Research Article
Auditing the Results of a Surgical Team, In the Treatment of Prolapsed Haemorrhoid by Stapled Transanal Proctomucosectomy (Longo Operation)
Henrique Vasconcelos Dias*, Isabel Iria and António Menezes da Silva
Department of General and Digestive Surgery, Hospital de Santa Maria, Portugal
*Corresponding author: Henrique Guilherme Rodrigues de Vasconcelos Dias, Department of General and Digestive Surgery, Centro Hospitalar Lisboa Norte (CHLN), Portugal
Published: 14 Dec, 2016
Cite this article as: Dias HV, Iria I, da Silva AM. Auditing
the Results of a Surgical Team, In the
Treatment of Prolapsed Haemorrhoid by
Stapled Transanal Proctomucosectomy
(Longo Operation). Clin Surg. 2016; 1:
1249.
Abstract
The aim of this manuscript is to report the experience of a surgical team in the treatment of patients with prolapsed grades III and IV haemorrhoids, including total or partial circular prolapse, by
Stapled Transanal Proctomucosectomy (STP) or Longo operation, having audited the outcomes
of the first 636 patients operated by this method, during four years (2000–2004), in what concerns
the operation duration, hospital stay, pain or discomfort postoperative, recovery to normal activity,
complications and therapeutic efficacy.
In comparison with haemorrhoidectomy, in its various forms (Milligan and Morgan, Ferguson or
diathermy), the results, seems, in our experience, favouring the Longo operation because:
- Although the duration of operation is identical, the Longo operation is less surgeon dependent (more easy to teach and doing, once the patients were treated, under surveillance, by surgeons with different graduation, technical differentiation and experience).
- As this operation is a “painless” procedure without surgical wounds, the hospital stay is defined by the anaesthetic recovery.
- Early and late pain is limited to level 3 in 10, and virtually non-existent defecation discomfort.
- Recovery for work and normal activity of daily life is observed until the 5th of postoperative day.
- According to our experience, the only complication of this procedure was haemorrhage, which occurred in 19 patients (3%), and only one patient requiring reoperation.
- The therapeutic effectiveness was 87.4%. But we extended the indication to huge prolapse and grade IV prolapsed haemorrhoids and considered as “therapeutic failures” the two stage treatment, adequate to this extreme conditions.
Compared to haemorrhoidectomy, in its various forms, and according with the literature, the Longo operation having an equivalent efficacy to the Milligan and Morgan has, in addition to the above mentioned advantages, the absence of long term anal sequela because it is a purely rectal procedure.
Introduction
The haemorrhoidectomy, in its various forms – Milligan and Morgan, Ferguson or diathermy
-, was considered, for many years, the gold standard approach for the treatment of grade III or IV
haemorrhoids, and, by some authors, admitted as a treatment also suitable in haemorrhoids grade
II. For many years we have learned to perform these procedures and acquired a wide experience in
its use. Until 2004 it was the approach we used preferably with overlapping results in the literature.
However, these techniques, based on haemorrhoidectomy imply short, medium and long term,
undesirable consequences, and can be associated with serious complications, some of them difficult
to solve, such as faecal incontinence and scar stenosis of the anal canal.
Although it is relatively easy to excise the well-defined haemorrhoidal piles with moderate
dimensions, on the other hand, it is very complicated, especially in cases of total or partial circular
prolapse (bourrelet in French), as described by Tuttle in 1902, to ensure the conservation and
sustainability of "mucosal bridges" necessary to prevent the scar stenosis of the anal canal.
With regard to postoperative pain, it is always associated with these techniques and it is more
or less intense and more or less prolonged causing the inevitable
functional disability, and delay in the recovery of normal activity.
These complaints, undervalued in published studies, have the effect
of panic patients, making them delay the surgical treatment with all
its disadvantages. Thus, associated with haemorrhoidectomy, in its
various forms, we should consider, postoperative pain, the delay in
recovery, bleeding and, more rarely, the infection. Belatedly, the anal
stenosis, the residual fibrosis, the anal incontinence and soiling.
