Case Report
Mucocele of the Sphenoid Sinus as a Rare Cause of Isolated Oculomotor Nerve Palsy: Case Report and Review of the Literature
Wenting Li, Jiancong Huang, Luoying Yang, Lihong Chang* and Gehua Zhang*
Department of Otolaryngology, Head & Neck Surgery, Sun Yat-sen University, China
*Corresponding author: Lihong Chang, Department of Otolaryngology, Head & Neck Surgery, The Third Affiliated Hospital, Sun Yatsen University, NO.600 Tianhe Road, Guangzhou, 510630, China
Published: 05 Dec, 2016
Cite this article as: Li W, Huang J, Yang L, Chang L, Zhang
G. Mucocele of the Sphenoid Sinus as
a Rare Cause of Isolated Oculomotor
Nerve Palsy: Case Report and Review
of the Literature. Clin Surg. 2016; 1:
1207.
Abstract
Mucocele of sphenoid sinus is a rare cause of oculomotor nerve palsy. A 59-year-old male presented
with a 2-week history of sudden ptosis of his right eyelid and right internal ophthalmoplegia.
Laboratory examination and radiological evaluation revealed mucocele of the right sphenoid sinus
with diabetes and chronic rhinosinusitis. The patients underwent nasal endoscopic surgery and
the right sphenoid sinus mucocele was confirmed. The patient recovered completely after 2weeks.
One year follow up indicated no recurrence. A sphenoid sinus mucocele presents various clinical
symptoms due to its relationship to the adjacent cavernous sinus and the base of skull. Involvement
of isolated oculomotor nerve palsy in sphenoid sinus mucocele is rare. The differential diagnosis
between compressive lesion caused by mucocele of sphenoid sinus and ischemic lesion caused by
diabetes should be noticed. Careful clinical evaluation and appropriate radiologic imaging can help
to identify a definitive cause. Computed tomography and magnetic resonance imaging are useful in
explaining the clinical symptoms of mucocele of sphenoid sinus by identifying the spreading of the
lesion. Proper and timely endoscopic marsupialization of the mucocele lead to complete resolution
of the oculomotor nerve palsy.
Keywords: Mucocele; Sphenoid sinus; Oculomotor nerve palsy; Ptosis
Introduction
Mucoceles are benign, encapsulated, expansile, locally invasive masses within a paranasal sinus filled with mucus and lined by epithelium. Sphenoid sinus mucocele is the most rarely afflicted sinus and comprise 1-2% of all paranasal sinusmucoceles [1]. Mucocele of the sphenoid is usually seen in fourth decade of life. Once the mucocele expand outside the bony wall, various vital complications may occur since several important structures are adjacent to it. Due to its concealing symptoms, patients usually consult opthalogist and neurologist first and easily got wrong or delayed treatment.
Case Presentation
A 59-year-old male, presented with a 2-week history of sudden complete drooping of his right
eyelid (Figure 1). His visual acuity was normal with no obviously diplopia, proptosis, facial numbness
nor headache. The patients firstly sought medical advice in neurology clinics. Examination revealed
uncontrolled hypertension and diabetes. He was initially considered as diabetes-related third nerve
palsy and given insulin therapy. However, the symptoms had no obvious relief. Cranium computed
tomography (CT) scan was then performed and images revealed soft tissue masses in nasal sinuses.
He was then referred to our clinic. Past history showed the patients had nasal surgery 10 years ago
and didn’t complain about obvious nasal obstruction and rhinorrhea.
Investigation
Physical examination revealed severe reduction of elevation, depression, and adduction in the
right eye. He had a dilated and unresponsive right pupil. The fundus examination and other eyes
was unremarkable. Nasal endoscopy showed multiple polyps derived from middle turbinate and
occupied nearly the whole nasal cavities accompanied by purulent secretion. The olfactory fissure
was also full of nasal polyps and ostium of sphenoid sinus could not be detected bilaterally (Figure
2). Cultures of nasal purulent secretion showed no growth of specific bacteria and fungus.
