Case Report
Neoplastic Degeneration of a Thyroglossal Duct Cyst: Case Report
Vincenzo Saita1, Domenico Michele Modica1,2, Nicolò Marino1, Carmela Emmanuele3 and Eugenia Allegra4*
1Azienda Ospedaliera Cannizzaro, Phonosurgery Unit, Catania, Italy
2Otorhinolaryngology Section, Department of Experimental Biomedicine and Clinical Neurosciences, (BioNeC), University of Palermo, Italy
3Azienda Ospedaliera Cannizzaro, Pathology Unit, Catania, Italy
4Otolaryngology, Department of Health Science, Magna Graecia University, Catanzaro, Italy
*Corresponding author: Eugenia Allegra, Otolaryngology,Department of Health Science, Magna Graecia University, Catanzaro, Catanzaro Viale Europa, Germaneto, 88100, Catanzaro, Italy
Published: 05 Dec, 2016
Cite this article as: Saita V, Modica D, Emmanuele C,
Allegra E. Neoplastic Degeneration of a
Thyroglossal Duct Cyst: Case Report.
Clin Surg. 2016; 1: 1205.
Abstract
The thyroglossal duct cyst is a congenital lesion of the neck, resulting from the incomplete obliteration
of the thyroglossal canal; in the embryonic period, its purpose is to facilitate the migration to the
final seat of the thyroid draft. Rarely, the retention of this cyst can cause a neoplastic degeneration.
A 33-year-old female presented to our outpatient clinic complaining of the appearance, about a
year ago, a swelling of the neck in the middle of the suprahyoid region. Clinical and medical history
characteristics were compatible with a thyroglossal duct cyst. Computed Tomography (CT) and
Magnetic Resonance Imaging (MRI) showed the presence of a thyroglossal duct cyst. The patient
was subjected to surgery according Sistrunk procedure, and the diagnosis was papillary carcinoma
based on histopathologic examination. After two years of follow-up, the patient is currently diseasefree.
This confirms the validity of the Sistrunk surgery for non-extended and well-differentiated
tumors, with no associated thyroid lesions.
Keywords: Thyroglossal duct cyst; Papillary carcinoma; Sistunk
Introduction
The thyroglossal duct cyst (TGDC), together with gill cysts, falls within scope of cervical disease
of embryonic origin. There are two theories about the pathogenesis of neoplastic degeneration: 1) the
“novo theory”, the most accepted, which argues that the tumor would originate from thyroid gland
ectopic tissue; 2) the metastatic theory, according to which the cancer arose in a cyst and represents
tissue of a primitive metastatic thyroid carcinoma [1,2]. Also as is known, inflammatory episodes
applicants help the tissue hyperplasia, which however can rarely lead to neoplastic degeneration.
Clinically it is not possible to differentiate a benign cyst from a degenerate cyst in malignancy
and the diagnosis is generally post-operative. Primary malignancy in TGDC is extremely rare and
among all cases of TGDC, carcinoma is reported only in 0.7–1% of cases [3,4]. Papillary carcinoma
(80-85 %) is the most common carcinoma reported in TGDC, followed by squamous cell carcinoma
(5-6 %) [5].
Here, we report a case of 33-year-old-female presented with a midline neck mass, which was
diagnosed and operated for TGDC. However, on final histopathology, a diagnosis of papillary
carcinoma arising in a TGDC was made.
Case Presentation
A 33-year-old female, smoker of 5 cigarettes per day, presented to our outpatient clinic
complaining of the appearance, about a year ago, a swelling of the neck in the middle of the
suprahyoid region. There was no history of pain, dysphagia, or hoarseness of voice. There was
no history of cold or hot intolerance, tremor, palpitation, diarrhea, constipation, any menstrual
irregularities’. The patient had no family history of metabolic abnormalities and no comorbidities.
She denied any radiation exposure or family history of thyroid cancer. The ear, nose and throat
examination identified a neck mass, which moved during deglutition. The swelling appeared round
with an approximate diameter of 2 cm, not skin hyperemia; not painful, superficial and deep mobile
plans, with hard-elastic consistency, no-palpable cervical lymphnodes.
The routine laboratory investigations including complete blood
count, liver function test, and kidney function test was whit in normal
limit. Determination of blood levels of the thyroid hormones showed
normal free triiodothyronine (FT3), free tetraiodothyronine (FT4),
and TSH level.
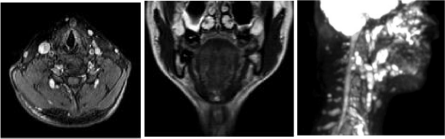
The ultrasonography (USG) of the neck to confirm the presence
of a lesion in the middle of suprahyoid region, cystic appearance,
reactive lymph nodes and normal thyroid. Computed Tomography
(CT) of the neck with contrast and Magnetic Resonance Imaging
(MRI) showed the presence of a thyroglossal duct cyst (Figure 1 and
2).
The patient was subjected to surgery according Sistrunk procedure
[6]. The resected specimen sent for histopathological examination.
