Research Article
Utilisation of Bicipital Aponeurosis for Banding to Treat the Dialysis Access Steal Syndrome (DASS) in High Flow Brachial-Cephalic Arterio-Venous Fistula: A Case Report
Przywara S*, Ilzecki M, Terlecki P and Zubilewicz T
Department of Vascular Surgery and Angiology, Medical University of Lublin, Poland
*Corresponding author: Stanislaw Przywara, Department of Vascular Surgery and Angiology, Medical University of Lublin, Staszica 11 Street, 20-081 Lublin, Poland
Published: 13 Oct, 2016
Cite this article as: Przywara S, Ilzecki M, Terlecki P,
Zubilewicz T. Utilisation of Bicipital
Aponeurosis for Banding to Treat
the Dialysis Access Steal Syndrome
(DASS) in High Flow Brachial-Cephalic
Arterio-Venous Fistula: A Case Report.
Clin Surg. 2016; 1: 1152.
Abstract
We present a case of 36 years old male with end stage renal failure, hemodialysed for 3 years, who developed symptomatic Dialysis Access Steal Syndrome (DASS) in his right hand due to high flow brachial–cephalic arterio-venous fistula. Surgical treatment of steal syndrome was performed by aneurysmorrhaphy of draining cephalic vein, reinforced by the use of the part of bicipital aponeurosis as a native material for external banding. Intra-operative ultrasound showed immediate decrease of flow through the fistula, which dropped down from 2,6 L/min. to 900 mL/min. In postoperative period we observed complete recovery from upper limb ischemia symptoms. Patient received renal transplant 11 months later. During the follow up period, we did not observe any symptoms of DASS recurrence or infection and the fistula provided adequate hemodialysis. In selected patients, utilisation of bicipital aponeurosis as a native material for banding to treat DASS in high flow upper arm arterio-venous fistulas may be an alternative for PTFE (polytetrafluoroethylene) external cuff or PTFE graft axial interposition procedures.
Introduction
The frequency of Dialysis Access Steal Syndrome (DASS) after creation of upper arm arteriovenous fistula is reported to range from 1 to 8%. DASS may produce clinical symptoms of hand ischaemia and additionally, in cases of high flow fistulas right ventricle overload. Both these factors significantly influence the patient’s health status and the quality of life [1]. There are several surgical procedures to treat DASS. Some of them as Distal Revascularisation with Interval Ligation (DRIL), Proximal Arterial Inflow (PAI) and Revision Using Distal Inflow (RUDI) are quite extensive and may not be appropriate for young patients awaiting urgent renal transplantation. Some, more simple approaches as PTFE (polytetrafluoroethylene) external cuff or PTFE graft axial interposition require use of the synthetic materials, what significantly may increase the risk of infection [2]. We present a simple procedure of DASS surgical treatment with utilization of bicipital aponeurosis as a native material for banding after standard aneurysmorrhaphy of draining vein.
Material and Methods
A 36 years old male with end stage renal failure, was hemodialysed for 3 years. After 3 years he
developed symptomatic DASS of his right hand due to high flow brachial–cephalic arterio-venous
fistula. This was a relatively rare case of DASS associated with high flow fistula with otherwise
normal vessels. Patient was hypertensive but had negative history of diabetes and peripheral arterial
disease. Ultrasound measurements showed an aneurysmal cephalic vein with an excessive blood
flow through the fistula, reaching 2,6 L/min. and moderate symptoms of the right ventricle overload.
His right hand presented typical subjective symptoms of peripheral upper limb ischemia such as
pain of the hand and paresthesias, with formation of an ischemic ulceration of the IIIrd finger (DASS
grade III) according to classification of Sidawy [3]. Objective confirmation of steal syndrome was
obtained by measurements of systolic pressure index and laser Doppler flowmetry assessment [4].
Patient was awaiting transplantation.
