Research Article
Left Renal Vein Balloon Venoplasty without Stenting for Management of Symptomatic Nutcracker Syndrome
Nassiri N1*, Shafritz R1, Rahimi S1, Patel PB2, Araujo L2 and Thomas J3
1Department of Surgery, Rutgers Robert Wood Johnson Medical School, USA
2Department of General Surgery, Rutgers Robert Wood Johnson Medical School, USA
3Medical Student, Rutgers Robert Wood Johnson Medical School, USA
*Corresponding author: Naiem Nassiri, Department of Surgery, Division of Vascular Surgery and Vascular Anomalies & Malformations Program (VAMP), Rutgers Robert Wood Johnson Medical School, One Robert Wood Johnson Place MEB 541, New Brunswick, New Jersey 08901, USA
Published: 14 Oct, 2016
Cite this article as: Nassiri N, Shafritz R, Rahimi S,
Patel PB, Araujo L, Thomas J. Left
Renal Vein Balloon Venoplasty
without Stenting for Management of
Symptomatic Nutcracker Syndrome.
Clin Surg. 2016; 1: 1157.
Abstract
Nutcracker Syndrome (NCS) is a rare vascular anomaly involving left renal vein outflow entrapment
most commonly secondary to compression between the aorta and the superior mesenteric artery.
This can lead to chronic renal venous hypertension which can cause varicosity formation, gonadal
vein reflux, hematuria, and if severe enough, renal failure. While open surgical reconstruction is
heralded as the gold standard for treatment of this disorder, endovascular treatment is increasingly
reported in recent literature. Herein, we present a unique approach to treatment of a severely
symptomatic Nutcracker Syndrome via left renal vein outflow venoplasty without stenting
performed in conjunction with embolization of refluxing varicosities.
Keywords: Left renal vein; Venoplasty; Stenting; Nutcracker syndrome
Introduction
Nutcracker Syndrome (NCS) or left renal vein entrapment syndrome is a rare congenital disorder involving compression of the left renal venous outflow. The most common scenario involves compression of the central-most segment of the left renal vein as it courses between the aorta and the Superior Mesenteric Artery (SMA). Compression can also take place with retroaortic (posterior nutcracker syndrome) and circumaortic left renal veins [1,2]. By far, the most commonly reported and the gold-standard treatment modality is open surgical reconstruction via left renal vein distal transposition, venolysis with patch venoplasty, or proximalization of the SMA [3]. While mid to long term outcomes using this approach remain satisfactory, the invasive nature of the operation and associated morbidity make it an undesirable first-line option. Recently, endovascular stenting of the central left renal vein has been reported more frequently with satisfactory short to midterm results. However, there have been reports of stent fracture, migration, and thromboembolic complications that have questioned the durability and safety of stenting [4-7]. Here in, we present a case of a severely symptomatic Nutcracker Syndrome in a 23 year old female treated successfully via central left renal venoplasty with coil embolization of refluxing varicosities.
Background
A 23 year old female with a history of Irritable Bowel Syndrome (IBS) presented to our institution
with a 3-dayhistoryof severe, throbbing, left flank pain. The pain was localized to the left flank and
perinephric region, radiating to the left groin, and was associated with nausea. She reported similar
episodes of severe flank and pelvic pain over the course of one year that was particularly worse
during menstruation. She also had several episodes of menorrhagia. On presentation, she was a
febrile, tachycardic (102 beats/min) with minimal costo-vertebral angle tenderness. The patient had
evidence of microscopic hematuria with negative urine cultures and no evidence of pregnancy.
Computed Tomography Angiography (CTA) with delayed venography (CTV) revealed severe
compression of the left renal vein outflow between the SMA and the aorta, a dilated left ovarian
vein, and enlarged tortuous left-sided pelvic vessels. The angle between the SMA and the aorta on
sagittal reconstructions measured approximately 20 degrees. A left renal vein duplex was obtained
confirming significant central venous compression between the SMA and the aorta measuring
approximately 4mm in diameter compared to a more peripheral maximum diameter of 19 mm (a
ratio of approximately 1:5). Spectral wave form analysis at the point of compression revealed apulsatile
venous signal with a velocity of 250 cm/second compared to caval velocities of approximately 60
cm/sec (a ratio of approximately 4:1). Given these findings, she was recommended to undergo
diagnostic angiography as well as venography to better delineate the
local angio architecture, rule out pelvic arteriovenous malformations,
and assess extent of pelvic venous reflux. Endovascular therapy if
deemed appropriate would be offered concomitantly.
