this method, the donor area
is shaved and an elliptical excision is made for hair follicle harvesting.
The dimensions of the ellipse are calculated up to the recipient area
that is to be grafted. The donor area is closed meticulously to reduce
the scar formation. The collected hair-bearing skin is dissected
under magnification and the extra tissues of the hair root as well as
the epithelium around are removed as much as possible. The grafts
containing clusters of one, two and three follicles are put into Petri
dishes containing cooled saline. Later on, the grafts are inserted
appropriately to the recipient area.
In contrast to FUT, follicular unit extraction (FUE) is a technique
with the extraction of follicular units with one or two roots using
circular punches. Okuda was the first that used self-made sharp
circular punches in various diameters (1-4 mm) [42]. He proposed
to use 2-4 mm punches with regard to 1 mm because, according to
him, the transection rate was interestingly high in 1 mm harvests. In
the market, there are several FUE donor harvesting devices available;
of which some are hand-held punches, some are motorized and
some are single user-directed robotic system which is also known
as SAFE (Surgically Advanced Follicular Extraction) and ARTAS
robotic systems [8-12]. Success with FUE depends on being able to
predictably dissect excellent-quality grafts with minimum transaction
rates from the donor region [7,9,18,40].
Ominigraft (Mecicamat S.A., Malakoff, France) has been
introduced to optimize mini and micrograft transplantation [9].
This device consists of three major parts: Hairtome; a hand-held
pneumatic graft implanter; and a hollow-shafted micromotor hand
piece with a punch blade in 0.8-1.25 mm. The transaction rates and
the operation time are significantly lower with this device. Here, we
used a new method in the transplantation of the hair follicles via
sliced razor blade rather than needles or scalpel. On the other hand,
the conventional harvesting technique remained same.
There are some advantages and disadvantages of FUE over FUT
which was very well discussed previously [10]. FUE needs longer
learning curve and operation time, excellent hand-eye coordination,
patience, stamina and hair must be short enough for appropriate
harvesting. Moreover, the practitioner may be a candidate for potential
repetitive motion disorder in time [10]. Besides, the outcomes of FUE
may be better and the number of follicles transferred may be higher
when compared with FUT. In addition, FUE gives a scarless solution
for the patients insisting on not accepting an incision.
Another hair transplantation method, direct hair transplantation,
is presented to attenuate the transit time which may reduce the graft
survival [21]. Here, follicles are implanted as soon as they are harvested.
This technique was found a simple and feasible modification of FUE.
An automated FUE technique, Neograft®, enables a suctionbased
follicle harvesting with one or two-step extraction technique.
The follicles are collected in a suction canister in which they are
transplanted later by using a hand-piece with 0.8, 1 and 1.2 mm
punches that are produced specifically for this purpose. The motor
is silent and vibration free; however the steep learning curve and the
cost of the machine are the disadvantages [41].
Microrefined microfolliclular hair transplantation is a recently
described method in which anterior hairline is constructed with
FUE whereas the bald area is transplanted with FUT including strip
harvesting (with beveled incisions) and slivering of the strip under
magnification. The author proposes the graft transaction rate to
nearly 0% [14].
Direct hair implantation (DHI), a modified version of FUE,
has similarities with FUE in hair follicle harvesting, whereas the
implantation of the follicles is carried out with unique instruments
that is licensed by Konstantinos (US 8,801,743 B2) and produced
specifically for this purpose. The needle of the pen may vary in size;
since there are 0.40-2 mm oblique-cut needles in the market. After
follicle harvesting, each pen is loaded with a micrograft containing 1
to 3 hair follicles and subsequently implanted to the recipient area that
was not previously perforated. This technique allows the practitioner
graft the recipient area denser and gives less trauma and bloodless
field when compared with FUE. Moreover, this procedure lacks
additional punching for grafting as noted in other transplantation
techniques. On the contrary, the learning curve is high meaning that
this surgery needs more qualified personnel per patient. In addition,
the procedure is carried out with 3 or 4 personnel, because every
stage is assigned to a unique staff which means that the room is more
crowded than the other techniques. The pens and so these procedures
are relatively expensive when compared to FUT or FUE. Nevertheless,
follicle harvesting is significantly cheaper than robotic systems.
Complications after hair transplantation can be placed in the
following categories: a) Standard surgical risks b) Physician planning
errors; c) Physician technical errors; d) Patient compliance factors;
e) Patient physiology factors; and f) Miscellaneous causes [42]. In
addition, we may observe some site-specific complications after
all including donor and recipient site problems [42]. Donor site
complications include wide variety of unwanted scar formation,
donor-site depletion, wound dehiscence, necrosis, effluvium (shockloss),
hypoesthesia, neuralgia and neuroma and hematoma. Recipient
site complications may be comprised of hairline location or shape
error, progression error, graft type error, graft placement error,
hypopigmentation, hair color mismatch, chronic folliculitis, necrosis,
effluvium, ingrown hairs, cysts and low graft yield.
