Case Report
Value of the Robotic Platform in a Complex Cholecystectomy: A Case Report
Esposito S*, Daskalaki D, Gonzalez-Ciccarelli LF and Giulianotti PC
Department of Surgery, Division of General, Minimally Invasive, and Robotic Surgery, University of Illinois Hospital
and Health Sciences System, USA
*Corresponding author: Sofia Esposito, Department of Surgery, Division of General, Minimally Invasive, and Robotic Surgery, University of Illinois Hospital and Health Sciences System, 840 S Wood St. MC 958, Chicago, IL 60612, USA
Published: 20 Sep, 2016
Cite this article as: Esposito S, Daskalaki D, Gonzalez-
Ciccarelli LF, Giulianotti PC. Value of
the Robotic Platform in a Complex
Cholecystectomy: A Case Report. Clin
Surg. 2016; 1: 1129.
Abstract
Introduction: Conversion rates for Laparoscopic Cholecystectomy (LC) still range from 1.9% to 15 % and are higher when it comes to acute cholecystitis. Preoperative risk factors for conversion
to open (CTO) technique are: previous upper abdominal surgery, male gender, age over 65, high
BMI and history of acute cholecystitis treated conservatively. Besides that, the reported incidence of
iatrogenic bile duct injuries varies between 0, 1% and 0, 5%.
Case Presentation: 67-year-old male with a history of previous laparoscopic distal splenopancreatectomy
complicated by severe pancreatitis, infected pseudocyst and colonic fistula.
During this complex postoperative course he also developed acute cholecystitis with suspicion of
rupture and pericholecystic abscess treated with a cholecystostomy tube. Months later, still with the
cholecystostomy in place, we performed a robotic cholecystectomy, without intra- or post-operative
complications.
Conclusion: The intrinsic advantages of the robotic platform and the use of Indocyanine green
fluorescent cholangiography (ICG) could make dissection and identification of anatomy easier, thus
possibly reducing the rates of CTO and biliary tract injuries. Robotic assisted surgery could be an
option for complex cases of cholecystectomy. ICG is an additional tool that can help identify the
cystic and common bile duct during the dissection of the Calot’s triangle.
Introduction
Laparoscopic cholecystectomy (LC) is the gold standard treatment for gallstone disease and
is one of the most frequently performed procedures in general surgery. Conversion rates are still
reported ranging from 1.9% to 15% [1,2] and they appear to be higher when considering acute
cholecystitis [3,4]. Several studies [3,5,6] investigated preoperative risk factors related to conversion
to open technique (CTO), among these, the most commonly accepted are: previous upper abdominal
surgery, male gender, age over 65, high BMI and history of acute cholecystitis treated conservatively
[3,5].
In a recently published study, Goonawardena et al. [7] reported that in 70% of the cases the
decision to convert from laparoscopic to open procedure was due to difficult interpretation of
anatomy because of inflammation and adhesions that made the dissection of the Calot’s triangle
challenging. Other common reasons of CTO are: open fistula to gastrointestinal tract or bowel
injury, gangrenous cholecystitis, uncontrollable intraoperative bleeding and atypical anatomy [7].
The reported incidence of iatrogenic bile duct injuries varies between 0, 1% and 0, 5% [8,9].
They represent the most feared complication of cholecystectomy and are associated with prolonged
hospitalization, high morbidity, recurrent complications and can often require the patient to be
referred to a tertiary center with a skilled hepatobiliary surgeon [8,10].
Several studies compared laparoscopic and robotic assisted cholecystectomy (RAC) [11,12].
Although comparable in terms of surgical outcomes and safety, some authors still find the costs
of the daVinci surgical system prohibitive [11]. The robotic platform with its intrinsic advantages
such as the endowristed instruments with 7 degrees of freedom and 3D vision, associated with
indocyanine green fluorescent cholangiography (ICG) could be a powerful tool that can justify its
role especially in challenging cholecystectomies.
We hereby report the case of a difficult cholecystectomy entirely performed in a minimally
invasive fashion with the robotic platform.
