Review Article
Management of Overwhelming Postsplenectomy Infection Syndrome
Naoki Hashimoto*
Kindai University School of Medicine, Japan
*Corresponding author: Naoki Hashimoto, Kindai University School of Medicine, 377-2 Ohno- Higashi Osaka-Sayama, Osaka 589- 8511, Japan
Published: 05 Oct, 2016
Cite this article as: Hashimoto N. Management of
Overwhelming Postsplenectomy
Infection Syndrome. Clin Surg. 2016;
1: 1148.
Abstract
Overwhelming postsplenectomy infection (OPSI) is a rare medical emergency, mainly caused by
encapsulated bacteria, shortly progressing from a mild flulike syndrome to a fulminant, potentially
fatal, sepsis. The risk of OPSI is higher in children and in patients with underlying benign or
malignant hematological disorders. The identification of Howell-Jolly bodies on peripheral blood
examination is an important clue to the diagnosis of asplenia or hyposplenia. Management of these
patients includes a combination of immunization, antibiotics prophylaxis. Patient’s education about
long-term risk of OPSI and physician’s awareness of a potentially lethal medical emergency are
important factor for preventing and management of OPSI.
Keywords: OPSI; Howell-Jolly body; Encapsulated bacteria; Vaccines
Introduction
Asplenic individuals can have major difficulties in dealing with specific infections where the spleen would normally play a prominent role in protection. The spleen is able to filter encapsulated bacteria such as streptococcus pneumoniae once blood stream invasion has occurred [1]. Splenectomized patients are a significant infection risk, because such surgery removes the splenic macrophages that filter and phagocytose bacteria and other blood borne pathogens. Overwhelming post-splenectomy infection (OPSI) is usually caused by the encapsulated bacteria Streptococcus pneumoniae, Haemophilus influenza and Neisseria meningitides and more than half of those infected die. King and Shumacker first described bacterial sepsis following splenectomy in infants and children in 1952 [2]. The disease may begin as a minor flu-like illness that rapidly escalates into a fulminant infection [3]. The clinical course may rapidly progress to coma and death within 24 to 48h, due to the high incidence of shock, hypoglycemia, marked acidosis, electrolyte abnormalities, respiratory distress, and disseminated intravascular coagulation (DIC). OPSI, a rare clinical infectious syndrome, affecting about 3% of splenectomized patients, is most common in the first two years after splenectomy but may occur decade’s later [4]. The mortality rate is 50%-70% despite aggressive therapy [5].
Risk Factors
Bisharar et al. [6] reviewed all 78 studies published between 1966 and 1996. Twenty eight contained data relating to incidence, morbidity, and mortality and the effects of infection in different age groups. In 19680 splenectomized patients, 3.2% developed invasive infection, and the overall mortality was 1.4%. The mean interval between splenectomy and infection was 22.6 months. The incidence of infection was higher for patients with thalassemia major (8.2%) and sick cell anemia (7.3%) than for patients with idiopathic thrombocytopenia (2.1%), and higher in children with thalassemia major (11.6%) and sick cell anemia (8.9%) than in adults with the same diseases (7.4% and 6.4% respectively). Infants do not acquire specific antibodies against encapsulated organisms until relatively late in the development of antibody response. Therefore, the major risk factors for OPSI in asplenic patients are younger age, underlying diseases (hematological disorder, thalassemia, hereditary spherocytosis, autoimmune hemolysis, immune thrombocytopenic purpura, or lymphoma), previous and concomitant immunosuppression.
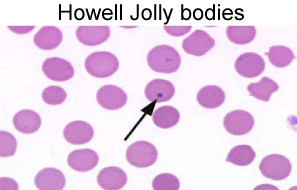
Figure 1
Figure 1
The presence of Howell-Jolly bodies (arrow) on the peripheral blood smear is suggestive of asplenia or hyposplenism.