Animal studies reveal creation of human follicles from cultured
dermal and epidermal cells in a mouse model [43]. A revolutionary
breakthrough in this field is the discovery of induced pluripotent
stem cells enabling to reprogram differentiated fibroblasts into an
embryonic stem cell state [44,45]. A recent study exhibits the creation
of a bioengineered hair follicle germ using embryonic skin-derived
epithelium and mesenchymal donor cells where the transplanted
germ integrate to the host epithelium producing a complete
functional hair [46].
Forthcoming studies will ensure better results. As the technology
contributes to the medicine, it is possible that the whole process will
be carried out entirely with robotic and automated systems. Indeed,
the future may give the solutions by solely cell-based applications
enabling hair growth without a surgery. Up-to-date, we believe that
the combination of the surgical methods with the help of additional
options may give the best option for the patients to re-gain their
natural-looking hair with adequate density.
Table 1
References
- Barrera A. Advances in Aesthetic Hair Restoration. Aesthet Surg J. 2003; 23: 259-264.
- Uebel CO. Refining Hair Restoration Technique. Aesthet Surg J. 2002; 22: 181-183.
- Bernstein RM, Rassman WR. The Aesthetic of Follicular Transplantation. Dermatol Surg. 1997; 23: 785-799.
- Orentreich N. Autografts in Alopecia and Other Selected Dermatological Conditions. Ann N Y Acad Sci. 1959; 83: 463-479.
- Shiell RC. A Review of Modern Surgical Hair Restoration Techniques. J Cutan Aesthet Surg. 2008; 1: 12-16.
- Rose PT. The Latest Innovations in Hair Transplantation. Facial Plast Surg. 2011; 27: 366-377.
- Uebel CO. Micrografts and Minigrafts: A New Approach for Baldness Surgery. Ann Plast Surg. 1991; 27: 476-487.
- Onda M, Igawa HH, Inoue K, Tanino R. Novel Technique of Follicular Unit Extraction Hair Transplantation with a Powered Punching Device. Dermatol Surg. 2008; 34: 1683-1688.
- Avram MR, Watkins SA. Robotic Follicular Unit Extraction in Hair Transplantation. Dermatol Surg. 2014; 40: 1319-1327.
- Williams KL Jr. Current Practices and Controversies in Cosmetic Hair Restoration. Dermatol Surg. 2013; 39: 797-801.
- Harris JA. New Methodology and Instrumentation for Follicular Unit Extraction: Lower Follicle Transection Rates and Expanded Patient Candidacy. Dermatol Surg. 2006; 32: 56-61.
- Rashid RM. Follicular Unit Extraction with the Artas Robotic Hair Transplant System: An Evaluation of FUE Yield. Dermatol Online J. 2014; 20: 22341.
- Ors S, Ozkose M, Ors S. Follicular Unit Extraction Hair Transplantation with Micromotor: Eight Years Experience. Aesthetic Plast Surg. 2015; 39: 589-596.
- Gupta A. Microrefined Microfollicular Hair Transplant: A New Modification in Hair Transplant. Ann Plast Surg. 2014; 73: 257-265.
- Stough DB 4th, Nelson BR, Stough DB 3rd. Incisional Slit Grafting. J Dermatol Surg Oncol. 1991; 17: 53-60.
- Nakatsui T, Wong J, Groot D. Survival of Densely Packed Follicular Unit Grafts using the Lateral Slit Technique. Dermatol Surg. 2008; 34: 1016-1022.
- Landau AG, Hudson DA, Adams K, Geldenhuys S, Pienaar C. Full-Thickness Skin Grafts: Maximizing Graft take using Negative Pressure Dressings to Prepare the Graft Bed. Ann Plast Surg. 2008; 60: 661-666.
- Gökrem S, Baser NT, Aslan G. Follicular Unit Extraction in Hair Transplantation: Personal Experience. Ann Plast Surg. 2008; 60: 127-133.
- Rousso DE, Presti PM. Follicular Unit Transplantation. Facial Plast Surg. 2008; 24: 381–388.
- Nusbaum AG, Rose PT, Nusbaum BP. Nonsurgical Therapy for Hair Loss. Facial Plast Surg Clin North Am. 2013; 21: 335-342.