The anal stenosis, despite may be transient in most cases, is a
constant consequence of all these techniques, and manifests itself
in the medium or long term in severe cases. The residual fibrosis,
which is constant and determines the existence of zones of lesser
elasticity and resilience in the anal canal, favours the development
of anal fissures and these lead to further anal fibrosis. Finally, the
anal incontinence, which can be severe, related to a poor technique
associated to sphincter injury, in a milder form may assume the
aspect of soiling which is a frequent consequence of the excision of
the haemorrhoidal cushions, which under normal conditions form a
" hydrostatic valve " closing the anal canal and avoiding that slight but
uncomfortable incontinence.
In 1999 having the first contact with this different kind of
approach (STP), technique developed and published by Antonio
Longo (Longo Operation), we performed the first one successful
procedure. Enticed us its concept and good results, the ease of
performing, its reproducibility, and above all, do not interfere with
the anal canal, in what concerns its structure and function, the
maintenance of the haemorrhoidal cushions and the near absence of
pain and postoperative functional disability.
We considered particularly important the absence of scar anal
fibrosis, that is constant in haemorrhoidectomy and here does not
occur, since the anus is not involved. Moreover, as this procedure
consists, in reality, a prolapse reduction, the existence of well
individualized selvedge or pedicles does not hamper the technical
approach. So, encouraged by the results and the safety referred
in published articles, we started to practice this procedure in 2000
and treated 636 patients, between 2000 and 2004 (four years). It was
essential to us to assess the results of this experience, a common
practice in our team when introducing a new procedure. After
this evaluation, taking into account the good results observed, we
adopted, from 2004, the Longo operation, as our preferred technique
for the treatment of grades III and IV haemorrhoids, and so far, we
treated until now, around 4,000 patients.
In this meantime we announced the procedure, participating in
various meetings and organizing International Courses "Hands On".
Finally, we accede to publish, now, the audit results of the first 636
operated cases and the method we used [1-3].
Figure 1
Figure 2
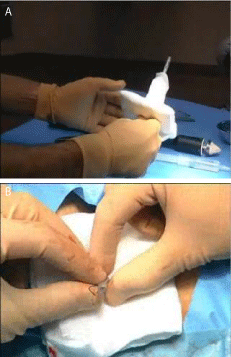
Figure 2
Haemostatic anal plug,
A: The soft tube in the centre to outwit bleeding;
B: Introduction in the anal canal.
Patients, Material and Methods
We operated 636 patients with haemorrhoids, 76% of grade
III and 24% grade IV, either by frankly individual pedicle or with
partial or total prolapse interesting from about 180 up to 360 in the
perimeter. The total or partial circular prolapse was not considered
important, once, unlike what happens in haemorrhoidectomy,
this does not affect the technique that is particularly useful in this
circumstance due to its circular nature.
Gender and age seem irrelevant to the selection of this treatment modality.
Patients preparation was made with cleaning enemas in day "-2"
at night, day "-1" in the morning and at night and in the morning of
operating day, associated low residue diet from the day "-3" favouring
the intake of liquids.
We gave all patients prophylactic antibiotic - Cefoxitin 1,000 mg
IV before the operation. The use of prophylactic antibiotic before
the operation result of the fearing of septic complications (Today,
long after the analysis that this study reports, we know that these
complications invariably are due to incorrect technique and antibiotic
therapy has no preventive role).
The type of mainly applied anaesthetic was spinals. This choice,
we do not consider particularly suitable as the preferred technique,
depended mainly from Anaesthesiologist option.
We used the Circular Stapler PPH® from Johnson & Johnson
and later CPH® developed by Check which is equivalent devices.
Occasionally we used some similar staplers, some of them made in
China, but their quality was not suitable according to the tests we
made.