Taking into consideration the age of the patient and possible kidney transplantation in the future,
the decision was made not to proceed with sophisticated and extensive surgical procedures neither to
use PTFE external banding or PTFE graft interposition. As we had negative clinical experience with
aneurysmorrhaphy only procedure in reduction of DASS (vein usually tends to dilate again with
time), we decided intraoperatively to utilize bicipital aponeurosis (also known as lacertus fibrosus)
as a native material for banding to reduce the steal syndrome and
high flow. The area of arterio-venous anastomosis was explored with
s-shape incision of the skin, what enabled exposure of anastomosis
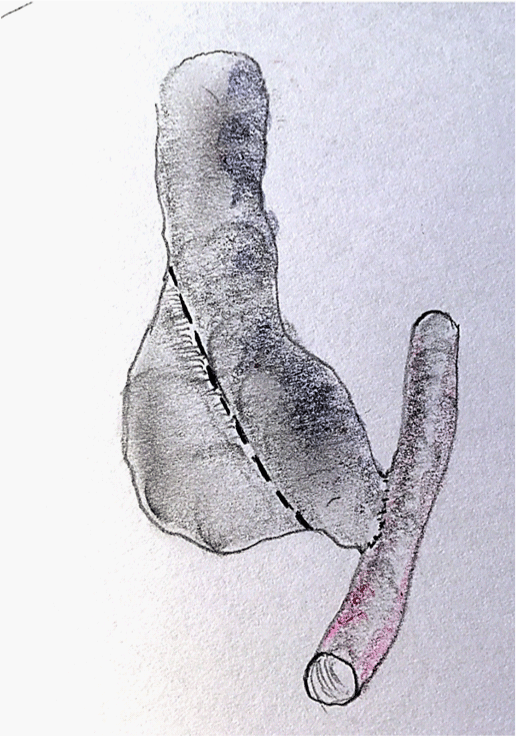
and aneurysmal segment of cephalic vein. The aneurysm of draining
cephalic vein underwent narrowing aneurysmorrhaphy with an
excision of superfluous wall of the aneurysm (Figure 1). Reduction of
the diameter of the vein during aneurysmorrhaphy was continuously
monitored by intra-operative ultrasound to achieve the reduction of
the flow to the level of 800-900 ml/min. as recommended by DOQI
guidelines [5]. Narrowing of the arterio-venous anastomosis was not
necessary, because the preoperative ultrasound showed the maximal
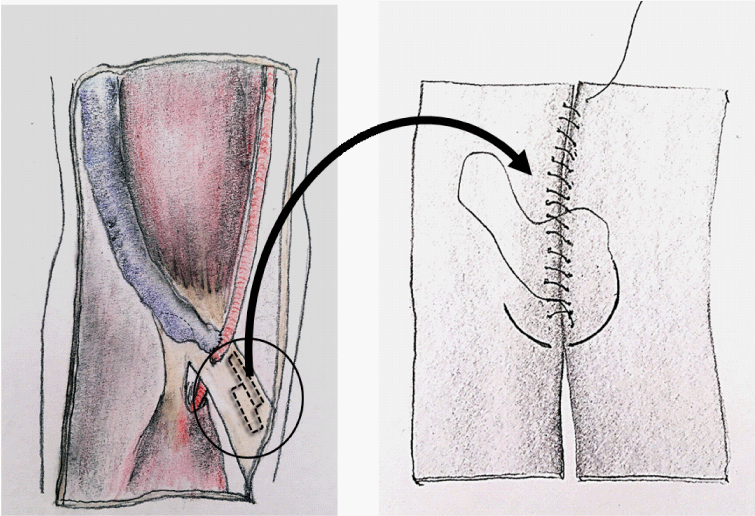
diameter of anastomosis of 4 mm. Part of aponeurosis was excised
as shown on the Figure 2. Then, the excised part of aponeurosis was
duplicated and re-sutured to form a native material for external cuff
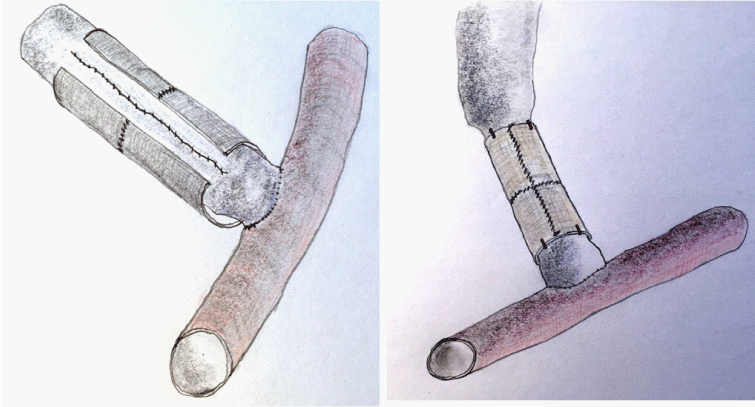
(Figure 2). Finally, previously prepared band, made of native bicipital
aponeurosis, was wrapped around the narrowed vein and sutured
(Figure 3). A few additional stiches secured the position of this
external cuff in place, thus preventing any movements of the band,
incidentally caused by high pressure, pulsative flow through the vein.
Figure 1
Figure 2
Figure 3
Results
We achieved immediate reduction of flow after aneurysmorrhaphy
and external banding from 2,6 L/min. to 900 ml/min as measured
by intraoperative ultrasound. The subjective symptoms of peripheral
upper limb ischemia, such as pain of the hand and paresthesias,
disappeared within a few days after the procedure. Ischemic ulceration
of the IIIrd finger healed completely after 1 month. The fistula provided
adequate flow to conduct the hemodialysis until the patient received
the renal transplant 11 months later. Monthly measured fistula flow
parameters oscillated in the range of 800 mL/min-1,1 L/min.
We did not observe any recurrence of DASS symptoms or
infection. Independent neurological and orthopaedic assessment did
not show any significant neurological and motor deficiencies after
surgery.
