Case Report
True Congenital Cysts of the Pancreas in the Newborn and Infant
Berger S1*, Bartenstein A1 and Schweizer P2
1Department of Pediatric Surgery, University of Bern, Switzerland
2Department of Pediatric Surgery, Eberhard Karls-University, Germany
*Corresponding author: Steffen Berger, Department of Pediatric Surgery, Children´s Hospital, Inselspital, University of Bern, CH-3010 Bern, Switzerland
Published: 05 Oct, 2016
Cite this article as: Berger S, Bartenstein A, Schweizer P.
True Congenital Cysts of the Pancreas
in the Newborn and Infant. Clin Surg.
2016; 1: 1149.
Abstract
Objectives: True congenital pancreatic cysts (CPC) are extremely rare, only 27 cysts were reported so far in children under 3 years of age. With several new cases reported here, conclusions for
diagnostic work up and treatment can be drawn.
Material and Methods: cases with CPC are analyzed retrospectively and reviewed together with
all previously published cases.
Result: Girls were affected by CPC about twice as frequent as boys, cysts were localized more
often in the tail than in the head or body of the pancreas. Unilocular cysts are seen more frequent
than multilocular cysts. Diagnosis can be made by prenatal or postnatal ultrasound. Usually, total
excision of the cyst(s) was performed and prognosis was good in otherwise healthy children.
Conclusion: This rare diagnosis should be considered when cystic lesions appear in routine
antenatal ultrasound. The benign nature of these cysts together with a certain risk for complications
when left in place justifies for a planned surgical approach in the neonate aiming at total excision of
the cyst with preservation of the pancreas. Ultrasound is sufficient for preoperative imaging.
Keywords: Pancreatic cyst; Congenital; Prenatal diagnosis; Pediatric
Introduction
The rareness of true CPC and the fact that it is increasingly detected nowadays by prenatal
ultrasound rather than by gastrointestinal symptoms in the adult requires an update on this disorder
for the obstetrician, pediatric surgeon and pediatric gastroenterologist. True pancreatic cysts may
be congenital or of neoplastic [1,2] or hydatid [3] origin. An epithelial lining of the luminal surface and a lack of inflammatory cells are diagnostic for true CPC which is extremely rare, previously reported in 27 infants (0-3 years). A first description and first successful operation of a congenital developmental pancreatic cyst in an infant dates back to 1895 [4]. In 1959, Miles [5] reviewed 8 cases in infancy, 2 of these however showed no epithelial lining in pathology [Eha, McPherson] and are therefore eliminated from review. Thereafter, 24 live born cases were reported [6-33].
Only 12 of these had a prenatal diagnosis [12,14-18,20-22,24,27,31] made at 21 weeks [27], 24 weeks [21], 26 weeks [31], 27 weeks [17,22], 30 weeks [14 and 26], 32 weeks [15-16], 33 weeks [24] and 36 weeks [18] of gestation.
Solitary cysts were found to have a good prognosis in contrast to polycystic pancreatic
malformation [34] which may be associated with cystic malformation of other organs. Cystic
fibrosis, Beckwith-Wiedemann syndrome. [18 and 35] and Hippel-Lindau disease [11] may be present in patients affected with polycystic pancreas. A syndrome related occurrence of CPC was suspected in Ivemark II syndrome [30].
A retrospective analysis of cases of CPC treated in two German university pediatric surgery
departments (Mainz and Tübingen) over a period of 20 years was made. Four cases of congenital
pancreatic cysts (cases 1-3: Tübingen, case 4: Mainz) with differences in clinical presentation
and diagnostic evaluation were found and are reported in the following. All previously reported
congenital pancreatic cysts in children were reviewed to give an overview of this entity.
Case Presentation 1
A 2 years and 7 month old girl presented with partially bilious vomiting for 10 days and a weight reduction of 450 g. Nocturnal and postprandial abdominal pain was complained of. Blood chemistry was normal. A plain abdominal x-ray showed a duodenal distension with little intraluminal gas beyond the ligament of Treitz. Ultrasound revealed a 3 x 2.5 cm cyst in the body of the pancreas. Intraoperatively, a solitary cyst arising with a vascularized hilus from the body of the pancreas was found. The cyst was resected; it contained proteinaceous fluid that was lipase (80 U/L) and amylase (82 U/L) positive. Histology of the cyst wall showed pancreatic tissue with acini but without Langerhans islets, the luminal surface of cyst was covered by flat epithelium. The postoperative course was uneventful, a control ultrasound at 6 months after the operation was normal.