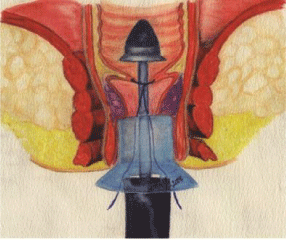
We fulfil the steps of the technique such as described by Longo:
sub mucosal ”tobacco pouch” suture, interested only mucosa, with
monofilament 0 to 00 with a 5/8 circle cylindrical atraumatic needle,
placed high in the rectum, above the base of the haemorrhoidal piles
pedicle, which is between 5 and 7 cm above the anal canal; placement
and introduction of the stapler exactly on anal canal axis (Figure 1);
waiting for about 2 minutes with the stapling closed before firing and
after a further 3 minutes before removing it (this manoeuvre is to
prevent bleeding and despite it was recommended both by technical
introducer Antonio Longo, either by the manufacturer of staple
machines Johnson & Johnson, was abandoned by our team after the
100 first cases, since having no relation or with bleeding or clotting
times).
We always put a haemostatic anal plug in the centre of which
put a soft tube (Figure 2) to outwit bleeding. Thus, we obtain an
assessment of the volume of losses and we can monitor them. We
believe significant loss greater than or equal to 100 cc, determining
that do buffering three Foley catheters with inflated balloons, for
about 6 to 12 hours [3-5].
The patients were evaluated in the first week, first month, 6
months and 1 year after surgery and the mean follow-up was about 2
to 3 years. Out of these periods any patient was promptly observed in
the case of any complaints. The observations made in the first week
and first month, unless there are suspected complications, did not
involve anuscopy to preserve the suture from trauma [6]. And that
is still our practice.
In our study we selected the following parameters to be evaluated:
- Operation duration independently the surgeon is a graduate or a trainee;
- Days of hospitalization;
- Pain or discomfort;
- Recovery to normal activity;
- Complications;
- Therapeutic efficacy
The incidence of pain or discomfort was evaluated under two
perspectives: the early pain (up to 48 hours), and the late pain, either
after the 48 hours, or following a free interval of complaints [7-10]. In
assessing the late pain was given particular relevance to the screening
and characterization of pain and discomfort during defecation, as
they are the main complains after haemorrhoidectomy.
Although septic complications may appear, more frequently
associated with the straight perforation when the suture is deeper
or stapling is not made respecting the axis of the anal canal, in
our experience we just had bleeding, so we only could assess this
complication.
With the objective to evaluate the effectiveness of this therapeutic
modality, we consider: relapse, recurrence of the disease and what
we call “insufficient treatment”, which is related to limitations of the
technique or the equipment and, according to our current experience,
although involving a reoperation, it can be considered as a treatment
in two stages.
This is not clear in the literature and is considered as relapse or
recurrence, but we must know that recurrences occur in all types
of surgical or instrumental treatment of haemorrhoid disease. In
spite of having extended this treatment to grade IV and selvedge
haemorrhoidal prolapse, prone to a two stage treatment, to ease the
discussion, we considered as treatment failure all the patients that
were not completely treated at the first operation.
Operation duration
Although the first cases had been operated by senior surgeons,
the last patients were operated also by younger surgeons and trainees,
once we understand to be an easily reproducible and easy to learn
procedure, after about 10 aid and adequate preparation from a
theoretical and practical point of view [11,12]. The mean operation
duration was 20 minutes (12' to 40'). There was no relationship
between this and the degree of differentiation of surgeons.
Hospital stay
As there is no need to hospital care before the operation (now we
currently perform this procedure in Ambulatory Surgery or Overnight
Surgery regime) we analyzed the postoperative hospitalization
period, which seems most appropriate [14]. Thus, considering only
this period, the mean postoperative length of hospital stay was 1.1
days (1 to 3 days). The longer hospital stays (3 days) result from
active postoperative bleeding, which occurred in 19 patients (3%),
and syndromes post spinal anaesthesia which we believe to be a bad
choice.
