Research Article
As the Population is Aging the Surgical Care Model Needs Refreshment: Implementation of a Vasculogeriatric Service for Vascular Surgical Patients in Australia
Ritter JC, Maher S, Bharat C, Stopher L, Ponosh S and Jansen S*
*Corresponding author: Shirley Jansen, Department of Vascular Surgery, Australian and New Zealand Society for Geriatric Medicine, Hobart, Australia
Published: 28 Dec, 2016
Cite this article as: Ritter JC, Maher S, Bharat C,
Stopher L, Ponosh S, Jansen S. As
the Population is Aging the Surgical
Care Model Needs Refreshment:
Implementation of a Vasculogeriatric
Service for Vascular Surgical Patients in
Australia. Clin Surg. 2016; 1: 1266.
Abstract
Introduction: Vascular surgical patients are elderly with multiple, significant co-morbidities requiring multi- specialist management. Optimal perioperative inpatient medical management may
have a positive impact on timely discharge. This study aims to investigate whether an integrated
geriatric service in a vascular surgical department reduces length of stay and cost.
Methods: A geriatric service was created as an integral part of a Vascular Surgical Unit in a tertiary
state referral center. In a retrospective cohort study design patient data was investigated six months
prior to installment of the service and the six months after.
Results: Total number of patients admitted was 669 (300 before, and 369 after institution of the
vasculogeiatric service. Patients with multiple admissions were excluded resulting in a patient
volume of 497. A significant reduction of length of stay was found after the introduction of the
vascular geriatric service (p= 0.003). This difference remains true when sub analysed for gender (p=
0.014), admission type (p< 0.001) and age (p= 0.012).
Conclusion: In this pilot study the institution of a vasculogeriatric service lead to a significant
reduction in LOS. The authors highly recommend this model of care, however specific benefits inpatient
care and impact on mortality needs evaluation in further studies.
Keywords: Vascular surgical procedures; geriatric medicine; Patient care; Length of stay gerontology; Healthcare economics
Introduction
Rising healthcare costs and progressively limited access to financial resources for individual
hospitals significantly influence daily medical practice [1]. In an effort to reduce cost socio-economic
factors are rapidly becoming an essential consideration in patient management. New pathways to
reduce the lengths of stay without compromising medical care are desirable.
Vascular surgical patients are generally elderly and have multiple, significant co-morbidities,
which impact their morbidity and mortality from vascular surgical intervention [2]. Management
of many of these co-morbidities is outside the expertise of the vascular surgeon and requires input
from mainly medical specialties. These multiple referral processes create delays in care pathways,
which become inefficient consequently delaying discharge to home, rehabilitation or another care
facility. As a result the length of stay increases negatively impacting on monetary cost, patient
turnover and availability of specialized tertiary service access.
In an in-hospital audit of vascular surgical inpatients at our institution, the authors determined
that patients waited an average of 8 days until all non-vascular specialist opinions, investigations
and management plans were obtained (unpublished data). In an effort to reduce any delays and
reduce the Length of Stay (LOS) a dedicated geriatric specialist service was embedded into the
vascular department. Hence, in addition to the surgical rounds a dedicated geriatric ward round
was installed as part of the daily routine addressing medical and social issues.
The aim of this pilot study was to determine whether the introduction of an integrated geriatric
service is feasible and has a positive impact on LOS for the vascular surgical patient.
Figure 1
Table 1
Methods
As this study was a retrospective analysis of a current hospital practice no approval from an
ethics committee had to be obtained. Sir Charles Gairdner Hospital
is a large teaching hospital providing a tertiary referral service for
Western Australia. With the support of the Western Australian
Health Service executive as part of the Quality Improvement Program
(QUIP) a Quality Program Geriatric Medicine (QPGM) was initiated.
A vasculogeriatric (VG) service was established in the form of a
consultant (0.3 Full Time Equivalents (FTE)) and registrar (0.5 FTE)
who would work as part of the vascular surgical staff to optimize the
management of vascular surgical patients.
From 1st June 2012 all patients admitted under the care of
vascular surgery were jointly managed with the VG service. The VG
team attended the weekly Grand Round, the weekly Multidisciplinary
Meeting and the weekly Joint Vascular Surgical / Radiology Meetings
in order to provide appropriate input into treatment goals, and
understand the vascular surgical management plans.
