Case Report
Periarterial Digital Sympathectomy for Severe Ischaemia of Raynaud`S
Sanjay Singh* and Moatasiem Bukhari
Department of Vascular Surgery, Royal Lancaster Infirmary, UK
*Corresponding author: Sanjay Singh, Department of Vascular Surgery, Royal Lancaster Infirmary, University Hospital of Morecambe Bay, 4, Rednal Park Court, Birmingham B38 8DS, UK
Published: 23 Dec, 2016
Cite this article as: Singh S, Bukhari M. Periarterial Digital
Sympathectomy for Severe Ischaemia
of Raynaud`S. Clin Surg. 2016; 1: 1258.
Abstract
Objective: The aim of the present study was to evaluate the results of periarterial digital
sympathectomy in cases of severe ischaemia of digits manifesting as digital ulceration and ischemic
pain refractory to medical treatments.
Methods: We reviewed all digital sympathectomise performed at our vascular unit between 2006-
2014. Demographics and outcomes were analyzed along with review of literature.
Results: Eleven patients representing 48 digits underwent periarterial digital sympathectomy for
severe ischaemia. Rest pain was resolved in all patient but in 2 patients recurrence occurred in
cold environment. Digital ulceration was healed completely in 92.8% (13/14). There were no major
complications of the surgery.
Conclusion: Our study findings demonstrate that digital artery sympathectomy is an effective
technique for diminution of pain, healing of ulcers and preservations of the digits in patients with
chronic digital ischemia. However we accept that multicentric prospective studies with standardized
inclusion criteria, timing for intervention and consistent follow up should be performed to evaluate
the efficacy and safety of digital sympathectomy before recommending the surgery to all cases of
chronic digital ischaemia.
Keywords: Digital sympathectomy; Raynaud`s Phenomenon; Ischaemia; Ulceration
Introduction
Digital ischemia in upper and lower extremity, with ulceration and gangrene can be a
manifestation of Raynaud’s phenomenon (RP). It is a difficult and frustrating problem to solve. The
early manifestation of RP may be in form of cold intolerance, ischemic pain and numbness; and in
severe cases manifested as ulceration and gangrene. The patients are usually referred to the vascular
surgeons when they have already developed refractory ulcers and necrosis of finger and toes. The
current conservative treatment includes pharmacological agents (calcium channel blockers and
prostaglandins); behavioural modifications (smoking cessation, avoidance of cold exposure and use
of gloves) and biofeedback therapies [1]. Although many pharmacological, behavioural and surgical
treatments have been reported, there is still no cure or gold standard therapy.
RP is excessively reduced blood flow in response to cold and emotional stress with manifestation
of discoloured fingers and toes. This was named after French Physician Maurice Raynaud (1834-
1881) who defined the first case in 1862 as episodic, symmetric, acral vasospasm characterized
by pallor, cyanosis, suffusion, and a sense of fullness or tautness, which may be painful [2]. RP is
classified as primary (Raynaud`s disease - cause unknown) and secondary (Raynaud`s syndrome -
identifiable cause). It is unusual to develop digital ulcers in primary RP but in secondary RP repeated
episodes of spasms can cause pitted scars and fingertip ulcers.
In severe cases of RP medical treatment is ineffective and this may lead to partial or complete
loss of digit. In cases refractory to medical treatment, surgical options in the form of open cervical
sympathectomy, endoscopic thoracic sympathectomy (ETS) and digital sympathectomy has been
used with varying results. Cervical sympathectomy has been used with either poor long term
results, as preganglionic sectioning does not remove all the sympathetic stimulations to the hand or
unpleasant side effects such as post operative compensatory hyperhidrosis. Both open and ETS have
high rate of initial relief but higher rates of recurrence [3]. Digital sympathectomy may be the only
salvage procedure to prevent amputation in cases refractory to medical treatment.
The aim of the present study was to evaluate the results of digital
sympathectomy in cases of severe ischaemia of digits manifesting as
digital ulceration and ischemic pain refractory to medical treatments.
