Research Article
A Successful Nine-Step Concept to Reduce the Risk of Perineal Infections after Abdominoperineal Resection of the Rectum
Wennström B1,2*, Henriksson G2, Johansen L2, Hassel K2 and Skullman S2
1Department of Anaesthesia, Skaraborg Hospital, Sweden
2Department of Surgery, Skaraborg Hospital, Sweden
*Corresponding author: Berith Wennström, Department of Anaesthesia and Surgery, Skaraborg Hospital, Skövde, Sweden
Published: 02 Nov, 2016
Cite this article as: Wennström B, Henriksson G, Johansen
L, Hassel K, Skullman S. A Successful
Nine-Step Concept to Reduce the
Risk of Perineal Infections after
Abdominoperineal Resection of the
Rectum. Clin Surg. 2016; 1: 1172.
Abstract
Objectives: Infections and wound healing problems after abdominoperineal resection of the
rectum (APR) are common. In 2013, a retrospective review of consecutive APRs in 2010-2012 was
performed at Skaraborg Hospital, Skövde, Sweden. The review showed that 66 % (27 out of 41)
of the patients, who were operated on in the prone jack-knife position, had a perineal infection
and wound healing problems. Because of these alarming results, we scrutinized every step of the
perioperative care process and created a nine-step concept. The aim of this study was to determine
whether the introduction of this intervention had resulted in a decrease in postoperative perineal
infections and the length of perineal wound healing in patients undergoing APR.
Materials and Methods: prospective study during 2013-2014 included 41 consecutive patients who had
undergone APR. The diagnoses were rectal cancer (n=36), Crohn’s disease (n=2), ulcerative colitis
(n=2), and familiar polyposis (n=1). A comparison was made with the consecutive historical
controls from 2010-2012. Time to wound healing was recorded and the severity of the infection was
classified according to a modified Clavien Classification of Surgical Complications. Clinical data
were collected from the Swedish ColoRectal Cancer Registry.
Results: After the introduction of the nine-step concept the infection rate was reduced from 66 %
to 10 % (p< 0.001).
Conclusion: The nine-step concept significantly reduced the perineal infections after APR. Fewer
infections mean less suffering for the patient and substantially reduced use of health care resources.
Keywords: Perineal infections; Abdominoperineal; Anaesthesia
Introduction
Abdominoperineal (APR) resection of the rectum is frequently associated with perineal wound
healing problems and infections, especially after neoadjuvant radio chemotherapy, where wound
problems have been reported in up to 50% of patients [1,2]. Postoperative complications may delay
the initiation of postoperative chemotherapy [3]. In addition to the direct suffering of the affected
patients, the cost implications for the health care system are substantial, as patients with perineal
infections require prolonged hospital stays, hospital readmissions, home-nursing wound care after
discharge and multiple outpatient visits [4]. Delayed perineal wound healing may also involve a risk
of persistent symptoms such as pain, paraesthesia, sitting disability, tension, tingling and cramps
[5].
To perform the perineal part of the procedure in the jack-knife position (JKP) has gradually
become the standard approach in Sweden. At Skaraborg Hospital, Skövde, we introduced the
JKP in 2010. After this change we noticed an increased rate of perineal infections. To identify the
true incidence of infections and wound healing problems, a retrospective review was performed
using consecutive data from 82 medical records from 2007-2012, including 41 patients operated
in the lithotomy position (2007-2009), versus 41 patients in the JKP (2010-2012). Wound healing
took significantly longer and infections were more common in patients operated in the JKP, 66%,
compared with the earlier lithotomy position, with 28% (p< 0.001). These results have been presented,
in part, at the National Swedish Congress for Surgeons, 2013. Thus, perineal complications after
APR are a clinical problem, regardless of patient positioning [2,6].
Ten of the patients in the retrospective review who had
postoperative infections were interviewed. They described a
substantial impact on quality of life, with problems of pain, leakage,
abscesses, smell, social isolation and loss of integrity, and extended
periods of hospitalization [7].