Pain or postoperative discomfort
Pain was assessed on a scale from 1 to 10, based on complaints of
patients and analgesic consumption. Although with some subjective
component, the pain related to the operation is one of the most
important factors in the treatment of haemorrhoids, reason that
seemed to us essential to assess [15]. Moreover, in the literature, this
kind of pain evaluation is also used in other therapeutic modalities,
including haemorrhoidectomy. So we distinguished:
- Postoperative early pain (until 36 or 48 hours if started within 24 hours after surgery).
- Postoperative late pain (between the 2nd and the 5th day)
Never exceed the level 3 (3 of 10), ranging between 1 and 3. The level 3 pain occurred only in very rare cases representing about 5% of all. Consequently, practically the patients do not consumed analgesics. The incidence of the rare cases of more severe pain (level 3) we believe was associated with relatively low suture lines (distal), as it decreased over the experience [16].
Occurred in 14% of cases, and never exceeded the level 3, in
almost all cases was associated with one of two circumstances: low
suture lines, involving the pedicles, or residual disease, this means,
large prolapse that could not be completely reduced after surgery. We
believe that in this particular circumstance it is associated with some
form of trauma caused by the anuscope device.
In any case, it should be noted that the Postoperative pain,
although in a subjective evaluation, has always been slight (maximum
level 3 in 10) and rare, only in about 19% of all patients either early
or late pain exceeded the level of a slight discomfort and reached the
level 3.
In the evaluation of postoperative pain, there is, from our point
of view, two very important aspects: the defecation pain and the
defecation discomfort.
Defecation pain was not reported by any patient in the first
postoperative defecation, but there were, however, a small percentage
of patients that referred late defecate pain or a stronger discomfort
[17-20]. These patients were divided in two groups: patients with
residual disease, and therefore candidates for reoperation; and
a very small percentage of patients in whom the suture was low,
corresponding to a technical error.
The discomfort defecation is hard to account and evaluate, due to
its subjectivity. Was not mentioned spontaneously by patients, and
when referred was always been very light, unless associated to pain
and urgency to defecate.
Complications
The complications of this procedure (Longo operation) may
be of four types: haemorrhage, septic complications (associated
with fistulas or perforation of the rectum), rectal stricture due to a
bad suture line with a rectum spiral, and chronic pain with intense
defecation pain related to intra anal or very low rectal sutures.
We just had, as complication, the haemorrhage, in the 636
patients we treated. Thus, scrupulously practicing the technique
described by Longo and Stutto, we had no septic complications, or
fistulae, strictures or chronic pain [21-25]. So, we only will analyse
the haemorrhage. This may appear early (immediate postoperative)
or lately (late in postoperative).
As early haemorrhage or perioperative haemorrhage, we
consider significant a bleeding equal or greater than 100 cc. As we
leave a haemostatic plug into the canal anal, whose centre we put a
soft tube to outwit bleeding, we obtain an assessment of the volume
of losses and we can monitor them. In these cases we try to control
bleeding by tamponade with three Foley catheters with the balloons
inflated, during around 6 to 12 hours. This type of buffering has
proved effective in almost all cases of bleeding having only one that
need an intervention for haemostasis review. Thus, in 636 patients
the haemorrhage was significant in 19 (3%) being resolved with
tamponade in 18 patients and requiring reoperation for revision of
haemostasis in one patient (0.2%).
Late bleeding was considered as the occurrence of a haemorrhage
between 1 week and 4 weeks after surgery. It occurred very sporadically
and was usually scarce and easily controllable. Those that took place
between the first and second weeks, were the most frequent and
related to patients under antiplatelet therapy, between the third and
fourth weeks occurred only in two cases (0.3%).
In assessing the late haemorrhage, we must consider the possibility
that not all patients have referred, or properly valued, the occurrence.
Recovery for work and normal activity
In most cases all patients were able to return to work and normal
activity of daily life around the fifth postoperative day, referring
significant improvement with the treatment, even those who had
residual disease or pain associated with low sutures. Adds the fact this
is a non wounds procedure.
Therapeutic effectiveness (residual disease, relapse and recurrence)
Of the 636 patients operated, only 80 (12.6%) needed reoperation,
what means the therapeutic effectiveness was 87.4%.