Discussion
DASS after creation of upper arm arterio-venous fistula occurs
in 1-8% of patients [1]. Available surgical techniques for DASS
treatment include narrowing of the draining vein or arteriovenous
anastomosis by simple re-suturing, external banding with
PTFE cuff, axial interposition of tapered PTFE prosthesis, Distal
Revascularisation with Interval Ligation (DRIL), Proximal Arterial
Inflow (PAI), Revision Using Distal Inflow (RUDI) and Minimally
Invasive Limited Ligation Endoluminal-assisted Revision (MILLER)
[1,2]. The most preferred option nowadays is DRIL, however it
is quite sophisticated and time consuming surgical technique. In
our experience aneurysmorrhaphy only of the draining vein is
a simple procedure, however the vein tends to dilate with time
and the symptoms of steal syndrome or high flow usually reoccur.
Implantation of synthetic material like PTFE as an external cuff or
axial interposition graft increases significantly the risk of infection [6].
Our novel surgical approach with utilization of bicipital aponeurosis
as a native material for banding may be a valuable option for selected
patients with high flow native arterio-venous upper arm fistula and
symptomatic DASS. Narrowing of the aneurysmal draining vein,
reinforced with external banding (to obtain a long term effect of the
procedure) aimed to increase the resistance of the fistula to divert
flow down the native artery [4].
The bicipital aponeurosis (also known as lacertus fibrosus) is a
relatively broad ligamental structure of the brachial biceps which
protects deep anatomical structures in cubital fossa. Although this
protective function of brachial artery and median nerve is important,
there are data in the literature, that complete trans-section of this
aponeurosis in specific clinical situations does not cause any motor
or neurological deficiencies to the upper extremity [7-9]. In our
technique, the resection of the part of aponeurosis was performed
mainly longitudinally with the great care to salvage the continuity
of its most lateral and medial fibers. There are cases describing
complete resection of aponeurosis to treat acute upper limb ischemia
caused by an entrapment of brachial artery due to anomalous
anatomy or supracondylar fracture [7,8]. In patients with symptoms
of claudication of upper limb and diagnosed with brachial artery
compression by aponeurosis, its surgical release restored normal
pulses [9]. In all those cases authors did not observe any subsequent
motor deficiencies.
Young age of the patient, a short perspective for kidney transplant
determined our intraoperative decision to utilize native material
during DASS surgical treatment rather than a use of synthetic PTFE
material which might have put the patient at a risk of infection. From
the same reasons, we did not decide to perform an extensive surgery
such as DRIL procedure. To our knowledge this is the first case of
utilization of bicipital aponeurosis as the native material for banding
procedure of high flow upper arm arterio-venous fistula producing
DASS.
Conclusion
Our case study shows that utilisation of bicipital aponeurosis as a native material for banding to treat DASS, in high flow brachialcephalic arterio-venous fistula may be an alternative to other techniques. External banding with PTFE cuff or axial interposition of PTFE graft may increase the risk of infection related to application of synthetic material. Surgery is not extensive when compared to DRIL, PAI or RUDI procedures. Native cuff, made of bicipital aponeurosis, seems to be durable, efficiently reduces flow through the fistula and releases from the symptoms of DASS.
References
- Goel N, Miller GA, Jotwani MC, Licht J, Schur I, Arnold WP. Minimally Invasive Limited Ligation Endoluminal-assisted Revision (MILLER) for treatment of dialysis access-associated steal syndrome. Kidney Int. 2006; 70: 765-770.
- Gupta N, Yuo TH, Konig G 4th, Dillavou E, Leers SA, Chaer RA, et al. Treatment strategies of arterial steal after arteriovenous access. J Vasc Surg. 2011; 54: 162-167.
- Sidawy AN, Gray R, Besarab A, Henry M, Ascher E, Silva M Jr, et al. Recommended standards for reports dealing with arteriovenous hemodialysis accesses. J Vasc Surg. 2002; 35: 603-610.
- Zamani P, Kaufman J, Kinlay S. Ischemic steal syndrome following arm arteriovenous fistula for hemodialysis. Vasc Med. 2009; 14: 371-376.
- AV Fistula First Breakthrough Coalition. National Vascular Access Improvement Initiative (NVAII).
- Schild AF, Perez E, Gillaspie E, Seaver C, Livingstone J, Thibonnier A. Arteriovenous fistulae vs. arteriovenous grafts: a retrospective review of 1,700 consecutive vascular access cases. J Vasc Access. 2008; 9: 231-235.
- Cevirme D, Aksoy E, Adademir T, Sunar H. A Perplexing Presentation of Entrapment of the Brachial Artery. Case Rep Vasc Med. 2015; 2015: 236193.
- Clark D, Astle L, Monsell F, Livingstone J. The bicipital aponeurosis may be involved in the anatomical etiology of arterial compromise after swelling in supracondylar fracture. J Orthop Trauma. 2009; 23: 731-733.
- Bassett FH 3rd, Spinner RJ, Schroeter TA. Brachial artery compression by the lacertus fibrosus. Clin Orthop Relat Res. 1994; 307: 110-116.