CT imaging of the nose and paranasal sinus revealed extensive soft tissue masses filled in all
sinuses bilaterally and an obvious expansion of right sphenoid sinus. Discontinuity of posterolateral
bony wall of the right sphenoid sinus was remarkable, while the other
part of bony wall was thickened. Magnetic resonance image (MRI)
was used to evaluate the extension of the lesion. The lesion of right
sphenoid sinus showed iso-intense in T1-weighted images and hyperintense
in T2-weighted images with a clear ring shape margin and
expand posterolaterally into the right cavernous sinus. The imaging
features suggested that the lesion was predominantly cystic (Figure
3). Normal size and shape of pituitary gland, normal optic-chiasma
and nerve complex, homogenous enhancement of cavernous were all
detected. No evidence of any aneurysm in the circle of Willis in MRA.
Treatment and outcome
The patient underwent functional endoscopic sinus surgery
bilaterally and drainage of the right sphenoid sinus under general
anesthaesia. Intraoperatively, we expanded and removed the anterior
wall of right sphenoid sinus in order to allow adequate drainage
into sphenoethomoidal recess. The secretion of the right sphenoid
sinus was serous and purulent. The posterolateral wall bone was
discontinuity but the mucus of sinus remained completed. His ptosis
was markedly reduced the following day. The patient’s symptom
completely diminished 2 weeks after surgery. The patient has been
followed in our outpatient clinic at regular intervals. On follow-up
nasal endoscopy there was a healthy mucous membrane lined cavity
widely open with no signs of recurrence nor other complication have
been found. The patient remains asymptomatic up to now (Figure 4).
Figure 1
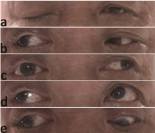
Figure 1
The patient presenting oculomotor nerve palsy of his right eye. Complete ptosis of right upper eyelid.
(a) Complete ptosis of right upper eyelid
(b) The abduction of the right eyeball was normal
(c) Adduction of the right eyeball
(d) Elevating of the right eyeball
(e) Depression of the right eyeball
Figure 2
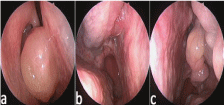
Figure 2
The nasal endoscopic investigation.
(a) Nasal polyps derived from the right middle meatus of the right nasal cavity
(b) Nasal polyps occupied the right olfactory cleft with no obvious ostium of the right sphenoid sinus
(c) Nasal polyps derived from the left middle meatus and the left middle turbinate was partially missing possibly due to past nasal surgery
Figure 3
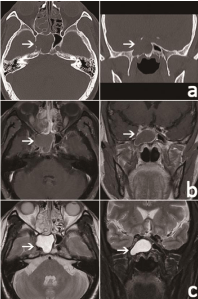
Figure 3
Horizontal and coronal plane of CT and MR images of the patient. The lesion was homogenous isointense in CT scan.
(a) The lesion was homogenous isointense in CT scan
(b) The lesion was homogenous iso-intense in T1 weighted images
(c) The lesion was hyper-intense in T2 weighted images
Figure 4
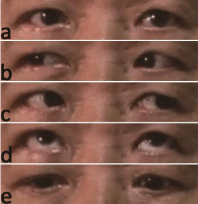
Figure 4
The patient recovered 2 weeks after surgery.
(a) His ptosis was completely resolved
(b) No limitation of abduction
(c) No limitation of adduction
(d) No limitation of elevating
(e) No limitation of depression
Table 1
Table 1
The characteristics of the past reports of sphenoid sinus mucocele presenting as the oculomotor nerve palsy.
Discussion
In adults the most common cause of acute oculomotor
mononeuropathies is diabetes-related microvascular ischemic third
nerve palsy, which is characteristic of various internal ophthalmoplegia
with papillary sparing. Pupillary sparing is believed to result from
microvascular ischemia of the central portion of the nerve with
sparing of the more peripherally placed parasympathetic fibers in
other words, the iris sphincter is usually unaffected by ischemic injury
[2]. In contrast, compressive lesions such as aneurysms or tumors
that produce third nerve palsy commonly presenting ocular motility
disturbance and iridoplegia at the same time. Sphenoid mucocele
is one of rare compressive causes of oculomotor nerve palsy, which
occur rarely and has an incidence of 1% of paranasal sinus mucocele
[3]. The importance of sphenoid sinus mucocele presenting with
isolated third nerve palsy lies in the differential diagnosis. However
the pupil-sparing cannot help to precisely distinguish these two kinds
of etiologies. The past reported frequency of pupil involvement in
several series that included up to 25 patients with diabetes-associated
oculomotor nerve palsy ranges from 14% to 32% [4]. What’s more,
other reports showed that the sphenoid sinus lesion could also
cause isolated pupil-sparing oculomotor nerve palsy, indicated
that mucocele probably cause symptoms by compressing the
microvascular supply to the nerve, resulting in ischaemia [5,6]. Thus,
careful clinical evaluation of identify a definitive cause is important
for differential diagnosis between compressive lesion caused by
mucocele of sphenoid sinus and ischemic lesion caused by diabetes,
especially for opthalogist and neurologist.