As, according to our opinion and practice, we operated grade
IV and selvedge haemorrhoidal prolapse, not all cases that require
a second intervention correspond to a recurrence or relapse. In fact,
most of them were associated to large prolapse, in which the option
of a second operation as a two stage treatment must be considered,
given the limitations of size of stapler.
Of the 80 patients a second Longo operation was performed in
48 (7.6%), and 32 patients (5%) required a haemorrhoidectomy, but
limited to one or two waste pedicles. In these cases, we admit that
there is what can be considered therapy failure, once the residual
pedicles correspond to a technical inefficiency or a runtime error.
These pedicles are, usually, much larger than the rest and require a
more appropriate and tailored approach.
So considering those circumstances what we can consider a “real”
therapeutic failure occurred only in 32 patients (5%) which may
mean a therapeutic effectiveness of 95%.
The stapled transanal proctomucosectomy with proctomucosopexy
(Longo operation) is based on two principles: first, the rectal mucosal
prolapse leading to the prolapse off the haemorrhoidal cushions
causes impairment of blood drainage in these structures as the veins
are distorted. This causes the vascular engorgement, oedema, swelling
and mucosal ulceration [26]. Thus, the treatment must be based on
prolapse reduction with the replacement of the haemorrhoidal
cushions, in order to regain their normal venous drainage, promoting
the restitutio ad integro of these lesions; second, the haemorrhoids or
haemorrhoidal cushions act as a hydrostatic valve, sealing the anal
canal, and improving the continence, mainly the continence of the
rectal mucus avoiding what we call the swelling. So, the treatment of
haemorrhoids must have in mind to preserve, whenever possible, the
haemorrhoidal cushions and their function.
The Longo operation meets these two objectives and reducing
the prolapse, normalizes the vascularisation and the venous drainage
of the haemorrhoid cushions, and reduces the swelling, the vascular
engorgement and the mucosal ulceration, leading, over time, to an
improvement or recovery of changes caused by the prolapse, without
sacrifice of the haemorrhoidal cushions and their function.
Indeed, in our experience of about 16 years of practice, we
observed, in most cases, a complete or almost complete recovery of
the total or partial circular prolapse, after replacement. This seems to
occur in a period of up to one year, after which we have the notion
that there is no further evolution. Based on that and, contrary to what
we did in these first 636 patients that we treated, now we postpone
one year the definition technical failure and in consequence a second
operation, unless it occurs an exceptional situation of particular
severity. This attitude resulted in a great decrease in reoperations and
so called therapeutic failures.
According to the analysis we made in this first 636 patients treated
by this method, is a well-tolerated procedure, with levels of pain and
discomfort that, at most, reach the level 3 (3 in 10), that does not
exceed the first week, except in cases related to a technical error (too
distal suture). Even in these cases, pain or discomfort did not exceed
two weeks. It provides a quick recovery with resumption of work and
normal activity within less than a week. Is a safe procedure if one
respects the correct technique, which seems to be easy, with a low rate
of serious complications? In a correct practice the complications are
limited to haemorrhage, generally with low incidence, low severity
and of easy resolution [27]. In this study only 3% of patients had
postoperative bleeding, and only one (0.2%) required reoperation.
The early postoperative bleeding may have some unclear relation
with the magnitude of the disease, but no relation with the patient’s
medication. On the other hand, when occasionally we used different
manufacturing staple devices more bleeding occurred, which leads us
to think that there may be a relationship that relates the occurrence of
bleeding with the quality of the device.
As for surgical sequels, the procedure does not affect the anal
canal, leaving no scarring areas that are weak points less elastic
and more prone anal fissures. As well, and for the same reasons,
the scar stricture of the anus is a non-existing problem. Finally, the
preservation of haemorrhoidal cushions keeps all the mechanisms of
anal continence.
This aspect of fibrotic and scar "weakness" of the anudermis and
mucosa, or the impaired continence and soiling, are particularly
important consequences of haemorrhoidectomies but they are not
particularly referred or valued, in most published articles [27-30].