Table 1
Table 2
Materials and Methods
A retrospective analysis of all digital sympathectomies performed
in our vascular unit between 2006-2014 was done. Eleven patients (7
females & 4 males) representing 48 affected digits (42 fingers and 6
toes) underwent digital sympathectomy for severe ischaemia. Patient
ages ranged from 37 to 76 years. All patients were Caucasian. Five
of the patients were heavy smokers (one of them had digital ulcers).
Digital ulcers were present in 11 digits. Preoperative pain was
present in all patients. All patients presented with cold intolerance,
numbness and worsening ischemic pain and had proximal vessel
disease excluded by arterial duplex scan and were refractory to
medical treatments. A written informed consent was given by all the
patients. Institutional review board approval was not needed as it was
a retrospective review. (Table 1) shows patient demographics.
The aetiology of the digital ischemia was 7 primary RP and 4
secondary RP (3 secondary to scleroderma and 1 vibration white
finger). Diagnosis of RP was made after a detailed history and
examination. All patients had full blood count, antinuclear antibodies
and ESR. We did not do any thermography tests. Out of the 7 primary
RP patients, 2 had an unusual presentation with finger tip ulcerations
which is not a typical presentation of primary RP, no secondary cause
for this presentation was found. All 3 patients with scleroderma
were referred by rheumatologists, diagnosed with limited cutaneous
systemic sclerosis and were found to be positive for autoantibodies
including antinuclear antibodies and anticentromere antibodies. The
patient with vibration white finger was a 51 year old male with severe
vasospasm and pain affecting the left hand for more than 15 years
related to his vibration machinery job and was not responding to any
medical treatment.
Preoperative conservative treatment included pharmacological
agents, such as calcium channel blockers, prostaglandins, and
behavioural modifications such as cessation of smoking, avoidance of
caffeinated drinks, and avoidance of cold exposure and use of gloves.
(Table 2) shows the different medications used pre operatively.
Patients were also evaluated for capillary refill, skin integrity, and
the presence or absence of ulcers or gangrenous areas and peripheral
pulses. All patients had proximal vessel duplex scans which did not
showed any occlusion or stenosis in proximal vessels. Hand held
Doppler scans showed triphasic signals which excluded digital artery
occlusion. Individual patient presentations are shown in (Table 3).
Parameters of interest included the postoperative resolution/
improvement of pain, ulcer healing and postoperative complications.
Surgical Technique of Digital Sympathectomy
All the procedures were done under general anaesthesia.
Perioperative antibiotic prophylaxis was administrated in all cases.
For digital sympathectomy in hand, a zigzag incision was made from
the distal palmer crease to web area. Using loupe magnification we
identified the common digital arteries and its bifurcation to proper
digital arteries. After identifying the vessels we stripped the adventitia
circumferentially from common digital arteries to proximal part
of both proper digital arteries of the affected digits. The length of
adventitia stripping was about 2 cms. Another incision was made in
the anatomical snuff box for access to the dorsal branch of the radial
artery and 2 cms circumferential stripping of radial artery was done.
Vessel patency was assessed, as no occluded segments were detected,
vascular reconstruction and vein grafting were not required.
