Case Report
A Case Report of Traumatic Perineal Degloving Injury
Joel Lau, Xuxin Lim, Ong Wei Chen, Yap Yan Lin, Jane Lim* and Lim Thiam Chye
Department of Surgery, National University Health System, Singapore
*Corresponding author: Jane Lim, Department of Surgery, Division of Plastic Reconstructive and Aesthetic Surgery, National University Health System, 1E Kent Ridge Rd, 119074, Singapore
Published: 25 Jan, 2017
Cite this article as: Lau J, Lim X, Chen OW, Lin YY, Lim J,
Chye LT. A Case Report of Traumatic
Perineal Degloving Injury. Clin Surg.
2017; 2: 1286.
Abstract
Introduction: Degloving injuries are most commonly caused by road traffic accidents and industrial accidents. They result from of a large rotational force, which avulses the skin and subcutaneous
tissue from the underlying fascia. The majority of such injuries involve the lower extremities.
Perineal degloving injury is uncommon and seldom reported in the literature.
Presentation of Case: In this case report, we present the case of a 22 year old male pedestrian
involved in a motor vehicle accident. He sustained an open perineal degloving injury.
Discussion: The management of perineal degloving injuries involves resuscitation and early
identification of bony fractures, urogenital or anorectal injuries. A multi-disciplinary team should
be activated to aid in the management of such injuries. Multiple wound irrigation with staged
debridement can salvage potentially viable degloved segments. The degloved skin flaps should be
secured to the wound bed without tension for the first 5 days. Additionally, the patient should
be nursed on a differential air-loss mattress. Delayed wound closure can be undertaken once full
demarcation has occurred.
Conclusion: Careful serial excision of devitalized tissues prior to reconstruction minimizes tissue
loss, minimizes septic complications and reduces patient’s morbidity.
Keywords: Perineal Injury; Degloving Injury; Perineal Trauma; Case Report
Introduction
A degloving injury is a result of a rotational force that stretches the skin and subcutaneous tissue causing its avulsion from the deeper less mobile musculoskeletal structures. It is commonly caused by motor vehicle and industrial accidents [1]. Degloving injuries of the perineum are anatomically complex involving the urogenital, anorectal, pelvic and sacrococcygeal structures. A multidisciplinary team consisting of surgeons from Plastic, General (i.e. trauma and colorectal), Orthopedic and Urological surgery is needed in the management of such injuries. This case reports, documents the management of an open perineal degloving injury (Table 1). It is written in accordance with the CARE guidelines [2].
Case Presentation
Patient information
Our patient, a 22 year old male, was a pedestrian involved in a motor vehicle accident, who
presented to the Emergency Medicine Department at the National University Hospital. His initial
blood pressure was 119/66 mmHg, heart rate 110 beats per minutes and oxygen saturation 99% on
oxygen delivered via nasal prong. He was alert with a Glasgow Coma Scale score of 14 (Eye 4, Verbal
4, Motor 6). He was found to have sustained extensive degloving injuries to his perineum.
Diagnostic assessment & clinical findings
Computer tomography (CT) scan of his abdomen and pelvis showed a comminuted fracture
of the right hemi-sacrum with anterior displacement of the distal sacral fragment & coccyx. No
pneumoperitoneum or hemoperitoneum was visible. Chest X-Ray showed no pneumothorax or
rib fractures. X-Rays of his lower extremities showed no long bone fractures. CT scan of his brain
and face revealed a scalp hematoma along the left occipital region, fracture of the maxillary alveolar
process and fracture of the right zygomatic arch.
The patient underwent examination under anesthesia (EUA) in the supine lithotomy position
(Figure 1). The tip of the coccyx was fractured and exposed. The anococcygeal body was avulsed. The
anus, together with a cuff of perianal skin was displaced anteriorly. A 6 cm perineal laceration was
present in the anterior, urogenital triangle exposing but not penetrating the underlying superficial
perineal (Colles’) fascia. The laceration extended from the anal verge
to the base of the scrotal sac. The degloved subcutaneous tissue flaps
(i.e. left gluteal, right gluteal and sacral) exposed the underlying left
and right Gluteal maximus muscle. The sacral degloved segments
extended superiorly to 15 cm above the lumbar and sacral regions.
The left degloving injury extended 15 cm laterally and the right 8 cm
laterally in multiple planes. Deep to the Gluteal maximus muscle, the
left superior gluteal artery was identified and preserved. The right
superior gluteal artery was avulsed. Other cutaneous injuries include
lacerations and abrasions over his face, trunks and limbs.