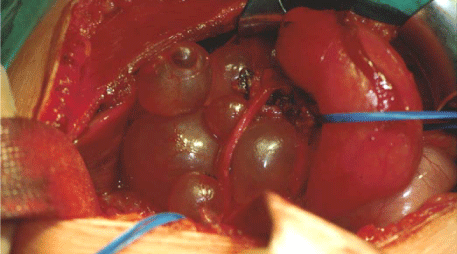
Figure 1, Case 2
Figure 1, Case 2
Intraoperative aspect of polycystic tumor of the pancreatic head with retroduodenal extension, visible after duodenal mobilisation.
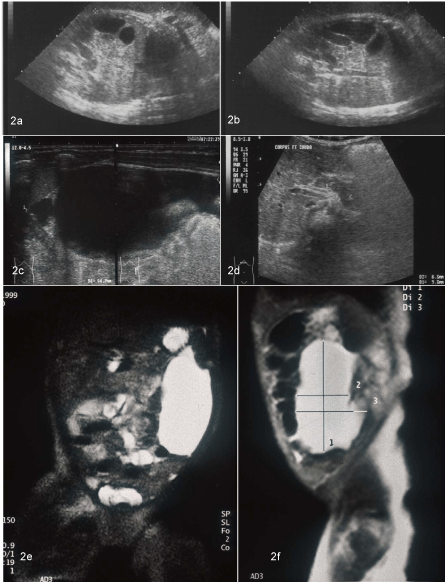
Figure 2_a-f, Case 4
Figure 2_a-f, Case 4
Prenatal ultrasound performed at 33+3 (Figure
2a) and 35+4 weeks (Figure 2b) of gestation, demonstrating rapid growth of
the cystic intra-abdominal lesion (orientation of fetus: caudal left, cranial right,
ventral upside).
2c: Preoperative ultrasound of left abdomen at age 11 days. A small cranial
and a large caudal cyst extend over the entire left half of the abdomen. The
small cyst is close to the pancreas.
2d: Postoperative ultrasound at age 7 months. Cross section of the
epigastrium, showing regular size and texture of the pancreatic body and tail.
2e+f: Preoperative MRI scans of the abdomen at age 6 days. Frontal (Figure
2e) and sagittal plane (Figure 2f). Similar finding as in preoperative ultrasound
with small cranial and large caudal cystic lesion.
Case Presentation 2
An 8 months old boy, normally developed, was referred because of bilious vomiting and food neglect in the past two weeks. A mandarin-sized painful tumor was palpable in the epigastrium. Serum bilirubin (1.8 mg/dL) and serum amylase (120 U/L) were elevated, other blood parameters (lipase, liver enzymes) were within normal range. Ultrasound showed a cystic tumor to the right of the duodenum and a choledochocele was suspected. A multicystic tumor of the head of the pancreas with retroduodenal extension was found intraoperatively (Figure 1). A single tubular connection to the main pancreatic duct was isolated and dissected. The cysts were excised, a resection of the pancreatic head was not performed. Histology showed either thick fibrous or membranous cyst wall partially with typical pancreatic tissue containing acini but no Langerhans islets. The luminal surface was covered by flat cuboidal epithelium. Some spots with few inflammatory cells (lymphocytes, macrocytes) were detected. 6 months postoperatively the child was free of symptoms of pancreatitis or cholestasis, blood chemistry and ultrasound were normal.
Case Presentation 3
A cystic tumor (2 x 2 cm) in the upper left abdomen of a male fetus (32 weeks of gestation) was detected by routine ultrasound. After uncomplicated delivery this finding was confirmed by ultrasound. Blood parameters of the child were normal and the child developed normal for 5 month under close observation. When the child began to vomit increasingly and tolerated less food, the cyst that meanwhile had grown to 3 x 2 cm was operated. A solitary retroduodenal cyst with a hilus to the head of the pancreas was found and resected. The hilus of the cyst contained blood vessels and a narrow duct. The cyst fluid was amylase (15 U/L) and lipase (21 U/L) positive. Histologically, a thin membranous cyst wall was seen with acinar structures and some deformed Langerhans islets. The inner surface was partly covered by flat cuboidal epithelium and partly consisted of connective tissue without epithelium. Besides single lymphocytes, no inflammatory cells were detected. A follow-up ultrasound at 6 month postoperatively was normal.