Detection of Patients at Risk
Nonsurgical and surgical asplenia predisposes to fatal infections. Therefore, simple, non-invasive and repeatable tests for assessing splenic function are required. Howell-Jolly bodies (Figure1) [7,8] are the most characteristic peripheral blood abnormality after splenectomy. Peripheral smear findings in patients with a dysfunctional spleen include the presence of Howell-Jolly bodies. Howell-Jolly bodies are small, intra-erythrocytic remnants of erythrocyte nuclei. These inclusions are solitary in each erythrocyte and strongly basophilic. A normally functioning spleen removes the remnants from erythrocytes, so their presence is important clue to the diagnosis of asplenia or functional hyposplenism. Howell-Jolly bodies may not occur with mild hyposplenism, but their presence is thought to identify the degree of hyposplenism that represents a risk for OPSI. Other, rarer causes of Howell-Jolly bodies include myelodysplasia and hemolysis. One reference laboratory processing more than 100000 peripheral blood smears per year reported an incidence of new patients showing Howell-Jolly bodies of 1 per 200 or 0.5% [9]. The presence of the Howell-Jolly bodies has historically been associated with diminished splenic function. However, Howell-Jolly bodies have been shown not to correlate with blood clearance of the 99mTc-labelled, heat-altered erythorocytes [10]. However, measuring the percentage of Howell-Jolly bodies via flow cytometry is a potentially more reliable parameter as large amounts of erythorocytes can be screened [11]. Measuring the percentages of both Howell-Jolly bodies by flow cytometry as well as argyrophilic inclusion-positive erythrocytes does not require special requirement. Both methods require expensive. More studies evaluating the value of new markers are needed. IgM memory B cells are potentially promising method to measure splenic function [12].
Managements of Patients at Risk
Preventive strategies including vaccination and education are also important for splenectomized patients. Functionally or anatomically asplenic patients are at increased risk of infection from encapsulated organisms compared to the general population. Vaccines available for the most common organisms include the 23-valent pnemococcal polysaccharide vaccine; a 7-valent protein conjugated pneumococcal vaccine, the hemophilus influenza type B vaccine, and the meningococcal vaccine [13]. Jockvich et al. [14] reported no OPSI among patients vaccinated before splenectomy; however, 10.4% of patients who did not receive vaccination developed OPSI. 5 % of patients who were taken vaccination after splenectomy developed OPSI. Therefore, pneumococcal vaccination should be performed at least two weeks before an elective splenectomy because the vaccine’s immunogenicity may be reduced when given after splenectomy. Unimmunized patients who have had a splenectomy or functional hyposplenism should be taken vaccination as soon as their conditions are identified. In asplenic patients or patients with functional hyposplenism who are older than 10 years, revaccination is recommended every five years or sooner if antibody titers may have declined. For children 10 years or younger, revaccination is recommended after three years [15]. Recent guidelines have suggested administering haemophilus b conjugate, meningococcal vaccines as well as the pneumococcal vaccine, to all asplenic or functionally hyposplenic persons. Unfortunately, sporadic cases of pneumococcal and other vaccine failures have been reported in appropriately immunized, some of whom had also been taking prophylactic antibiotics. Besides vaccination, patients who have lost their spleens or have functional hyposplenism must be made aware of the possibility of OPSI. All such persons should have medical alert, such as a card or a bracelet. These medical alerts have two purposes. First, it should provide a constant reminder to the individual of their condition and, second, knowledge of their state might be vital for medical attendants in the event of a medical emergency.
Antibiotics
Most authorities recommend antibiotics prophylaxis for asplenic or hyposplenic children, especially for the first two years after splenectomy [16]. Some investigators also advocate continuing chemoprophylaxis in children for at least five years or even until they reach age 21 [17]. Because commonly used prophylactic antibiotics agents caused the increasing resistance of pneumococci, it is now recommended that chemoprophylaxis in adults should be limited to a supply of standby antibiotics. Traditional prophylactic use of penicillin and amoxicillin has given way to the use of antibiotics with a broader spectrum of activity.
