Research Article
On the use of Geometric Modeling to Predict Aortic Aneurysm Rupture
Sruthi L. Muluk1*, Pallavi D. Muluk2, Judy Shum3 and Ender A. Finol4
1Harvard College, Cambridge MA, USA
2The Ellis School, Pittsburgh PA, USA
3The MathWorks, Natick MA, USA
4University of Texas at San Antonio, USA
*Corresponding author: Sruthi L. Muluk, Harvard College, 294 Dunster Mail Ctr, 945 Memorial Drive, Cambridge, MA 02138-7544, USA
Published: 22 Dec, 2016
Cite this article as: Muluk SL, Muluk PD, Shum J, Finol EA.
On the use of Geometric Modeling to
Predict Aortic Aneurysm Rupture. Clin
Surg. 2016; 1: 1252.
Abstract
Background: Currently, the risk of abdominal aortic aneurysm (AAA) rupture is determined using the maximal diameter (Dmax) of the aorta. We sought in this study to identify a set of CT-based
geometric parameters that would better predict the risk of rupture than Dmax.
Methods: We obtained CT Scans from 180 patients (90 ruptured AAA, 90 elective AAA repair)
and then used automated software to calculate 1-dimensional, 2-dimensional, and 3-dimensional
geometric parameters for each AAA. Linear regression was used to identify univariate correlates
of membership in the rupture group. We then used stepwise backward elimination to generate a
logistic regression model for prediction of rupture.
Results: Linear regression identified 40 correlates of rupture. Following stepwise backward
elimination, we developed a multi-variate logistic regression model containing 15 geometric
parameters, including Dmax. This model was compared to a model containing Dmax alone. The
multivariate model correctly classified 98% of all cases, whereas the Dmax-only model correctly
classified 72% of cases. Receiver operating characteristic (ROC) analysis showed that the multivariate
model had an area-under-the-curve (AUC) of 0.995, as compared to 0.770 for the Dmax-only
model. This difference was highly significant (P< 0.0001).
Conclusion: This study demonstrates that a multivariable model using geometric factors entirely
measurable from CT scanning can be a better predictor of AAA rupture than maximum diameter
alone.
Introduction
Abdominal aortic aneurysms (AAA) are an important preventable cause of death in patients
over age 65. Currently, the rupture risk of AAA is determined based on measurement of the
maximum aortic diameter [2]. The current evidence-based threshold for surgical repair of AAA
is 5.5 cm. However, diameter is not always an accurate predictor of rupture risk. For example,
some aneurysms over 5.5 cm do not rupture, whereas a significant fractions of aneurysms that do
rupture have a diameter smaller than 5.5 cm [2,3]. Therefore, refinement in the ability to predict
AAA rupture would improve patient selection for AAA interventional treatment. In turn, this could
result in improved patient outcomes and better resource utilization.
The purpose of this investigation was to use computed tomography (CT) scan imaging data
to find if there exists a more accurate metric to predict aneurysm rupture than the standard of
care maximum diameter. Our focus was to use geometric parameters as potential predictors
of AAA rupture. We used image analysis to measure several 1-dimensional, 2-dimensional, and
3-dimensional geometric factors which describe the AAA and associated intraluminal thrombus.
Our hypothesis was that a model including multiple geometry-based parameters would be superior
to using maximum diameter alone as a predictor of AAA rupture. This hypothesis is supported by
previously published work on AAA geometry quantification [2,4,5].
Methods
This study was conducted with approval from the Institutional Review Boards of both Allegheny
General Hospital (Pittsburgh, PA) and Northwestern Memorial Hospital (Chicago, IL). We obtained
contrast-enhanced CT scans from the retrospective review of the
medical records of 180 patients, 90 of whom were either symptomatic
or had a confirmed ruptured AAA, and 90 who were asymptomatic
and had elective AAA repair. The images were processed using AAA
Vasc 1.0, in-house image analysis application developed at Carnegie
Mellon University to calculate the geometric parameters for each
AAA. This process, which was described previously [5-7] involved:
(1) image segmentation, including detection of the lumen, inner and
outer wall boundaries of the AAA, (2) 3-dimensional reconstruction
and meshing, and (3) computation of the geometric parameters that
describe the size, shape, curvature, and regional variations of wall
thickness.