Case Presentation 4
In a female fetus of 30 wk gestation, a cystic tumor in the abdomen
was diagnosed upon a routine screening ultrasound (Figure 2a,b).
The child was born by vaginal delivery at 37 weeks of gestation with
a weight of 3000 g. The early postnatal period was uneventful and
the child was referred for surgical treatment on day 6 on a full oral
diet and without any abdominal symptoms or irregular laboratory
parameters.
Postnatal ultrasound (Figure 2c) confirmed the MRI finding
(Figure 2e,f) of a 5 x 6 x 4 cm cystic tumor in the left side of the abdomen.
Bilirubin, alcalic phosphatase, liver enzymes, serum amylase and
lipase were within normal range. Preoperative differential diagnosis
included intestinal duplication, a mesenteric cyst, and ovarian cyst,
splenic and pancreatic cyst.
Surgery was performed at the age of 9 days. Intraoperatively,
a large cyst was seen in the left abdomen. Adhesions to the lateral
abdominal wall, the left colonic flexure, the omentum majus, and
splenic hilus were dissected easily. A tight adhesion of the cyst to
the tail of the pancreas was then seen (Figure 3a). This pedicle-like
structure contained the blood vessels supplying the cyst. The hilus of
the cyst was ligated, dissected and the entire cyst and the pedicle were
removed. The remaining pancreas was macroscopically free of cysts.
Histology of this tissue showed parts of exocrine pancreatic tissue
and fibrous tissue containing a vascular pedicle. Histology of the cyst
wall showed a PAS-positive epithelial lining and islets of glandular
tissue with ductal ectasia (Figure 3b,c). The epithelial lining of these
ducts was slightly reactive to antibodies against pancreatic amylase.
The liquid content of the cyst was sterile, free of hemoglobin, and
contained lipase (130 U/l), amylase (3 U/l) and protein (1 g/l). The
corresponding serum concentrations were within normal range
(lipase 19 U/l, amylase < 100 U/l, protein 62 g/l).
The postoperative course was uneventful, a complete recovery
was made. Upon the last follow up at 8 months after the operation,
no residual or recurrence was found. Control ultrasound studies were
without pathologic findings (Figure 2d).
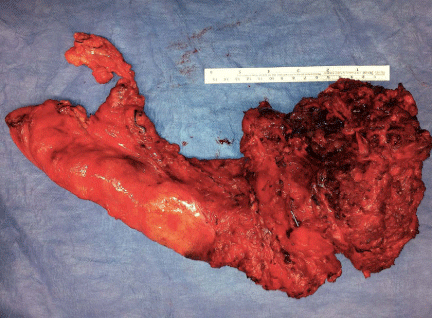
Figure 3, Case 4
Figure 3, Case 4
3a: Intraoperative view of the eventrated cyst with its pedicle to the pancreatic tail. Adhesions to the splenic vessels, colon and abdominal wall were removed.
3b: Pathology specimen of the completely resected cyst.
3c: Microphotograph of cyst wall with Langerhans´ islets, acinar structures and epithelial lining.
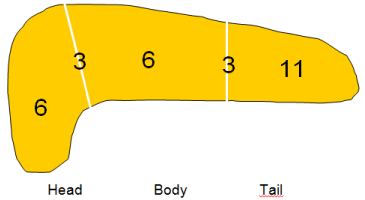
Figure 4
Figure 4
Localisation of congenital pancreatic cysts in 29 cases with known localisation. Cysts were found to arise more frequently from the tail than from the head or body of the pancreas.
Discussion
Pathogenesis
Ectasia of pancreatic ducts has been accused as the major
reason for the formation of intraparenchymal pancreatic cysts.
Since the pancreas exhibits exocrine function already in early fetal
life, pancreatic cysts may appear on ultrasound before 30 weeks of
gestation. Pancreatic pseudocysts may be congenital as well but are
no true cycts since an epithelial lining is missing.
Diagnostic procedures
Pancreatic cysts are a rare cause of a fetal intraabdominal mass
[5], only in recent decades prenatally detectable by ultrasound
[17]. Before the era of prenatal high-resolution sonography most
congenital pancreatic cysts were diagnosed at higher age, usually
when an abdominal mass became palpable or when gastrointestinal
symptoms occurred due to compression of adjacent viscera [36]
during childhood [37], adolescence, or in adult patients [13].