Paranasal sinus mucocele is commonly defined as the
accumulation and retention within a sinus of its mucoid secretion
and erosion of one or several of its bony walls. The mechanism in
the development of mucocele is not clear, but postulated as the
obstruction of the sinus initiates its development [1]. The secretions
accumulated within the sinus have no exit and a gradual expansion
of the cavity occurs due to the release of osterolytic prostaglandins
and mediators with bony remodeling and erosion [7]. In our case, the
ostium of right sphenoid is stenosis approached to close completely,
possibly caused by potential congenital abnormality. What’s more,
the patient suffered from chronic rhinosinusitis for decades and didn’t
receive the regular and adequate therapy. Thus the inflammation of
sinus, especially the right posterior group of nasal sinuses, would
enhance the obstruction of the right sphenoid sinus. Above all, these
would be the potential precipitating factors of sphenoid mucocele of
this patient.
The mucocele of sphenoid sinus present no symptoms in the
early stage. In the late stage, it usually has varied presentations mostly
related to the direction of extension towards neighboring structures.
Headache is the most common symptom in 70-80% patients, probably
caused by involving and irrigating the dura [1]. Expanding sphenoid
sinus mucocele may compress the optic nerve or the cavernous sinus
which carries the III, IV, V and VI nerves (oculomotor, trochlear,
trigeminal and abducent nerves), causing visual disturbance or III,
IV, V and VI nerves palsy [8-10]. Oculomotor nerve involvement was
reported to account for 70% of ocular palsies [6]. The oculomotor
nerve is affected more frequently than the trochlear and abducent
nerve but mostly accompanied with palsy of optic nerve [11]. The
sole oculomotor palsy caused by sphenoid mucocele is very rare.
In our case, it should noticed that the bony wall of right sphenoid
sinus is entirety thickening, especially the anterior bony wall.
Thus the sphenoid mucocele extended forward to the lateral and
posterior direction and invasion into cavernous sinus, which in the
end compress the oculomotor nerve and cause symptoms. Table
1 displayed the characteristic of past reports of sphenoid sinus
mucocele presenting as third nerve palsy. The patients were mostly
mid-aged and ptosis was the most frequent symptom.
A large mucocele produces a classic radiographic appearance of
an enlarged distorted sinus with a large bony defect representing a
breakthrough into the adjacent structures [6]. CT scan of nasal and
paranasal sinuseswould shows a hypo-dense cystic lesion in the
sphenoid sinus and bony erosion. In our case, CT showed extensive
soft tissue masses in all sinus and bony discontinuity of sphenoid wall,
which also indicated fungus rhinosinusitis and inverted papilloma.The
contrast medium would help to differential diagnosis. There is usually
no increase in the intrinsic density of mucocele after injection of
contrast mediumdue to its avascular mucoid content [6]. The features
canbe hypo-, iso-, or hyperintense or signal void on the MRI images,
depending on their stage of development and protein content [2]. Our
case have moderate signal intensity on T1 weighted images and a high
signal intensity on T2 weighted images, with peripheral enhancement
after administration of contrast, indicating comparatively water-ish
content which confirmed during the surgery. What’s more, it is also
necessary to exclude potential haemorrahage and cerebral aneurysm
by using MRI and MRA, which are the most common and fetal causes
for isolated oculomotor nerve palsy. Imaging is important in early
diagnosis and help identifing the characteristic of the lesion. CT and
MR imaging can supply a reliable diagnosis of mucocele of sphenoidal
sinus and give guidance to surgery.