In addition, the VG registrar performed daily ward rounds and
the VG consultant provided 3 rounds weekly. The surgical team
made surgical and related decisions, whereas medical management
issues were preferentially managed by the VG team. There was close
collaboration at all times and a junior member of the vascular surgical
team would always accompany the VG registrar on ward rounds.
A 12 months period from December 2011 until December 2012
was investigated. Hospital data on length of stay of all patients
admitted under vascular surgery was collected from The Open
Patient Administrating System (TOPAS) for the six months prior
(Dec 2011-May 2012; pre QPGM)) and the six months during the VG
service (June 2012-Nov 2012; QPGM)). The data was analyzedfor the
relationship between length of stay (days) (LOS) and the following
variables: Quip (Pre QPGM/QPGM), patient age, Sex and type of
admission (Table 1) with emergency admissions pooled into one
subgroup. Summary statistics including mean, standard deviation,
minimum, maximum, median and interquartile range (IQR) are
provided for all continuous variables. Descriptive plots are provided
for relationships of interest. A Generalised Additive Models for
Location Scale and Shape (GAMLSS) model was used to analyse
length of stay and determine the effect of QPGM on length of stay.
Data were analysed using the R environment for statistical computing
[3].
Results
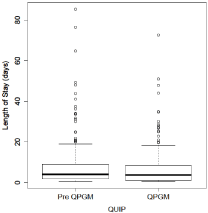
The number of patients admitted under the vascular service during the investigated period was 670. All individuals with multiple episodes of care were removed with the exception of their first admission (as determined from the admission year and month). This reduced the sample size from 670 to 497. One individual was also removed during the model fitting process as it was violating the underlying assumptions. Summary statistics have been provided with this individual removed. Table 2 contains summary statistics for length of stay (LOS) separated by QUIP group for all variables. A significant difference in LOS between QPGM and pre-QPGM (p-value = 0.003) with a raw difference of approximately 1.1 days is observed. This is also graphically demonstrated in the Box Plot separated by QUIP (Figure 1). Sex was also found to be significant (p-value = 0.014) with female staying an average of 1.3 days less. Looking at the raw data the difference from Pre-QPGM to QPGM is larger for males, whereas for females, though the mean decreased, the median stayed approximately the same (Table 3). Age (continuous) and admission code were also found to be significant (p-value 0.012 and < 0.001 respectively). Table 3 provides the summary statistics for sex, age groups and admission codes separated by QUIP. There was a reduction in median LOS from Pre QPGM to QPGM for all age groups except 55-64 and 65-74. A decrease was also observed in the median LOS for all 3 admission code groups - with the most noticeable difference being for admission code group 2 (decrease of 6 days).
Table 2
Table 2
Summary statistics for length of stay (LOS) separated by QUIP group for sex, age and admission category.
Table 3
Discussion
Vascular surgical patients have significant co-morbid
conditions related to risk factors for peripheral vascular disease
such as cardiac disease, smoking-related lung disease, hypertension,
hypercholesterolemia, diabetes and renal impairment. Many have
cognitive and functional impairments, particularly of mobility. In a
population with diminished physiological and psychological reserve,
foot wounds, lower limb surgery and amputation whether major or
minor, all impact on mobility and morbidity further. This ordinarily
creates delays in care pathways in vascular surgery, extending
in-patient stay, increasing time to rehabilitation, and increasing
cost. The management of medical conditions of older people is
traditionally the field of expertise of medical specialists. A geriatrician
is able to undertake the appropriate management of most medical
problems and facilitate the involvement of other specialists as needed.
Furthermore they have expertise in providing a holistic approach and
streamline service for their social requirements. This reduces the need
for many inter-specialty referrals and potential delayed discharge.
Our cohort study showed a significant reduction in length of
stay after the institution of an integrated geriatric service. This effect
was true for both genders and all age groups with the exception of
younger patients (55-74). It was also true for all admission categories,
whether elective or emergency, which implies a general applicability
regardless of pathology. Although the exact mechanisms have not
been investigated in detail in this study, there are various aspects
that explain the observed effect. The timely preoperative assessment
of inpatients requiring urgent treatment will be improved. Early
institution of cardio respiratory treatments will medically optimize
the patient. This will reduce the need for further non-vascular
investigations prior to surgery. Prior geriatric assessment may also
increase the acceptance for the necessity of additional consultations
by other relevant medical specialties. Although it seems logical
that quick preoperative patient optimization and elimination of
investigative and surgical delays will reduce perioperative morbidity
and mortality rates further studies are required. Similar advantages
apply to the management of incidental pathologies and geriatric
syndromes such as dementia, delirium, falls, incontinence and poly
pharmacy. These can be undertaken as an inpatient ensuring an
appropriate follow-up. In fact the American College of Surgeons
and the American Geriatric Society have published joint guidelines
in the National Surgical Quality Improvement Program (NSQIP) in
an effort to achieve structured geriatric assessment of preoperative
elderly patients [4].