Figure 1
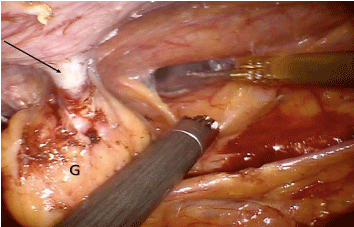
Figure 1
Intraoperative picture showing massive adhesions sectioned with
the Robotic Cautery Hook and the Cadiere forceps. The arrow points the
cholecystostomy tube. G: Gallbladder.
Figure 2
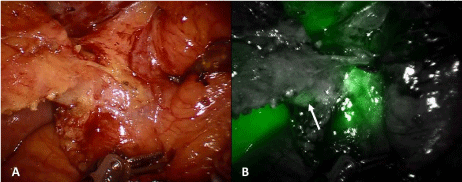
Figure 2
ICG evaluating the anatomy of the cystic duct. (A: White light, B:
Near-infraredfluorescence ICG). The arrow points the cystic duct.
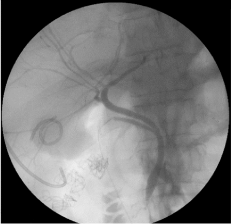
Figure 3
Case Presentation
We present the case of a 67-year-old male that was referred to us
for possible cholecystectomy. The patient underwent a laparoscopic
distal spleno-pancreatectomy in July 2014, complicated by severe
pancreatitis, infected pseudocyst and colonic fistula. He was treated
for several months in a conservative manner with multiple abdominal
drain placements and antibiotic therapy. During his postoperative
course he also developed acute cholecystitis with suspicion of rupture
and pericholecystic abscess. At that time, in consideration of the
complex clinical picture, only a cholecystostomy tube was inserted to
drain the gallbladder.
When he presented to us in December 2014, the cholecystostomy
drain had been in place for 3 months with a major impact on the
patient’s quality of life. He had consulted several other doctors that,
in the light of the hostile abdominal setting, were reluctant to perform
surgery. We offered the option of a minimally invasive, robotic
approach. A cholangiogram performed prior to surgery did not show
any signs of obstruction in either the cystic duct or the common bile
duct.
Intraoperatively, the procedure started with a diagnostic
laparoscopy. The ports were placed under direct vision and the
robotic system was docked, coming from the patient’s head. The
procedure started with careful adhesiolysis, detaching the omental
and colonic adhesions (Figure 1). ICG was used in order to identify
the cystic and common bile duct (Figure 2). The cystic duct was long
and dilated. The cystic artery was clipped, allowing better control
of the cystic duct. A Fogarty catheter (#4) was inserted in the cystic
duct in order to clear the sludge. An intraoperative cholangiogram
was negative for filling defects (Figure 3). The cystic duct was clipped
and the gallbladder was detached from the liver bed. No drains were
placed. The operative time was 100 minutes, including docking time. The postoperative course was uneventful and the patient was
discharged on postoperative day 2.
Discussion
When faced with complex inflammation, with multiple adhesions
that hinder a clear visualization of the anatomy, LC can be associated
with higher rates of CTO [7]. This occurrence has proven to lead to
increased overall morbidity, longer hospital stay, increased surgical
site infection, increased reoperation rate and mortality [5].
Placement of a percutaneous cholecystostomy tube is considered
a relatively safe option in critically ill patients presenting with acute
cholecystitis [13-14]. Whether or not this procedure is associated
with higher conversion rates when laparoscopic cholecystectomy is
performed is still debated [15-17].
Our patient presented with several other risk factors for
conversion: previous complicated upper abdominal surgery, male
gender, age over 65 and previous episode of acute cholecystitis [7].
Nevertheless, with the assistance of the robotic platform, we were able
to perform a difficult cholecystectomy in a minimally invasive way,
without the need to convert and without any intra- or postoperative
complications.
We performed an intraoperative cholangiogram (IOCG)
to rule out the presence of common bile duct stones and ICG
cholangiography to help us visualize and confirm the biliary anatomy.