Also the way the operation is well tolerated by patients, allows,
in large and complicated prolapsed haemorrhoids, to envisage the
implementation of a two stage treatment which is well accepted by
the patients.
Also, not providing the pain or morbidity that associated with
haemorrhoidectomy, the Longo Operation enables a greater adhesion
to surgical treatment and processing of a larger number of patients at
earlier stages of the disease, grade II/III, at which the results of any
such intervention are the best with the easily execution.
Now with a greater experience we can state that the modality
“treatment in two stages”, corresponds to an absolutely accepted
therapeutic strategy, associated with good results. Thus, the residual
disease should not be considered treatment failure. It can be treated
with a second Longo operation, because the total or partial circular
prolapse was not fully resolved in the first procedure. Relapses or
recurrence of the disease have not been observed, certainly occur, but
much later, in a period that exceeds our patient tracking capability,
i.e. after 4 to 5 years of surgery.
The technique is easily reproducible and, therefore, can be
performed by surgeons less differentiated, when properly trained and
oriented.
Finally, the situations of total or partial circular prolapse,
that always causes complicated technical problems in any type of
haemorrhoidectomy with a considerable risk off of stenosis, can be
treated by Longo operation in one or two stages with less morbidity
than any type of haemorrhoidectomy without stenosis risky.
Referring to noticed literature, the comparative studies are limited
to compare the Longo-operation with the Milligan and Morgan. Very
few are multicentre studies; is given little emphasis on long-term
results, with very few studies and referring to periods of follow-up
ranging from 1.5 to 3.5 years and, finally, it is given great importance
to the changes defecation but then concludes that its incidence is not
significant.
We noticed that in the literature as well, compared to
haemorrhoidectomy Milligan and Morgan, Longo Operation:
- Has less pain, shorter hospital stay and faster recovery to normal activity;
- One year after surgery both have the same effectiveness in solving symptoms;
- In a study with two years follow up: the incidence of late complications was the same (faecal impaction in Milligan and Morgan and pseudotrombosis in Longo); sphincter function alterations were identical and equal incidence (12% urgency, change of continence 10% and tenesmus 3%); the residual prolapse had an incidence of 7.5% on the Longo operation and only 1.8% in Milligan and Morgan. But we must notice that the residual prolapse of Longo operation can be solved with a second operation with much less morbidity and pain in the two procedures than in one Milligan and Morgan. On the other hand, the residual prolapse after Milligan and Morgan procedure cause a greater risk of stenosis if e second Milligan and Morgan is done;
- Also according to the literature, the success percentage evolves from 92% at 1 year to 89% at 2 years (87.4% In our experience) and in the case of grade IV haemorrhoids the risk of haemorrhage and, as expected most as well as the need for reoperation (usually well accepted by the patients), which is more frequently at most 43%, but after this previous results equal;
- Considering the scarce numbers of most of the series, the reluctance to include haemorrhoids grade IV and some such complications in our experience did not pass immediate and transitional effects, such as defecation urgency, we think this techniques accepted with some reserve which could have led to a prudent selection of patients and this would explain the good results.
As for the analyzed aspects it seems to us that we should consider
that literature, especially in comparative studies, considered with the
same importance sequels and transient disturbances which naturally
changes the nature of the results.
From our experience with haemorrhoidectomy techniques,
including Milligan and Morgan, which undoubtedly was the most we
practiced, we consider significant adverse aspects:
- Pain: Intense and incapacitating or in the Postoperative Period Immediate or Delayed the pain or the pain will defecation, conditioning this rather the occurrence of fecalomas by defence reaction and retraction of the patient.
- Scar fibrosis of anudermis and mucosa with decreased elasticity and brittleness at increased risk of fissures. In cases of very lush haemorrhoids requiring large resections, or in case of necrosis "mucosal bridges", can have the same scar stenosis that are very difficult to solve.