Many vascular surgical patients require a period of rehabilitation
prior to discharge. Regularly they are rejected for reasons relating
to unresolved medical problems. A geriatrician will ensure that
medical issues are addressed, management plans established and
that there are reasonable rehabilitation goals to achieve. Transition
to rehabilitation is then safe and acceptable to the patient and the
receiving rehabilitation team. A geriatrician will also be able to
enhance discharge planning when rehabilitation is not required, but
medico social problems need addressing. Residential care, community
services, discussions about advanced care planning or terminal care
would fall into this category. Again, more detailed future studies
investigating patient outcome in this setting would be desirable.
In addition to the practical advantages of patient management
outlined above, there are significant benefits to the involved medical,
nursing and allied health personnel. Junior medical staffs as well
as the nursing staff have the opportunity of enhanced learning or
maintaining their skill of medicine as it pertains to the elderly and
having a reliable, single port of call for patient- related non- surgical
problems. At the same time it enables surgical trainees and senior
surgeons to focus on their core skills, whilst still able to have a
targeted discussion about medical problems of their patients with a
single senior physician.
Another significant conclusion that may be drawn from this
study is the potential for cost reduction. Traditionally multiplying
the length of stay by an average per-diem cost from external sources
derives this. Using figures from our institution (daily average hospital
cost 1666 AUD at the time of writing) the institution of a geriatric
vascular service yields a benefit of roughly 1830 AUD per admitted
patient. The authors are aware that there is significant controversy
in regards to appropriate and accurate patient cost estimation in
relation to length of stay [5,6]. In the times of activity based funding,
which is now applied to most health care systems, the cost related to
length of stay may decreasing in proportion. In fact quite complex
models for cost calculation are advocated in recent literature taking in
account multiple institutional, patient and economic factors [7,8]. It
can be therefore safely said, that LOS does have an impact on overall
hospitalization cost per patient and remains an important marker of
hospital efficiency. It further needs to be considered, that decreased
LOS results in faster patient turnover and higher total admissions per
year. Commercial business consultancies still consider reducing LOS
as an efficient way to increase hospital revenue [9]. A more detailed
cost analysis would be desirable and should be subject of further
research.
The authors are aware that there are limitations to their study. The
nature of a retrospective cohort study limited access to single patient
data. Hence, a detailed demographic comparison is lacking. However,
since a homogenous group of patients in an established facility was
investigated, it is fair to assume that the demographics did not change
with the employment of additional doctors. Also, whilst a quite
impressive effect on LOS and cost could be demonstrated it certainly
would have been of interest to look at rates of 30 day and long term
mortality and possibly number of specialty referrals. However, this is
study is meant as a pilot to establish the feasibility of a vasculogeriatic
service. The former aspects certainly need to be investigated in further
prospective research.
To the authors’ knowledge, this is the first time an integrated
geriatric service has been investigated in the vascular surgical setting.
Similar models have been studied and established in other surgical
specialties particularly orthopedic surgery. Both specialties, vascular
and orthopedic surgery, share a similar patient pool of the elderly
and frail with multiple comorbid conditions. They also regularly
suffer from impaired mobility. Orthogeriatric care was pioneered
in the 1950s in the UK by Devas and colleagues who reported
earlier restoration of patient independence and reduced length of
hospital stay [10]. A recent meta-analysis investigating the effect of
orthogeriatric care for patients with hip fractures found significant
reduction in mortality (long-term and in-hospital) as well as LOS
especially in the “shared care” model [11], Orthogeriatric care is
now considered best practice in most countries and in many it is
incorporated in the guidelines of the relevant societies or governing
bodies [12-14].
