Case Report
A Case Report of a Gastrointestinal Fistula Patient with Severe Complication
Yueping Fan*, Hanping Shi and Jiujiang Li
Department of General Surgery, Aviation General Hospital, China
*Corresponding author: Yueping Fan, Department of General Surgery, Aviation General Hospital, Beijing, China
Published: 15 Sep, 2016
Cite this article as: Fan Y, Shi H, Li J. A Case Report of
a Gastrointestinal Fistula Patient with
Severe Complication. Clin Surg. 2016;
1: 1114.
Abstract
The management of gastrointestinal fistula still remains a tough challenge to most of surgeons. It is associated with high mortality and morbidity. The following case is biliary-enteric anastomosis fistula, with complicated and severe complications: sepsis, hemorrhage of digestive tract, malnutrition and disorder of electrolyte. Finally, the fistula closed by actively a bundle of therapeutic methods without operation. In this paper, we focus on two aspects of fistula management, source control and enteral nutrition. Adequate source control plays the most important role in management of fistula, especially with sump drainage tube. Enteral nutrition should be considered as possible as we can. We should try our best to establish a route delivering enteral nutrition in intricate situation of gastrointestinal fistula patient.
Introduction
Gastrointestinal fistula is defined as an abnormal pathological communication between skin surface and gastrointestinal track. It usually develops after abdominal surgical procedure. Despite advances in intensive care, nutrition support, antibiotics, wound local care, and surgical technique, gastrointestinal fistula continues to be a major challenge in management, with high morbidity and mortality. It would company many serious complications such as electrolyte disorder, malnutrition, severe sepsis, hemorrhage of digestive tract, even MODS (multiple organ dysfunction syndrome), if there has not an effective procedure to control intra-abdominal infection and fluid outflow from gastrointestinal track immediately. We want to share our experience in management of gastrointestinal fistula patient through following case report.
Case Presentation
The patient was female, 67 years old. She was admitted to our hospital in 2016-04-22. The chief
complains were “post radical resection of pancreas ampulla carcinoma for 1 month, yellow fluid out
flowed from abdominal drainage tube for 3 weeks, blood out flowed from stomach drainage tube
for 1 week”.
The patient underwent procedure of Whipple operation because of a mass in pancreas
ampulla in 2016-03-21. The pathologic diagnosis was moderately differentiated adenosquamous
carcinoma of pancreas ampulla. A week postoperatively, hyperpyrexia occurred accompanied with
hypotension. Another important symptom was purulent fluid out flowed from abdominal drainage
tube. According to serious condition the patient was transferred to ICU. The patient received fluid
resuscitation, vasoactive agents and anti-infective therapy, the blood pressure gradually tended to
stabilize. But fever still persisted. Type-B ultrasonic and CT check of abdomen found there was
localized pyoperitoneum. Two pigtail drainage tubes were successfully set to abdominal abscess
guided by Type-B ultrasonic. Symptom of fever seemly improved a little. The condition was changed
on 3 weeks postoperatively; blood was seen in stomach tube accompanied with tarry stools, and
again with high fever up to 39.0°C. Then the patient was transferred to our hospital in 2016-04-22
(4 weeks postoperatively).
Admission condition
Vital sign: T 37.4°C, P 98 bpm, R 21 times/min, BP 135/85 mmHg. Consciousness was clear,
expression was anxious. There were no obvious positive sign with pulmonary physical examination.
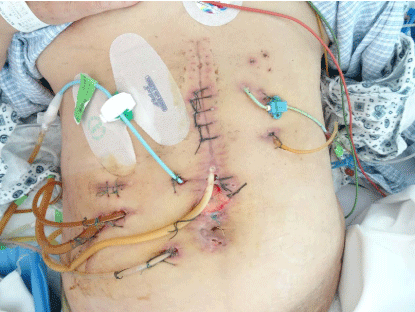
Abdominal physical examination: slightly distended, a long vertical incision with suture not yet
removed. The lower part of incision was poor healing. A total seven drainage tubes were seen on
abdomen. One was jejunal feeding tube, one was biliary-enteric anastomosis tube, and the other
5 were drainage tube of abdominal cavity. Yellow fluid could be seen in two tubes in right part
of abdomen, one was abdominal cavity drainage tube, and one was
biliary-enteric anastomosis tube. Tenderness was diffused but not
notable. Bowel sounds decreased. And dark red blood was seen in
gastric tube, stool was tarry. The situation of abdomen while admitted
to our hospital was shown in Figure 1.
