Research Article
Speech Outcomes after Tonsillectomy (For Tonsillitis) in Patients with Submucous Cleft Palate
Sherif M. Askar1*, Hazem S. Amer1, Amal S. Quriba2, Mostafa H. Hassaan1, Ahmad M. Anany1 and Ashraf Al- Malt1
1Department of Otorhinolaryngology, Head and Neck Surgery, Zagazig University, Egypt
2Department of Otorhinolaryngology, Head and Neck Surgery, phoniatric unit, Zagazig University, Egypt
*Corresponding author: Sherif Mohammad Askar, Department of Otorhinolaryngology, Head and Neck Surgery, Zagazig University, Egypt
Published: 08 Nov, 2016
Cite this article as: Askar SM, Amer HS, Quriba AS,
Hassaan MH, Anany AM, Al- Malt A.
Speech Outcomes after Tonsillectomy
(For Tonsillitis) in Patients with
Submucous Cleft Palate. Clin Surg.
2016; 1: 1174.
Abstract
Objectives: Otolaryngologists often face a problem when they have a patient with inflammatory indications for tonsillectomy particularly in developing countries where infection is endemic and its
complications are dangerous. This work aims at presenting our experience in tonsillectomy (due to
inflammatory indications) in patients with submucous cleft palate and to assess its effects on speech.
Materials and Methods: Thirteen patients with submucous cleft palate complaining of inflammatory
indications for tonsillectomy were subjected to the protocol of speech assessment including videonasopharyngoscopy
and nasometric assessment.
Results: Comparison between preoperative and postoperative results of speech assessment,
endoscopic velopharyngeal closure as well as nasometric assessment all revealed non-significant
differences.
Conclusion: Tonsillectomy due to inflammatory indications could be performed in patients with
SCP, and gives no or little effects on the performance of velopharyngeal sphincter.
Keywords: Speech; Tonsillectomy; Submucous cleft palate
Introduction
The otolaryngologist often faces a decision-making problem when he has a patient with
submucous cleft palate (SCP) who has an indication to undergo tonsillectomy. Surgeons are often
reluctant to operate in the oropharynx to avoid hazardous effects on the velopharyngeal sphincter
(VPS) and speech difficulties, but the situation differs when surgical intervention is strongly
indicated. Controversy often exists over whether tonsillectomy will affect speech in patients with
known velopharyngeal insufficiency (VPI), particularly in those with SCP [1,2]. Recent studies have
challenged the old assumption that tonsillectomy is contraindicated in patients with or at risk for
VPI [1,3,4].
For a long time infection had been the most common indication for tonsillectomy up until the
1980s; however recently, obstruction is now more commonly reported as a primary indication [5].
Researchers mainly described tonsillectomy in cases of sleep disturbance or obstructive sleep apnea
while inflammatory indications were not widely discussed [1,3,4]. This may be the situation in the
western developed communities, but in the less developed countries (where infection is endemic)
inflammatory indications might still lead the indications [5,6].
This work aims at presenting our experience in tonsillectomy (due to inflammatory indications)
in patients with SCP and to assess its effects on speech.
Patients and Methods
This prospective study was carried out on patients with SCP who were referred to pediatrics
unit, ORL-HN Department, Zagazig university hospitals in the period between January 2010 and
June 2015. Patients were referred to our unit complaining of different forms of inflammatory
tonsillitis (Table 1). Patients with high grades of hypertrophied adenoidal tissues (Grade 3-4) and/
or sleep-disordered breathing were excluded from the study. Other exclusion criteria included
syndromic cleft palate and neurologic-mental disorders. Patients who did not attend regular follow
up sessions of speech assessment were also excluded from the study. The study was approved by the
International Review Board of our institution.
Thorough history taking was the first step stressing upon details
of recurrent attacks of tonsillitis (for each attack as regard its period,
presence of fever, effects on performance and school absence, needs
of antibiotics, etc…), mouth breathing and bad breath. Personal or
family history of rheumatic fever was a point of detailed discussion.