Routine performance of IOCG to avoid biliary tract injuries is still
controversial. Several studies stated that it could have a protective
effect [18], while others believe that the association is non-causal
and the procedure only lengthens operative time [19-20]. We
believe that IOCG should be reserved in cases with suspicion of
choledocholithiasis and should not be performed routinely, since
it is a time consuming procedure, with long learning curve and
exposes the patient to radiations. In our department ICG has become
standard practice; in a previously published study, were ported that
ICG is a safe and effective procedure that can help identify at least one
biliary structure in 99% of the cases, including emergency procedures
for acute or gangrenous cholecystitis [21]. Fluorescence has minimal
risks for the patient and doesn’t significantly prolong operative time
[22].
One of the major criticism leveled at the daVinci surgical system is
about costs, especially regarding its use in general surgery procedures
that are commonly performed laparoscopically [23,24]. Several
studies have already stated that RAC is more expensive than LC [11],
even though we witnessed a reduction in costs in recent years [12]. In
a recently published study, Bedeir et al. [25] Compared robotic single
site cholecystectomy to conventional LC and found that the robotic
approach was actually cheaper. The robotic system is definitely an
expensive technique, but we believe that it can undoubtedly justify
its role in difficult procedures that have high risk of conversion to
open and of iatrogenic injury. These eventualities could result in
reoperation and prolonged hospital stay, thus incrementing costs and
distress for the patient. In our case, hospital stay was 1, 5 days.
Conclusion
Robotic assisted surgery may be an option for complex cases of cholecystectomy. ICG is an additional tool that can help identify the cystic and common bile duct during the dissection of the Calot’s triangle. The IOCG should be reserved for cases where there is a doubt of choledocholithiasis. The intrinsic advantages of the robotic technology, combined with the fluorescence scanning can offer a substantial advantage in the more challenging cases of cholecystectomy, thus possibly reducing conversion to open and iatrogenic bile duct injury rates.
References
- Kaafarani HM, Smith TS, Neumayer L, Berger DH, Depalma RG, Itani KM. Trends, outcomes, and predictors of open and conversion to open cholecystectomy in Veterans Health Administration hospitals. Am J Surg. 2010; 200: 32-40.
- Simopoulos C, Botaitis S, Polychronidis A, Tripsianis G, Karayiannakis AJ. Risk factors for conversion of laparoscopic cholecystectomy to open cholecystectomy. Surg Endosc. 2005; 19: 905-909.
- Philip Rothman J, Burcharth J, Pommergaard HC, Viereck S, Rosenberg J. Preoperative Risk Factors for Conversion of Laparoscopic Cholecystectomy to Open Surgery - A Systematic Review and Meta- Analysis of Observational Studies. Dig Surg. 2016; 33: 414-423.
- Licciardello A, Arena M, Nicosia A, Di Stefano B, Cali G, Arena G, et al. Preoperative risk factors for conversion from laparoscopic to open cholecystectomy. Eur Rev Med Pharmacol Sci. 2014; 18: 60-68.
- Sippey M, Grzybowski M, Manwaring ML, Kasten KR, Chapman WH, Pofahl WE, et al. Acute cholecystitis: risk factors for conversion to an open procedure. J Surg Res. 2015; 199: 357-361.
- Lee NW, Collins J, Britt R, Britt LD. Evaluation of preoperative risk factors for converting laparoscopic to open cholecystectomy. Am Surg. 2012; 78: 831-833.
- Goonawardena J, Gunnarsson R, de Costa A. Predicting conversion from laparoscopic to open cholecystectomy presented as a probability nomogram based on preoperative patient risk factors. Am J Surg. 2015; 210: 492-500.
- Connor S, Garden OJ. Bile duct injury in the era of laparoscopic cholecystectomy. Br J Surg. 2006; 93: 158-168.
- Halbert C, Pagkratis S, Yang J, Meng Z, Altieri MS, Parikh P, et al. Beyond the learning curve: incidence of bile duct injuries following laparoscopic cholecystectomy normalize to open in the modern era. Surg Endosc. 2016; 30: 2239-2243.