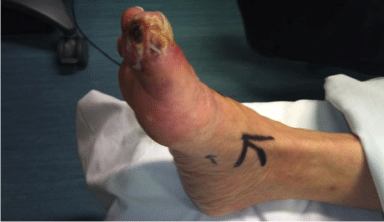
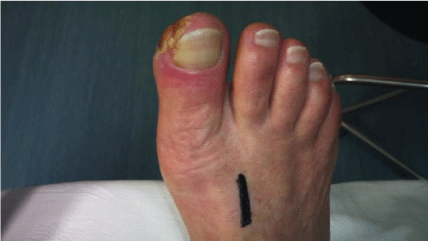
For digital sympathectomy in foot a vertical incisions was made
over the pre operative mark site in the first web space and another in
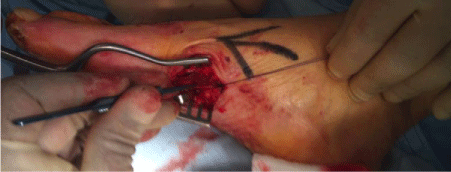
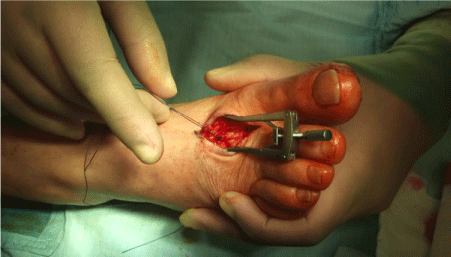
the mid-medial border of foot (Figure 1 and 2). In the web spaces,
dorsal metatarsal artery and it`s bifurcation into dorsal digital
arteries were identified, in the medial border of the foot medial
plantar artery identified (Figure 3 and 4). Intra operative Doppler was
used to confirm the arteries. Two cm circumferential stripping was
performed.
Post operatively the temperature and colour of digits were
observed, we did not use any vasodilator or therapeutic heparin post operatively.
Figure 1
Figure 2
Table 3
Figure 3
Figure 4
Results
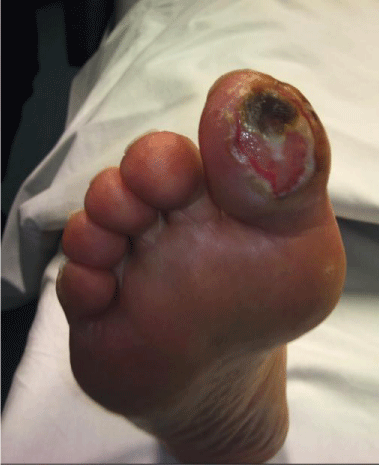
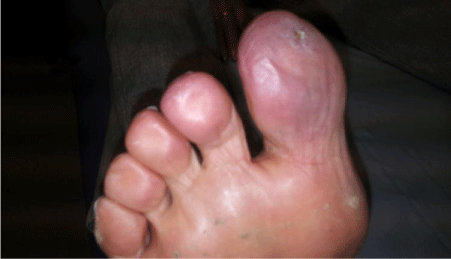
In our study 11 patients underwent digital sympathectomies representing 48 digits (42 hand digits & 6 toes). Rest pain was resolved in all the patients except in two patients where pain returned in cold environment. Ulcerations and gangrenous areas were healed completely in 92.8% (13/14). However recurrent ulcer formation in 2 digits needed digital amputation after 6 months and 1 year respectively. There were no major complications of the surgery except 8 digital paresthesia; 6 resolved and 2 are under surveillance. The duration of follow up ranged from 6-72 months (median follow up of 24 months). Except 1 all patients who were smokers stopped smoking during the follow up period. The details of post operative outcomes are shown in (Table 4). (Figure 5) shows preoperative photograph of the great toe with ulcer. Figure 6 shows three month postoperative photograph showing complete ulcer healing.
Table 4
Discussion
Patients suffering from severe form of RP may develop critical
digital ischemia, with ulceration and gangrene at the fingertips.
Although medical treatment with calcium channel blockers and
other vasodilators is now widely used in this disease, it is unsuccessful
in many cases and digits are at risk needing amputation. Surgical
interventions to prevent amputation include cervicothoracic
sympathectomy, ETS, digital sympathectomy and microvascular
constructions with or without vein graft. Literature search has shown
spinal cord stimulation to help refractory cases of digital ischaemia,
but it`s effectiveness is limited and associated with complications
such as infection, bleeding, dural puncture as well as high cost of
treatment [4].
Sympathectomy either open or endoscopic is an invasive
procedure, most patients have initial improvement in symptoms
of RP but a relapse almost occurs after a period of six months [5].
