Research Article
Open Appendicectomy and the Surgical Trainee in Ireland. The Experience of a University Teaching Hospital
Norton S*, Anas M, Slattery C, Murphy JO and O’Donoghue G
Department of Surgery, University Hospital Waterford, Ireland
*Corresponding author: Norton S, Department of Surgery, University Hospital Waterford, Ireland
Published: 07 Dec, 2016
Cite this article as: Norton S, Anas M, Slattery C,
Murphy JO, O’Donoghue G. Open
Appendicectomy and the Surgical
Trainee in Ireland. The Experience of a
University Teaching Hospital. Clin Surg.
2016; 1: 1233.
Abstract
Introduction: Both societal changes and technological advancements in recent decades have
resulted in an evolutionary time for both surgical trainees and their mentors. A reduction in the
amount of available working hours and the introduction of minimally invasive surgery has resulted
in a need for an innovative approach to training our surgical trainees. This innovative approach
should be in the form of simulated surgical training.
Methods: The Hospital Inpatient Enquiry (HIPE) database was used to identify laparoscopic and
open appendicectomies performed during a 6 year period, from January 2009 to December 2014.
The rates of laparoscopic and open appendicectomy performed during the first three years (2009-
2011) were compared with those in the second three years (2012- 2014).
Results: Of 1072 appendicectomies performed over the six year period, 62% were Laparoscopic. The
median patient age, length of hospital stay, and the male to female ratio did not differ between the two
time periods studied. The open appendicectomy rate fell from 54% during the first half of the study
to 22.5% during the second half (p< 0.001). A significant increase in laparoscopic appendicectomy
rates were noted in both male and female patients, as well as in paediatric (8-16 years) and adult
(≥16 years) patients. Only 25(14.1%) open appendicectomies were performed in 2014.
Conclusion: Simulated surgical training provides a risk free and safe learning environment for
surgical trainees and should be utilised more in the National Surgical Training Programme in
Ireland.
Keywords: Laparoscopic appendicectomy; Open appendicectomy Ireland; Training; Technology
Introduction
Recent decades have brought with them several advances in medicine and surgery. One of the
main advances has been in technology. Selected early gastric cancer is now treated with endoscopic
submucosal or full thickness dissection combined with a laparoscopic lymphadenectomy if there
is a high risk of metastatic spread [1]. Research into biomaterials over the last twenty years have
revolutionised bone tissue engineering in orthopaedic surgery with 3rd generation biomaterials
being not only osteo-conductive but also osteo-inductive allowing in-situ tissues to regenerate and
combine with engineered tissues [2]. As imaging technologies improve it is likely that ultrasound
is destined to become the new stethoscope, giving all clinician easily accessible and better bedside
information regarding their patient [3]. The Da Vinci robot is changing the face of minimal access
surgery in urology and colorectal surgery. It not only offers a reduction in morbidity but also
allows the surgeon to overcome the challenges of reduced tactile perception in laparoscopic surgery
[4]. Furthermore the robot has been shown to give equivalent oncological outcomes to the open
surgery alternative. With these newly developing and improving technologies available in the field
of surgery, the modern surgeon has had to adapt and evolve technical skills in order to utilise these
advancements.
The laparoscopic approach to an appendicectomy is currently the treatment of choice for acute
appendicitis in Ireland. The laparoscopic appendicectomy is superior to the open procedure with
studies showing a reduction in wound infection rates, post-operative pain and shorter length of
hospital stay [5]. There has been some important societal changes in recent years. This has resulted in
concerns regarding the ability of core surgical trainees, on completion of basic surgical training, to be
able to perform a laparoscopic appendicectomy [6]. In 2009, the European Working Time Directive
(EWTD) placed a restriction of 48 working hours per week on Doctors [7]. Running parallel to this
is the newly introduced eight years National Surgical Training Programme in Ireland which has
further limited the time available for surgeons to become competent
on surgical training completion. Trainees are now faced with the need
for more technical skills than previously required. Furthermore, the
old apprenticeship model of “See one, do one, teach one” is no longer
viewed as an ethically acceptable learning environment in today’s
society due to increased patient risk. An innovative approach must
therefore be undertaken to ensure the proficiency and quality of
surgical training in Ireland.
