Case Report
Sclerotherapy and Resection of a Giant Lymphatic Malformation of the Head in a Neonate
Colin Muncie1*, Richard Whitlock1, Michael Morris1, Claude Harbarger2 and David Sawaya1
1Department of Pediatric Surgery, University of Mississippi Medical Center Jackson, MS, USA
2Department of Pediatric Otolaryngology, University of Mississippi Medical Center Jackson, MS, USA
*Corresponding author: Colin Muncie, Department of Pediatric Surgery, Department of Surgery, University of Mississippi Medical Center Jackson, USA
Published: 30 Dec, 2016
Cite this article as: Muncie C, Whitlock R, Morris M,
Harbarger C, Sawaya D. Sclerotherapy
and Resection of a Giant Lymphatic
Malformation of the Head in a Neonate.
Clin Surg. 2016; 1: 1275.
Abstract
Lymphatic malformations, sometimes referred to as “lymphangiomas” are composed of malformed,
dilated lymphatic channels. They should be removed either for cosmesis or function when located
in the head and neck region. They have traditionally been approached surgically. However, high
recurrence rates with surgery alone have caused multimodal therapy to be an attractive approach.
We present a case report of a giant macrocystic lesion of the head approached with staged therapy,
in an attempt to salvage the patient’s involved ear.
Keywords: Lymphatic Malformation; Neonate; Head
Introduction
Lymphatic malformations (LM) are non-malignant collections of enlarged lymphatic channels or vessels. They are most commonly found in the head and neck region of infants. Although benign, they tend to have a high rate of recurrence after resection. Due to this challenge, a variety of treatment modalities exist to remove these masses. This case report discusses the drainage, sclerotherapy, and delayed resection of a giant lymphatic malformation in the left temporal region of a neonate.
Case Presentation
This patient presented as a 2-day-old female, born at 38 weeks gestational age by uncomplicated
vaginal delivery. She was 2.8 kg at birth and had limited prenatal care. She was noted on delivery to
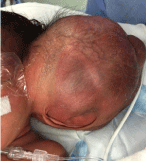
have a large fluid-filled mass on the left side of her head, displacing the ear inferiorly. The auricle
was noted to be floating on the surface of the cystic structure. Her mother had been unaware of any
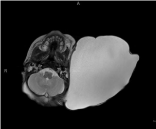
abnormalities prior to delivery. The mass was evaluated by MRI, which showed a large macrocystic,
fluid-filled lesion, without evidence of intracranial extension. The mass measured at 11 cm x 10
cm. After discussion with plastic surgery and otolaryngology, it was felt that the ear was potentially
viable. Due to concerns of local infection of the cyst, when erythema from the external auditory
meatus developed, antibiotics were initiated. When the cellulitis improved plans were made for
intervention.
At 2 weeks of age the patient underwent drainage followed with sclerotherapy in the operating
room. After decompression of 690 ml of straw colored fluid, 45 ml of doxycycline (15 mg/kg) were
injected into the cavity. A drain was left in place to aid with decompression and to maintain access
for potential future treatments.
Over the next several days it became apparent that the cartilage of the auricle was well developed
at that ear would be viable. Therefore the decision was made to perform resection and tacking of the
ear in the correct anatomical position. Due to risk of facial nerve injury at this age, restoration of
external auditory canal continuity planned to be delayed.
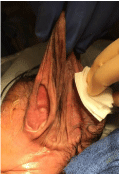
At 1-week post sclerotherapy the patient underwent planned resection. The majority of the
mass, along with some excess skin, was excised. A small portion of the cyst was noted to be adherent
to the posterior aspect of the auricle. The decision was made to ablate this tissue to avoid injuring the
blood supply to the ear. The pinna was fixed in the correct anatomical position, and the skin defect
was closed over a drain. Pathology report returned consistent with lymphatic malformation. The
patient recovered uneventfully in the neonatal intensive care unit. On post-op day 4, the Jackson
Pratt drain was removed. She was discharged home at 1 week post-op.
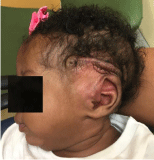
At her follow up in clinic at 2 months post-op, she showed an acceptable cosmetic result with
the ear in position in relation to the temporal bone. Some excess skin
was noted superiorly and posteriorly, but there was no evidence of
recurrence. Hearing screening on the left ear was performed at 2
months post-op and was interpreted as normal.
Figure 1
Figure 1
L. Temporal Lymphatic Malformation; note the external ear on the inferior margin of the mass.
Figure 2
Figure 3
Figure 4
Discussion
Lymphatic malformation, also referred to as cystic hygroma
or lymphangioma, is a rare benign malformation of lymphatic
vasculature. LMs are traditionally hamartomatous, with
approximately 75% of all cases being discovered in the cranio-facial
and cervical regions [1]. However, these malformations can occur
anywhere in the body, including the chest, abdomen, or axilla [2].
Approximately 66% of cystic lymphangiomas are present at birth,
with the majority presenting by the end of the second year of life.
Developmentally, LMs are thought to arise from sequestrations
of lymphatic vasculature, which fail to make appropriate connections
with draining vasculature [1]. They are classified based on size.
Microcystic lymphangiomas are described as containing cysts less
than 2 cm in size, while macrocystic lymphangiomas contain cysts
greater than 2 cm.
These typically present as a painless cystic mass in the head
and neck region. When discovered by antenatal ultrasound, airway
obstruction at birth can potentially be anticipated. An Ex-utero Intrapartum
Treatment (EXIT procedure) can be performed to avoid
prolonged intubation and hypoxia at birth [3]. Partial drainage of the
mass to assist with delivery at caesarian section has been reported.