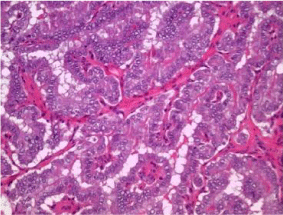
Final pathology showed a papillary thyroid carcinoma in the context
of a thyroglossal duct cyst (Figure 3). All of the margins were clear.
The patient was discharged three days after surgery. Based on the
histopathology, it was decided to perform a close follow-up (every
3 months). After two years of follow-up, the patient is currently
disease-free. Repeat USG of neck showed normal thyroid scan.
Figure 1
Figure 2
Figure 2
Histological relief: Microphotograph showing papillary projections arising from cyst wall (h and E, x 100).
Discussion
TGDCs are the most common congenital anomaly of the thyroid,
usually manifested as enlarging, painless midline neck mass. This is
the most common cause of midline neck mass in children (75%), but
this is reported only in 7% of adult population. In the majority of
the cases, TGDCs are benign [7]. However, malignancy is reported in
around 1% of cases and is usually diagnosed as an incidental finding
after histopathological evaluation of resected TGDC [8]. Thyrogenic
carcinoma is the most common malignant tumor of TGDC, which
originates from thyroglossal tract remnant followed by squamous cell
carcinoma which originates from metaplastic columnar cells of the
thyroglossal duct lining [9].
In literature, there are about 250 cases of cancer of the
thyroglossal duct cyst degeneration, variously localized on the same
route of the duct, from the cecum foramen to the intrathyroidal
level; the main location (75%) is in subhyoid, of which only six cases
are intrathyroidal, while those at the suprahyoid region, like in our
case, are a rarity [10]. The average age of diagnosis of neoplastic
degeneration of the thyroglossal duct cyst is about 50 years, with an
M/F ratio of 1/2. In a percentage from 11.4 to 33% of cases, it coexists
with cancer in the thyroid parenchyma. Histological variants of
cancer of thyroglossal duct cysts are: 80% papillary carcinoma, 8%
mixed papillary-follicular, 6% squamous cell carcinoma, and rarely
follicular forms as well, at Hurtle cell, insular or anaplastic [11].
In most cases, the presence of a swelling in the middle of the
neck is the only clinical sign, and the combination with an infectious/
inflammatory phenomenon causes skin hyperemia, spontaneous pain
or cervical lymphadenopathy triggered by palpation and consensual.
Symptomatology, both in cases of benign disease and malignant
degeneration, is similar and it depends by the size of the cyst.
Symptoms may occur with dysphagia, dysphonia, cutaneous
fistulas and rapid increase in volume.
Diagnostic methods are represented by ultrasound, computed
tomography and MRI. There are no diagnostic and therapeutic
protocols able to identify the cancer development, as in most of
the cases diagnosis is casual [12]. The therapy is surgical and the
technique for excision of the cyst is represented by Sistrunk procedure:
originally described by Charles Sistrunk, the key to the procedure and
prevention of recurrence of the cystis to resect the central portion
(body) of the hyoid bone and follow any tract up towards the base
of the tongue, the embryological site of origin of the thyroid gland
[13]. Remains debated the role of a partial or total thyroidectomy and
radioiodine therapy in the cases with suprahyoid location.
Our case report has demonstrated the validity of Sistrunk
procedure in follow-up, because we did not detect relapse.
Furthermore, Patel and colleagues have revisited 62 clinical cases of
well-differentiated thyroid cancer arising from thyroglossal duct cysts.
These authors observed that total thyroidectomy and the radioiodine
therapy did not further improve clinical outcomes [14]. Therefore,
the Sistrunk procedure may be considered valid in the presence of a
well-differentiated carcinoma confined inside of a thyroglossal duct
cyst. Vigneri and coll, after analyzing studies of the last 25 years,
have confirmed the validity of Sistrunk intervention in the cases
without associated risk factors [15]. Therefore, a conservative surgical
management is indicated in low-risk patients (female, age< 40 years,
no capsular invasion, sizes of less than 1 cm in diameter tumor), while
a more aggressive surgery is to be reserved for those patients with
thyroid lesions associated, clinically obvious or apparent at follow-up.
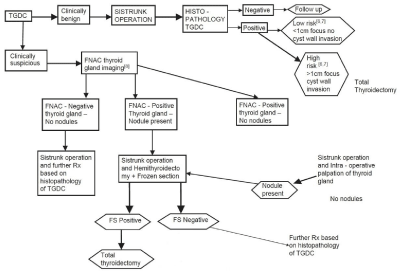
Senththil kumar et al. [16] have proposed a treatment algorithm
on the basis of the literature evidence in cases of cancer of thyroglossal
cysts, which shows several therapeutic approaches for the clinically
benign cysts with subsequent detection of malignancy on histologic
examination (Figure 4) [16]. In the most suspicious cases, we carry
out additional pre-operative investigations, such as fine needle
aspiration cytology (FNAC), without differentiating between cysts or
infrahyoid.
Finally, from a careful analysis of the literature, we found that
actually the phenomenon (cancer arising in a thyroglossal duct cyst)
may be less rare than reported in the incidence statistics published
until now: in the first 6 months of 2016 have already been published
five case reports on the topic and probably there were other
unpublished cases [17-21].
