Case Report
Atypical Shard “Bullet” Penetrating the Chest
Guiducci GM1*, Kawamukai K1, Salomone Di Saverio2, Anna M. Parisi1, Leuzzi G3, Sergio N. Forti Parri1 and Tugnoli G2
1Thoracic Surgery Unit, Maggiore and Bellaria Hospitals, Italy
2Emergency Surgery and Trauma Surgery Unit, Trauma Center, Maggiore Hospital, Italy
3Department of Surgical Oncology, Thoracic Surgery Unit, Regina Elena National Cancer Institute, Italy
*Corresponding author: Gian Marco Guiducci, Thoracic Surgery Unit, Maggiore and Bellaria Hospitals, Ospedale Maggiore, Largo Nigrisoli 2, Bologna, Italy
Published: 21 Sep, 2016
Cite this article as: Guiducci GM, Kawamukai K, Di Saverio
S, Parisi AM, Leuzzi G, Sergio N.
Atypical Shard “Bullet” Penetrating the
Chest. Clin Surg. 2016; 1: 1134.
Abstract
A case of a 47-year-old male with a chest wall wound is reported. An accurate understanding of the
events was unobtainable from the patient because he was born deaf-mute. The initial suspect of a
limited superficial injury, suggested by the absence of major clinical consequences, was contradicted
by a subsequent CT scan that revealed a retained metallic foreign body within the chest. The right
lung was deeply injured but fortunately without major hemorrhage, although the shard was very
close to the superior vena cava. Right thoracotomy was performed and the atypical “bullet” was
removed without complications.
Keywords: Trauma; Trauma penetrating; Hemothorax; Pleural space
Case Presentation
A 47 years old Caucasian male was referred to Emergency Department (ED) after being
accidentally injured in the right hemi-thorax while handling an angle grinder. Since the patient was
born deaf and dumb, it was not possible to completely understand the exact mechanism of trauma.
At the time of ED acceptance, the patient was clinically and hemodynamically stable (blood
pressure 130/70, heart rate 105 bpm, and respiratory rate 20 per minute). Physical chest examination
showed a 4 cm non-linear laceration of the right anterior chest at para-sternal level, but no retained
objects were visible from the injured skin.
For these reasons the presence of a retained metal fragment was not initially suspected by
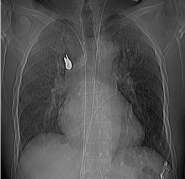
the ED physicians and the patient underwent further standard imaging. Chest X-Ray (Figure 1)
and subsequent CT scan (Figure 2, 3a and b) documented a metallic blade-shaped object deeply
penetrating pulmonary parenchyma, whose inner end was very close to the superior vena cava. A
moderate hemopneumothorax was also evident.
The patient was promptly taken to Operatory Room (OR) and underwent double-lumen
intubation and right postero-lateral thoracotomy. The metallic shard was removed without major
consequences (Figure 4a and b) and the upper pulmonary lobe was primarily sutured. Antibiotic
therapy was early administered and post operative course was substantially uneventful.
Figure 1
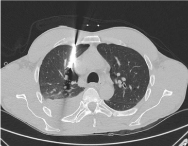
Figure 2
Figure 2
Chest CT showing the metal shard penetrating the superior lobe of
right lung and resting in close proximity of the superior vena cava.
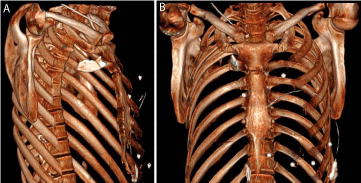
Figure 3a and 3b
Figure 3a and 3b
CT based 3D reconstruction of the rib cage and the location and penetration site of the metal shard right to the sternal manubrium.
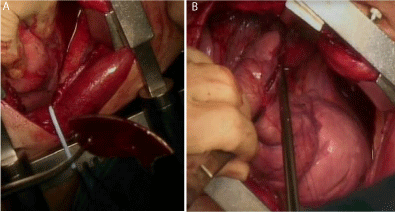
Figure 4a and 4b
Figure 4a and 4b
Surgical field view of the extraction of the metal shard and of the lung laceration suture.
Discussion
Clinical history and physical examination play a cornerstone role
in early work-up planning of traumatic injuries. They are essential
steps to figure out the correct mechanism of trauma and to guide
further diagnostic and treatment steps [1-2].
In this case all vitals were normal and no major symptoms, besides
a moderate chest pain, were reported by the patient. Moreover, it
was basically impossible to collect an accurate clinical history, since
the patient was deaf-mute and no relatives were present at the time
of ED admission. All these circumstances prevented immediate
and thorough understanding of the cause of trauma. A penetrating
metallic fragment was discovered only when the patient underwent
imaging.
In a non-military urban scenery, the most likely cause of
penetrating chest trauma is knife stabbing [1]. The early diagnostic
suspect of ED physicians was oriented towards a superficial chest wall
injury since the wound was compatible with a knife stabbing without
a retained blade. Surprisingly, CT scan showed a retained metallic
foreign body not otherwise clinically detectable.
The absence of haemodynamically symptomatic bleeding allowed
the operators to surgically manage the patient with a semi-elective
procedure: after obtaining pulmonary exclusion, a standard posterolateral
thoracotomy was performed, the metallic shard was removed
without any major vascular damage and the superior upper lobe of
the right lung was subsequently sutured, as it was the only injury.
In other cases, described in the literature, the retention of knives
or other penetrating foreign bodies can provide a momentarily
deceptive haemostasis with a tamponade of the great vessel
lacerations. Inaccurate or unintentional removal of the knife can lead
to a catastrophic hemorrhage [3].
Several Authors advocate Video Assisted Thoracoscopy (VATS)
as the approach of choice for thoracic trauma when haemodynamics
is permissive [4-6]. We were tempted for a mini-invasive approach,
but the potential for major bleeding during extraction led us to prefer
an open standard procedure.
Further late complications can be the consequences of concealed
foreign bodies migration, contamination and consequent infection of
the pleural cavity [7].
When managing penetrating wounds, ED physicians should
always consider the possibility of retained foreign bodies despite
clinical history and physical examination may apparently exclude
such occurrence. Prompt imaging [2] is mandatory in order to avoid
early and late complications.
References
- Bège T, Berdah SV, Brunet C. Stab wounds in emergency department. Presse Med. 2013; 42: 1572-1578.
- Kavanagh PV, Mason AC, Müller NL. Thoracic foreign bodies in adults. Clin Radiol. 1999; 54: 353-360.
- Sobnach S, Nicol A, Nathire H, Kahn D, Navsaria P. Management of the retained knife blade. World J Surg. 2010; 34: 1648-1652.
- Ben-Nun A, Michael Orlovsky M, Anson Best L. Video-Assisted Thoracoscopic Surgery in the Treatment of Chest Trauma: Long-Term Benefit. Ann Thorac Surg. 2007; 83: 383–387.
- Ahmeda N, Jones D. Video-assisted thoracic surgery: state of the art in trauma care. Injury. 2004; 35: 479-489.
- Williams CG, Haut ER, Ouyang H, Riall TS, Makary M, Efron DT, et al. Video-assisted thoracic surgery removal of foreign bodies after penetrating chest trauma. J Am Coll Surg. 2006; 202: 848-852.
- Petersen K, Waterman P. Prophylaxis and treatment of infections associated with penetrating traumatic injury. Expert Rev Anti Infect Ther. 2011; 9: 81-96.