Research Article
Long-Term Outcomes of Laparoscopic Peritoneal Lavage for Complicated Diverticulitis in a Dedicated Emergency Surgery Service
Rhodes K and Behar N D*
Emergency Surgery Department, Chelsea and Westminster Hospital, UK
*Corresponding author: Nebil Behar, Department of Surgery, Chelsea and Westminster Hospital, 369 Fulham Road, London, SW10 9NH. UK
Published: 05 Jul, 2016
Cite this article as: Rhodes K, Behar N. Long-Term Outcomes of Laparoscopic Peritoneal Lavage for Complicated Diverticulitis in a Dedicated Emergency Surgery Service. Clin Surg. 2016; 1: 1066.
Abstract
Aim: A dedicated emergency surgery service allows for faster accumulation of experience in procedures that are otherwise infrequent; Laparoscopic Peritoneal Lavage (LPL) of complicated
diverticulitis is one such procedure. We describe our long-term outcomes on an intention to treat
basis with LPL.
Method: Data was collected on 31 consecutive patients undergoing LPL in our unit between 2011
and 2015. Outcomes assessed were post-operative complications including the requirement for
further interventions, length of stay and mortality. All patients requiring surgery underwent initial
laparoscopy with a view to lavage without resection.
Results: In the early outcomes, across all Hinchey grades, there were 6 further radiological or
operative interventions out of 31 (19%). There were no deaths.
In the late outcomes (median 34 months follow up), across all Hinchey grades, there were 7 further
operative interventions out of 31 (23%). There were 5 deaths overall (16%) with mean days to death
of 498 days. All deaths were of non surgical causes. Two cancers were detected due to our routine
policy of colonoscopic follow up. 3 out of 22 (14%) remaining patients with non-respected colon
were admitted with uncomplicated diverticulitis during median follow up period of 34 months.
Conclusion: Laparoscopy with a view to washout on an intention to treat basis appears safe, across
all Hinchey grades of diverticulitis within the context of close post-operative monitoring and
colonoscopic follow up. LPL also allows laparoscopic relief of small bowel obstruction in patients
presenting with this bystander complication of diverticulitis. Further radiological drainage after
LPL in this study appears feasible without resorting to resection although 1 of 3 patients progressed
to a Hartmann’s procedure which was uneventful. Based on our findings of subsequent malignancy
in two patients, we would advise timely post-operative colonoscopy and follow up in all patients.
Introduction
Laparoscopic Peritoneal Lavage (LPL) has become a recognised and useful procedure for
managing complicated diverticulitis [1-4].
Within the context of a dedicated emergency surgery service, experience can accumulate faster
than would otherwise be possible. Furthermore, close monitoring of these patients may enable the
surgeon to recognise complications and failures early, resulting in successful salvage.
In our department, all patients presenting with diverticulitis are admitted under a single team
dedicated to management of emergency surgical patients without the distraction of elective surgery.
Patients with significant peritonitis undergo prompt CT scanning and decisions are made early at a
consultant level whether to proceed to surgery or not.
Those patients with CT diagnosis of Hinchey I diverticulitis with a consistent clinical picture,
are managed conservatively with antibiotics. Patients with Hinchey II diverticulitis diagnosed on
CT scan are considered for radiological interventional drainage (IR) in the first instance; whereas
patients, in whom IR is unfeasible or unsuccessful, are offered LPL. All patients suspected to be
Hinchey III or IV are offered LPL and those found to be Hinchey IV at the time of LPL are converted
to laparotomy and resectional surgery.
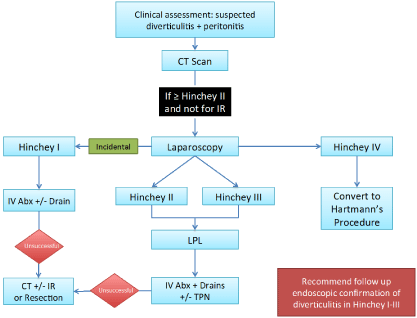
Figure 1
Aims
In this study, we aim to demonstrate our early and late outcomes adhering to a LPL first approach in all patients requiring surgery. We also describe our use of antibiotics, drains, parental nutrition and intensive care bed stay in this group of patients.
Methods
Data was collected on 31 consecutive patients undergoing LPL in
our unit between 2011 and 2015.
Decision to operate was undertaken based on patient’s clinical
picture (peritonitis and sepsis) in conjunction with CT scan findings.