This innovative approach must be in the form of simulated surgical
skills training. The American Board of Surgery expressed concerns
regarding many residents extending their training and not directly
entering practice on completion of training [8]. Simulated surgical
training removes the high pressured environment of the operating
theatre which is a suboptimal learning environment [8]. This training
can be low or advanced technology depending on the skills to be
learned at the surgical trainees’ relevant stage in career progression.
The risk free learning opportunity provided by simulation training
can be undertaken without infringing on the EWTD while allowing
trainees to enhance and improve technical skills.
Methods
A retrospective study was undertaken in the University Hospital Waterford, a main teaching hospital associated with the Royal College of Surgeons in Ireland training body. Patients were identified using the Hospital Inpatient Enquiry (HIPE) coding system. The aim was to analyse the number of open versus laparoscopic appendicectomies performed over a six year period (January 2009 to December 2014). Data was collected regarding patient age, gender and hospital length of stay post-operatively. The number of these procedures that were performed by surgical trainees in the final year of the study (2014) was also collected. A comparison was made based on two three year timelines, January 2009 to December 2011 and January 2012 to December 2014, period 1 and period 2, respectively. Post-operative complications were not recorded for the purposes of this study and the HIPE coding system did not allow for analysis of those procedures that converted from laparoscopic to open. A standard three port technique was used for the laparoscopic approach to the appendicectomy [9] . Information was obtained regarding the expectations set out by the Royal College of Surgeons in Ireland training body of a surgical trainee on completion of the higher surgical training programme.
Figure 1
Table 1
Figure 2
Figure 3
Figure 4
Results
A total of 1072 patients were included in the study. In period 1
(January 2009 to December 2014) there were 512 patients and 555
patients in period 2 (January 2012 to December 2014). The median
age was 20.1 and 20.9 in period 1 and 2 respectively (non-significant).
The male to female ratio and mean inpatient stay between the two
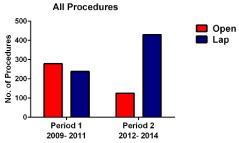
groups was also non-significant (Table 1). Open procedures decreased
from 54% to 23% between the two time periods and laparoscopic
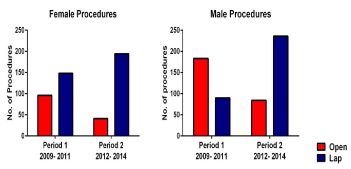
rates increased from 46% to 77% (Figure 1). There was an increase
in laparoscopic procedures undertaken in period 2 from 61% to 83%
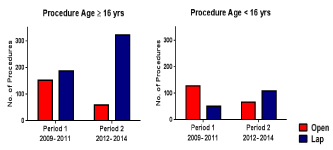
and 33% to 74% in females and males, respectively (Figure 2). This
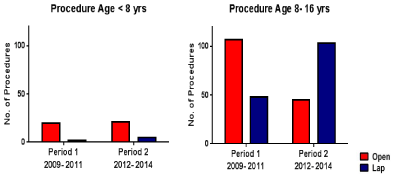
trend was evident in children between the ages of eight to sixteen
who had an increase in laparoscopic procedures from 31% in period
1 to 71% in period 2 (Figure 3 and 4). The same trend was not seen
however in children under eight, with the majority of this age group
still undergoing an open procedure (Figure 4).
Even with the trend for preference to laparoscopic procedures
clearly evident, of the 555 patients in period 2 who underwent an
appendicectomy 125 were performed by the open method (23%).
In 2014, the last year of our study, 177 appendicectomies were
performed, 14%(25) of these were open procedures. There were
a total of 14 trainees in UHW (7 Registrars and 7 Senior House
Officers). Therefore on average a trainee performed/assisted in < 2
open appendicectomies.
According to RCSI, a general surgical trainee should have
80 appendicectomies performed, which can be either open or
laparoscopic. A paediatric surgical trainee is required to have
performed at least 20 appendicectomies, and of these at least 20
(100% of required procedures) must be performed laparoscopically.