Materials and Methods
The procedure was performed in the hybrid operating suite
under general endotracheal anesthesia. Flush aortography via right
common femoral artery puncture revealed no evidence of high-flow
arteriovenous malformations, uterine leiomyomas, or congenital
renal arterial anomalies. However, delayed phase venographic runs
revealed delayed emptying of the left renal nephrogram relative to the
normal right side suggesting a venous outflow compromise (Figure
1A and B).
At this point, the left common femoral vein was accessed
and diagnostic iliocavogram revealed no abnormalities. Selective
catheterization of the Left Renal Vein (LRV) revealed a high-grade
stenosis at the LRV outflow close to its insertion into the Inferior
Vena Cava (IVC) (Figure 1C). The area of stenosis was crossed using
an angled glidewire and a 5-Fr Cobra catheter (Terumo, Tokyo,
Japan) exchanged for a 5-Fr marked pigtail catheter positioned as
far peripherally as possible into the LRV. Diagnostic venogram in
multiple projections including anteroposterior, oblique, and sagittal
windows revealed significant stagnation of LRV outflow due to central
LRV stenosis with subsequent formation of large LRV refluxing
varicosities extending into the left pelvic circulation with subsequent
drainage into the accessory hemiazygous system. In addition, a large,
refluxing left gonadal vein was also noted with extensive pooling
of venous blood into the left para-uterine region collateralizing in
this area with the right side (Figure 1D-F).A pressure gradient of
10mmHg was noted across the area of LRV stenosis.
We initially proceeded with balloon venoplasty of the LRV stenosis
using a 10 x 40 mm Mustang balloon (Boston Scientific, Marlborough,
MA) (Figure 2). Post venoplasty showed brisk, unobstructed flow
through the previously stenotic area with significantly decreased
filling of the LRV varicosities (Figure 3) and no evidence of recoil or
restenosis across the treated area. There was also noted to be improved
flow through the adrenal and lumbar tributaries. No further pressure
differential was noted across the venoplastied area.
Given the presence of incompetent left gonadal vein and LRV
varicosities causing significant pelvic congestion syndrome, decision
was made to proceed with coil embolization of these veins. These veins
were selectively catheterized using a 5-French Berenstein catheter
(Angio-dynamic Co, Queensboro, NY) with subsequent insertion
of a6-French 55 cm Raabe Sheath (Cook Medical, Bloomington,
IN). Left gonadal vein embolization was performed via3 densely
packed pushable 0.035 platform coils (Interlock, Boston Scientific,
Marlborough, MA) (Figure 2B). Similarly, the large dominant LRV
varicosity was accessed and coil embolized with a single pushable
coil (Figure 2C and D). Completion venogram showed elimination
of pelvic reflux with maintained brisk, unobstructed flow through
the LRV into the IVC (Figure 3). There were no perioperative
complications. Patient was admitted for overnight observation.
She reported elimination of left flank pain at the time of discharge.
She was seen in follow-up at 2 weeks, 3 months, 6 months, with no
recurrence of symptoms. Follow-up LRV duplex revealed a velocity
gradient of less than 3 with a LRV outflow diameter ranging from
6-15 mm. In absence of recurrence of symptoms, she will be followed
annually with LRV duplex surveillance. Consent to publish this
manuscript was formally obtained from the patient.
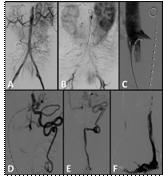
Figure 1A-B
Figure 1A-B
Flush aortography demonstrates no evidence of arterial pathology but reveal evidence of left renal venous hypertension with sluggish washout of left nephrogram contrast.
C: Selective left renal vein catheterization confirms central renal venous stenosis.
D-F: The lesion is crossed and flush venography demonstrates significant renal vein varicosities with significant reflux into the left gonadal venous system.
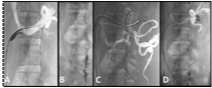
Figure 2A
Figure 2A
Significant wasting noted during balloon venoplasty of the central left renal vein.
B: Selective catheterization and sheath insertion with deposition of pushable coils into the left gonadal vein.
C-D: Selective catheterization of the left renal vein varicosities with coil embolization.
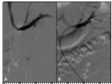
Figure 3A-B
Figure 3A-B
Completion venography shows brisk washout of contrast through left renal view with no visualization of the varicosities and gonadal vein reflux even on delayed venous runs.