Education
About 50% of asplenic patients are unaware of their increased risk for serious infection or of the health precautions that they should undertake [18]. MS EL-Alfy’s study [19] clearly shows that the quality of knowledge in splenectomized patients has a great bearing on the risk of life-threatening sepsis. Patients displaying greatest knowledge had a prevalence of OPSI of 1.4% compared to 16.5% among those with poor knowledge. Good knowledge has remarkably reduced OPSI.
Conclusion
Although the introduction of an adequate vaccination program against encapsulated bacteria and systematically oral penicillin prophylaxis have decreased the overall risk of OPSI, its mortality rate remain high, ranging from 50% to 70% within 48h. OPSI is a serious medical emergency requiring immediate therapeutic administration of antimicrobial agents and aggressive care support according to the guidelines for management of sever sepsis and septic shock. Observational evidence have documented that early aggressive antimicrobial therapy combined with intensive care support may decrease the mortality rate for OPSI as low as 10%.
References
- Jenks PJ, Jones E. Infections in asplenic patients. Clin Microbiol Infect. 1996; 1: 266-272.
- King H, Shumacker HB Jr. Splenic studies: I. Susceptibility to infection after splenectomy performed in infancy. Ann Surg. 1952; 136: 239-242.
- Cullingford GL, Watkins DN, Watta AD, Mallon DF. Sever late postsplenectomy infection. Br J Surg. 1991; 78: 716-721.
- Evans DI. Postsplenectomy sepsis 10 years or more after operation. J Clin Pathol. 1985; 38: 309-311.
- Long SG, Smith AG, Perry BA, Leyland MJ, Milligan DW. Implementing a policy for pneumococcal prophylaxis in a haematology unit after splenectomy. Qual Health Care. 1995; 4: 194-196./a>
- Bisharat N, Omari H, Lavi I, Raz R. Risk of infection and death among post-splenectomy patients. J Infect. 2001; 43: 182-186.
- Brigden M, Pattullo AL. Prevention and management of overwhelming postsplenectomy infection: an update. Crit Care Med. 1999; 27: 836-842
- Styrt B. Infection associated with asplenia: risks, mechanisms, and prevention. Am J Med. 1990; 88: 33-42N.
- Brigden ML, Preece E. Preventing postsplenectomy sepsis (Letter). Can Med Assoc J. 1984; 130: 334.
- Robertson DA, Bullen AW, Hall R, Losowsky MS. Blood film appearances in the hyposplenism of coeliac disease. Br J Clin Pract. 1983; 37: 19-22.
- Harrod VL, Howard TA, Zimmerman SA, Dertinger SD, Ware RE. Quantitative analysis of Howell-Jolly bodies in children with sickle cell disease. Exp Hematol. 2007; 35: 179-183.
- Di Sabatino A, Rosado MM, Ciccocioppo R, Cazzola P, Morera R, Corazza GR, et al. Depletion of immunoglobulin M memory B cells is associated with splenic hypofunction in inflammatory bowel disease. Am J Gastroenterol. 2005; 100: 1788-1795.
- Shatz DV. Vaccination considerations in the asplenic patient. Expert Rev Vaccines. 2005; 4: 27-34.
- Jockovich M, Mendenhall NP, Sombeck MD, Talbert JL, Copeland EM, Bland KI. Long-term complications of laparotomy in Hodgkin’s disease. Ann Surg. 1994; 219: 615-621.
- Advisory Committee on Immunization Practices (ACIP). Prevention of pneumococcal disease. MMWR Morb Mortal Wkly Rep. 1997; 46: 1-24.
- Styrt B. Infection associated with apslenia: Risks, mechanisms, and prevention. Am J Med. 1990; 88: 33N-42N./a>
- Stryker RM, Orton DW. Overwhelming postsplenectomy infection. Ann Emerg Med. 1988; 17: 161-164.
- White KS, Covington D, Churchill P, Maxwell JG, Norman KS, Clancy TV. Patient awareness of health precautions after splenectomy. Am J Infect Control. 1991; 19: 36-41.
- EL-Alfy MS, El-Sayed MH. Overwhelming postsplenectomy infection: is quality of patient knowledge enough for prevention. The Hematology Journal. 2004; 5: 77-80.