Research Article
The PEAK Plasma Blade may Reduce Postoperative Analgesic Medication use in Breast Cancer Surgery
Chi-Yu Huang1#, Hui-Yu Chiu2,3#, Hung-Wen Lai2,4,5,6 and Dar Ren Chen2,5*
1Department of Surgery, Lin Shin Hospital, Taiwan
2Comprehensive Breast Cancer Center, Changhua Christian Hospital, Taiwan
3School of Nursing, Chung Shan Medical University, Taiwan
4Endoscopic & Oncoplastic Breast Surgery Center, Changhua Christian Hospital, Taiwan
5Division of General Surgery, Changhua Christian Hospital, Taiwan
6School of Medicine, National Yang Ming University, Taiwan
#Equal contribution
*Corresponding author: Dar-Ren Chen, Comprehensive Breast Cancer Center, Changhua Christian Hospital, 135 Nanhsiao Street, Changhua 500, Taiwan
Published: 30 Dec, 2016
Cite this article as: Huang C-Y, Chiu H-Y, Lai H-W, Chen
DR. The PEAK Plasma Blade may
Reduce Postoperative Analgesic
Medication use in Breast Cancer
Surgery. Clin Surg. 2016; 1: 1278.
Abstract
Objective: Postoperative wound pain is one of common problems in modern breast surgery. With a lower energy spread, Plasma Blade potentially induces less tissue damage. This study was aimed to
investigate effects of Plasma Blade on postoperative wound pain.
Patients and Methods: The records of patients who underwent breast surgery by a single surgeon
from August 2012 to December 2012 were retrospectively collected. There were 13 and 24 patients
in groups Plasma Blade and traditional electrocautery; respectively. Postoperative wound pain was
evaluated with the Visual Analogue Scale (VAS).
Results: Varieties of VAS pain scores in group electrocautery were greater than that in group Plasma
Blade; the declining trend of pain score in group Plasma Blade was also greater than that in group
electrocautery. Furthermore, there was a significant decrease in analgesic medication use in group
Plasma Blade.
Conclusion: The Plasma Blade showed benefit in the reduction of postoperative pain and analgesic
medication use compared to traditional electro surgery.
Keywords: Mastectomy; Pain management; Postoperative; Surgical instruments
Introduction
The main goal in breast cancer surgery traditionally has been to achieve focal clearance and
prevent local recurrence. However, with the increased interest in pursuing a better cosmetic
outcome, the best way to achieve good wound healing has become a more and more important
issue. Traditional electrosurgical devices are in dissection and hemostasis. A significant thermal
injury to adjacent tissue is sometimes inevitable, and this may increase wound inflammation [1,2],
delay wound healing and result in a dissatisfying aesthetic outcome and wound pain [3,4].
The PEAK Plasma Blade is a novel surgical device that uses very brief, high-frequency pulses
of radiofrequency energy [5] to induce electrical plasma along the edge of a thin (12.5 μm), 99.5%
insulated electrode [6,7]. The Plasma Blade uses less total energy at a significantly lower temperature
than the traditional electrosurgical device (40-170°C vs. 200-350°C) [8]. This property may
theoretically lead to the advantages of less smoke during operation, less postoperative pain, and
better wound healing. Plasma Blade incisions had the same wound strength as scalpel incisions, and
less thermal damage than traditional electro surgery, in both animal [9] and human models [10].
Fine’s case control study showed the Plasma Blade may help reduce the risk of skin flap necrosis
after mastectomy and exhibited a better cosmetic outcome [11]. This study aimed to evaluate the
advantages of the Plasma Blade compared to traditional electro surgery relative to postoperative
wound pain.
Figure 1
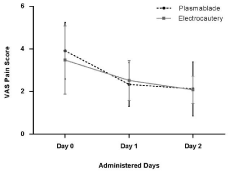
Figure 1
VAS pain scores of patients. On day 0 and day 1, varieties of VAS pain scores when using electrocautery were greater than those when using the Plasma Blade; the downgrade trend in the pain scores in the Plasma Blade group was also greater than in the electrocautery group.
Table 1
Table 1
Analgesic medications used on operation day and postoperative day 1 with different operative methods in the groups Plasma Blade and traditional electrocautery.