Treatment of sphenoid mucocele is surgical. Traditionally,
the management of sphenoid mucoceles was complete removal
via transfacial or transcranial approach. However, transnasal
sphenoidotomy has largely replaced the conventional open method
with excellent results. The endoscopic transnasal sphenoidotomy with
sufficient removal of the anterior and inferior walls of the sinus is now
strongly recommended to allow adequate drainage of the sphenoid
sinus and to avoid recurrences [12]. The prognosis of oculomotor
nerve palsy is comparatively better than the optic nerve. The average
recover time is 1-4weeks (Table 1). Proper and timely endoscopic
marsupialization of the mucocele lead to complete resolution of the
oculomotor nerve palsy.
Conclusion
We reported a rare case of mucocele of sphenoid sinus as a cause of isolated oculomotor nerve palsy. The differential diagnosis between mucocele of sphenoid sinus and diabetes should be noticed by clinic surgeon. Careful clinical evaluation and appropriate radiologic imaging can help to identify a definitive cause and give guidance for surgery. CT and MRI are useful to identify the extension of the lesion. Endoscopic marsupialization of the mucocele lead to complete resolution of the oculomotor nerve palsy and needed to be performed properly and timely.
References
- Giovannetti F, Filiaci F, Ramieri V, Ungari C. Isolated sphenoid sinus mucocele: etiology and management. J Craniofac Surg. 2008; 19: 1381- 1384.
- Vaphiades MS, Roberson GH. Sphenoid sinus mucocele presenting as a third cranial nerve palsy. J Neuroophthalmol. 2005; 25: 293-294.
- Kosling S, Hintner M, Brandt S, Schulz T, Bloching M. Mucoceles of the sphenoid sinus. Eur J Radiol. 2004; 51: 1-5.
- Jacobson DM. Pupil involvement in patients with diabetes-associated oculomotor nerve palsy. Arch Ophthalmol. 1998; 116: 723-727.
- Mohebbi A, Jahandideh H, Harandi AA. Sphenoid sinus mucocele as a cause of isolated pupil-sparing oculomotor nerve palsy mimicking diabetic ophthalmoplegia. Ear Nose Throat J. 2013; 92: 563-565.
- Akan H, Cihan B, Celenk C. Sphenoid sinus mucocele causing third nerve paralysis: CT and MR findings. Dentomaxillofac Radiol. 2004; 33: 342-344.
- Lund VJ, Harvey W, Meghji S, Harris M. Prostaglandin synthesis in the pathogenesis of fronto-ethmoidal mucoceles. Acta Otolaryngol. 1988; 106: 145-151.
- Cakmak O, Shohet MR, Kern EB. Isolated sphenoid sinus lesions. Am J Rhinol. 2000; 14: 13-19.
- Tang IP, Brand Y, Prepageran N. Evaluation and treatment of isolated sphenoid sinus diseases. Curr Opin Otolaryngol Head Neck Surg. 2016; 24: 43-49.
- Wang ZM, Kanoh N, Dai CF, Kutler DI, Xu R, Chi FL, et al. Isolated sphenoid sinus disease: an analysis of 122 cases. Ann Otol Rhinol Laryngol. 2002; 111: 323-327.
- Friedmann G, Harrison S. Mucocoele of the sphenoidal sinus as a cause of recurrent oculomotor nerve palsy. J Neurol Neurosurg Psychiatry. 1970; 33: 172-179.
- Sautter NB, Citardi MJ, Perry J, Batra PS. Paranasal sinus mucoceles with skull-base and/or orbital erosion: is the endoscopic approach sufficient? Otolaryngol Head Neck Surg. 2008; 139: 570-574.
- Lee JC, Park SK, Jang DK, Han YM. Isolated Sphenoid Sinus Mucocele Presenting as Third Nerve Palsy. J Korean Neurosurg Soc. 2010; 48: 360- 362.
- Kataria R, Gupta S, Chopra S, Bagaria H, Sinha VD. Mucocele of the sphenoid sinus: A rare cause of reversible 3(rd) nerve palsy. Ann Indian Acad Neurol. 2012; 15:158-160.