Thune et al. [6] did a retrospective study of patients treated for RP
by thoracoscopic sympathectomy and concluded that ETS side effects
are frequent, excellent immediate effects and one third achieve a long
term effect.
Flatt in 1980 [7] first reported successful digital artery
sympathectomy for the treatment of Raynaud’s phenomenon.
He stripped the adventitia from the common digital arteries and
separated the digital nerves from these vessels for a length of 3-4
mm. He advocated that sympathectomy was more effective at more
distal levels such as the proper digital artery than proximal levels [7].
Wilgis [8] has reported a modified technique with increased length
of adventitial stripping of the proper digital artery or of the common
digital artery from 4 mm to 2 cm. El-Gammal and Blair [9] advocated
a more extensive approach by stripping the adventitia from the
ulnar and radial arteries at the wrist. Koman et al. [10] found a
significant improvement in the response to cold stress testing without
significant increase of the digital temperature after distal peripheral
sympathectomy, including adventitial stripping of the radial and
ulnar arteries, for a distance of 2 cm.
Mccall et al. [11] looked at digital sympathectomy as a salvage
procedure for severe ischemia in Raynaud`s in 7 patients. Six of the
7 ulcers healed, and one patient needed amputation of a digit. A long
term follow up study by Murata et al. [12] questions whether digital
sympathectomy should be performed when the digit is ischemic
rather than waiting for ulceration and gangrene. They followed up
7 patients with 39 digits with ischemia but no ulceration, digital
sympathectomy was performed and patients were followed for over
10 years. All patients were symptom free [12]. A systemic review of
the outcome of digital sympathectomy for treatment of chronic digital
ischemia found out that 14% of all patients required amputation and
18% had ulcer recurrence [13]. Hotchkiss et al. [14] treated a total of
33 patients and 78 digits surgically with either distal sympathectomy
or interposition vein graft or a combination of the two procedures.
All 33 patients had eventual healing of ulcers without amputation, 8
patients required a bypass to obtain adequate blood supply distally.
Momeni et al. [15] did a retrospective analysis of 17 patients with
scleroderma (26 hands), who underwent digital sympathectomy.
Digital ulcers healed in all patients with only 2 patients needing
amputation due to recurrence of ulcers. They concluded that peripheral
sympathectomy is well tolerated by patients of scleroderma, and it
is prudent to offer surgical treatment not as a last resort but rather
earlier in the disease.
In our study adventitial stripping for a length of 2 cm of the
involved arteries was sufficient to achieve adequate circulation to heal
the ulcers both in upper and lower extremities. Our long-term results
are similar to those of several previous works [11-14]. The goal is to
offer these patients pain relief as well as improve blood flow to the
digits and avoid amputation. For most of our patients reperfusion
was established intraoperatively, suggesting that both sympathetic
denervation and decompression of the ischemic vessels from the
fibrotic adventitia are important. Our observations are similar to
those of Yee, who has proposed this dual cause of vessel constriction
[16]. The narrowing of the vessel lumen is often a combination
of sympathetic activity and external compression caused by a
thickened adventitia or contraction of the tissues surrounding the
arteries. Perfusion of the hand is determined by a sufficient pressure
gradient that is achieved by increasing the luminal diameter with
sympathectomy and decompression. Thus, a high, increased pressure
gradient in the arteries and enhanced collateral circulation via the
cutaneous vessels may benefit the ischemic digits.
Although digital artery sympathectomy is effective in preventing
amputation, it is technically demanding and is highly dependent on
surgical skills. In most series, postoperative and intermediate followup
has shown good clinical results. However, it is possible that after
long time periods, periarterial fibrosis and digital ischemia may recur.
The limitations of the present study include its retrospective
design, small number of patients as well as short variable lengths of
follow up. The small number of patients with heterogenic etiology
of ischaemia precludes a meaningful statistical correlation. One may
criticize the fact that we did not perform preoperative angiogram as a
part of the preoperative work up.