Following these alarming data, we scrutinized each step of the
perioperative care process, and a new nine-step concept was created
in order to improve the situation for these patients.
The aim of this study was to explore whether the new concept
would decrease the incidence of postoperative perineal infections in
patients undergoing APR.
Methods
As a quality improvement project, a prospective study was
performed during 2013-2014, including 41 consecutive patients
who underwent APR in the prone position (JKP) and were treated
according to the new nine-step concept. This prospective group was
compared, with regard to postoperative perineal infection, with a
retrospective group of 41 consecutive patients, who had undergone
APR in the JKP just prior to the introduction of the new ninestep
concept, as historical controls. All patients where operated on
according to the TME method. No extralevator abdominoperineal
excisions were performed. cT4 tumours were referred to the regional
university hospital and are thus not included in this series. The
indications for surgery were similar in the two groups (Table 1). Two
different methods were used to measure wound healing: 1) Time
to perineal wound healing, assessed by the stoma therapists at the
outpatient clinic; a completely healed wound within one month was
considered normal, and 2) Classification of the severity of the wound
complications, by a modified Clavien-Dindo Classification of Surgical
Complications [8] (Table 2). Clinical data were also collected from
the Swedish ColoRectal Cancer Registry. The study was approved by
the regional Ethical Committee in Gothenburg (Reg. no: T941-13).
Statistical analysis
The statistical analysis was performed using the Statistical Package
for the Social Sciences (SPSS version 22-0). The T test and the Mann-
Whitney U test were applied to a univariate analysis of the data. There
was no difference between the group before and the group after the
intervention with respect to the variables in (Table 1). To control for
possible confounders, we applied a multivariate logistic regression
model with infections as outcome and surgical approach, TNM stage
and preoperative radiotherapy as covariates.
The new concept
The new concept was created after a consensus meeting in a group
including the colorectal surgeons, stoma therapists, and nurses from
the surgical ward, anaesthesia department and the outpatient clinic.
The changes to the perioperative routines are referred to as “the ninestep
concept”. Apart from this new, nine-step concept, nothing else
was changed in the perioperative care.
Table 1
Table 1
Data comparing the retrospective group operated on in the JKP before the intervention and the patients in the present, prospective study (T test, Mann- Whitney U test).
Table 2
Figure 1
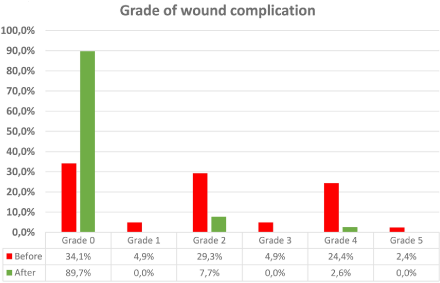
Figure 1
The grade of postoperative perineal wound complications before and after the introduction of the new nine-step concept.
The Nine Step - Concept
- A small enema (120 ml), for mechanical bowel preparation, is administered in the evening before surgery and in the morning on the day of surgery to minimize the risk of faecal leakage to the operation site (responsible: surgical ward).
- The operation starts with a perineal antibacterial wash with Descutan®, after which the anus is closed with double rows of sutures to minimize the risk of faecal leakage to the operation site. This step is completed with a repeated antibacterial wash. Thereafter the abdominal part of the operation is performed and completed (responsible: operating team).
- The patient is placed in the prone position/JKP: According to our guidelines for antibiotic prophylaxis, one dose of Cefuroxime (1.5g) and one dose of Metronidazole (1g) are administrated preoperatively. In the new concept, an additional dose of 1.5g Cefuroxime is given before the perineal part of the operation starts. This is occasioned by the short duration of cefuroxime, with a T½ of 70 minutes, and the start of the perineal phase is often more than three hours after the start of the operation (responsible nurse anaesthetist).