The currently reported cysts were diagnosed at 30 and 32 weeks
of gestation (cases 3,4) or postnatally at 8 and 19 months of age (cases
1,2). Since considerable postnatal growth of congenital pancreatic
cysts has been reported [17], prenatal diagnosis and early operation
may avoid complications due to extrinsic pressure on adjacent organs
as seen in cases 1-3 and in some cases in literature [7,19,32,38]. An
increasing number of prenatally detected pancreatic cysts may be
expected along with the rapid spread of routine prenatal ultrasound.
However, prenatal ultrasound cannot differentiate between pancreatic
cysts and pancreatic pseudocysts, which may also be visible before
birth [39].
For preoperative diagnostic work up, plain abdominal
radiograms, barium x-ray studies, angiography [9], sonography
[17], CT scan [12] and MRI [25,27] were employed so far. Postnatal
MRI scans were reported only occasionally in this condition. For
preoperative topographic evaluation, however, sonography offers
sufficient information with a spatial resolution exceeding that of an
MRI scan in the neonate (for direct comparisons see Figure 2c and
2e). This is confirmed by the other reports of MRI-findings in this
entity, made in 3 days [27], 4 months [25] and 15 months [32] old
infants. Ultrasound may therefore be regarded as the gold standard in
the diagnosis of cystic intraabdominal tumors in the neonate.
Important features of congenital pancreatic cysts
Including the present cases, antenatal diagnosis was made in 14
of 25 children so far since the first description of antenatal diagnosis
by Hopper in 1979. If the diagnosis is not made antenatally, it is
usually delayed for some months, with an average age at diagnosis
(among 11 children of 0-3 years after 1979) of 8.7 months. Among
all children younger than 3 years were 10 boys and 23 girls, the sex
was not indicated in 2. The sex ratio is therefore 1:2.3 with a female
predominance [40]. The localization of the cyst was not specified in 5
cases. In 11 cases the cyst arose from the tail, in 3 cases from tail and
body, in 6 from the body, in 3 from body and head, and in 6 cases
from the head of the pancreas. The tail of the pancreas is thus involved
more frequently than the head or body of the pancreas (Figure 4).
Unilocular cysts (n=24) were seen more frequent than multilocular
cysts (n=8) [12].
The content of pancreatic enzymes of the cyst fluid was described
only in 20 of the cases. A low enzyme concentration was reported in 8,
a high concentration in 6 patients. In 4 cases, no pancreatic enzymes
were detected in the cyst fluid and no data were given in 15 cases.
After 1920, mortality from pancreatic cysts was 0% among
published cases, excluding cases with severe associated malformations
where mortality was high (4 of 5 patients). In otherwise healthy
children, pancreatic cysts thus have an excellent prognosis.
Treatment
Since total resection is the treatment of choice in pancreatic cysts
whenever feasible, all of the currently reported cases were treated by
complete excision. An exception to this rule should only be made
when major damage to the pancreas has to expected as in large cysts
of the pancreatic head. Those conditions should then better be treated
by drainage of the cyst into the duodenum or to a jejunal loop by
a Roux-en-Y procedure (11 cases). In literature however, most cysts
were excised. Treatment by excision (laparotomy) was successful in
all 19 cases where it was employed. Recurrence of a cyst has only been
reported so far in 2 of 2 cases after laparoscopic resection [33].
Table 1
Table 1
Literature overview of congenital true pancreatic cysts in neonates and infants. Cases of children older than 3 years upon diagnosis, numerous cases with manifestation in adulthood and cases of stillborn children with pancreatic cysts are not included. Cysts of heterotrophic pancreatic tissue are not included as well.
Conclusion
It is concluded that CPC will be diagnosed increasingly by routine prenatal ultrasound thus avoiding complications that were seen previously when such cysts were only diagnosed secondary to growth induced compression of adjacent organs. It is assumed from several reported cases [41-43] that cystic intraabdominal tumors may also arise from ectopic pancreatic tissue and show similar histologic features and cyst fluid composition as pancreatic cysts of the pancreas itself. Analysis of the current cases and the findings in literature revealed a female predominance, preferred localization in the pancreatic tail, cuboid epithelial lining of the lumen, and usually low pancreatic enzyme concentration of congenital pancreatic cysts. Early sonographic diagnosis (prenatal diagnosis in 2/3 of cases) of cyst affecting the body and tail of the pancreas should be followed by total excision which yields an excellent prognosis. Results of the first cases of excision by laparoscopy are not satisfying until now. Cysts originating from the pancreatic head sometimes require internal drainage if excision is not feasible.
