Case Report
Revision “Layer-by-Layer” of Severe Iatrogenic Ectropion: Technical Notes
Cotrufo S, Omakobia E* and Liew C
Department of Head and Neck Cancer Service, University College Hospital, UK
*Corresponding author: Eugene Omakobia, Department of Head and Neck Cancer Service, University College Hospital, 1st Floor East, 250 Euston Road, NW1 2PG, London, UK
Published: 09 Aug, 2016
Cite this article as: Cotrufo S, Omakobia E, Liew C. Revision “Layer-by-Layer” of Severe Iatrogenic Ectropion: Technical Notes. Clin Surg. 2016; 1: 1078.
Abstract
Iatrogenic ectropion is a severe condition that requires careful assessment and management. There
are various techniques available to correct different degrees of ectropion and for the management
of the most severe cases it becomes necessary to combine them together. This article presents the
assessment and treatment of a severe case of ectropion following resection of a basal cell carcinoma
of the middle third of the face and initial reconstruction with an inappropriate technique.
The authors present the correction of the above case with a combination of skin and muscle flaps to
obtain reconstruction “layer-by-layer”. The result achieved with this approach is excellent because
each missing component of the lower eyelid is replaced ad hoc with local tissues; the orbicularis
oculi muscle flap has proved to be a very powerful sling supporting the lower eyelid all the way from
canthus-to-canthus.
Introduction
Iatrogenic ectropion is a serious complication following tissue loss of the lower orbital or
malar area. In most of the cases seen in our unit, this is the consequence of 1) damage to the facial
nerve, 2) resection performed with wrong orientation in the mid third of the face and 3) following
reconstruction with an inappropriate method.
There are various techniques available to correct different degrees of ectropion and for the
management of the most severe cases, it becomes necessary to combine them together. Careful
evaluation of the tissue loss – mucosa, cartilage, muscle and skin – will guide this decision.
In 2007, Stagno et al. [1] showed how a medially based upper orbicularis oculi muscle flap could
be transposed to the lower eyelid through a subcutaneous tunnel at the medial canthus to support
the edge of the lower eyelid by working as a sling. The authors have proved the efficacy of this
technique in the long term and we have also applied it successfully in our cancer unit.
In this letter, we present a correction “layer-by-layer” of a severe iatrogenic ectropion by
combining the Stagno’s muscle flap and an advancement V-Y skin flap.
Case Presentation
A 73 year old lady diagnosed with basal cell carcinoma of the lower eyelid was treated 18 months
earlier with excision and reconstruction using a Mustarde flap. Unfortunately, she developed an
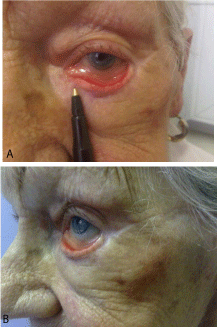
ectropion in the early post-operative period, suggesting inappropriate flap design. Figure 1 shows
the significant retraction of the lower eyelid at the time of her first consultation. Relevant details
of this injury were 1) vertical skin loss of the lower eyelid and 2) redundancy of the conjunctival
mucosa.
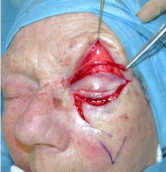
The decision was to treat this case with a combined approach by using a V-Y advancement skin
flap from the cheek and the Stagno's technique to support the lower eyelid as shown in Figure 2.
Through a blepharoplasty skin approach, a transverse strip of orbicularis muscle was harvested
from lateral canthus (distal end of the flap) to the medial canthus (pedicle). Once the flap was
elevated, its distal end was obviously very well perfused. A subcutaneous tunnel was performed at
the medial canthus to permit transposition of the flap into the lower eyelid.
A V-Y skin flap was designed following the natural creases of the malar area and advanced to
replace the vertical skin loss of the lower eyelid from medial to lateral canthus. Once the skin flap
was sutured to the redundant conjunctiva, the orbicularis oculi flap was fixed to the lateral canthal
ligament to work as a sling to keep the eyelid in the desired position.
We also found it opportune to use a full thickness skin graft
(obtained from excess from the medial tip of the V-Y flap) to give
extra support to the lateral third of the eyelid. A Frost stitch was left
in place for 1 week post-operatively and the results shown are from 6
weeks post surgery.
Six months after surgery, the patient did not require any further
surgical intervention and since then she has unfortunately not
attended any further clinic reviews with the surgical team. However,
she has been seen by her general practitioner and also by the oncology
team with no problems reported.
Figure 1
Figure 1
Severe left ectropion secondary to inappropriate reconstruction of
lower eyelid with a Mustarde Flap. Note redundant conjunctiva mucosa. The
tip of the pen is showing the medial margin of the previous flap.
Figure 2
Figure 2
Intraoperative detail: combined approach using the Stagno’s
technique, a V-Y skin flap and a full thickness skin graft. Note that after
release of the Mustarde flap the eyelid margin came back to a more normal
position.
Discussion
The use of a sling is often essential to sustain the lower eyelid.
In cases of early stage facial palsy, there is good indication for using
a sling, as this allows repositioning of the lower eyelid without
shortening (and thinning) it, which can happen when using the
tarsal strip or similar. The use of a transposition muscle flap is a more
conservative and effective approach to creating a sling because it does
not require the involvement of different anatomical sites such as the
temporal area or the lateral aspect of the thigh. The muscle flap is also
very well perfused at its distal end, which reduces the risk of infection
possibly associated with fascia grafts. We found this technique very
powerful in restoring correct symmetry of eyelid position following
a severe case of vertical tissue loss of the lower eyelid. The support
provided to the edge of the lower eyelid goes all the way from medialto-lateral
canthi.
In our experience, we observed some degree of stretching of this
muscle sling during the first 6 weeks but never afterwards; for this
reason we recommend 1) performing an initial “mild” hypercorrection
when suturing it to the lateral rim of the orbit and 2) an early follow
up to consider the need for revision surgery. All candidates for this
procedure need to be informed about the possibility of loosening
of the sling; and hence the potential need for tightening in a second
stage procedure.
Figure 3
Figure 3
Follow up at 3 weeks. Very good healing of flaps and graft with
correction of ectropion. Good symmetry between the eyes.
Conclusions
Reconstruction layer-by-layer is ideal when working on complex
and delicate functional structures. The combination of the Stagno’s
flap and the V-Y advancement skin flap is very reliable and provides
excellent results in this case of iatrogenic ectropion. The orbicularis
oculi muscle flap has a very reliable blood supply and its use is
“forgiving” allowing secondary tightening if necessary without skin
excision.
We recommend the use of this combined approach for all cases of
severe vertical skin loss of the lower eyelid.