Patients and Methods
From August 2012 to December 2012, patients who received breast cancer surgery by a single
surgeon at the Changhua Christian Hospital (Changhua, Taiwan)
were enrolled. The PEAK Plasma Blade 4.0 Tissue Dissection Device
(PS200-040, Medtronic Advanced Energy LLC, and United States)
was used with 13 patients, and electro surgery with 24. Using the
PEAK Plasma Blade for surgery was decided by the patient's own due
to the differences in health insurance coverage.
Their medical records were retrospectively reviewed. The
operative method, blood loss, drainage amount, postoperative wound
pain and analgesic agent usage were documented and compared
between the two groups.
As general breast surgery procedures, the patient was prepared
for operation after anesthesia. The Plasma Blade was used for skin
incision, subcutaneous dissection and tumor excision, with the same
setting commonly used in breast surgery.
Postoperative pain was measured and documented using the
Visual Analogue Scale (VAS) during the operative day, and on
postoperative day 1 and day 2, because most of the patients were
discharged on day 2. In our clinical practice, oral non-steroidal
anti-inflammatory drug (NSAID) is routinely used in breast cancer
surgery patients since postoperative day 0. Acetaminophen (500 mg)
was routinely used after operation for pain relief. If the patient still
suffered from pain, we would give her a single dose of NSAID after
assessment. The extra analgesic medications used during the operative
day and on postoperative day 1 were recorded. The operative methods
for both groups are listed in Table 1.
Data analysis had been performed with SPSS (Statistical Package
for Social Science) 16.0 version.
Results
The varieties of VAS pain scores on day 0 and day 1 postoperatively
were greater when using electrocautery than when using the Plasma
Blade (Figure 1). The downgrade trend in the pain score with the
Plasma Blade was also greater than that when using electrocautery.
However, there is no statistical significance given for difference
between varieties of VAS pain score in day 0, day 1, and day 2 (p=0.23,
0.28 and 0.46).
Eighteen patients received breast-conserving surgery with
sentinel lymph node biopsy. During the operative day, most of the
patients in both groups needed an analgesic agent. However, during
postoperative day 1, none of the patients in the Plasma Blade group
needed analgesic agents, although most of the patients in the electro
surgery group still did. Similar results were noted in other subgroups.
In total, only one of 13 patients in the Plasma Blade group needed
analgesic medication during postoperative day 1, and 23 of 24 patients
in the electro surgery group did (p< 0.01) (Table 1). Besides, the blood
loss and drainage amount documented in both group showed no
statistic difference.
Discussion
Due to the shortened duty cycle and the electrode with a small
exposed area, the PEAK Plasma Blade consumes much less total
energy and has a much lower average power output than conventional
electro surgery to achieve an equivalent rate of tissue cutting, and
this may reduce collateral thermal damage [6 and 7]. This characteristic
revealed its benefit in cosmetic terms, with less skin or flap necrosis
during nipple-sparing or skin-sparing mastectomy [11-13], which
contributed to better wound healing and a more aesthetic outcome.
The downgrade of the pain score with the Plasma Blade has
tended to be greater than when using electrocautery. However, there
is no statistical significance in two groups. An unpublished trial
(ClinicalTrials.gov Identifier: NCT00986453) using VAS pain score
as primary end point but failed to show any significant difference. We
faced the same problem, and looked forward to another parameter to
show a benefit of Plasma Blade. The need of analgesia may indicate
higher degree of pain. Less demand of postoperative analgesic
medication in Plasma Blade group may imply less postoperative pain.
Fortunately, there was a significant difference between the two groups
in postoperative analgesic agent usage. On day 0 postoperatively,
all the patients in the electrosurgical group needed analgesic
medications, and most of the patients in the Plasma Blade group.
On day 1 postoperatively, this trend of analgesic medication usage
was becoming more obvious (Table 1). One possible explanation
could be the lesser amount of thermal injury depth, scarring, and
inflammation produced by the Plasma Blade. Loh et al. [9] reported
fewer CD3+ lymphocytes and macrophages in the wounds produced
by the Plasma Blade than by electro surgery [9]. With less energy
delivery, the Plasma Blade could produce less thermal injury, which
might lead to a less active inflammatory process. This low energy
delivery device also showed its benefit in the flap survival of bilateral
skin-sparing mastectomy reported by Rusby and Stolier [12,13].
Also, Plasma Blade showed shorten of drainage duration time and
amount without increase operation duration or the amount of blood
loss compared to electrocautery in Dogan’s study [14]. Electrocautery
applications in surgical operations produce smoke, which is due to
the incomplete combustion of electrical current in the tissues and
blood vessels that contains significant unknown chemicals and
biological forms; the potential hazards and cancer risk, should not be
ignored [15]. The lesser amount of evasive odorous smoke produced
by the Power Blade may have potential advantages for surgical staff
occupational health.