Discussion
Venous entrapment syndromes such as May-Thurner Syndrome,
Thoracic Outlet Syndrome, and NCS are increasingly recognized
and reported in the recent literature in large part due to enhanced
endovascular diagnostic capabilities and growing awareness amongst
treating specialists [8-10]. The Hamburg Classification Scheme
categorizes these venous entrapment syndromes as congenital,
obstructive venous anomalies and labels them as truncal vascular
malformations given their central location and embryological patterns
of development [11]. NCS involves hemodynamically significant
compression of the LRV outflow near its insertion point into the IVC
most commonly secondary o a hyperacute angle between the SMA
and the aorta. NCS can also occur with retroaortic and circumaortic
LRV configurations [1,2]. Symptoms, when present include most
commonly left flank and lower abdominal pain, hematuria (both
microscopic and gross), and pelvic congestion syndrome [10,12,13].
The latter develops secondary to the formation of incompetent
varicosities and development of reflux within the left gonadal vein.
Diagnosis is mainly one of exclusion after the onset of symptoms
which can be generalized and non-specific or potentially ignored
and brushed off as psychogenic in origin as was the case in our
patient who was given a diagnosis of IBS prior to vascular surgery
evaluation and subsequent workup. Once more common diagnoses
such as primary pelvic congestion syndrome, neoplasm, iatrogenesis,
and medical renal pathology (especially autoimmune and postinfectious
etiologies) have been ruled out, clinical suspicion for
NCS rises most often due to the incidental finding of LRV pathology
on imaging performed for work up of other etiologies. Once the
diagnosis of NCS is entertained, LRV duplex in combination with
Computed Tomography Venography (CTV) or Magnetic Resonance
Venography (MRV) is strongly recommended for confirmation of
the diagnosis and assessment of the hemodynamic significance of the
lesion. What will determine the need for diagnostic venography is
presence of several key distinctive features on dedicated LRV duplex
ultrasound. These include LRV compression ratio of greater than 5,
compared to the dilated peripheral portion, and compressed velocity
ratio of greater than 5 compared to adjacent IVC velocities [3,10].
The third definitive criteria for diagnosis of NCS requires selective
LRV catheterization with venography and measurement of pressure
gradients across the area of compression. A pressure gradient of
greater the3 is considered hemodynamically significant [3,14].
Venography can also facilitate use of intravascular ultrasound (IVUS)
and multiplanar imaging for more accurate assessment of degree and
hemodynamic significance of the stenosis, venous drainage patterns,
and extent of pelvic reflux if present [15].
Open surgical reconstruction is the current gold-standard
modality for intervention, with favorable mid to long term outcomes
noted in several reports [14,16]. The most common open approach
is an inferior transposition of the LRV [3]. Distal transposition, with
end to side reanastomosis, has shown to provide good patency out
comes in pediatric patients [17]. However, the morbidity associated
with the invasive nature of these open procedures continues to
make them a less desirable first-line option. Indeed, when presented
with potential options for treatment, our patient refused all open
interventions given associated morbidity. Endovascular intervention,
on the other hand, is a newer, less invasive, fairly effective approach
for treatment of symptomatic NCS. Historically and by and large,
endovascular therapy has comprised of stent deployment across the
area of compression often requiring extension into the IVC [2,4].
Stent use has seen favorable outcomes in several case reports and
series, but significant concerns remain with their use in the young
population owing mostly to reports of in-stent thrombosis and
stent migration [4-7]. Furthermore, long-term outcomes remain
unknown. The dynamic configuration of LRV wall circumference
makes it suboptimal for stent placement. Proper apposition is often
difficult, and therefore formation of gutters as well as stent migration
with fracture and thromboembolic phenomenon are not uncommon
[4-7,18]. In a large series by Chen et al. [7] perioperative stent
complications requiring operative intervention and stent migration
into the right atrium have occurred.
Venoplasty alone without stent placement has not been reported
commonly in the literature. Indeed we encountered only a single case
in the English language literature reporting the use of venoplasty for
treatment of symptomatic NCS. Similar to the current case, Bekou
and colleagues reported a case of NCS with severe pelvic congestion
treated with LRV venoplasty and ovarian vein embolization [19].
Their patient was asymptomatic at 18-month follow-up with widely
patent LRV, as confirmed by LRV duplex.
Not unlike symptomatic varicose veins of the lower extremities,
pelvic varicosities associated with NCS develop as a result of
venous hypertension caused by obstruction and subsequent reflux.