- Karanikas M, Bozali F, Vamvakerou V, Markou M, Memet Chasan ZT, Efraimidou E, et al. Biliary tract injuries after lap cholecystectomy-types, surgical intervention and timing. Ann Transl Med. 2016; 4: 163.
- Breitenstein S, Nocito A, Puhan M, Held U, Weber M, Clavien PA. Robotic-assisted versus laparoscopic cholecystectomy: outcome and cost analyses of a case-matched control study. Ann Surg. 2008; 247: 987-993.
- Kaminski JP, Bueltmann KW, Rudnicki M. Robotic versus laparoscopic cholecystectomy inpatient analysis: does the end justify the means? J Gastrointest Surg. 2014; 18: 2116-2122.
- Okamoto K, Takada T, Strasberg SM, Solomkin JS, Pitt HA, Garden OJ, et al. TG13 management bundles for acute cholangitis and cholecystitis. J Hepatobiliary Pancreat Sci. 2013; 20: 55-59.
- Pang KW, Tan CH, Loh S, Chang KY, Iyer SG, Madhavan K, et al. Outcomes of Percutaneous Cholecystostomy for Acute Cholecystitis. World J Surg. 2016.
- Mizrahi I, Mazeh H, Yuval JB, Almogy G, Bala M, Simanovski N, et al. Perioperative outcomes of delayed laparoscopic cholecystectomy for acute calculous cholecystitis with and without percutaneous cholecystostomy. Surgery. 2015; 158: 728-735.
- Kais H, Hershkovitz Y, Abu-Snina Y, Chikman B, Halevy A. Different setups of laparoscopic cholecystectomy: conversion and complication rates: a retrospective cohort study. Int J Surg. 2014; 12: 1258-1261.
- Khasawneh MA, Shamp A, Heller S, Zielinski MD, Jenkins DH, Osborn JB, et al. Successful laparoscopic cholecystectomy after percutaneous cholecystostomy tube placement. J Trauma Acute Care Surg. 2015; 78: 100-104.
- Halawani HM, Tamim H, Khalifeh F, Mailhac A, Jamali FR. Impact of intraoperative cholangiography on postoperative morbidity and readmission: analysis of the NSQIP database. Surg Endosc. 2016.
- Sheffield KM, Riall TS, Han Y, Kuo YF, Townsend CM, Jr., Goodwin JS. Association between cholecystectomy with vs without intraoperative cholangiography and risk of common duct injury. JAMA. 2013; 310: 812- 820.
- Ford JA, Soop M, Du J, Loveday BP, Rodgers M. Systematic review of intraoperative cholangiography in cholecystectomy. Br J Surg. 2012; 99: 160-167.
- Daskalaki D, Fernandes E, Wang X, Bianco FM, Elli EF, Ayloo S, et al. Indocyanine green (ICG) fluorescent cholangiography during robotic cholecystectomy: results of 184 consecutive cases in a single institution. Surg Innov. 2014; 21: 615-621.
- Schols RM, Bouvy ND, Masclee AA, van Dam RM, Dejong CH, Stassen LP. Fluorescence cholangiography during laparoscopic cholecystectomy: a feasibility study on early biliary tract delineation. Surg Endosc. 2013; 27: 1530-1536.
- Higgins RM, Frelich MJ, Bosler ME, Gould JC. Cost analysis of robotic versus laparoscopic general surgery procedures. Surg Endosc. 2016.
- Tsuda S, Oleynikov D, Gould J, Azagury D, Sandler B, Hutter M, et al. SAGES TAVAC safety and effectiveness analysis: da Vinci (R) Surgical System (Intuitive Surgical, Sunnyvale, CA). Surg Endosc. 2015; 29: 2873- 2884.
- Bedeir K, Mann A, Youssef Y. Robotic single-site versus laparoscopic cholecystectomy: Which is cheaper? A cost report and analysis. Surg Endosc. 2016; 30: 267-272.