- Changes of continence are the most frequent condition of Soiling and may determine itching and skin changes. These changes are a final mode is not noticed on the long operation, but on the other hand had some incidence of Urgency defecate by increasing the pressure on the "cup" of the distal rectum, anal just at the place where they are nerve receptors defecation. This sensation disappeared by the 5th day and lasted only exceptionally in one case up to 3 months (associated with development/resolution to sub necessity of a manual suture for haemostasis during surgery).
Conclusion
From the analysis we made of the stapled transanal proctomucosectomy with proctomucosopexy (Longo operation), the first 636 patients we treated, we can conclude:
- The operation has a therapeutic efficacy similar to haemorrhoidectomy in its various forms: is feasible and effective with good results in grade IV haemorrhoids and large prolapse, if one accepts treatment in two stages, in most cases very well accepted and tolerated by patients.
- The procedure does not interfere with the anus, unlike haemorrhoidectomy, causes no harm nor leave permanent sequela, such as scar fibrosis that, reducing its elasticity, promote the occurrence of cracks.
- Preserving the haemorrhoidal cushions and its role of hydrostatic valve, unlike haemorrhoidectomy that dry out, preserves or improves anal continence, not being associated with soiling, itching or other consequences of haemorrhoidectomy.
- It is virtually painless and the occurrence of pain has a very short duration, is not associated with defecation pain and discomfort it causes is short (about 1 week) and very well tolerated. The analgesic consumption is virtually nil in the postoperative period.
- It provides a quick recovery, even in cases of advanced disease, this being obtained in the first week.
- Corresponds to a technique easy to teach and play, so it is easily performed even by surgeons with little differentiation, and Trainees.
- No need for postoperative care after the first hour and practically does not require medication.
- Although a significantly more expensive operation than the methods of haemorrhoidectomy, it seems economically viable and rewarding a social economic perspective.
References
- Adami B, Eckardt VF, Suermann RB, Karbach U, Ewe K. Bacteremia after proctoscopy and hemorrhoidal injection sclerotherapy. Dis Colon Rectum. 1981; 24: 373-374.
- Angelone G, Giardiello C, Prota C. Stapled hemorrhoidopexy. Complications and 2-year follow-up. Chir Ital. 2006; 58: 753-760.
- Altomare DF, Rinaldi M, Sallustio PL, Martino P, De Fazio M, Memeo V. Long-term effects of stapled haemorroidectomy on internal anal function and sensivity. Br J Surg. 2001: 88: 1487-1491.
- Beattie GC, Lam JPH, Loudon MA. A prospective evaluation of the introduction of circumferential stapled anoplasty in the management of haemorrhoids and mucosal prolapse. Colorectal Dis. 2000; 2: 137-142.
- Beattie GC, Loudon MA. Follow up confirms sustained benefit of circumferential stapled anoplasty in the management of prolapsing haemorrhoids. Br J Surg. 2001; 88: 850-852.
- Cerato MM, Cerato NL, Passos P, Treiguer A, Damin DC. Tratamento cirúrgico das hemorroidas: análise crítica das atuais opções (Surgical treatment of haemorrhoids: critical appraisal of the current options). ABCD Arq Bras Cir Dig. 2014; 27: 66-70.
- Eu KW, Lai JH. Stapled haemorrhoidectomy or Longo’s procedure? Two totally different concepts. Singapore Med J. 2005; 46: 566-567.
- Ferguson JA, Mazier WP, Ganchrow MI, Friend WG. The closed technique of hemorroidectomy. Surgery 1971; 79: 480-484.
- Ganio E, Altomare DF, Gabrielli F, Milito G, Canuti S. Prospective randomized multicentre trial comparing stapled with open hemorrhoidectomy. Br J Surg. 2001; 88: 669-674.
- Guy RJ, Ng CE, Eu KW. Stapled anoplasty for haemorrhoids: a comparison of ambulatory vs. in-patient procedures. Colorectal Dis. 2003; 5: 29-32.
- Guy RJ, Seow-Choen F. Septic complications after treatment of haemorrhoids. Br J Surg. 2003; 90: 147-156.