Laboratory examination
WBC 17.6*109/L, N 15.1*109/L, N% 85.6%, RBC 2.38*1012/L, Hb
75g/L, Hct 22.7%, PLT 231*109/L; ALT 45.7 u/L, AST 48.0 u/L, ALB
35.5 u/L, TBIL 34.2 mmol/L, DBIL 0 mmol/L, IDBIL 11.4 mmol/L,
BUN 2.53 mmol/L, Cr 31 umol/L, k+ 3.08 mmol/L, Na+ 138 mmol/L,
Ca++ 2.02 mmol/L, Mg++ 0.44 mmol/L; PT 13.30s, INR 1.17; Fecal
occult blood (+++); Gastric occult blood (+++); Culture result
(drainage of abdominal cavity): Pseudomonas aeruginosa growth.
Diagnosis on admission
1. Intra-abdominal infection, 2. Gastrointestinal fistula, 3.
Hemorrhage of digestive tract, 4. Anemia, 5. Hypoproteinemia, 6.
Hypokalemia, 7. Hypocalcemia 8. Hypomagnesemia, 9. Malnutrition,
10. Hypertension, 11. Pancreas ampulla carcinoma (postoperatively).
Result of radiography
Radiography was done as soon as possible. When contrast
medium (meglucamine diatrizoate) was injected from one drainage
tube (that was already set in procedure of Whipple’s operation) in
the right part of abdomen, we found the contrast medium went into
a part of intestinal tract, and continued went into common bile duct
then left and right hepatic ducts (Figure 2). Radiography of another 4
drainage tubes showed localized abscess cavity, found none contrast
medium went into intestinal tract.
Strategy of therapy
Diagnosis of gastrointestinal fistula was clear, the site was on
biliary-enteric anastomosis, the amount of fistula was only one,
and type of fistula was enterocutaneous fistula. Complication of
gastrointestinal fistula of the patient was complicated and severe:
sepsis, hemorrhage of digestive tract, malnutrition and disorder of
electrolyte.
Strategy of therapy was that firstly gave active conservative
treatment in order to achieve the goal of stabilization of the
condition and even fistula closing, if fistula didn’t heal by the means
of conservative treatment, definitive operation would be performed
after at least 3 months.
There were two stages in the whole process of treatment. The
goal of the first stage was controlled the patient’s condition,
and meanwhile actively assessed situation of fistula, function of
digestive tract and degree of intra-abdominal infection. Detailed
procedures were following: fasted for solids and liquids; continuous
gastrointestinal decompression; proton pump inhibitor was given;
subcutaneous injection of octreotide; bacterial culture was performed,
and meanwhile antibiotics were administrated by intravenous drip
to covered spectrum of G+, G- and anaerobia; calcium gluconate,
vitamin K1 and FFP (fresh frozen plasma) were given to improve
coagulation function; transfused RBC suspension to improved
anemia; correcting electrolyte disorder; balanced body fluid; effective
source control. Three original drainage tubes were changed into sump
tubes which could continue negative draining while flushing (Figure
3). The other two pigtail tubes remained too irrigated intermittently.
And another important measure was early ambulation.
Temperature was less than 38.0°C for three days after given
sump drainage method. On the 4th day after admission (2016-04-
25) the patient got a fever up to 39.5°C with obvious chill. Catheter
of deep vein of right subclavian was removed immediately, a part
of catheter was sending to have bacteria culture. Then temperature
remained stable until the patient discharged from hospital. Symptom
of blood fluid out flowed from stomach tube and tarry stools were
gradually relieved. On the 5th day after admission (2016-04-26)
fluid out flowed from stomach tube turned to be yellow-green, and
symptom of tarry stools never occurred. Anemia, hypoproteinemia,
hypokalemia, hypocalcemia and hypomagnesemia also significantly
improved. Color of drainage fluids from the sump tube in right part
of the abdomen changed gradually. The first two days it was yellow,
and then light yellow, on the 4th day after admission (2016-04-25)
it was complete clear just like the flushing fluid. Then radiography
was done again to assess situation of fistula. When contrast medium
(meglucamine diatrizoate) was injected from drainage tube, we
didn’t found the contrast medium went into intestinal tract, and also
common bile duct, left and right hepatic ducts anymore.
When the condition has been effectively controlled, the second
stage of treatment began. It was proved to be closed of the fistula by
the result of radiography. The sump tube was with drawn little by
little; meanwhile sump tube with smaller in diameter was used. The
sump tube was removed when it withdrew until reached subcutaneous
tissue. Moreover the other four drainage tubes were removed one by
one gradually. There was only one tube remained which was jejunal
feeding tube. The biliary-enteric anastomosis tube was also removed
finally when total enteral nutrition support proceeds effectively.
Enteral nutrition support was considered when radiography indicated
fistula closing. Short peptide type of enteral nutrition was used at the
beginning from jejunal feeding tube, 20 ml/h, continuously pumped.