Sixty geometric parameters were calculated for each AAA, as
shown in Table 1. These included 11 one-dimensional indices, 9
two-dimensional indices, 4 three-dimensional size indices, 1 threedimensional
shape index, 5 thrombus-related indices, 18 secondorder
curvature-based indices, and 12 wall-thickness indices. All
length metrics were measured in millimeters (mm). Measurement
of the geometric parameters depends heavily on identifying the wall
of the aorta, both in non-ruptured and in ruptured AAA cases. The
algorithm to identify the aortic all has been described and validated in
previous publications [5-7].
A linear regression analysis was performed to determine whether
each geometric parameter had a significant correlation (either positive
or negative) with membership in the rupture group, based on the use
of Med Calc (v16.8, Ostend, Belgium). Subsequently, a predictive
logistic regression model was developed in R (The R Foundation) by
using the significant parameters (based on a statistical significance
level of P< 0.05) in a stepwise backward elimination method [8].
The ensuing variables identified were then used to compare the
multivariate model’s predictive ability against that of the maximum
diameter alone, using Med Calc.
Table 1
Table 1
Description of the 60 geometric parameters evaluated by means of image-based quantitative geometric characterization, the binary outcome of the univariate
linear regression analysis, which yielded 40 parameters correlated with AAA rupture, and the binary outcome of the logistic regression model, which yielded 15 of the
correlates as statistically significant for the predictive model.
Table 2
Table 2
Coefficients, standard errors and P-values for the 15 significant
geometric correlates of the multivariate logistic regression model.
Figure 1
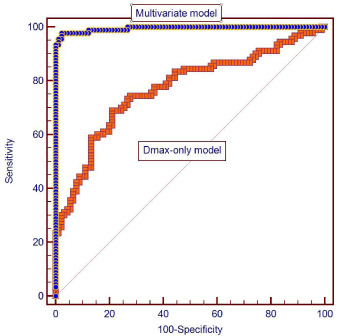
Figure 1
Receiver operating characteristic (ROC) curves for multivariate and
maximum diameter-only models. The area-under-the-curve is significantly
larger for the multivariate model indicating higher sensitivity and specificity of
the model for identifying an aneurysm as ruptured.
Table 3
Table 3
Coefficients, standard errors and P-values for aunivariate logistic
regression model that includes maximum diameter as the only geometric correlate.
Table 4
Table 4
Summary of classification results for multivariate logistic regression
model (with 15 geometric correlates) considering membership in elective repair or ruptured groups.
Table 5
Table 5
Summary of classification results for univariate logistic regression
model (with maximum diameter as the only correlate) considering membership in elective repair or ruptured groups.
Results
As shown in Table 1, univariate linear regression, using
membership in the rupture group as the dependent variable, identified
40 geometric parameters as significant correlates of rupture. The
latter were entered into a multivariate logistic regression model
and fifteen of the correlates were identified in this manner as being
statistically significant for the predictive model. Table 2 describes
the logistic regression coefficients for each parameter, the standard
error, and the P-value for each coefficient and for the constant in this
logistic regression equation. The model includes 4 one-dimensional
indices, 1 two-dimensional index, 1 three-dimensional size index, 1
thrombus-related index, 4 second-order curvature-based indices, and
4 wall-thickness indices.
For comparison, we used the same data set to create a univariate
logistic regression model using only maximum diameter (Dmax) as
the independent predictor. Table 3 shows the coefficient, the standard
error, and the P-value for Dmax and for the constant in this logistic
regression equation. In this model, the predicted probability of
rupture is greater than 50% when Dmax exceeds 61.2 mm.
The two predictive models were subsequently compared as
follows. Patients were predicted to belong to either the elective
repair or ruptured groups on the basis of the calculated probability
being < 50% or ≥50%. This predicted classification was compared to
the actual patient classification. Table 4 shows that the multivariate
model correctly classified 98% of the study patients. By contrast, the
Dmax-only model classified 72% of the patients, as shown in Table
5. Receiver operating characteristic (ROC) curves were constructed
for each model. As illustrated in Figure 1, the ROC curve for the
multivariate model had higher sensitivity and specificity for predicting
membership in the rupture group than the ROC curve of the Dmax-
only model. The area under the curve (AUC) for the multivariate
model was 0.995, while the AUC for the Dmax-only model was 0.770.
This difference was statistically significant (P< 0.0001).
Discussion
AAA maximum diameter is widely used clinically to assess the
probability of aneurysm rupture. However, recent image-based
modeling research suggests that the risk of rupture can be better
predicted using other metrics. These include wall stress [9-17], wall
shear stress [18], geometric factors other than diameter [2,4], and
thrombus-related factors [19,20].