Complete general and head and neck examination was the following
step, and Antistreptolysin O titer [ASOT] was requested for all of
them. Then, patients were subjected to speech assessment in the
Phoniatric unit of our department; all patients were assessed blindly
by 3 Phoniatricians.
Patients’ and parents’ interview and detailed history were
obtained. Then auditory perceptual assessment (APA) of the patient’s
speech was done: The subjective evaluation of patients’ speech in a
free conversation included type (hyponasality or hypernasality)
and degree of nasality, consonant precision, the compensatory
articulatory mechanisms (glottal and pharyngeal articulation), facial
grimace, audible nasal emission of air, and the overall intelligibility of
speech. All these elements are graded along a 5-point scale in which
0=normal and 4=severe affection.
Video-nasoendoscopy (VNE) was performed for all patients
using a flexible fiberoptic nasopharyngeal endoscope from (Xion
medicals) Figure 1(a-c-d); and Figure 2(a-d). The velopharyngeal
valve movement was recorded while the patient was repeating the
speech samples following recommendation given by an International
Working Group [16]. The movement of the velum and lateral
pharyngeal walls was traced on the monitor and given a score from 0
to 4 as follows: (0=the resting (breathing) position or no movement;
2=half the distance to the corresponding wall; 4=the maximum
movement reaching and touching the opposite wall). Pattern of
closure of the VPI was specified whether circular, coronal, sagittal,
or other.
Nasometer II 6400 from (Kay Pentax Corporation, Montvale,
NJ. USA) was used for the analysis of speech samples of all patients.
The Picture-Cued Subtest from the Egyptian SNAP test was applied
to assess nasometric changes. All subjects were asked to read or repeat
six sentences separately containing the following phonemes (bilabial
plosives, lingual-alveolar plosives, velar plosives, velar fricatives,
sibilant fricatives and nasals), guided with their corresponding
pictures [7].
A written informative consent was obtained from each patient
after clarification of the procedure in details to patients and/or
parents. Tonsillectomy was performed (after routine preoperative
laboratory and radiological evaluations). Patients were sent to the
Phoniatrics unit after 1 month of surgery (after the complete healing).
The VPS function and speech were assessed on regular sessions
(every 4-6 months) till the end of the follow up period. The
study focused on the Phoniatrics results after tonsillectomy (for
inflammatory indications) in patients with SCP.
The data were collected; tabulated and analyzed using SPSS
statistical package Version 20 for windows. Comparison between
preoperative and postoperative speech evaluations was done.
Qualitative data were presented as numbers and corresponding
percentages. Non parametric tests were used when appropriate
(Wilcoxon matched pairs test for quantitative data; and chi square test
for qualitative data). P< 0.05 is considered significant and P< 0.001 is
considered highly significant. A literature review was performed, to compare results with other reports.
Table 1
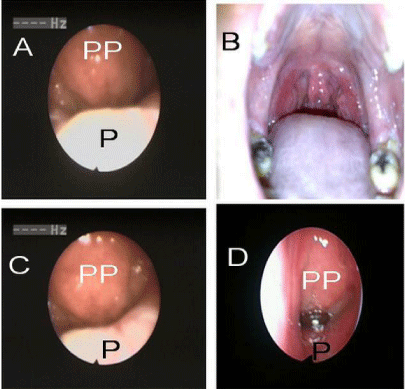
Figure 1
Figure 1
A: preoperative nasoendoscopy
B: oral view; notice the bifid uvula and the blue line
C, D: postoperative nasoendoscopy.
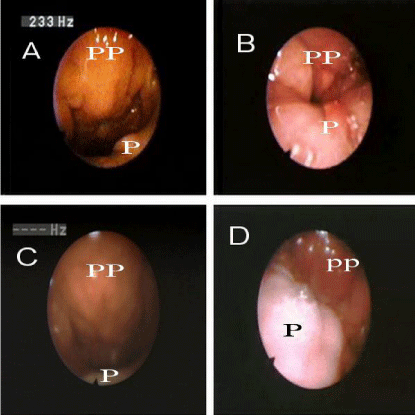
Figure 2
Figure 2
A: preoperative nasoendoscopy in resting position
B: preoperative nasoendoscopy in action
C: postoperative nasoendoscopy in resting position
D: postoperative nasoendoscopy in action.