- The levators are divided only as far laterally as oncologically needed, according to the preoperative MRI results, to minimize tissue loss and tissue tension (responsible: surgeon).
- The levators are closed with antibacterial sutures, 2-0 PDS Plus® (polydioxanone with triclosan) [9] (responsible surgeon).
- Septocoll® or Collatamp® (gentamicin-impregnated collagen fleece), 5 x 10 cm, is inserted immediately above the levators before they are closed, for a local antibiotics deposit [10] (responsible surgeon).
- Active Univac Ch10 drainage is placed beneath the levators via a separate incision to avoid pooling of wound secretion (responsible surgeon). The drainage is usually removed on day 2 postoperatively.
- Subcutaneous tissues are sutured with antibacterial suture 2-0 Monocryl Plus® (with triclosan) [9] (responsible surgeon).
- Postoperatively, a seat ring is mandatory to reduce compression of the wound (responsible: surgical ward).
- de Haas WG, Miller MJ, Temple WJ, Kroll SS, Schusterman MA, Reece GP, et al. Perineal wound closure with the rectus abdominis musculocutaneous flap after tumor ablation. Ann Surg Oncol. 1995; 2: 400-406.
- Bullard KM, Trudel JL, Baxter NN, Rothenberger DA. Primary perineal wound closure after preoperative radiotherapy and abdominoperineal resection has a high incidence of wound failure. Dis Colon Rectum. 2005; 48: 438-443.
- Tevis SE, Kohlnhofer BM, Stringfield S, Foley EF, Harms BA, Heise CP, et al. Postoperative complications in patients with rectal cancer are associated with delays in chemotherapy that lead to worse disease-free and overall survival. Dis Colon Rectum. 2013; 56: 1339-1348.
- Ip B, Jones M, Basset P, Philips R. Factors affecting the healing of the perineum following surgery. Ann R Coll Surg Engl. 2013; 95: 252-257.
- Asplund D, Prytz M, Bock D, Haglind E, Angenete E. Persistent perineal morbidity is common following abdominoperineal excision for rectal cancer. Int J Colorectal Dis. 2015; 30: 1563-1570.
- AsplundD, Haglind E, Angenete E. Outcome of extralevator abdominoperineal excision compared with standard surgery. Results from a single centre. Colorectal Dis. 2012; 14: 1191-1196.
- Hassel K, Andersson K, Koinberg IL, Wennström B. Postoperative wound infections after a proctectomy-Patient experience. Int J Qual Stud Health Well-being. 2016; 11: 3039.
- Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien-Dindo Classification of Surgical Complications - Five- Year Experience. Ann Surg. 2009; 250: 187-196.
- Daoud FC, Edmiston CE, Leaper D. Meta – analysis of prevention of surgical site infections following incision closure with triclosan-coated sutures: robustness to new evidence. Surg Infect (Larchmt). 2014; 15: 165- 181.
- de Bruin AF, Gosselink MP, Wijffels NA, Coene PP, van der Harst E. Local gentamicin reduces perineal wound infection after radiotherapy and abdominoperineal resection. Tech Coloproctol. 2008; 12: 303-307.
- Welsch T, Mategakis V, Contin P, Kulu Y, Büchler MW, Ulrich A. Results of extralevator abdominoperineal resection for low rectal cancer including quality of life and long-term wound complication. Int J Colorectal Dis. 2013; 28: 503-510.
- Gunnarsson U, Seligsohn E, Jestin P, Påhlman L. Registration and validity of surgical complications in colorectal cancer surgery. Br J Surg. 2003; 90: 454-459.
- Karanika S, Karantanos T, Theodoropoulos GE. Immune response after laparoscopic colectomy for cancer: a review. Gastroenterol Rep. 2013; 1: 85-94.
- West NP, Finan PJ, Anderin C, Lindholm J, Holm T, Quirke P. Evidence of the oncologic superiority of cylindrical abdominoperineal excision for low rectal cancer. J Clin Oncol. 2008; 26: 3517-3522.