The limitations of this study include that all of the cases in the two
groups were selected retrospectively during the same period and in
a single institution, and the same surgeon performed all operations.
Since this was not a randomized controlled study, there could be some
bias in case selection and patient characteristics. Furthermore, neither
surgeon nor patient was blinded, which may influence objective pain
scores and usage of analgesic agents.
Once a patient knew that a novel device with lower energy delivery
was used during the operation, an anticipation of less pain and better
comfort could be expected, which might reduce the demand for
analgesic medication. In addition, the surgeon was not blinded. There
could have been more surgical precision and delicate dissection in the
Plasma Blade group, because people tend to pay more attention to a
new or unfamiliar device. Last, several kinds of surgical procedures
were included, and the case number of each was limited. Further
larger scale, randomized studies with controlled characteristics may
provide more significant and reliable data about the benefit of the
Plasma Blade in breast surgery.
Conclusion
PEAK Plasma Blade is a novel device that showed benefit in the reduction of postoperative pain and analgesic medication use compared to traditional electro surgery.
References
- Arashiro DS, Rapley JW, Cobb CM, Killoy WJ. Histologic evaluation of porcine skin incisions produced by CO2 laser, electrosurgery, and scalpel. Int J Periodontics Restorative Dent. 1996; 16: 479-491.
- Butler PE, Barry-Walsh C, Curren B, Grace PA, Leader M, Bouchier-Hayes D. Improved wound healing with a modified electrosurgical electrode. Br J Plast Surg. 1991; 44: 495-499.
- Hambley R, Hebda PA, Abell E, Cohen BA, Jegasothy BV. Wound healing of skin incisions produced by ultrasonically vibrating knife, scalpel, electrosurgery, and carbon dioxide laser. J Dermatol Surg Oncol. 1988; 14: 1213-1217.
- Keenan KM, Rodeheaver GT, Kenney JG, Edlich RF. Surgical cautery revisited. Am J Surg. 1984; 147: 818-821.
- Glover JL, Bendick PJ, Link WJ, Plunkett RJ. The plasma scalpel: a new thermal knife. Lasers Surg Med. 1982; 2: 101-106.
- Palanker D, Vankov A, Jayaraman P. On mechanisms of interaction in electrosurgery. New J Phys. 2008; 10: 123022.
- Palanker DV, Vankov A, Huie P. Electrosurgery with cellular precision. IEEE Trans Biomed Eng. 2008; 55: 838-841.
- Temperature profile report ETR-00023, data generated by internal testing in chicken breast. PEAK Surgical, Inc.
- Loh SA, Carlson GA, Chang EI, Huang E, Palanker D, Gurtner GC. Comparative healing of surgical incisions created by the PEAK PlasmaBlade, conventional electrosurgery, and a scalpel. Plast Reconstr Surg. 2009; 124: 1849-1859.
- Ruidiaz ME, Messmer D, Atmodjo DY, Vose JG, Huang EJ, Kummel AC, et al. Comparative healing of human cutaneous surgical incisions created by the PEAK PlasmaBlade, conventional electrosurgery, and a standard scalpel. Plast Reconstr Surg. 2011; 128: 104-111.
- Fine RE, Vose JG. Traditional electrosurgery and a low thermal injury dissection device yield different outcomes following bilateral skin-sparing mastectomy: a case report. J Med Case Rep. 2011; 5: 212.
- Rusby JE, Smith BL, Gui GP. Nipple-sparing mastectomy. Br J Surg. 2010; 97: 305-316.
- Stolier AJ, Levine EA. Reducing the risk of nipple necrosis: technical observations in 340 nipple-sparing mastectomies. Breast J. 2013; 19: 173- 179.
- Dogan L, Gulcelik MA, Yuksel M, Uyar O, Erdogan O, Reis E. The effect of plasmakinetic cautery on wound healing and complications in mastectomy. J Breast Cancer. 2013; 16: 198-201.
- Tseng HS, Liu SP, Uang SN, Yang LR, Lee SC, Liu YJ, et al. Cancer risk of incremental exposure to polycyclic aromatic hydrocarbons in electrocautery smoke for mastectomy personnel. World J Surg Oncol. 2014; 12: 31.