Furthermore, the benefits of Geriatric Evaluation and
Management (GEM) in improving patient outcomes, reducing
functional decline, mortality, readmissions, length of stay and cost,
are well known and have a strong evidence base [15-20]. Between
2004 and 2051 the proportion of the Western Australian population
aged over 65 years is predicted to increase from approximately 12%
to 26%. Those over 85 years of age will increase from 1% to 6% [21].
Efficient use of hospital beds will require excellent care of older people
with a focus on maintaining function during an episode of acute care
and moving into sub acute care quickly.
Conclusion
A joint vascular surgical and geriatric service reduces inpatient length of stay and cost. This is congruent with established joint geriatric services in other surgical specialties that deal with similar patient cohorts. Whether the improvement in perioperative care, secondary prevention and management of geriatric syndromes translates into improved morbidity and mortality remains a subject of further study. We recommend this model as a beneficial improvement in vascular surgical care.
References
- Australian Institute of Health and Welfare.
- Pham C, Gibb C, Field J, Gray J, Fitridge R, Marshall V, et al. Managing high-risk surgical patients: modifiable co-morbidities matter. ANZ J Surg. 2014; 84: 925-931.
- R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. 2013.
- American College of Surgeons National Surgical Quality Improvement Project.
- Taheri PA, Butz DA, Greenfield LJ. Length of stay has minimal impact on the cost of hospital admission. J Am Coll Surg. 2000; 191: 123-130.
- Raut M, Schein J, Mody S, Grant R, Benson C, Olson W. Estimating the economic impact of a half-day reduction in length of hospital stay among patients with community-acquired pneumonia in the U.S. Curr Med Res Opin. 2009; 25: 2151-2157.
- Ishak KJ, Stolar M, Ming-yi Hu, Alvarez P, Wang Y, Getsios D, et al. Accounting for the relationship between per diem cost and LOS when estimating hospitalisation costs. BMC Health Serv Res. 2012; 12: 439.
- Polverejan E, Gairdner JC, Bradley CJ, Holmes-Rovner M, Rovner D. Estimating mean hospital cost as a function of length of stay and patient characteristics. Health Econ. 2003; 12: 935-947.
- Milliman Consulting. http://publications.milliman.com/research/healthrr/ pdfs/Reducing-InPatient-Length-Stay-CC.pdf.
- Devas M, Ed. Geriatric orthopaedics. New York: Academic Press, 1977.
- Grigoryan KV, Javedan H, Rudolph JL. Orthogeriatric care models and outcomes in hip fracture patients: a systematic review and meta-analysis. J Orthop Trauma. 2014; 28: e49-55.
- Scottish Intercollegiate Guidelines Network. Prevention and Management of Hip Fracture in Older People. A national clinical guideline. SIGN publication no. 56. 2002.
- Department of Health. National Service Framework for Older People, DH: London. 2001.
- Australian and New Zeeland Society for Geriatric Medicine.
- Asplund K, Gustafson Y, Jacobsson C, Bucht G, Wahlin A, Peterson J, et al. Geriatric based versus general wards for older acute medical patients: a randomized comparison of outcomes and use of resources. J Am Geriatr Soc. 2000; 48: 1381-1388.
- Cohen HJ, Feussner JR, Weinberger M, Carnes M, Hamdy RC, Hsieh F, et al. A controlled trial of inpatient and outpatient geriatric evaluation and management. N Engl J Med. 2002; 346: 905-912.
- Ellis G, Whitehead MA, O’Neill D, Langhorne P, Robinson D. Comprehensive geriatric assessment for older adults admitted to hospital. Cochrane Database Syst Rev. 2011; 7: CD006211.
- Graham Ellis, Martin A Whitehead, David Robinson, Desmond O’Neill, Peter Langhorne. Comprehensive geriatric assessment for older adults admitted to hospital: meta-analysis of randomized controlled trials. BMJ. 2011; 343: d6553.
- Van Craen K, Braes T, Wellens N, Denhaerynck K, Flamaing J, Moons P, et al. The effectiveness of inpatient geriatric evaluation and management units: a systematic review and meta-analysis. J Am Geriatr Soc. 2010; 58: 83-92.
- Saltvedt I, Mo ES, Fayers P, Kaasa S, Sletvold O. Reduced mortality in treating acutely sick, frail older patients in a geriatric evaluation and management unit. A prospective randomized study J Am Geriatr Soc. 2002; 50: 792-798.
- Australian Bureau of Statistics. Population projections, Australia 3222.0- Table B5 Population projections by age and sex, WA.