References
- Grosfeld J, Vane D, Rescorla F, McGuire W, West K. Pancreatic tumors in childhood: analysis of 13 cases. J Pediatr Surg. 1990; 25: 1057-1062.
- Jaksic T, Yaman M, Thorner P, Wesson D, Filler R, Shandling B. A 20-year review of pediatric pancreatic tumors. J Pediatr Surg. 1992; 27: 1315-1317.
- Erdener A, Sahin A, Özcan C. Primary pancreatic hydatid disease in a child: case report and review of the literature. J Pediatr Surg. 1999; 34: 491- 492.
- Richardson M. A case of pancreatic cyst treated by drainage with recovery. Boston Med Surg J. 1895; 132: 280.
- Miles RM. Pancreatic cyst in the newborn. Ann Surg. 1959; 149: 576-581.
- Power WH. Pancreatic cyst in infancy: recovery by marsupialization. Brit Med J. 1961; 2: 625-626.
- Pilot LM, Gooselaw JG, Isaacson PG. Obstruction of the common bile duct in the newborn by a pancreatic cyst. Lancet. 1964; 84: 204-205.
- Siafarikas C, Dennhardt D. Ein Beitrag zum congenitalen Cystenpancreas. Z Kinderchir. 1971; 9: 381-386.
- Mares AJ, Hirsch M. Congenital cysts of the head of the pancreas. J Pediatr Surg. 1977; 12: 547-552.
- Hollingworth P, Isaacs D, Bydder G. Recurrent osteolytic lesions and subcutaneous fat necrosis in association with a developmental pancreatic cyst. Arch Dis Child. 1979; 54: 790-792.
- Welch K. The pancreas. In: Welch K, Randolph J, Ravitch M, editors. Pediatric Surgery. Chicago: Year Book Medical. 1986; 1091-1095.
- Auringer ST, Ulmer JL, Sumner TE, Turner CS. Congenital cyst of the pancreas. J Pediatr Surg. 1993; 28: 1570-1571.
- Casadei R, Campione O, Greco VM, Marrano D. Congenital true pancreatic cysts in young adults: case report and literature review. Pancreas. 1996; 12: 419-421.
- Daher P, Diab N, Melki I, Abi Aad G, Korkmaz G. Congenital cyst of the pancreas. Antenatal diagnosis. Eur J Pediatr Surg. 1996; 6: 180-182.
- Hopper MS, Boultbee JE, Watson AR. Polyhydramnios associated with congenital pancreatic cysts and asphyxiating thoracic dysplasia. A Case Report. S Afr Med J. 1979; 56: 32-33.
- Fleet M, Milne D, Scott J. Congenital cyst of the pancreas in a newborn. Pediatr Surg Int. 1993; 8: 149-150.
- Baker LL, Hartman GE, Northway WH. Sonographic detection of congenital pancreatic cysts in the newborn: report of a case and review of the literature. Pediatr Radiol. 1990; 20: 488-490.
- Fremond B, Poulain P, Odent S, Milon J, Treguier C, Babut JM. Prenatal detection of a congenital pancreatic cyst and Beckwith-Wiedemann syndrome. Prenat Diagn. 1997; 17: 276-280.
- Shieh CS, Eng HL, Huang SC, Chuang JH. Congenital pancreatic cyst presenting as acute pancreatitis in an adolescent. J Pediatr Gastroenterol Nutr. 1994; 18: 490-493.
- Maiullari E, Vinardi S, Magro P, Gamba S, Sacco Casamassima MG, Canavese F. [Congenital cysts of the pancreas. A case report]. Minerva Pediatr. 2000; 52: 143-146.
- Kebapci M, Aslan O, Kaya T, Ilhan H. Prenatal diagnosis of giant pancreatic cyst of a neonate. AJR Am J Roentgenol. 2000; 175: 1408-1410.
- Sepulveda W, Carstens E, Sanchez J, Gutierrez J. Prenatal diagnosis of congenital pancreatic cyst: case report and review of the literature. J Ultrasound Med. 2000; 19: 349-352.
- Boulanger S, Borowitz D, Fisher J, Brisseau G. Congenital pancreatic cysts in children. J Pediatr Surg. 2003; 38: 1080-1082.