- Shihab OC, Heald RJ, Holm T. A pictorial description of extralevator abdominoperineal excision for low rectal cancer. Colorectal Dis. 2012; 14: e655-660.
Results
A comparison of the data for the retrospective group operated
in the JKP before the introduction of the nine-step concept and the
consecutive patients in this prospective study showed no significant
difference in background data between the two groups, except for
laparoscopic vs. open surgery (p< 0.043) (Table 1).
Perineal infections were registered for a total of 10 % of the patients
in the prospective group, compared with 66 % in the retrospective
group (p< 0.001). The infection rate remained significantly reduced
after intervention (OR=0.05; 95%CI 0.01-0.3) also when we applied
a multiple model including TNM stage (OR=7.04; 95%CI 1.8-
27.7), preoperative radiotherapy (OR=1.52; 95% CI 0.20-11.6) and
surgical approach (open surgery OR=1.65; 95% CI 0.34-8.11). The
postoperative infections were also less severe in the prospective
group (Figure 1). The time to perineal wound healing was shorter in
the prospective group compared with the retrospective group (Figure
2). Four patients in the prospective group developed a postoperative
infection. Three patients had a superficial infection, which healed
within three months. One patient had a severe infection that required
surgery. This patient died after four months, still having a perineal
infection, and is included in the analysis.
Two patients died within 30 days after surgery (one of stroke and
one of circulatory collapse), and were excluded from the analysis.
No differences in the oncological results were seen in our study.
Discussion
This study showed that this new concept of preoperative
enema, dual anal suturing and disinfection, additional prophylactic
antibiotics, moderate levator excision, antibacterial sutures, antibioticimpregnated
collagen, perineal drainage and postoperative seat ring
use is effective. To be able to assess wound healing and postoperative
infections we modified the Clavien-Dindo classification of surgical
complications [8], to make it more suitable for different grades of
postoperative perineal problems. Small infections also affect patients
and increase the costs for society, for example, in terms of change of
dressings, extra visits to district nurses and outpatient clinics, need
for longer sick leave, etc. For those reasons we decided to identify and
report every deviation from “the normal” as a problem. The extreme
infection rate noted after introducing the JKP, and before introduction
of the new concept, is high when compared with other studies [2 and 6].
One explanation could be that we recorded all disturbances in terms
of perineal postoperative infections and wound healing. Minor
problems are often not accounted for in the literature. In the Swedish
ColoRectal Cancer Registry (SCRCR), the recording of complications
(such as infections) starts with Clavien-Dindo II and ends 30 days
postoperatively. In this study, we discovered, as in other studies [11],
that a number of perineal infections occurred later than 30 days after
the index operation (Table 2). In a validation of the SCRCR, it was
shown that 22% of surgical complications were missed [12]. This is
in accordance with our findings, where a comparison showed that
20% of the perineal complications would have been missed if only
the registry had been used. The same Clavien-Dindo scale has been
used in all three cohorts of patients (before JKP retrospectively, after
JKP retrospectively, and in this prospective study), but in the first two
historical cohorts, we classified the patients retrospectively from case
records and the registry. Some minor infections may therefore have
been missed in the retrospective groups, but in this prospective study
group, all wound problems have been accounted for.
The strength of this study is the design with consecutive patients
without dropouts. The two study groups are comparable with respect
to gender, age, preoperative diagnosis, diabetes, steroid medication,
and perioperative bleeding and bowel perforation (Table 1). The
study was performed in one department, with the same staff, and
with the same surgeons performing the surgery throughout the whole
study period.