In some cases, a tracheostomy may be required before the mass is
addressed [4]. However, if presenting after birth without airway
compromise these masses typically have an innocuous presentation.
Imaging workup can include ultrasound, CT or MRI. The important
distinction is whether the intra-cystic component of the mass is
macrocystic, microcystic or mixed.
Historically treatment was purely surgical in nature. However,
complete resection has been difficult, with recurrence rates as high
as 20%. Benazzou et al. [5] noted that a partial resection of head and
neck LMs had a 100% recurrence rate. Resection after recurrence
has been reported as extremely challenging in the literature [6]. This
has inspired the use of alternative therapies such as sclerotherapy.
This particular therapy involves drainage of the lesion followed by
injection of a solution to ablate the endothelium of the lymphatic
mass. Potential agents reported in the literature used for cervicofacial
or supraclavicular LMs include; hypertonic saline [4], ETOH [5],
sotradecol [7], doxycycline [7], and Ethibloc [8]. Bleomycin [9] is
an option for sclerotherapy that has been avoided due to reports of
pulmonary fibrosis after systemic use [9]. However, recent literature
reports it as effective in treating microcystic disease in children and
denied any evidence of pulmonary fibrosis with local use. OK432
has been reported as being used in Europe and Japan as a form
of sclerotherapy [10]. It contains cell components of neutralized
Streptococcus bacterium, which produce an inflammatory reaction
isolated to the cyst itself. Golinelli et al. [10] reported aspiration and
injection of OK432 in a supraclavicular LM with no recurrence at 2
years.
Although sclerotherapy as primary therapy has shown promise,
two limitations are important to keep in mind. The first is that repeated
injections are often required [8]. The second is that sclerotherapy is
similar to surgery in that it has a better response to macrocystic disease
than microcystic or mixed disease [7,8]. And, although the therapy
has displayed good results, reports continue in the literature showing
that primary surgery alone continues to have success [11]. Sanger
et al. [4] reported the use of combination therapy for treatment of a
mixed lesion. Although post-op imaging showed some deep residual
microcystic disease, recurrence was not appreciated. Due to the rarity
of these cases, no large studies exist comparing outcomes between
resection only to the use of sclerotherapy or a combination of the two.
Ghritlaharey et al. [11] reported successful primary resection in
a 3 month old with giant lymphangioma displacing the ear. Their
patient appeared to have maintained a structurally normal ear
with displacement. In our case, it was unclear if the patient would
benefit from surgery, as the ear may have become too distorted to be
functional. Therefore, initially sclerotherapy was performed with the
potential as being solitary therapy. When a structurally normal ear
appeared over several days the decision was made to proceed with
surgery so that the ear could be placed in the appropriate anatomical
position. This staged process afforded a good functional outcome for
our patient.
Conclusion
No general consensus has been made about the ideal treatment of lymphatic malformations in the head and neck region. However, the literature shows that macrocystic disease has a better response regardless of treatment used, when compared to microcystic disease. When faced with mixed disease the use of sclerotherapy and surgery simultaneously has shown good outcomes. Staging the combined approach is effective when the function of nearby structures is in question. It remains at the surgeon’s discretion which therapy is best given the situation.
References
- Fonkalsrud EW. Pediatric Surgery. 6th Edn. Mosby Inc. Lymphatic disorders. In: Grosfeld Jay L, O’Neill JA, Fonkalsrud EW, Coran AG, editors. 2006; 2: 2137–2146.
- Mirza B, Ijaz L, Saleem M, Sharif M, Sheikh A. Cystic Hygroma: An Overview. J Cutan Aesthet Surg. 2010; 3: 139- 144.
- Lazar DA, Olutoye OO, Moise KJ Jr, Ivey RT, Johnson A, Ayres N, et al. Ex-utero Intrapartum Treatment Procedure for Giant Neck Masses—fetal and Maternal Outcomes. J Pediatr Surg. 2011; 46: 817-822.
- Sanger C, Wong L, Wood J, David LR, Argenta LC. Giant Facial Lymphangioma. J Craniofac Surg. 2011; 22: 1271-1274.
- Benazzou S, Boulaadas M, Essakalli L. Giant Pediatric Cervicofacial Lymphatic Malformations. J Craniofac Surg. 2013; 24: 1307-1309.
- Seffah JD, Adu-Bonsaffoh K. "Giant Recurrent Cystic Lymphangioma: A Case Report." J West African College of Surgeons. 2014: 100-111.
- Farnoosh S, Don D, Koempel J, Panossian A, Anselmo D, Stanley P. Efficacy of Doxycycline and Sodium Tetradecyl Sulfate Sclerotherapy in Pediatric Head and Neck Lymphatic Malformations. Int J Pediatr Otorhinolaryngol. 2015; 79: 883-887.
- Emran MA, Dubois J, Laberge L, Al-Jazaeri A, Bütter A, Yazbeck S. Alcoholic Solution of Zein (Ethibloc) Sclerotherapy for Treatment of Lymphangiomas in Children. J Pediatr Surg. 2006; 41: 975-979.
- Chaudry G, Guevara CJ, Rialon KL, Kerr C, Mulliken JB, Greene AK, et al. Safety and Efficacy of Bleomycin Sclerotherapy for Microcystic Lymphatic Malformation. CardioVasc Intervent Radiol. 2014; 37: 1476-1481.
- Golinelli G, Toso A, Borello G, Aluffi P, Pia F. Percutaneous Sclerotherapy with OK-432 of a Cervicomediastinal Lymphangioma. Ann Thorac Surg. 2015; 100: 1879-1881.
- Ghritlaharey RK. Management of Giant Cystic Lymphangioma in an Infant. J Clin Diagn Res. 2013; 1755-1756.