- Liao YY, Chen HC, Chou CM, Lin YM. Antenatal detection of congenital pancreatic cyst. J Formos Med Assoc. 2003; 102: 273-276.
- Kazez A, Akpolat N, Kocakoc E, Parmaksiz M, Köseogullari A. Congenital true pancreatic cyst. Diagn Interv Radiol. 2006; 12: 31-33.
- Choi SJ, Kang MC, Kim YH, Lim JS, Lim SC, Chang JH. Prenatal detection of a congenital pancreatic cyst by ultrasound. J Korean Med Sci. 2007; 22: 156-158.
- Chung JH, Lim G, Song YT. Congenital true pancreatic cyst detected prenatally in neonate: a case report. J Pediatr Surg. 2007; 42: E27-E9.
- Ishimaru T, Uchida H, Yotsumoto K, Gotoh C, Yoshida M, Oguma E, et al. Recurrence of a congenital pancreatic cyst mimicking omental cyst after laparoscopic cyst resection. Eur J Pediatr Surg. 2009; 19: 53-54.
- Castellani C, Zeder SL, Spuller E, Hollwarth ME. Neonatal congenital pancreatic cyst: diagnosis and management. J Pediatr Surg. 2009; 44: e1-4.
- Chahed J, Mekki M, Aloui S, Hidouri S, Ksia A, Krichene I, et al. Congenital pancreatic cyst with Ivemark II syndrome: a rare case. J Pediatr Surg. 2012; 47: e33-6.
- Gerscovitch E, Jacoby B, Field N, Sanchez T, Woottoon-Gorges S, Saroufeem R. Fetal true congenital cyst. J Ultrasound Med. 2012; 31: 809- 815.
- Al-Salem AH, Matta H. Congenital pancreatic cyst: diagnosis and management. J Pediatr Gastroenterol Nutr. 2014; 59: e38-40.
- Warnock W, Khoshnam N, Bird KM, Schaffer LR, Lou LH, Hawkins CM, et al. Congenital cyst of the pancreas: a case report and review of the literature. Fetal Pediatr Pathol. 2016; 35: 265-271.
- Reiher P, Matthies S. On congenital pancreatic cyst. 1966; 91: 1407-1412.
- Wockel W, Scheibner K, Lageman A. A variant of the Wiedemann- Beckwith syndrome. Eur J Pediatr. 1981; 135: 319-324.
- Rosato FE, Mackie JA. Pancreatic cysts and pseudocysts. Arch Surg. 1963; 86: 551-556.
- Nartowicz A, Nowicka C, Piotrowski M, Kasprzak S. [Giant congenital pancreatic cyst in a 16-month-old boy]. Wiad Lek. 1975; 28: 1225-1226.
- Wolloch Y, Chaimoff C, Lubin E, Dintsman M. Splenic vein thrombosis, segmental portal hypertension and bleeding esophageal varices produced by a congenital pancreatic cyst. Isr J Med Sci. 1974; 10: 670-673.
- Kurrer MO, Ternberg JL, Langer JC. Congenital pancreatic pseudocyst. J Pediatr Surg. 1996; 31: 1581-1583.
- Johnson P, Spitz L. Cysts and tumors of the pancreas. Semin Pediatr Surg. 2000; 9: 209-215.
- Allman D, Lynch B, Edson M. Intrarenal pancreatic cyst. Urology. 1991; 38: 82-83.
- Rattan K, Garg P, Jain R. Neonatal ectopic pancreatic cyst. Indian J Gastroenterol. 2001; 20: 38.
- Bethel C, Luquette M, Besner G. Cystic degeneration of heterotopic pancreas. Pediatr Surg Int. 1998; 13: 428-430.
- Railton T. A case of pancreatic cyst in an infant. Brit Med J. 1896; 2: 1318- 1319.
- Telling W, Maxwell H, Dobson J. Pancreatic cyst in an infant. Brit J Child Dis. 1909; 6: 202.
- Connolly D. Note on a case of pancreatic cyst in a child aged 14 months. Lancet. 1911; 1: 803.
- Friedenwald J, Cullen T. Pancreatic cysts, with the report of seven cases. Am J Med Sci. 1926; 172: 313-334.
- deLange C, Janssen TA. Large solitary pancreatic cyst and other developmental errors in a premature child. Am J Dis Child. 1948; 75: 587- 594.