The present work focused on the hypothesis that geometric
characteristics of the AAA sac and the associated thrombus could be
used to predict rupture. The analysis was limited to parameters that
can be measured from standard of care CT images. The methodology
used semi-automatic CT scan segmentation and meshing to
measure detailed geometric parameters of 180 patients with AAA.
Of these, 90 received elective repair due to the maximum diameter
of their aneurysm meeting or exceeding the critical value clinically
recommended for repair and 90 presented with rupture or were
symptomatic and received emergent repair within 1 month of the
CT scan used for this study. We found that a model using multiple
geometric parameters was far superior at classifying patients in the
ruptured or elective repair groups, compared to a model relying on
maximum diameter alone. Noteworthy is that our multivariate model
also includes maximum diameter as an important predictive factor.
A predictive model based on geometric parameters derived
from standard of care CT images is theoretically easier to implement
clinically than a model requiring biomechanical parameters such as
wall stress and shear stress. The rationale for this is that the accurate
calculation of stress requires the implementation of finite element
analysis or computational fluid dynamics modeling, and knowledge
of non-anatomic factors such as individual blood pressure and heart
rate at the time of administration of the CT scan. The geometric
parameters used in the current study require specialized software
analysis, but they can all be measured from the CT scan alone.
The multivariate regression model we identified in this study
correctly classified 98% of the patients we used to create the model,
whereas the Dmax-only regression model correctly classified only
72% of patients. This does not necessarily mean that the multivariate
model will correctly classify new AAA patients with the same level
of accuracy, specificity or sensitivity. Additional studies with larger
population groups will be necessary to determine the clinical utility
of the model. However, our findings suggest that rupture can be
better predicted using a multivariate model compared to measuring
maximum diameter only. This has important implications for
monitoring of AAA patients and selection of cases for surgery.
The fact that a multivariate model is a better classifier of patients
indicates that the additional geometric parameters besides Dmax have
an important role in determining whether an aneurysm ruptures. This
concept is consistent with several recent publications [2,4,9-12,15-
20]. Wall stress, AAA growth and rupture have all been shown to
be dependent on factors other than aneurysm diameter. The precise
biomechanical significance of the factors identified in the current
study remains to be clarified. Additional analysis will be needed to
determine, for example, whether these factors are associated with
changes in wall stress or material fatigue.
This investigation has important limitations. First, some of the
aneurysms in the elective repair group may have been close to rupture
had they not undergone elective surgical repair. There is no way to
know what might have happened to these otherwise asymptomatic
patients. Furthermore, most of the patients in our ruptured cohort
had already suffered rupture, an event that may substantively change
the AAA geometry compared with their state immediately before
rupture. This limitation is inherent in the study of this particular
subject, because it would be unethical to deny patients surgical
intervention for the purpose of monitoring them until they suffer
rupture. Additionally, stepwise backward elimination was used to
derive the multivariate model in this study but there are many other
methods that could have been used; potentially, other strategies such
as those based on machine learning techniques [4,21,22] may have
yielded a better model.
Conclusion
This study demonstrates that a multi-variable regression model using 15 geometric parameters measurable from standard of care computed tomography angiography images can be a better predictor of AAA rupture than maximum diameter alone.
Funding
Research funding from the Bill and Melinda Gates Foundation, Carnegie Mellon University’s Biomedical Engineering Department, the John and Claire Bertucci Graduate Fellowship program, and NIH grants R21EB007651, R21EB008804, and R15HL087268.
Acknowledgement
The authors gratefully acknowledge the valuable help of Mark Eskandari, MD for contributing the CT images from Northwestern University and Satish Muluk, MD for contributing the CT images from Allegheny General Hospital.
References
- Jeong JH, Kim JT, Kim NS, Cho JH, Kim JH, Oh JY, et al. Riskdiagnosis based on diameter of abdominal aortic aneurysm. Technol Health Care. 2016; 24: S569-S575.
- Raut SS, Chandra S, Shum J, Washington CB, Muluk SC, Rodriguez JF, et al. Biological. Geometric and biomechanical factors influencing abdominal aortic aneurysm rupture risk: A comprehensive review. Recent Patents Med Imaging. 2013; 3: 44-59.
- Darling RC, Messina CR, Brewster DC, Ottinger LW. Autopsystudy of unoperated abdominal aortic-aneurysms - Case for early resection. Circulation. 1977; 56: 161-164.
- Lee K, Zhu J, Shum J, Zhang Y, Muluk SC, Chandra A, et al. Surface curvature as a classifier of abdominal aortic aneurysms: a comparative analysis. Ann Biomed Eng. 2013; 41: 562-576.