The integrity of the anorectal canal was confirmed by
sigmoidoscopy. A de-functioning sigmoid loop colostomy was
fashioned and the efferent colonic limb was washed out with
normal saline. The degloved skin flaps was thoroughly irrigated and
hemostasis secured. The wound bed was packed with gauze dressing
and the degloved skin flaps were returned to the wound bed without
tension, kinking or suturing. The patient was nursed on a differential
air loss mattress to minimize pressure necrosis.
Intervention
Serial wound washouts and debridement were performed till
complete skin closure was achieved (Figure 2). On post-injury day
1, the anterior perineal laceration was sutured (Figure 2A). The tips
(distal 5 mm) of the sacrum and left triangular gluteal skin flaps
were found to be dusky with slow capillary refill time (Figure 3). The
remainder of the flaps appeared well perfused. Negative pressure
wound therapy (NPWT) with continuous pressure of 125 mmHg
was applied over the wounds (Figure 3). By post-injury day 4, the
tips (distal 10 mm) of the sacral and left triangular gluteal flaps were
necrotic. Their apices were debrided until punctuate dermal bleeding
was seen (Figure 2B). Staged wound closure commenced on the 4th
post injury day. The anterior border of the left triangular gluteal flap
was reduced to its anatomical position and sutured in place (Figure
2C). A portable NPWT dressing was applied. The patient was able
to ambulate by day 4. The sacral degloved flap was repaired last. As
there was too much tension to allow for anatomical reduction, the
lateral tissues were advanced towards the midline position in a V-Y
fashion to ensure a tension free repair (Figure 2D). Complete closure
was achieved within 8 days.
Follow-up and outcome
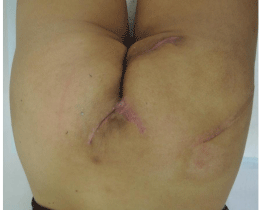
The patient was seen in the outpatient colorectal and plastic clinic
and assessed to have good sphincter tone and complete wound union
in his perineum (Figure 4). He underwent an uneventful reversal of
his loop colostomy 3 months after the initial injury.
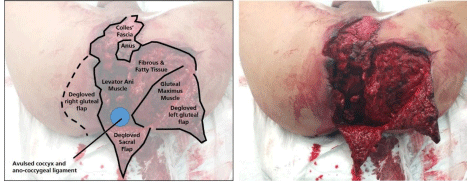
Figure 1
Figure 1
Initial appearance of the patient’s perineal degloving injury when examined under anesthesia.
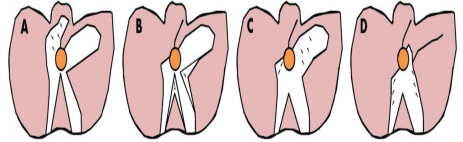
Figure 2
Figure 2
(A) Closure of anterior perineal laceration on post-injury day1
(B) Debridement of necrotic tips
(C) Closure of anterior border of left degloved segment on post-injury day 4
(D) V-Y closure of sacral degloved segment on post-injury day 7.
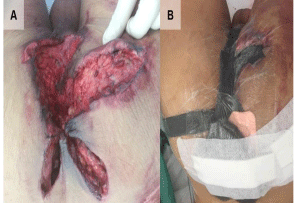
Figure 3
Figure 3
Perineal degloving injury on post-injury day1
(A) pre-op
(B) postop with VAC dressing applied.
Discussion
The nature of this injury was initially described by Slack in 1952
as a form of torsional injury [1]. He described the mechanism of
shearing resulting from large rotational forces i.e. such as a spinning
tire, causing traumatic avulsion of the skin and subcutaneous tissue
from underlying musculoskeletal structures. While the avulsed
skin flap may initially appear viable, it is not reflective of the true
extent of the injury [2]. The skin contains a rich vascular plexus
within the dermis that is supplied by perforators from underlying
muscles and fascia. Thus, degloving injuries often result in loss of
perforating musculo-cutaneous and fascio-cutaneous vessels. This
compromises the arterial supply to the degloved tissue posing a threat
to its viability. The venous drainage can be compromised resulting in
subsequent venous congestion, increased vascular pressure across the
dermal plexuses and ultimately flap necrosis [3]. Hence, if primary
re-attachment is attempted, these flaps often have high rates of flap
necrosis that can progress to severe wound infection [4].
An alternative proposition was radical excision and wound
coverage with skin grafting [5]. Farmer proposed excision of all nonviable
avulsed skin, defeating of the avulsed skin and utilizing that as
a full thickness skin graft for coverage in a single stage procedure [5].
This allowed for optimal coverage of the denuded areas with minimal
morbidity [4]. Early radical debridement is controversial as it can
lead to unnecessary tissue loss. In addition, deciding the excision
margins is difficult as there is no good method to assess viability
of the avulsed flap in the acute trauma setting. Another alternative
proposed involves serial examination of the degloved skin via dermal
bleeding, capillary refill and color of skin. The necrotic tissue can
then be debrided repeatedly with reconstruction performed once full
demarcation has occurred.