Discussion
Recent decades have brought with them advances in surgical technology. Our study shows an uptake in laparoscopic appendicectomy versus the open method in the later years of our study. This was with the exception of children under the age of eight. This is consistent with studies undertaken worldwide [10-11]. Furthermore, McCoy et al. [12] in 2013 reported that trainees in the United States were performing 50% less open appendicectomies, while those undertaken laparoscopically had increased by 542%. In Ireland, a recent study by Emmanuel et al. [13] reported that laparoscopic appendicectomies are a safe procedure for trainees to perform. However there has been a reported 50% reduction in the number of appendicectomies performed by basic surgical trainees in Ireland since the uptake in laparoscopy [14]. This highlights the need for increased surgical simulation training [15-16].
Conclusion
Simulation training removes the high pressure environment of the operating theatre. It allows trainees to improve surgical skills and practice dealing with emergency surgical scenarios prior to the real life situation. There are many similarities between pilots and surgeons – a high pressure work environment with detrimental outcomes to people if incorrect decisions are made. The aviation industry has been utilising simulation training for decades. Studies have shown that flight simulators have been a very effective method in improving psychomotor skills and in retaining these learned skills. With the introduction of the EWTD in Ireland, simulated surgical training is a realistic and useful resource in training core surgical trainees as an adjunct to the operating theatre.
References
- Kim MY, Cho JH, Cho JY. Ever-changing endoscopic treatment for early gastric cancer: Yesterday-today-tomorrow. World J Gastroenterol. 2014; 20: 13273-13283.
- Henkel J, Woodruff MA, Epari DR, Steck R, Glatt V, Dickinson IC, et al. Bone regeneration based on tissue engineering conceptions – A 21st century perspective. Bone Research. 2013; 3: 216-248.
- Gillman LM, Kirkpatrick AW. Portable bedside ultrasound: the visual stethoscope of the 21st century. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine. 2012; 20: 18.
- Roy S, Evans C. Overview of robotic colorectal surgery: Current and future practical developments. World J Gas-trointest Surg. 2016; 8: 143-150.
- Buia A, Stockhausen F, Hanisch E. Laparoscopic surgery: A qualified systematic review. World J Methodol. 2015; 5: 238-254.
- Mehmood S, Ahmed J, Anwar S, Ur Rehman S, El-Barghouti N. Letter to the editor. Appendicectomy as an index procedure to train junior surgical trainees in an era of reduced working hours. Int J Surg. 2011; 9: 441-442.
- Royal College of Surgeons. Surgery and the European working time directive – Background briefing. 2010.
- Samia H, Khan S, Lawrence J, Delaney CP. Simulation and its role in training. Clin Colon Rectal Surg. 2013; 26: 47-55.
- Semm K. Endoscopic appendectomy. Endoscopy. 1983; 15: 59–64.
- Masoomi H, Mills S, Dolich MO, Ketana N, Carmichael JC, Nguyen NT, et al. Comparison of outcomes of laparoscopic versus open appendectomy in adults: data from the Nationwide Inpatient Sample (NIS), 2006-2008. 2011; 15: 2226-2231.
- Ruffolo C, Fiorot A, Pagura G, Antoniutti M, Massani M, Caratozzolo E, et al. Acute appendicitis: What is the gold standard of treatment? World J Gastroenterol. 2013; 19: 8799-8807.
- McCoy AC, Gasevic E, Szlabick RE, Sahmoun AE, Sticca RP. Are open abdominal procedures a thing of the past? An analysis of graduation general surgery residents’ case logs from 2000 to 2011. J Surg Educ. 2013; 70: 683-689.
- Emmanuel A, Byrne J, Wilson I. Is laparoscopic appendicectomy a safe procedure for trainees in the peripheral hospital setting? Ir Med J. 2011; 104: 276-278.
- McCormick P, Tanner W, Keane F, Tierney S. Minimally Invasive Techniques in Common Surgical Procedures: Implications for Training. Irish J Med Sci. 2003; 172: 27-29.
- Lintern G, Roscoe SN, Koonce JM, Segal LD. Transfer of landing skills in beginning flight training. Human Factors: The Journal of the Human Factors and Ergonomics Society. Hum Factors. 1990; 32: 319-327.
- Hays R, Jacobs J, Prince C, Salas E. Flight simulator training effectiveness: a meta-analysis. Mil Psychol. 1992; 4: 63–74.