Meanwhile partial parenteral nutrition support still used. Drop rate
of enteral nutrition was up-regulate according to reflection of gut,
finally up to 80 ml/h. Parenteral nutrition didn’t administrated when
drop rate of enteral nutrition got to 40 ml/h. When enteral nutrition
began, therapies of proton pump inhibitor, octreotide, antibiotics
were with draw. The fluid from biliary-enteric anastomosis tube was
collected and then transfused into jejunal feeding tube as possible as
it could be until the biliary-enteric anastomosis tube was removed.
The patient discharged from hospital with healing gastrointestinal
fistula on 2016-06-04, total hospital stay was 43 days. The jejunal
feeding tube was still remained. Family enteral nutrition support
continued for at least one month.
Figure 1
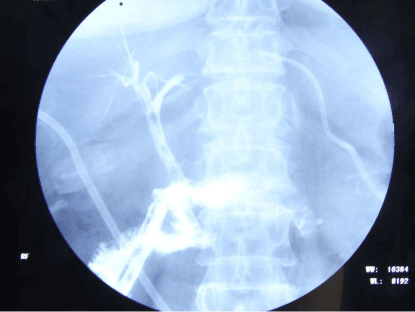
Figure 2
Figure 2
Result of radiography from one drainage tube in the right part
of abdomen. The contrast medium went into a part of intestinal tract and
continued went into bile ducts.
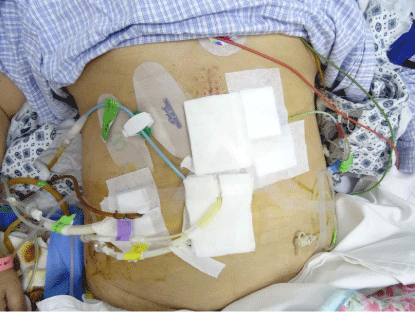
Figure 3
Figure 3
The original tube on right lower abdomen has been changed into
sump drainage tube which is a kind of double drainage tube.
Discussion and Summarize
Gastrointestinal fistula is not a common disease. Although rare,
but it is associated with considerable morbidity and mortality. The
management of it continues to present a tough challenge to most of
surgeons. It also brings prolonged hospital stay, expensive medical
cost and considerable psychological burden on patients [1-2].
We have been focused on the field of gastrointestinal fistula
treatment since 2011. There are nearly 130 gastrointestinal patients
transferred to our department underwent effective therapy by now.
This is one of the typical, successful cases received systemic effective
treatment. We want to share our opinion and experiences through
this case; we hope there would be something useful for some surgeons
who might encounter gastrointestinal fistula patient.
Adequate source control
There may be a bundle of therapeutic methods when encounter
a gastrointestinal fistula, including parenteral and enteral nutrition
support, acid suppressive therapy, application of somatostatin to let
bowel rest, drainage, antibiotics, correct electrolytic disturbances,
and local care of the fistula tract as well as emergency or definitive
operation, et al. But above all, the most important measure we should
perform is adequate source control. Uncontrolled infection is the
most common cause of treatment failure and mortality. Inadequate
source control results in uncontrolled infection. If inadequate
source control persists, the following complications would occur:
severe sepsis, sepsis shock, acute lung injury, acute kidney injury,
malnutrition, metabolic acidosis, serious electrolyte disturbances,
dysfunction of coagulation, hemorrhage of digestive tract, bleeding
from fistula tract and even MODS [3-4].
How can we get the goal of adequate source control? Drainage,
change the type of drainage may has effective result. Although
antibiotics play important role in treatment of intra-abdominal
infection, but drainage can’t be replaced by antibiotics. Drainage
is always primacy in procedure of intra-abdominal infection. The
common drainage tube placed in abdominal cavity during operation
does not drain effectively; it is more likely a signal tube which could
tell us whether there is bleeding or intestinal juice in abdominal cavity
postoperatively. It is a kind of passive drainage, but not active drainage.
Most of gastrointestinal fistula patients transferred to our department
almost always remained this common drainage tube, companied with
fever, disorder of metabolism, malnutrition even bleeding. In our
department we change this common tube to another drainage tube
that is sump drainage tube or called double-drainage tube, a kind of
active drainage tube. There are two parts in the sump drainage tube.
One is drainage part, connected with vacuum system in the wall, so
it is active drainage. Another part is irrigation, connected with sterile
saline liquid. This kind of sump drainage could get goal of adequate
source control. Once achieving adequate source control, condition
may get better soon and complication may decrease obviously. Even
some gastrointestinal fistula may be closed by the sump drainage
avoiding operation once more. This case showed a good outcome by
adequate source control using the sump drainage tube. But one thing
we should clear, this kind of sump tube isn’t omnipotent, if it is used
not correctly, side-effects may occur such as bleeding, aggravated
infection, et al.
