Case Report
An Asymptomatic Esophageal Duplication Cyst
Chandramohan SM1, Nagarajan N1, Vaithiswaran V2 and Jayanthi V2*
1Department of Gastroenterology, Global Health City, India
2Department of Gastroenterology, Rajiv Gandhi Government General Hospital Chennai, India
*Corresponding author: Jayanthi V, Department of Gastroenterology, Institute of Surgical Gastroenterology and Thoracic Surgery, Rajiv Gandhi Government General Hospital Chennai, India
Published: 05 Dec, 2016
Cite this article as: Chandramohan SM, Nagarajan
N, Vaithiswaran V, Jayanthi V. An
Asymptomatic Esophageal Duplication
Cyst. Clin Surg. 2016; 1: 1200.
Abstract
We report a case of a mediastinal mass detected incidentally during evaluation of a patient with
fever of unknown origin. Upper endoscopy showed a smooth indentation in middle and lower third
of esophagus. Surgical excision of the mass confirmed an esophageal duplication cyst.
Keywords: Duplication cyst; Esophagus; Mediastinal mass
Introduction
Duplication cyst of the gastrointestinal tract is rare, rarely symptomatic and often reported in young adults. These cysts can arise from foregut, small and large intestine. We report a case of an incidental asymptomatic esophageal duplication cyst which was removed through a transthoracic approach.
Case Presentation
A 39 year old male, was undergoing investigation for pyrexia of unknown origin. Chest x ray
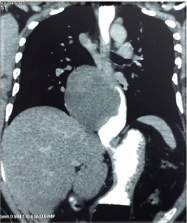
showed mediastinal widening. Computed tomography of the chest showed a large mass 10 x 6 x
5 cm posterior mediastinum indenting the lower and middle third of esophagus and contiguous
with distal third (Figure 1 and 2). There was no internal enhancement or invasion of surrounding
structures.
On retrospective questioning, patient had no intra luminal symptoms to suggest a mechanical
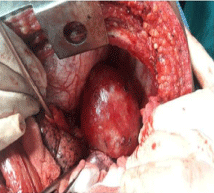
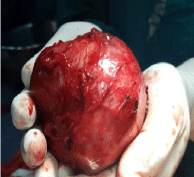
dysphagia. Upper endoscopy confirmed an extrinsic compression at the same site. Patient underwent
transthoracic resection of the mass which was in the plane of submucosa and muscular wall of the
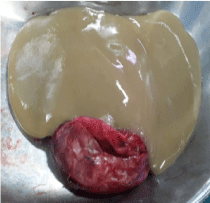
esophagus and none communicating with the lumen (Figure 3). The excised mass was filled with
mucinous material (Figure 4) and histology showed typical lining by squamous epithelium with wall
of the cyst containing components of both submucosa and muscular layer. Patient was started on
clear fluid on day 2. Recovery was uneventful.
Figure 1
Figure 2
Figure 3
Figure 4
Discussion
Duplication cyst of the esophagus was described by Blasius in 1711 and was further classified as
simple epithelial – lined cysts and esophageal duplication cyst. They are benign mediastinal mass.
Embryologically, there is a defective development of the primitive foregut.
Typically, an esophageal duplication cyst has duplication of
portions of mucosa and submucosa; epithelium remains none
duplicated while a simple esophageal cyst have duplication of the
epithelium. Either cyst does not communicate with the esophageal
lumen. These cysts can occur in the neck, mediastinum or abdomen
[1-2].
The most common location of esophageal duplication cyst is right
posteroinferior mediastinum and this was also the location of cyst in
our patient. While large cysts are often symptomatic, smaller cysts are
incidental findings and are asymptomatic as was seen in our patient.
Further, symptoms are common in children and seldom manifest in
adulthood.
Dysphagia is the most common symptom (60%) and is due
to extrinsic compression of the esophagus. Cysts in upper third
of the esophagus manifests with respiratory symptoms due to
compression of trachea bronchial tree, while middle third lesions
present (20%) with dysphagia and chest pain radiating to the back.
Rare presentations include cardiac dyssrhythmia by cysts located
posteriorly in lower third of the esophagus, gastrointestinal bleed if
the lining epithelium has gastric mucosa and very rarely malignant
transformation of the cyst.
Differential diagnosis includes congenital cysts pericardial cyst,
neuroenteric cyst, lymphangioma, cyst arising from thyroid and
thymus, and transthoracic extension of pseudocyst of pancreas.
Diagnosis is confirmed by computed tomography of chest. The
lesion is seen as a fluid filled cyst in relation to the esophagus. Magnetic
resonance imaging is complementary. Chest X-ray shows widening
of the mediastinum. Endoscopy shows extrinsic compression of the
esophagus and is indicated for ruling out malignancy. Endoultrasound
will provide information on the contents and origin and extent of the
cyst [3].
Treatment of esophageal duplication cyst is surgical resection
as majority of the cysts eventually become symptomatic. Options
include transthoracic approach, minimal invasive procedure,
endoscopic approach [4] and robotic assisted thoracic surgery [5-6].
Intra-abdominal cyst can be excised laparoscopically.
Our patient had cyst excision through transthoracic approach.
The muscle layers were reapproximated after excision to prevent
formation of pseudodiverticulum.
References
- Harvell JD, Macho JR, Klein HZ. Isolated intra-abdominal esophageal cyst. Case report and review of the literature. Am J Surg Pathol. 1996; 20: 476- 479.
- Castelijns PS, Woensdregt K, Hoevenaars B, Nieuwenhuijzen GA. Intraabdominal esophageal duplication cyst: A case report and review of the literature. World J Gastrointest Surg. 2014; 6: 112-116.
- Chaudhary V, Rana SS, Sharma V, Sharma AR, Nada R, Gupta R, et al. Esophageal Duplication Cyst in an Adult Masquerading as Submucosal Tumor. Endosc Ultrasound. 2013; 2: 165–167.
- Martin JT, Cibull ML, Zwischenberger JB, Reda HK. Infection of an esophageal cyst following endoscopic fine-needle aspiration. Int J Surg Case Rep. 2011; 2: 144-146.
- Fernando HC, Erdem CC, Daly B, Shemin RJ. Robotic assisted thoracic surgery for resection of an esophageal cyst. Dis Esophagus. 2006; 19: 509- 511.
- Obasi PC, Hebra A, Varela JC. Excision of esophageal duplication cysts with robotic-assisted thoracoscopic surgery. JSLS. 2011; 15: 244-247.