If either of these implicated Hinchey III or Hinchey IV diverticulitis
then patient was taken to theatre for LPL. If Hinchey II was suspected
on CT scan, then patient was referred for IR drainage and only
offered LPL if this was not feasible. Patients felt to be Hinchey I was
managed conservatively with antibiotics. See Figure 1. Despite this
algorithmic approach, we have performed LPL on 10 patients with
finding of Hinchey I diverticulitis at the time of laparoscopy. Our
decision to include all patients undergoing LPL was based on our
aim to analyse outcomes on an intention to treat basis. We believe
that including Hinchey I in this context is important; as operations
performed in patients who could otherwise improve without surgery
must be included to fully assess the role of LPL in diverticulitis.
We have collected data on the post-operative progress of all
patients who were managed with LPL. We have also followed these
patients up in the months following discharge using GP records,
outpatient letters and subsequent admissions, to determine the need
for further interventions.
Results
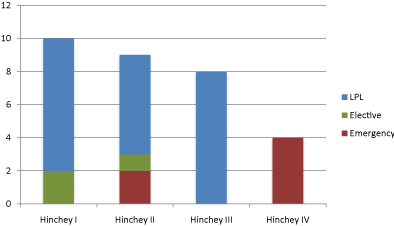
In total 31 patients underwent LPL; 4 patients were noted to
have Hinchey IV diverticulitis at laparoscopy and were converted
to laparotomy and Hartmann’s procedure. Of these patients, 2
required further surgical intervention within the same admission
and 2 subsequently as an elective procedure (1 for incisional hernia
repair and 1 for reversal of Hartmann’s).Of the remaining 27 patients,
10 were found to have Hinchey I diverticulitis, 9 Hinchey II and 8
Hinchey III (Table 1).
8/27 (30%) patients were given TPN for 7 days or more.
8/27 (30%) patients had small bowel obstruction relieved at the
time of LPL as evidenced by a clear transition point related to septic
focus.
Antibiotics were given to all patients, Hinchey I for median length
of 10 days (range 5-13), 15 days for Hinchey II (range 12-43) and 17
days for Hinchey III (range 7-37).
High-dose probiotics were given in 10/27 patients and no patients
were found to have toxin positive C diff infection post-operatively
(Table 2).
There were 5 deaths in total in long term follow up; these were
of non-surgical causes and not related to diverticulitis. These are
detailed in (Table 3).
Early outcomes, same admission
• 1/10 Hinchey I required IR drainage in post-op period
• 1/9 Hinchey II required sigmoid colectomy
• 2/8 Hinchey III required IR drainage
• 2/4 Hinchey IV required further laparotomy and washout
• No deaths within same admission, across all Hinchey grades
Late outcomes, at median 34 months (range 1-60)
• 2/10 Hinchey I required further resection. 1 cancer, 1 benign
• 2/9 Hinchey II required further resection. 1 cancer, 1 benign
• 0/8 Hinchey III required further resection.
• 2/4 Hinchey IV/Hartmann’s required further elective operations
• 5/31 deaths overall at long-term follow up (16%), 3 Hinchey
II, 2 Hinchey III. Mean days to death 498 days. All deaths were of
non-surgical causes.
• Only 3 patients were readmitted with uncomplicated
diverticulitis (Hinchey I)during the follow up period across all groups
despite a relative policy of non-resection
‘Surgical Outcomes Risk Tool’ (SORT) Predicted Mortality
In our case series, 30-day mortality was zero. However we decided
to compare the predicted mortality associated with our departmental
protocol of intention to treat laparoscopy against that of a first line
Hartmann’s procedure (For Hinchey II and III patients), to do this
we used the SORT Surgery score. Further to this, we also assessed the
risk associated with an elective resection, which may be required in
the future by some patients with recurrent disease (Table 4).
Table 1
Table 1
Table of patient demographics.
8/27 (30%) patients were given TPN for 7 days or more.
8/27 (30%) patients had small bowel obstruction relieved at the time of LPL as
evidenced by a clear transition
Table 2
Table 3
Table 4
Table 5
Discussion
In our unit, further elective resection was offered only to patients
with future complications such as fistulating disease, obstruction
or cancer. Despite this policy, only 3 patients had uncomplicated
diverticulitis which was successfully managed with antibiotics at
median follows up of 34 months. This is in contrast to other studies
that have used LPL as a bridge to elective resection [5]. In our study 2
patients required subsequent elective surgery; 1 patient for obstruction
at 11 months in whom it could be argued that earlier surgery would
have prevented the deterioration to obstructing disease and one
patient for colovesical fistula at 4 months. Both patients recovered
from elective surgery without complications. Of the 2 patients with
cancer both were diagnosed post LPL at colonoscopy at 1 month and
2 months and managed palliatively with defunctioning colostomy in
view of advanced disease and co-morbidities (Figure 2).