Table 2
Table 2
Comparison between preoperative and early (1 month) postoperative assessment of speech (n = 13).
Results
General characteristics
A total of 21 patients with SCP underwent tonsillectomy for
inflammatory indications over the time period. Of these, 8 patients
were excluded and 13 patients were enrolled in the study. The
excluded eight patients included two patients with high grades of
hypertrophied adenoidal tissues and sleep-disordered breathing; two
patients with syndromic cleft palate; and one patient with neurologicmental
disorders. Patients who did not attend scheduled follow up
sessions of speech assessment were also excluded from the study (3
patients).
The studied patients (13) were six males (46.2%) and seven
females (53.8%) and their age ranged from 5 to 19 years (mean=8
years and 6 months). Bifid uvula was seen preoperatively in all cases
but zona pellucida and notching of hard palate were identified in 10
patients. Transnasal nasopharyngoscopy revealed loss of the midline
convexity of the nasal surface of the soft palate with flattening (8
patients) and a clear midline groove (5 patients).
Six patients presented with seven or more attacks of acute
bacterial tonsillitis (documented by a physician) per year for two
years or more that was associated with fever and absence from
school. Four patients presented with chronic tonsillitis, associated
with chronic cervical lymphadenitis. One patient had two attacks
of left peritonsillar abscess, documented with drainage of pus. High
ASOT was obtained from the eleven patients, and was reported to be
1300 IU/mL in recurrent tonsillitis; 975 IU/mL in chronic tonsillitis;
and 660 IU/mL in peritonsillar abscess. Two patients had a chief
complaint of halitosis, with wide tonsillar crypts and their ASOT
was 530 and 570 IU/mL. Recovery period passed smoothly with no
reports of postoperative complications. The follow up was extended
to 15-18 months after surgery.
Speech assessment
Pre-operative assessment speech: Assessment of APA of patients
revealed that among 13 patients, 5 patients (38%) had hypernasality
and 2 (18%) had hyponasality. Audible nasal air emission was
detected in 3 patients (23%). Compensatory mechanisms were
detected in 4 patients (31%) in the form of pharyngealized fricatives
and facial grimace. Speech intelligibility was affected mildly in 4
patients (31%). Endoscopic velopharyngeal closure revealed that 5
(38%) had incompetent closure (Tables 2,3).
Early (1 month) postoperative assessment: Assessment of APA
revealed the presence of 7 patients (54%) with hypernasal speech and
1 (8%) with hyponasal speech. 5 patients (38%) had nasal emission
of air. 4 patients (31%) suffered imprecision of consonant. While
5(38%) had un-intelligible speech. Endoscopic velopharyngeal
closure revealed that 6 (46%) had incompetent closure (Tables 2,3).
Late postoperative speech (at the end of the follow up):
Postoperative APA of patients’ speech revealed that among 13 patients
of the study 6 patients (46%) suffered hypernasality and 1 patient
(8%) suffered hyponasality, the same as preoperative assessment.
Among participants of the study there were 4 patients (31%) suffered
postoperative audible nasal air emission Imprecision of consonants
and compensatory speech mechanisms were detected in 5 patients
(38%) with different grades of severity. While 5(38%) had unintelligible
speech. Endoscopic velopharyngeal closure revealed that
6(46%) had incompetent closure (Table 3).
Statistical comparisons: Comparisons between preoperative
results once with early postoperative and then with late postoperative
results revealed non-significant difference. Comparisons between
Endoscopic velopharyngeal assessments also revealed non-significant
differences (Tables 2,3). Also comparisons between preoperative
and postoperative nasometric results revealed that there was nonsignificant
difference for all sentence of the subtest (Tables 2,3).