- Shum J, Martufi G, Di Martino E, Washington CB, Grisafi J, Muluk SC, et al. Quantitative assessment of abdominal aortic aneurysm geometry. Ann Biomed Eng. 2010; 39: 277-286.
- Shum J, Di Martino ES, Goldhammer A, Goldman D, Acker L, Patel G, et al. Semiautomatic vessel wall detection and quantification of wall thickness in computed tomography images of human abdominal aortic aneurysms. Med Phys. 2010; 37: 638-648.
- Shum J, Xu A, Chatnuntawech I, Finol EA. A framework for the automatic generation of surface topologies for abdominal aortic aneurysm models. Ann Biomed Eng. 2011; 39: 249-259.
- R Core Team. R: A Language and Environment for Statistical Computing. 2013.
- Di Martino ES, Bohra A, Vande Geest JP, Gupta N, Makaroun MS, Vorp DA. Biomechanical properties of ruptured versus electively repaired abdominal aortic aneurysm wall tissue. J Vasc Surg. 2006; 43: 570-576.
- Di Martino ES, Guadagni G, Fumero A, Ballerini G, Spirito R, Biglioli P, et al. Fluid-structure interaction within realistic three-dimensional models of the aneurysmatic aorta as a guidance to assess the risk of rupture of the aneurysm. Med Eng Phys. 2001; 23: 647-655.
- Fillinger MF, Marra SP, Raghavan ML, Kennedy FE. Prediction of rupture risk in abdominal aortic aneurysm during observation: Wall stress versus diameter. J Vasc Surg. 2003; 37: 724-732.
- Fillinger MF, Racusin J, Baker RK, Cronenwett JL, Teutelink A, SchermerhornML, et al. Anatomic characteristics of ruptured abdominal aortic aneurysm on conventional CT scans: Implications for rupture risk. J Vasc Surg. 2004; 39: 1243-1252.
- Kleinstreuer C, Li Z. Analysis and computer program for rupture-risk prediction of abdominal aortic aneurysms. Biomed Eng Online. 2006; 5: 19.
- Larsson E, Labruto F, Gasser TC, Swedenborg J, Hultgren R. Analysis of aortic wall stress and rupture risk in patients with abdominal aortic aneurysm with a gender perspective. J Vasc Surg. 2011; 54: 295-299.
- Erhart P, Hyhlik-Dürr A, Geisbüsch P, Kotelis D, Müller-Eschner M, Gasser TC, et al. Finite element analysis in asymptomatic,symptomatic, and ruptured abdominal aortic aneurysms: in search of new rupturerisk predictors. Eur J Vasc Endovasc Surg. 2015; 49: 239-245.
- Khosla S, Morris DR, Moxon JV, Walker PJ, Gasser TC, Golledge J. Metaanalysis of peak wall stress in ruptured, symptomatic and intact abdominal aortic aneurysms. Br J Surg. 2014; 101: 1350-1357.
- Lindquist Liljeqvist M, Hultgren R, Gasser TC, Roy J. Volume growth of abdominal aortic aneurysms correlates with baseline volume and increasing finite element analysis-derived rupture risk. J Vasc Surg. 2016; 63: 1434-1442.
- Boyd AJ, Kuhn DCS, Lozowy RJ, Kulbisky GP. Low wall shear stress predominates at sites of abdominal aortic aneurysm rupture. J Vasc Surg. 2015; 63: 1-7.
- Thubrikar MJ, Robicsek F, Labrosse M, Chervenkoff V, Fowler BL. Effect of thrombus on abdominal aortic aneurysm wall dilation and stress. J Cardiovasc Surg. 2003; 44: 67-77.
- Vorp DA, Lee PC, Wang DHJ, Makaroun MS, Nemoto EM, Ogawa S, et al. Association of intraluminal thrombus in abdominal aortic aneurysm with local hypoxia and wall weakening. J Vasc Surg. 2001; 34: 291-299.
- Monsalve-Torra A, Ruiz-Fernandez D, Marin-Alonso O, Soriano-Payá A, Camacho-Mackenzie J, Carreño-Jaimes M. Using machine learning methods forpredicting inhospital mortality in patients undergoing open repair of abdominalaortic aneurysm. J Biomed Inform. 2016; 62: 195-201.
- Canchi T, Kumar SD, Ng EY, Narayanan S. A review of computational methods topredict the risk of rupture of abdominal aortic aneurysms. Biomed Res Int. 2015; 2015: 861627.