Figure 3
Conclusion
Based on our experience and in the absence of international guidelines about this disease, we believe that the Sistrunk procedure is more effective rather than others surgical interventions for primary tumors that occur in the context of thyroglossal cysts, without associated risk factors. Based on the increasing incidence of cancers arising from thyroglossal duct cyst, probably we should always take into account this possibility when it is diagnosed TGDC.
References
- Hilger AW, Thompson SD, Smallman LA, Watkinson JC. Papillary carcinoma arising in a thyroglossal duct cyst: a case report and literature review. J Laryngol Otol. 1995; 109: 1124-1127.
- Tew S, Reeve TS, Poole AG, Delbridge L. Papillary thyroid carcinoma arising in thyroglossal duct cyst incidence and management. Aust NZ J Surg. 1995; 65: 717-718.
- Heshmati HM, Fatourechi V, van Heerden JA, Hay ID, Goellner JR. Thyroglossal duct carcinoma: report of 12 cases. Mayo Clin Proc. 1997; 72: 315-319.
- Fernandez JF, Ordoñez NG, Schultz PN, Samaan NA, Hickey RC. Thyroglossal duct carcinoma. Surgery. 1991; 110: 928-934.
- Yamada S, Noguchi H, Nabeshima A, Tasaki T, Kitada S, Guo X, et al. Papillary carcinoma arising in thyroglossal duct cyst in the lateral neck. Pathol Res Pract. 2013; 209: 674-678.
- Balfour M, Al-Reefy HM, Dilkes MG. Sistrunk’s 1920 description of thyroglossal cyst excision. Grand Rounds. 2006; 6: L1–L2.
- Hassan MJ, Rana S, Khan S, Jairajpuri ZS, Monga S, Jain A, et al. An Incidental Primary Papillary Carcinoma Arising in a Thyroglossal Duct Cyst: Report of a Rare Finding. J Lab Physicians. 2016; 8: 62-64.
- Gupta N, Dass A, Bhutani M, Singhal SK, Verma H, Bhutani M, et al. Papillary carcinoma in thyroglossal duct cyst: An unusual case. Egypt J Ear Nose Throat Allied Sci. 2014; 15: 45-47.
- Peretz A, Leiberman E, Kapelushnik J, Hershkovitz E. Thyroglossal duct carcinoma in children: case presentation and review of the literature. Thyroid. 2004; 14: 777-785
- Hatada T, Ichii S, Sagayama K, Terada N, Yamamura T. Intrathyroid thyroglossal duct cyst simulating a thyroid nodule. Tumori. 2000; 86: 250- 252.
- Chu YC, Han JY, Han HS, Kim JM, Min SK, Kim YM. Primary papillary carcinoma arising in a thyroglossal duct cyst. Yonsei Med J. 2002; 43: 381- 384.
- Shemen L, Sherman CH, Yurovitsky A. Imaging characteristics and findings in thyroglossal duct cyst cancer and concurrent thyroid cancer. BMJ. 2016.
- Righini CA, Hitter A, Reyt E, Atallah I. Thyroglossal duct surgery. Sistrunk procedure. European Annals of Otholaryngology, Head and Neck Disease. 2016; 133: 133-136.
- Patel SG, Escrig M, Saha AR, Singh B, Shah JP. Management of welldifferentiated thyroid carcinoma presenting within a thyroglossal duct cyst. J Surg Oncol. 2002; 79: 134-139.
- Pellegriti G, Lumera G, Malandrino P, Latina A, Masucci R, Scollo C, et al.Thyroid Cancer in Thyroglossal Duct Cysts Requires a Specific Approach due to Its Unpredictable Extension. J Clin Endocrinol Metab. 2013; 98: 458–465.
- Senthilkumar R, Neville JF, Aravind R. Malignant thyroglossal duct cyst with synchronous occult thyroid gland papillary carcinoma. Indian J Endocrinol Metab. 2013; 17: 936–938.
- Proia G, Bianciardi Valassina MF, Palmieri G, Zama M. Papillary carcinoma on a thyroglossal duct cyst: diagnostic problems and therapeutic dilemma. A case report. Acta Otorhinolaryngol Ital. 2014; 34: 215-217.
- Song-I Y, Kwang-Kuk P, Jeung-Hoon K. Papillary carcinoma arising from thyroglossal duct cyst with thyroid and lateral neck metastasis. Int J Surg Case Rep. 2013; 4: 704–707.
- Cheon NJ, Lee YM, Lee JH, Han JK, Lee JH. Papillary Carcinoma within a Thyroglossal Duct Cyst in a 17-Year-Old Child. J Craniofac Surg. 2016; 27: e282-e283.
- Patel NS, Sheykholeslami K. Papillary carcinoma in thyroglossal duct cyst: Two case reports and review of the literature. Ear Nose Throat J. 2016; 95: E36-E38.
- Hassan MJ, Rana S, Khan S, Jairajpuri ZS, Monga S. An Incidental Primary Papillary Carcinoma Arising in a Thyroglossal Duct Cyst: Report of a Rare Finding. J Lab Physicians. 2016; 8: 62-64.