Although it has been over three decades since Flatt [7] introduced
this procedure, it is surprising that surgery is still considered as
a last resort option. Our study findings demonstrate that digital
artery sympathectomy is an effective technique for diminution of
pain, healing of ulcers and preservations of the digits in patients
with chronic digital ischemia. However we accept that multicentric
prospective studies with standardized inclusion criteria, timing
for intervention and consistent follow up should be performed to
evaluate the efficacy and safety of digital sympathectomy before
recommending the surgery to all cases of chronic digital ischaemia.
Figure 5
Figure 6
Conclusion
Digital sympathectomy as a treatment modality for ischemic digits and toes have shown good outcome and it is a heroic salvage and not a futile exercise. We recommend this procedure to be carried out to salvage the digits in both extremities, in those patients who have disabling symptoms such as ischemic pain or ulceration and those who are refractory to medical therapy.
References
- Wang WH, Lai CS, Chang KP, Lee SS, Yang CC, Lin SD, et al. Peripheral sympathectomy for Raynaud`s phenomena: a salvage procedure. Kaohsiung J Med Sci. 2006; 22: 491-499.
- Bakst R, Merola JF, Franks AG Jr, Sanchez M. Raynaud`s phenomenan: Pathogenesis and management. J Am Acad Dermatol. 2008; 59: 633-653.
- Matsumoto Y, Ueyama T, Endo M, Sasaki H, Kasashima F, Abe Y, et al. Endoscopic thoracic sympathecotomy for Raynaud`s Phenomena. J Vasc Surg. 2002; 36: 57-61.
- Pedrini L, Mugroni F. Spinal cord stimulation for lower limb ischemic pain treatment. Interact Cardiovasc Thorac Surg. 2007; 6: 495-500.
- Claes G, Drott C, Gothberg G. Thoracoscopic sympathicotomy for arterial insufficiency. Eur J Surg. 1994; 572: 63-64.
- Thune TH, Ladegaard L, Licht PB. Thoracoscopic Sympathectomy for Raynaud`s phenomenon- a long term follow up study. Eur J Vasc Endovasc Surg. 2006; 32: 198-202.
- Flatt AE. Digital artery sympathectomy. J Hand Surg Am. 1980; 5: 550- 556.
- Wilgis EF. Digital Sympathectomy for vascular insufficiency. Hand Clin. 1985; 1: 361-367.
- El-Gammal TA, Blair WF. Digital periarterial sympathectomy for ischemic digital pain and ulcers. J Hand Surg Br. 1991; 16: 382-385.
- Koman LA, Smith BP, Pollock FE Jr, Smith TL, Pollock D, Russell GB. The microcirculatory effects of peripheral sympathectomy. J Hand Surg Am. 1995; 20: 709-717.
- McCall TE, Petersen DP, Wong LB. The use of digital sympathectomy as a salvage procedure for severe ischaemia of Raynaud`s disease and phenomenon. J Hand Surg Am. 1999; 24: 173-177.
- Murata K, Omakawa S, Kobata Y, Tanaka Y, Yajima H, Tamai S. Long term follow up peri-arterial sympathectomy for chronic digital ischaemia. J Hand Surg Eur Vol. 2012; 37: 788-793.
- Kotsis SV, Chung KC. A systemic review of the outcome of digital sympathectomy for treatment of chronic digital ischemia. J Rheumatol. 2003; 30: 1788-1792.
- Hotchkiss R, Marks T. Management of acute and chronic vascular conditions of the hand. Curr Rev Musculoskelet Med. 2014; 7: 47-52.
- Momeni A, Sorice SC, Valenzuela A, Florentino DF, Chung L, Chang J. Surgical treatment of systemic sclerosis- is it justified to offer peripheral sympathectomy earlier in the disease process? Microsurgery. 2015; 35: 441-446.
- Yee AM, Hotchkiss RN, Paget SA. Adventitial stripping: a digit saving procedure in refractory Raynaud`s phenomenon. J Rheumatol. 1998; 25: 269-276.