In our hospital, we have excellent access to interventional
radiology. As a result, many of our Hinchey II cases would not have
progressed to LPL. Furthermore, if a patient developed a sequential
drainable collection after LPL we were able to employ radiological
drainage in the first instance rather than undertaking resection. In
total 3 patients required post-LPL radiological drainage; although
one of these patients later required Hartmann’s procedure within the
same admission for on-going sepsis.
On the other hand, based on our outcomes for Hinchey II
patients, it could be argued that if IR is not available then LPL appears
to be a safe alternative to resection in Hinchey II patients.
Studies have shown that mortality in complicated diverticulitis
requiring surgery ranges from 12-36% [6-9]. Whilst we accept that
Hinchey I patients might not have needed LPL or resection; some
of these patients, if laparoscopy is not performed, end up with a
laparotomy and resection in an emergency setting with associated
increased mortality. In our pragmatic study, no patient died in the
short or long-term follow-up period from surgery for diverticulitis
when following the algorithm in Figure 1.
In total, 4 patients had to undergo further elective surgery
after LPL. These operations were conducted either for further
complications of disease or for finding of cancer at subsequent
colonoscopic examination. Of these, 2 were early elective operations
for cancer, 1 anterior resection for diverticular stricture at 11 months
and 1sigmoid colectomy and defunctioning ileostomy for colovesical
fistula at 4 months. Only 1 patient required further emergency
surgery after successful LPL; this was for poor control of sepsis which
required Hartmann’s Procedure at day 4 (Table 5).
Interestingly our study reveals prolonged hospital stay and
antibiotic usage despite the minimally invasive nature of LPL. We
believe that in the context of complicated diverticulitis our study
shows the benefits of LPL to be reduction in mortality and morbidity
compared with the standard resectional surgery rather than the
commonly used outcomes in laparoscopic surgery of shorter hospital
stay and earlier return to daily activities.
Figure 2
Conclusion
Low mortality is achievable with LPL first approach in an
unselected group of patients presenting with peritonitis and/or CT
findings of complicated diverticulitis. LPL allows good initial control
of sepsis and does not appear to compromise the outcome of future
interventions such as radiological drainage or resectional surgery in
our study.
Patients in Hinchey II and III categories required prolonged
hospital stay (19 and 18days respectively) and antibiotics (15 and 17
days respectively). In total, 23% (7/31) of patients required further
emergency interventions across all Hinchey grades during the index
admission. In this context, we believe continuity of care by a team of
dedicated Emergency Surgery Service is essential for daily monitoring
and early decisions that lead to timely changes in management.
References
- Toorenvliet BR, Swank H, Schoones JW, Hamming JF, Bemelman WA. Laparoscopic peritoneal lavage for perforated colonic diverticulitis: a systematic review. Colorectal Dis. 2010; 12: 862–867.
- O'Sullivan GC, Murphy D, O'Brien MG, Ireland A. Laparoscopic management of generalized peritonitis due to perforated colonic diverticula. Am J Surg. 1996; 171: 432–434.
- Alamili M, Gogenur I, Rosenberg J. Acute complicated diverticulitis managed by laparoscopic lavage. Dis Colon Rectum. 2009; 52: 1345–1349.
- Afshar S, Kurer MA. Laparoscopic peritoneal lavage for perforated sigmoid diverticulitis. Colorectal Dis. 2012; 14: 135–142.
- Cirocchi R, Trastulli S, Vettoretto N, Milani D, Cavaliere D, Renzi C, et al. Laparoscopic peritoneal lavage: a definitive treatment for diverticular peritonitis or a "bridge" to elective laparoscopic sigmoidectomy?: a systematic review. Medicine (Baltimore). 2015; 94: e334.
- Elliott TB, Yego S, Irvin TT. Five-year audit of the acute complications of diverticular disease. Br J Surg.1997; 84: 535–539.
- Peoples JB, Vilk DR, Maguire JP, Elliott DW. Reassessment of primary resection of the perforated segment for severe colonic diverticulitis. Am J Surg. 1990; 159: 291–293.
- Zeitoun G, Laurent A, Rouffet F, Hay J, Fingerhut A, Paquet J, et al. Multicentre, randomized clinical trial of primary versus secondary sigmoid resection in generalized peritonitis complicating sigmoid diverticulitis. Br J Surg. 2000; 87: 1366–1374.
- Kronborg O. Treatment of perforated sigmoid diverticulitis: a prospective randomized trial. Br J Surg. 1993; 80: 505–507.