Case Report
AT: The Bony Tommy John Injury – Medial Epicondyle Fractures in Throwing Athletes
Carney DD, Wells L*, Akoto A, Aoyama J and Lowe J
Department of Surgery, Children’s Hospital Of Philadelphia, USA
*Corresponding author: Lawrence Wells, Department of Surgery, Children’s Hospital of Philadelphia, Main Campus 34th Street and Civic Center Boulevard, Philadelphia, PA 19104-4399, USA
Published: 06 Dec, 2016
Cite this article as: Carney DD, Wells L, Akoto A, Aoyama
J, Lowe J. AT: The Bony Tommy John
Injury – Medial Epicondyle Fractures in
Throwing Athletes. Clin Surg. 2016; 1:
1213.
Abstract
The optimal method of treatment for medial humeral epicondyle fractures in pediatric patients is
still controversial. This injury can occur due to excessive valgus stress placed on the elbow by the
pronator muscle mass that have a common point of origin at the medial epicondyle. In throwing
athletes such as baseball pitchers this can occur during a pitch. Non-operative as well as operative
management have been reported to have positive outcomes and lack consensus about when
either is indicated. This disparity is the root of the controversy. The only consensus for operative
intervention exists when there is incarceration of the fracture fragment in the joint space, ulnar
nerve involvement or dislocation. This report outlines the injury of a 15-year-old baseball player
who injured his elbow while pitching. His physical examination and x-rays confirmed a right-sided
medial humeral epicondyle fracture and treatment options were discussed. With the intention of a
speedy return to baseball and normal function, the patient and his family opted for open reduction
and internal fixation (ORIF).
Keywords: Medial epicondyle fracture; Elbow fracture; Throwing athletes
Introduction
The medial epicondyle serves as the origin of the flexor pronator musculature and the proximal
attachment of the medial ulnar collateral ligament (UCL). The flexor pronator mass functions as
a dynamic stabilizer of valgus stress to the elbow while the UCL acts as static stabilizer of static
stress to the same region. The UCL is comprised of 3 components or bundles: the anterior oblique,
posterior oblique, and transverse ligaments. The anterior oblique bundle resists most of the valgus
stress throughout both flexion and extension [1-3]. The median epicondyle is the third of six main
ossification centers which usually develops between the ages of 4-6 [4]. However, an open apophysis
is often present until the age of 14 to 15. The apophyseal cartilage is relatively weaker than the
ligaments that attach to it, and therefore, is a major determinant of possible injury to the medial
epicondyle in a subpopulation of individuals.
Fractures of the medial humeral epicondyle account for approximately 12% of all pediatric
elbow fractures [5]. These injuries most frequently occur within the age range of 9-14 and are four
times more common in males [5]. Avulsion fractures may result in young athletes who experience
a mechanical overload of the medial epicondylar apophysis [6]. This injury is especially common
amongst youth baseball players in particular, pitchers. A recent trend in single sport concentration
and year-round participation renders these young athletes more susceptible to ulnar nerve
dysfunction and avulsion fractures of the elbow [6].
The mechanism for acute avulsion fractures of the medial humeral epicondyle during baseball
pitching is a sudden increase in tension of the flexor pronator muscles and valgus stress on the
elbow, which in turn pulls the medial epicondyle from the humeral attachment site [7]. Repeated
valgus force can also successively contribute to an avulsion injury in this manner [8]. Treatment
for the fracture can be either non-operative or operative, with there being a fair amount of
disagreement about which of these two options is preferred [4]. Generally, avulsion fractures of the
medial humeral epicondyle with more than 5mm of displacement, presence of significant instability,
or containing fragments that are incarcerated in the joint space are treated with ORIF followed by
range of motion and strength rehabilitation [8]. For those fractures with minimal displacement or
no instability, treatment consists of immobilization in a long arm cast at 90 degrees for 3-4 weeks
followed by similar rehabilitation [9].
Here we describe a case of an avulsion fracture of the medial epicondyle which serves as an
excellent example one of the most common injuries among baseball
pitchers [8]. The focus of this case report will be to educate the reader
on the evaluation, diagnosis, treatment and prognosis of this injury,
with particular focus on the controversy that surrounds operative vs.
non-operative treatment.
Case Presentation
A 15-year-old male, A.T., previously in good health, presented
to an urgent care facility with a history of non-contact injury to his
right elbow suffered earlier that day. A long-time baseball player,
A.T. was throwing a pitch when he heard a loud pop immediately
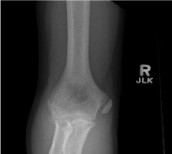
followed by intense pain. Plain anterior-posterior (AP) X-ray (Figure 1) examination of the elbow showed a complete avulsion fracture
with mild displacement of the medial epicondyle, and he was referred
for consultation with a pediatric orthopedic surgeon.