Alleviation of both obstruction and reflux is necessary to achieve
maximum therapeutic benefit. In this case, we have demonstrated
that LRV venoplasty alone without routine stenting in conjunction
with embolization of the refluxing gonadal vein and LRV varicosities
can be highly effective in alleviating LRV hypertension and associated
NCS symptoms. It forgoes the need for stent surveillance and
maintenance and obviates the need for a major morbid operation.
While larger experience and longer follow ups are needed before any
stern recommendations can be made, it is safe to propose that this
approach may serve as an acceptable first-line treatment modality
for symptomatic NCS before stenting or open surgical revisions are
entertained.
References
- Skeik N, Gloviczki P, Macedo TA. Posterior nutcracker syndrome. Vasc Endovascular Surg. 2011; 45: 749–755.
- Cronenwett JL, Johnson KW. Iliocaval Venous Obstruction: Surgical Treatment Rutherford’s Vascular Surgery. 8th ed. London: Elsevier Health Sciences. 2010; 950.
- Said SM, Gloviczki P, Kalra M, Oderich GS, Duncan AA, D Fleming M, et al. Renal nutcracker syndrome: Surgical options. Semin Vasc Surg. 2013; 26: 35–42.
- Chen S, Zhang H, Shi H, Tian L, Jin W, Li M. Endovascular stenting for treatment of Nutcracker syndrome: report of 61 cases with long-term follow up. J Urol. 2011; 186: 570–575.
- Hartung O, Grisoli D, Boufi M, Marani I, Hakam Z, Barthelemy P, et al. Endovascular stenting in the treatment of pelvic vein congestion caused by nutcracker syndrome: lessons learned from the first five cases. J Vasc Surg. 2005; 42: 275–280.
- Rana MA, Oderich GS, Bjarnason H. Endovenous removal of dislodged left renal vein stent in a patient with nutcracker syndrome. Semin Vasc Surg. 2013; 26: 43–47.
- Chen S, Zhang H, Tian L, Li M, Zhou M, Wang Z. A stranger in the heart: LRV stent migration. Int Urol Nephrol. 2009; 41: 427–430.
- Nazzal M, El-FedalyM, Kazan V, Qu W, Renno A, Al-Natour M, et al. Incidence and clinical significance of iliac vein compression. Vascular. 2015; 23: 337-343.
- Poretti D, Lanza E, Sconfienza LM, Mauri G, Pedicini V, Balzarini L, et al. Simultaneous bilateral magnetic resonance angiography to evaluate thoracic outlet syndrome. Radiol Med. 2015; 120: 407-412.
- Gulleroglu K, Gulleroglu B, Baskin E. Nutcracker syndrome. World J Nephrol. 2014; 3: 277–281.
- Belov S. Anatomopathological classification of congenital vascular defects. Semin Vasc Surg. 1993; 6: 219–224.
- He Y, Wu Z, Chen S, Tian L, Li D, Li M, et al. Nutcracker Syndrome--how well do we know it? Urology. 2014; 83: 12–17.
- D’Archambeau O, Maes M, De Schepper AM. The pelvic congestion syndrome: Role of the “nutcracker phenomenon” and results of endovascular treatment. JBR-BTR. 2004; 87: 1–8.
- Reed NR, Kalra M, Bower TC, Vrtiska TJ, Ricotta JJ, Gloviczki P. Left renal vein transposition for nutcracker syndrome. J Vasc Surg. 2009; 49: 386–393.
- Mahmood SK, Oliveira GR, Rosovsky RP. An easily missed diagnosis: flank pain and nutcracker syndrome. BMJ Case Rep. 2013; 2013.
- Hohenfellner M, D’EliaG, Hampel C, Dahms S, Thüroff JW. Transposition of the left renal vein for treatment of the nutcracker phenomenon: longterm follow-up. Urology. 2002; 59: 354–347.
- Ullery BW, Itoga NK, Mell MW. Transposition of the Left Renal Vein for the Treatment of Nutcracker Syndrome in Children: A Short-term Experience. Ann Vasc Surg. 2014; 28: 1938. e5-8.
- Gloviczki P. Nutcracker Syndrome. From Foam to Filters: What’s New in Venous Disease in 2012. 2012 Feb 4; Durham, NC.
- Bekou V, Zollikofer C, Nieuwkamp N, von Weymarn A, Duewell S, Traber J. A therapeuticoption in nutcracker syndrome and ovarian vein insufficiency. Phlebololgy. 2014; 29: 144–149.