Enteral nutrition support
Enteral nutrition support also plays very important role in
procedure of gastrointestinal fistula. Enteral nutrition should be
considered as possible as we can. It has been already accepted that
if gut works, use it. And as we all know, if a critical could use enteral
nutrition, it is successful by half. So, enteral nutrition is another
critical aspect as well as source control. Compare to parenteral
nutrition, enteral nutrition has many advantages as following: it
is more conformed to the physiological process of human body; it
can protect intestinal barrier; it reduces bacterial translocation from
gut; it improves hepatic function and reduces cholestasis; it has a
better favorable benefits improving nutrition; avoiding catheter
related blood stream infection; morbidity decreases when enteral
nutrition begins. Also, enteral nutrition is cheaper than parenteral
nutrition, and easier to handle even could be carried on at home
[5-6]. According to our experience, once enteral nutrition support
successfully developed, condition of patient would be stable than
during the period of parenteral nutrition.
It is not simple to applicate enteral nutrition correctly. There
are several things should be notice in gastrointestinal fistula patient.
Firstly, only after hemodynamic stabilization, nutrition support
could be considered including enteral nutrition. When a patient is
in the situation of unstable hemodynamic, fluid resuscitation and
vasopressors agents are always primary. Secondly, if we want to
start enteral nutrition, a thorough evaluation of digestive track and
fistula must be known well. To assess situation of digestive track and
fistula, radiography is recommended. The investigation of digestive
track by means of radiography can tell us the length of intestine
and whether it is obstructed, and help us to decide whether enteral
nutrition can be used. The investigation of fistula tell us site of fistula,
amount of fistula, and help us to decide how to use enteral nutrition,
from nasogastric tube or from nasointestinal tube, or whether it is
possible to collect intestinal contents then transfer into nutrient tube?
If investigation of bowel and fistula is not clear, enteral nutrition
shouldn’t start until enough information about bowel and fistula is
achieved. If there are several fistulas on abdomen, it is hard to use
enteral nutrition. We should try our best to design an idea route to
use enteral nutrition, even though a part of intestine. Utilize every
part of intestine which still has function. It is easy to say but hardly
to perform. The third, there is a specific duration that shouldn’t
use enteral nutrition. When it is possible to close fistula through a
conservative treatment, total parenteral nutrition and somatostatin
are applied in order to reduce secretion of gastrointestinal fluid. So
it reduce amount of gastrointestinal fluid from fistula, meanwhile,
accompany with effective drainage, promote closure of fistula. If
enteral nutrition is used during this stage, effect of total parenteral
nutrition and somatostatin would diminish because of stimulation to
secret of gastrointestinal fluid enhanced.
Conclusion
This case is one of successful cured gastrointestinal fistula
patient without definitive operation in our department. To our
experience, adequate source control plays the most important role in
management of fistula, especially with sump drainage tube, a kind of
active drainage tube. On the other hand, enteral nutrition support
also plays very important role in procedure of gastrointestinal fistula.
Enteral nutrition should be considered as possible as we can. We
should try our best to establish a route delivering enteral nutrition in
intricate situation of gastrointestinal fistula patient. It is easy to say,
but we will always counter unexpected situation because of individual
difference in gastrointestinal fistula patients.
There are also many other aspects should be notice, but not
mention in this paper. In this case we focus on above points of
experiences in clinics. We hope it would be somewhat helpful to
surgeon who might encounter gastrointestinal fistula. There must
be some disagreements or incorrect points in the paper, welcome
exchange experience together later.
References
- Whelan JF Jr, Ivatury RR. Enterocutaneous fistulas: an overview. Eur J Trauma Emerg Surg. 2011; 37: 251–258.
- Visschers RG, van Gemert WG, Winkens B, Soeters PB, Olde Damink SW. Guided treatment improves outcome of patients with enterocutaneous fistulas. World J Surg. 2012; 36: 2341–2348.
- Terzi C, Egeli T, Canda AE, Arslan NC. Management of enteroatmospheric fistulae. Int Wound J. 2014; 11: 17–21.
- Davis KG, Johnson EK. Controversies in the care of the enterocutaneous fistula. Surg Clin North Am. 2013; 93: 231–250.
- Oshima T, Singer P, Pichard C. Parenteral or enteral nutrition: do you have the choice? Curr Opin Crit Care. 2016; 22: 1-7.
- Petrov MS, Loveday BP, Pylypchuk RD, McIlroy K, Phillips AR, Windsor JA. Systematic review and meta-analysis of enteral nutrition formulations in acute pancreatitis. The Br J surg. 2009; 96: 1243-1252.