Physical examination results revealed tenderness on the medial
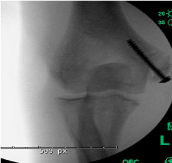
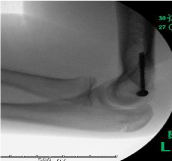
aspect of the right elbow and valgus laxity. Hoping to quickly return to
baseball, A.T. elected to undergo open reduction and internal fixation
(ORIF) of the fracture (Figures 2 and 3), which was performed 4 days
after injury.
The patient’s elbow was immobilized in a removable posterior
splint for 1 week post-operatively, after which it was removed and
converted to a sling. Early protected active range of motion exercises
were also started 1 week post-operatively. By 8 weeks A.T. had
regained full strength and range of motion in the injured elbow, see
(Figures 4 and 5), and was cleared to participate in tryouts for his fall
baseball team.
Figure 1
Figure 2
Figure 3
Figure 4
Figure 5
Discussion
The management of medial epicondyle fractures in the pediatric
population has remained controversial for some time with some
studies showing positive results for both operative and non-operative
management [4,6,10,11]. Traditionally, indications for operative
versus non-operative management are dependent upon the degree
of displacement of the fracture fragment from the fracture bed with
displacement < 5mm managed non-operatively and those 5mm-
15mm managed operatively [4,6,10,11]. The Rang Medial Epicondyle
Classification system has four categories: I minimally displaced II
rotated III trapped fragment in joint space and IV dislocated elbow
and can guide surgeons’ decision making [12].
Youth baseball pitchers are playing for larger parts of the year
now and are especially prone to developing avulsion fractures of the
medial epicondyle depending on their degree of usage [4,6,11]. In an
increasingly competitive sporting culture and with the prospect of
earning a collegiate scholarship, overhead athletes and their families,
through a shared decision making process, are considering all options
for speedy return to sports following these injuries. We assert that open
reduction and internal fixation is the optimal treatment for athletes
who desire a quick return to normal function regardless of degree of
displacement and patients and families such as AT’s are selecting it
as a treatment option. Despite the lack of high level evidence studies,
there are a few lower level studies that show there is an earlier return
to play in those athletes treated operatively [7,13]. Studies have also
shown a 9.33 odds of union for operative management as compared
to non-operative treatment [15]. Non-operative treatment such
as prolonged casting might result in stiffening of the elbow as well
as inappropriate lengthening of the ulnar collateral ligament as a
result of misalignment of the fracture fragment which can result in
increased valgus instability at the elbow [14].
Displacement as a means for determining the proper course of
management is mainly determined by the use of anterior-posterior
(AP) and lateral elbow X-rays [15]. Disagreement when measuring
fracture displacement on an X-ray was defined as a reading greater
than 2mm difference between observers [15]. Surgical team members
were shown to disagree 54%, 87% and 64% on AP, lateral and oblique
X-ray views, respectively [15]. These figures indicate an inherent
controversy especially for surgeons who prefer non-operative
treatment for less displaced fractures as the fragment might be more
displaced than originally thought. Surgeons preferring to proceed with
management based on degree of displacement will be better served by
using a 45-degree internal oblique X-ray to improve their accuracy at
judging the degree of displacement [15]. This angle has been shown to
have less disagreement amongst observers [15]. More accurate than
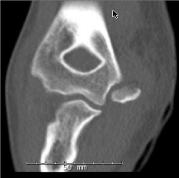
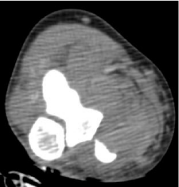
X-rays is computed tomography (CT) see (Figures 6 and 7), however,
access and cost might be a deterrent to adaptation of this modality.
A.T. regained full range of motion and strength in 8 weeks. After
surgery he was placed in a cast and then was able to complete physical
therapy to help restore his elbow function. Different types of ORIF
can assure speedy return to full range of motion such as cannulated
screw with washer fixation, also Kirschner (K-wires) wires can be
used but should be removed being 2 and 6 months after placement
[12]. A cannulated screw and washer interfragmentary compression
construct was used for A.T.