For treatment of anatomically complex perineal wounds,
the principles are to minimize tissue loss, and minimize wound
contamination. Sequential irrigation and debridement coupled with
the use of negative pressure wound therapy (NPWT) as a temporary
wound dressing help facilitate wound healing in a clean environment
[6]. NPWT protects the wound via polyurethane foam which is sealed
airtight by a polyvinyl foil [7]. A high negative pressure applied allows
for continuous drainage of the exudative fluids and necrotic tissue
from the wound bed [8,9]. This enhances wound care management
by reducing the need for frequent dressing change, reducing risk of
urinary contamination and reducing bacterial counts in the wound
[7,9].
From this case report, we documented the potential benefits
of serial excision of devitalized tissue prior to reconstruction. We
brought our patient to the operating theatre for a planned re-look on
post-injury day 1 and ensured hemostasis of the wound bed before
commencement of NPWT. The degloved skin flaps were secured
to the wound bed without tension and the patient was nursed on a
differential air-loss mattress. We used the NPWT (ActiV.A.C. Therapy
Unit) at continuous negative pressure of 125 mm Hg. Our decision
for the next re-look operation was clinically indicated based upon
the NPWT output or at about five days post-injury. Demarcation of
non-viable tissue is most pronounced after 24 hours with the distal
tip of the flap most affected. From our experience, the extent of
necrosis tapers over the course of the next few days with demarcation
established by day five to seven post-injury. The wound bed should be
clean with minimal exudation prior to reconstruction of the degloved
skin flap. In our patient, as tissue viability was in doubt at day 5, we
continued to perform debridement and staged closure with complete
wound closure achieved on day 8 post-injury. Based on the above
treatment approach, we were able to achieve wound closure without
the need for any skin grafting and without septic complications.
Our case report deals with a specific type of perineal degloving
injury and our management strategy should not be generalized. Our
patient did not sustained concomitant pelvic and lower extremities
fractures, rectal injuries, genitalia injuries or injuries to the great
vessels. These associated injuries which are common with perineal
trauma would necessitate additional surgical procedures such as
fracture stabilization, fecal and/or urinary diversion, testicular repair,
bladder repair and great vessel repair [10]. In these scenarios, a
multidisciplinary team consisting of surgeons from Plastic, General
(i.e. trauma and colorectal), Orthopedic and Urological surgery
would need to be involved.
Figure 4
Conclusion
The initial management of hemodynamic stabilization and evaluation of the extent of injuries should be carried out for all patients presenting with perineal trauma. Our approach deals with a specific presentation of an open perineal degloving injury which led to a favorable outcome. We document that degloving perineal injuries can be managed successfully with serial debridement coupled with temporary wound dressing utilizing NPWT. This approach minimizes tissue loss, minimizes septic complications and reduces patient’s morbidity. With other injuries involved, an individualized, multi-disciplinary approach should be employed..
References
- Slack CC. Friction injuries following road accidents. Br Med J. 1952; 2: 262-264.
- Gagnier JJ, Kienle G, Altman DG, Moher D, Sox H, Riley D; CARE Group. The CARE guidelines: consensus-based clinical case reporting guideline development. BMJ Case Rep. 2013; 110: 603-608.
- De Korte N, Dwars BJ, van der Werff JF. Degloving injury of an extremity. Is primary closure obsolete? J Trauma. 2009; 67: E60-61.
- Kudsk KA, Sheldon GF, Walton RL. Degloving injuries of the extremities and torso. J Trauma. 1981; 21: 835-839.
- Farmer AW. Treatment of avulsed skin flaps. Ann Surg. 1939; 110: 951- 999.
- Meara JG, Guo L, Smith JD, Pribaz JJ, Breuing KH, Orgill DP. Vacuumassisted closure in the treatment of degloving injuries. Ann Plast Surg. 1999; 42: 589-594.
- Labler, Trentz O. The use of vacuum assisted closure (VAC) in soft tissue injuries after high energy pelvic trauma. Langenbecks Arch Surg. 2007; 392: 601-609.
- Schaffzin DM, Douglas JM, Stahl TJ, Smith LE. Vacuum-assisted closure of complex perineal wounds. Dis Colon Rectum. 2004; 47: 1745-1748.
- Hao S, Juan L, Xin W. Treatment of traumatically cutaneous necrosis of buttocks using vacuum sealing drainage combined with ileostomy. Eur J Trauma Emerg Surg. 2016; 42: 87-90.
- Petrone P, Inaba K, Wasserberg N, Teixeira PG, Sarkisyan G, Dubose JJ, et al. Perineal injuries at a large urban trauma center: injury patterns and outcomes. Am Surg. 2009; 75: 317-320.