Table 3
Discussion
The role of tonsils on velum position and function is poorly
characterized. The velum position during speech depends on the
complex balance of vector forces created by palatal elevators,
depressors, and constrictors [8]. Elevation is primarily achieved by
the levator veli palatini, and transverse closure is mediated primarily
by the superior constrictor. The palatopharyngeal and palatoglossal
muscles, between which the palatine tonsils reside, serve to depress
the palate. The position of these arches can vary based on the size and
shape of the tonsils, and, theoretically, the forces exerted on the palate
may be affected [1]. A SCP indicates a muscular dehiscence in the soft
palate despite an overlying intact mucosal envelope, and can often
go undetected. Bifid uvula, zona pellucida and notching of the hard
palate are the usual triad. On transnasal nasopharyngoscopy there is
loss of the usual midline convexity of the superior surface of the soft
palate, with either flattening or a midline groove, consistent with the
absence of muscular is uvulae. Different grades of dehiscence were
mentioned [9].
Although several studies have reported change in voice and
speech after removal of palatine tonsils, the effects of tonsillectomy
on speech remain unclear [10,11]. Moreover many theories and
practices exist, but the effect of tonsillectomy in patients with VPI is
largely unknown, yet there remains hesitancy among few surgeons
to perform tonsillectomy in these patients [1,12]. Cosman and
Falk, 1975 [13] mentioned that few cases of VPI may be expected to
worsen with tonsillectomy, as the tonsils are thought to act as lateral
obturators. In these cases tonsillectomy would not be recommended
or may necessitate simultaneous or staged flap augmentation. They
stated that careful endoscopy should be done for proper identification
of these cases. In the recent time, this assumption could be considered
historical, and recent data have challenged the old notion that
tonsillectomy is contraindicated in patients with or at risk for VPI
[25]. Moreover, Paulson et al., [1] 2012 argued that tonsillectomy
may play a role in improving VPI in such cases.
In our study, (VNE) was performed for all patients and
represented an important item in the pre and postoperative sessions.
Its significance in diagnosing, documenting and follow up of patients
with speech concerns was mentioned [15-16]. VNE demonstrated no
or minimal change as regard VPS closure patterns, VP gap and other
VP functions. This was evident from the non significant difference in
the comparison between preoperative and postoperative endoscopic
assessments.
Given the potential long-term sequelae of untreated chronic
tonsillitis and/ or recurrent acute tonsillitis, especially in endemic
areas tonsillectomy may be unavoidable, even in cases with
dysfunction of the palate. Moreover some patients with weak palate
might develop VPI later on in middle or late adolescence due to
changes of cephalometric parameters; hence surgeries to correct VPI
could probably not be avoided [12-16].
Although acute rheumatic fever (ARF) is relatively rare in
developed economies, it is much more common in the developing
world and among aboriginal populations [17]. The prevalence of
rheumatic heart disease (RHD) was reported to be 5.1 per 1000 in
school children in Egypt [18]. In addition, the course of ARF was
found to be severe and aggressive in different parts of the country
where rheumatic fever is still one of Egypt’s major public health
problems [18-20]. Laboratory tests including ASOT play an important
role in confirming a diagnosis and in the follow-up of rheumatic
diseases in the pediatric age group [21]. In a recent study, the upper
limit of normal (ULN) values of ASOT in normal Egyptian children
is quite high, reaching up to 400 IU/mL. This value differs in different
countries, but does not exceed 340 IU/mL (18). ASOT values of our
patients met with the Egyptian criteria.
The American Academy of Otolaryngology-Head and Neck
Surgery offers guidelines of 3 or more infections of tonsils per
year despite adequate medical therapy; the Scottish Intercollegiate
Tonsillectomy Guidelines Network recommends 5 or more episodes
per year of tonsillitis with disabling symptoms and lasting for
longer than I year [24,25]. In this work, patients had seven or more
documented attacks of acute tonsillitis for 2 years or more.
Gysin, 2013 [22] stated that peritonsillar abscess tends to be an
indication for (and treated with) tonsillectomy; in this work, we
reported one patient with a documented history of two attacks of
homolateral quinsy.