There have been some documented cases of late ulnar nerve
palsy after ORIF, however, this was absent in our patient. If a
patient initially presents with an ulnar nerve palsy noted on initial
physical examination, then ORIF is indicated. The ulnar nerve may
be damaged during the initial trauma or via iatrogenic means such
as during surgery or compressive effects of casting on the nerve
[16]. For the cases illustrated the nerve was compressed by the deep
fascia between the heads of the flexor carpi ulnaris (FCU), release of
compression was achieved by early release of the aponeurosis of the
FCU as well as the fascia between the heads of the FCU [16].
Figure 6
Figure 7
Conclusion
Throwing athletes such as baseball pitchers who play year around are often seeking to return to play quickly. Patients such as A.T. and his family opted for surgery to achieve this goal. ORIF has been proven to provide bony union at significantly higher rates and has been shown to restore range of motion more quickly and allow for speedy return. Though there is a place for non-operative management with some minimally displaced fractures, athletes faced with the decision between operative and non-operative treatment can be assured that operative management can reliably expedite return to function and sport.
References
- Beaty JH, Kasser JR. “The Elbow: Physeal Fractures, Apophyseal Injuries of the Distal Humerus, Osteonecrosis of the Trochlea, and TCondylar Fractures” in Rockwood & Wilkins’ Fractures in Children, 6th ed. Philadelphia PA: Lippincott Williams & Wilkins;2006:628–642.
- Silberstein MJ, Brodeur AE, Graviss ER, Luisiri A. Some vagaries of the medial epicondyle. J Bone Joint Surg Am. 1981; 63: 524–528.
- Ciccotti MC, Hammoud S, Dodson CC, Cohen SB, Nazarian LN, Ciccotti MG. Stress ultrasound evaluation of medial elbow instability in a cadaveric model. A J of Sports Med. 2014; 42: 2463–2469.
- Cruz AI, Steere JT, Lawrence JT. Medial Epicondyle Fractures in the Pediatric Overhead Athlete. J Ped Ortho. 2016; 36: S56-S62.
- Cain E Jr., Dugas JR, Wolf RS, Andrews JR. Elbow Injuries in Throwing Athletes: A Current Concepts Review. A J of Sports Med. 2003; 31: 621- 635.
- Osbahr DC, Chalmers PN, Frank JS, Williams RJ 3rd, Widmann RF, Green DW. Acute, avulsion fractures of the medial epicondyle while throwing in youth baseball players: A variant of the Little League elbow. J Shoulder and Elbow Surg. 2010; 19: 951-957.
- Lee HH, Chen HC, Chang JH, Lee CH, Wu SS. Operative treatment of displaced medial epicondyle fractures in children and adolescents. J Shoulder and Elbow Surg. 2005; 14: 178–185.
- Lokiec F, Velkes S, Engel J. Avulsion of the medial epicondyle of the humerus in arm wrestlers: a report of five cases and a review of the literature. Injury. 1991; 22: 69-70.
- Pathy R, Dodwell ER. Medial epicondyle fractures in children. Curr Opin Ped. 2015; 27: 58-66.
- Patel NM, Ganley TJ. Medial Epicondyle Fractures of the Humerus: How to Evaluate and When to Operate. J Ped Ortho. 2012; 32: S10-S13.
- Lawrence JT, Patel NM, Macknin J, Flynn JM, Cameron D, Wolfgruber HC. Return to Competitive Sports after Medial Epicondyle fractures in Adolescent Athletes: Results of Operative and on operative Treatment. A J of Sports Med. 2013; 41: 1152-1157.
- Mehlman CT, Howard AW. Medial Epicondyle Fractures in Children: Clinical Decision Making in the Face of Uncertainty. J Ped Ortho. 2012; 32: S135-S142.
- Case SL, Hennrikus WL. Surgical treatment of displaced medial epicondyle fractures in adolescent athletes. A J of Sports Med. 1997; 25: 682–686.
- Pace GI, Hennrikus WL. Fixation of Displaced Medial Epicondyle Fractures in Adolescents. J Ped Ortho. 2016.
- Gottschalk HP, Bastrom TP, Edmonds EW. Reliability of Internal Oblique Elbow Radiographs for Measuring Displacement of Medial Humeral Epicondyle Fractures: A Cadaveric Study. J Ped Ortho. 2013; 33: 26-31.
- Anakwe RE, Watts AC, McEachan JE. Delayed ulnar nerve palsy after open reduction and internal fixation of medial epicondylar fractures. J Ped Ortho B. 2010; 19: 239-241.
- Kamath AF, Baldwin K, Horneff J, Hosalkar HS. Operative versus non-operative management of pediatric medial epicondyle fractures a systematic review. J Child Ortho. 2009; 3: 345-357.