- Sethi P, Bansal A. Direct Hair Transplantation: A Modified Follicular Unit Extraction Technique. J Cutan Aesthet Surg. 2013; 6: 100-105.
- Bernstein RM, Rassman WR. Follicular unit transplantation. In: Haber RS, Stough DB, editors. Hair Transplantation. Philadelphia: Elsevier Saunders. 2006; 91-98.
- Venkataram M. Changing Trends in Hair Restoration Surgery. Indian J Dermatol Venereol Leprol. 2006; 72: 103-111.
- Bouhanna P. Androgenetic alopecia: Combining medical and surgical treatments. Dermatol Surg. 2002; 28: 136-142.
- Avram MR, Cole JP, Gandelman M, Haber R, Knudsen R, Leavitt MT, et al. The Potential Role of Minoxidil in the Hair Transplantation Setting. Dermatol Surg. 2002; 28: 894-900.
- Luis A. Garza, Yaping Liu, Zaixin Yang, Brinda Alagesan, John A Lawson, Scott M Norberg, et al. Prostaglandin D2 Inhibits Hair Growth and is Elevated in Bald Scalp of Men with Androgenetic Alopecia. Sci Transl Med. 2012; 4: 126-134.
- Blume-Peytavi U, Lönnfors S, Hillmann K, Garcia Bartels N. A Randomized Double-Blind Placebo-Controlled Pilot Study to Assess the Efficacy of a 24-Week Topical Treatment by Latanoprost 0.1% on Hair Growth and Pigmentation in Healthy Volunteers with Androgenetic Alopecia. J Am Acad Dermatol. 2012; 66: 794–800.
- Li ZJ, Choi HI, Choi DK, Sohn KC, Im M, Seo YJ, et al. Autologous Plateletrich Plasma: A Potential Therapeutic Tool for Promoting Hair Growth. Dermatol Surg. 2012; 38: 1040–1046.
- Rinaldi F. Improving the revascularization of transplanted hair follicles through up-regulation of angiogenic growth factors. Hair Transplant Forum Int’l. 2005; 17: 117–126.
- Greco J, Brandt R. Preliminary experience and extended applications for the use of autologous platelet-rich plasma in hair transplantation surgery. 2007.
- Uebel CO, da Silva JB, Cantarelli D, Martins P. The Role of Platelet Plasma Growth Factors in Male Pattern Baldness Surgery. Plast Reconstr Surg. 2006; 118: 1458–1466.
- Cooley JE. Optimal graft growth. Facial Plast Surg Clin North Am. 2013; 21: 449-55.
- Parsley WM, Perez-Meza D. Review of Factors Affecting the Growth and Survival of Follicular Grafts. J Cutan Aesthet Surg. 2010; 3: 69-75.
- Bernstein RM. Measurements in Hair Restoration. Hair Transplant Forum International. 1998; 8: 27.
- Chang SC. Estimation of number of grafts and donor area. Hair Transplant Forum Int. 2001; 11: 101-103.
- Bernstein RM, Rassman WR. The Logic of Follicular Unit Transplantation. Dermatol Clin. 1999; 17: 277-295.
- Unger WP. Density Issue in Hair Transplantation. Dermatol Surg. 1998; 24: 297.
- Bernstein RM, Rassman WR, Szaniawski W, Halperin A. Follicular transplantation. Int J Aesth Rest Surg. 1995; 3: 119-132.
- Okuda S. The study of clinical experiments of hair transplantation. Japan J Dermatol Urol. A939; 46: 135-138.
- Cole JP. An analysis of follicular punches, mechanics, and dynamics in follicular unit extraction. Facial Plast Surg Clin North Am. 2013; 21: 437-447.
- NeoGraft Hair Transplant Machine for FUE.
- Konior RJ. Complications in hair-restoration surgery. Facial Plast Surg Clin North Am. 2013; 21: 505-520.
- Li S, Thangapazham RL, Wang JA, Rajesh S, Kao TC, Sperling L, et al. Human TSC2-null fibroblast-like cells induce hair follicle neogenesis and hamartoma morphogenesis. Nat Commun. 2011; 2: 235.
- Marshall BT, Ingraham CA, Wu X, Washenik K. Future horizons in hair restoration. Facial Plast Surg Clin North Am. 2013; 21: 521-528.
- Takahashi K, Yamanaka S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell. 2006; 126: 663–676.
- Koh-ei Toyoshima, Kyosuke Asakawa, Naoko Ishibashi, Hiroshi Toki, Miho Ogawa, Tomoko Hasegawa, et al. Fully functional hair follicle regeneration through the rearrangement of stem cells and their niches. Nat Commun. 2012; 3: 784.