In the present study (at the end of follow up period) patients with
SCP who underwent tonsillectomy had very little overall change in
speech parameters which was evident in all comparisons between
preoperative and late postoperative APA of speech: Type of nasality,
audible nasal air emission, Imprecision of consonants, compensatory
speech mechanisms and intelligibility of speech. Among thirteen
patients with SMC, there were 5(38%) presented with preoperative
mild to moderate VPI according to VNE assessment. This number
increased postoperatively to become 6(46%). This change showed
non-significant statistical difference. Moreover there were nonsignificant
differences between preoperative and post operative
nasometric assessment. The Picture-Cued Subtest from the Egyptian
SNAP test was applied to assess nasometric changes due to its
suitability for the age range of this study, variability of speech tasks
that assess different phonemes and availability of normal results.
Abou-Elsaad et al., [7] 2012 studied 92 Egyptian Arabic speakers
and mentioned standardization of nasometry among Egyptians.
Non-significant differences in nasometric assessment confirmed the
results of other lines of speech assessment, as it is an objective test
giving automatically tested nasalance score which do not depend on
examiner’s opinion. This means that non complicated tonsillectomy
has no or minimal effect on speech and velopharyngeal functions
even in patients with risk of VPI.
Our speech findings are consistent with several studies. D’Antonio
et al. [23] in 1996 demonstrated improved or unchanged speech
parameters in 15 patients at risk for VPI after tonsillectomy. Similar
results have been demonstrated in other researches. In a recent study,
Paulson et al., [1] 2012 demonstrated improved or unchanged speech
parameters in 23 patients at risk for VPI after tonsillectomy. Also, a
Taiwanese study by Hu et al. [11] comparing management of VPI
in the presence of tonsillar hypertrophy, a subset of patients who
underwent an isolated tonsillectomy had similar speech outcomes to
our study. In their study, 19 of the patients underwent tonsillectomy;
14 patients had no change in function, three patients improved, and
two patients worsened after tonsillectomy.
The results of this study can conclude that tonsillectomy (due to
inflammatory indications) could be done in patients with SCP, and
gives no or little effect on the VPS.
It should be mentioned that the reported few cases of posttonsillectomy
VPI (including our cases) might release the question
whether this incident occurred as a natural pathway of the weak
palate or as a result from surgery. In other words, could VPI (in this
incident) have happened whether surgical procedure was performed
or not.
At the end of this work, the authors might recommend
tonsillectomy (if indicated) in patients with SCP, after good
preoperative preparation including nasoendoscopy and speech
evaluation.
Conclusion
The results of this work can conclude that tonsillectomy due to inflammatory indications could be performed in patients with SCP, and gives no or little effects on the VPS and its function. Preoperative adequate clinical assessment including proper speech evaluation and video-nasoendoscopy plays an important role and can help to anticipate postoperative outcomes particularly in cases of SCP. Further studies are still needed to elucidate the impact of tonsillectomy on patients with or at risk for velopharyngeal insufficiency, particularly given the high prevalence of streptococcal infection in our population.
References
- Paulson LM, MacArthur CJ, Beaulieu KB, Brockman JH, Milczuk HA. Speech outcomes after tonsillectomy in patients with known velopharyngeal insufficiency. Int J Otolaryngol. 2012; 2012: 912767.
- Haapanen ML, Gnatius JI, Rihkanen H, Ertama L. Velopharyngeal insufficiency following palatine tonsillectomy. Eur Arch Otorhinolaryngol. 1994; 251: 186-189.
- Muntz H, Wilson M, Park A, Smith M, Grimmer JF. Sleep disordered breathing and obstructive sleep apnea in the cleft population. Laryngoscope. 2008; 118: 348-353.
- Robison JG, Otteson TD. Increased prevalence of obstructive sleep apnea in patients with cleft palate. Arch Otolaryngol. 2011; 137: 269-274.
- Ahmed AO, Aliyu I, Kolo ES. Indications for tonsillectomy and adenoidectomy: Our experience. Niger J Clin Pract. 2014; 17: 90-94.
- Adoga AA, Okeke. Hemostasis during cold dissection tonsillectomy: Comparing the use of adrenaline and normal saline. J Clin Med Res. 2011; 3: 105‑108.