- Hetzer FH, Demartines N, Handschin AE, Clavien PA. Stapled vs excision hemorrhoidectomy long-term results of a prospective randomized trial. Arch Surg. 2002; 137: 337-340.
- Hoffman G, Firoosmand E. Haemorrhoids – to staple or not to staple: that is the question. Surgical Rounds, 2004; 27: 213-224.
- Jayaraman S, Colquhoun PH, Malthaner RA. Stapled versus conventional surgery for haemorrhoids. Cochrane Database Syst Rev. 2006; 4: D005393.
- Lohsiriwat V. Hemorrhoids: From basic pathophysiology to clinical management. World J Gastroenterol. 2012; 18: 2009-2017.
- Longo A. Treatment of hemorrhoidal disease by reduction of mucosa and hemorrhoidal prolapse with a circular suturing device: a new procedure. In: Proceedings of the 6th World Congress of Endoscopic Surgery. Bologna, Italy: Monduzzi Editore. 1998: 777-784.
- Mehigan BJ, Monson JR, Hartley JE. Stapling procedure for haemorrhoids versus Milligan-Morgan haemorrhoidectomy: randomised controlled trial. Lancet. 2000; 355: 782-785.
- Milligan ETC, Morgan CN. Surgical anatomy of the anal canal and operative treatment of haemorrhoids. Lancet. 1937; 2: 1119-1124.
- Nahas SC, Borba MR, Brochado MC, Marques CF, Nahas CS, Miotto-Neto B. Tratamento da doença hemorroidária pela técnica de grampeamento: análise de 100 casos (Stapled hemorrhoidectomy for the treatment of hemorrhoids). Arquivos de Gastroenterologia. 2003; 40.
- Nesselrod J. Hemorrhoidal disease. In: Proctology in general practice. W.B. Saunders Company, Philadelphia, London. 1950: 69-100.
- Ortiz H, Marzo J, Armendariz P. Randomized clinical trial of stapled hemorrhoidopexy versus conventional diathermy hemorrhoidectomy. Br J Surg. 2002; 89: 1376-1381.
- Papillon M, Arnaud JP, Descottes B, Gravie JF, Huten X, De Manzini N. Treatment of haemorrhoids with the Longo technique. Preliminary results of a prospective study on 94 cases. Chirurgie. 1999; 124: 666-669.
- Pescatori M, Gagliardi G. Postoperative complications after procedure for prolapsed haemorrhoids (PPH) and stapled transanal rectal resection (STARR) procedures. Tech Coloproctol. 2008; 12: 7-19.
- Ravo B, Amato A, Bianco V, Boccasanta P, Bottini C, Carriero A, et al. Complications after stapled haemorrhoidectomy: can they be prevented? Tech Coloproctol. 2002: 6: 83-88.
- Rowsell M, Bello M, Hemingway DM. Circunferenterial mucosectomy (stapled haemorrhoidectomy) versus conventional haemorrhoidectomy: randomized controlled trial. Lancet. 2000; 355: 779-781.
- Sayfan J. Complications of Milligan-Morgan hemorrhoidectomy. Dig Surg. 2001; 18: 131-133.
- Shalaby R, Desoky A. Randomized clinical trial of stapled versus Milligan- Morgan hemorrhoidectomy. Br J Surg. 2001; 88: 1049-1053.
- Smith LE, Goodreau JJ, Fouty WJ. Operative hemorrhoidectomy versus cryodestruction. Dis Colon Rectum. 1979; 22: 10-16.
- Sobrado CW, Cotti GC, Coelho FF, Rocha JR. Initial experience with stapled hemorrhoidopexy for treatment of hemorrhoids. Arquivos de Gastroenterologia. 2006; 43; 3.
- Yagmur Y, Yigit E, Bahce Z, Gumus S. Stapled Haemorrhoidopexy With Longo Process in the Treatment of 3rd and 4th degree Internal haemorrhoids and Rectal Mucosal Prolapsus: A Prospective Study. Journal of Gastroenterology and Hepatology Research. 2015; 4.