There are some limitations to the study, as it is not randomized
and the controls are historical. However, since we had an unacceptably
high infection rate and long wound healing time, we felt that it
would be unethical to perform a randomized study. The sample size
is small, but patients are consecutive APR cases before and after the
intervention. There are some differences between the groups, such
as a tendency towards less preoperative radiotherapy and lower
tumour stages in the intervention group. Both these differences could
contribute to fewer infections. However, these differences are not
statistically significant. The only statistical difference between the two
groups is that the abdominal part of the operation was performed
by laparoscopy in more patients in the intervention group (64% vs.
43%, p < 0.043). This fact should not influence the perineal part of the
operation, but it has been suggested that the immunological response
is less affected after laparoscopy compared with open surgery [13],
which may also influence the infection rates.
Which of the nine steps in the concept are the key factors? Two
main differences can be recognized, for instance, the early closure of
the anus with a double row of sutures and the extra dose of antibiotics
(Cefuroxime). The early closure of the anus resembles what we did
in the supine position and could prevent leakage of fluid and stools
contaminating the perineal skin. Before the concept was introduced,
this closure was postponed until after the patient was turned to the
JKP.
Our choice of prophylactic antibiotics includes Cefuroxime with
a short half-life. An extra dose was therefore given just before the start
of the perineal part of the operation, to ensure good MIC values in the
operating area. The perineal dissection starts approximately 3-4 hours
after the first administration of the antibiotic. The roles of perineal
drainage, local antibiotics [10] and antibacterial sutures [9] are more
difficult to assess. Hence, since the total concept works, we have not
excluded any of the steps so far. The combined concept involves all
perioperative steps of the patient care process and the whole team
is aware of the process, as well as of their role in implementing the
concept.
A further consideration, which could affect the outcome, might
be the learning curve for the surgeons. We altered our positioning
of the patient according to the JKP in the retrospective group from
2010. This means that the surgeons were more accustomed to the JKP
in the prospective group in 2013-2014. However, the infections were
evenly distributed in the retrospective group without any observed
learning curve effect.
Postoperative wound complications are expensive. The costs
include prolonged hospital stays, readmissions, surgery, home nursing
care, repeated wound dressing, materials costs and outpatient visits. It
is difficult to estimate the costs, but our hospital economist estimated
the extra costs to at least €8800 per patient with complications. The
results have huge implications for many patients. Prevention of an
infection means less suffering for the patient and reduced health care
expenditure.
This study highlights the importance of how team collaboration
can improve results by introducing a multi-modal approach and a
check-list to address a defined problem (such as the SSI rate). The
alarm signal of an increasing number of postoperative problems came
from the stoma therapists and the retrospective analysis confirmed
their suspicions. The team discussed the situation and all steps of the
perioperative care process were evaluated. We contemplated returning
to the lithotomy position; however, the presumptive advantages of the
JKP, such as better ergonomics, view and assistance, and potentially
better oncological surgery with increased circumferential margins
and fewer bowel perforations [14,15], convinced us to continue with
the JKP.
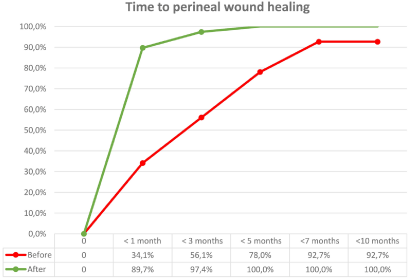
Figure 2
Figure 2
Time to perineal wound healing before and after the introduction of
the new nine-step concept.
Conclusion and Clinical Implications
In summary, after introducing a new concept, including nine perioperative steps during APR, we found a substantial reduction in the rate of postoperative perineal infections. The effect is promising, does not involve any expensive investments or special equipment, and is easy to implement in clinical practice. Fewer infections mean less suffering for the patient and substantially reduced use of health care resources.
Acknowledgement
We would like to express our thanks to Salmir Nasic and Anna- Lena E-son Loft for statistical expertise, the stoma therapists Anna Johansson and Lise-Lotte Kempe, and to the ward and operating staff, as well as the colorectal team at Skaraborg Hospital, Skövde.