- Abou-Elsaad T, Quriba A, Baz H, Elkassaby R. Standardization of nasometry for normal egyptian arabic speakers. Folia Phoniatr Logop. 2012; 64: 271-277.
- Kuehn DP, Folkins JW, Cutting CB. Relationships between muscle activity and velar position. Cleft Palate J. 1982; 19: 25-35.
- Reiter R, Brosch S, Wefel H, Schlömer G, Haase S. The submucous cleft palate: Diagnosis and therapy. Int J Pediatr Otorhinolaryngol. 2011; 75: 85-88.
- Svancara P, Hora´cek J, Vokra´l J, Cerný L. Computational modelling of effect of tonsillectomy on voice production. Logoped Phoniatr Vocol. 2006; 31: 117-125.
- Hu TL, Yun C, Wang R, Chen PK, Lo LJ. Management of velopharyngeal insufficiency in the presence of enlarged tonsils: comparing a one-stage versus two-stage treatment result. J Plast Reconstr Aesthet Surg. 2008; 61: 883-888.
- Salami A, Jankowska B, Dellepiane M, Crippa B, Mora R. The impact of tonsillectomy with or without adenoidectomy on speech and voice. Int J Pediatr Otorhinolaryngol. 2008; 72: 1377-1384.
- Cosman B, Falk AS. Pharyngeal flap augmentation. Plast Reconstr Surgery. 1975; 55: 149-155.
- Tweedie DJ, Skilbeck CJ, Wyatt ME, Cochrane LA. Partial adenoidectomy by suction diathermy in children with cleft palate to avoid velopharyngeal insufficiency. Int J Pediatr Otorhinolaryngol. 2009; 73: 1594-1597.
- Askar SM, Quriba AS. Powered instrumentation for transnasal endoscopic partial adenoidectomy in children with submucosal cleft palate. Int J Pediatr Otorhinolaryngol. 2014; 78: 317-322.
- Askar SM, Abou-El Saad TS. A speech nasoendoscopy-based surgeon’s decision for correction of velopharyngeal insufficiency following adenotonsillectomy. Eur Arch Otorhinolaryngol. 2014; 271: 391-398.
- Madden S, Kelly L. Update on acute rheumatic fever. It still exists in remote communities. Can Fam Physician. 2009; 55: 475-478.
- Abdel-Moula AM, Sherif AA, Sallam SA, Mandil AM, Kassem AS, Zaher SR. Prevalence of rheumatic heart disease among school children in Alexandria, Egypt: a prospective epidemiological study. J Egypt Public Health Assoc. 1998; 73: 233- 254.
- Kassem AS, Madkour AA, Massoud BZ, Zaher SR. Benzathine Penicillin G for Rheumatic Fever Prophylaxis: 2-Weekly versus 4-Weekly Regimens. Indian J Pediatr. 1992; 59: 741-748.
- Kotby AA, Habeeb NM, Ezz El Elarab S. Antistreptolysin O titer in health and disease: levels and significance. Pediatr Rep. 2012; 4: e8.
- Breda L, Nozzi M, De Sanctis S, Chiarelli F. Laboratory tests in the diagnosis and follow-up of pediatric rheumatic diseases: an update. Semin Arthritis Rheum. 2010; 40: 53-72.
- Gysin C. Indications of pediatric tonsillectomy. ORL J Otorhinolaryngol Relat Spec. 2013; 75: 193-202.
- D’Antonio LL, Snyder LS, Samadani S. Tonsillectomy in children with or at risk for velopharyngeal insufficiency: effects on speech. Otolaryngol Head Neck Surg. 1996; 115: 319-323.
- Baugh RF, Archer SM, Mitchell RB, Rosenfeld RM, Amin R, Burns JJ, et al. Clinical Practice Guideline: Tonsillectomy in Children. Otolaryngol Head Neck Surg. 2011; 144: 1-30.
- Munir N, Clarke R. Indications for tonsillectomy: the evidence base and current UK practice, Review. Br J Hosp Med. 2009; 70: 344-347.