Research Article
Laparoscopic Surgery for Splenic Flexure Cancers: Short and Long-Term Outcomes in Comparison with Conventional Open Surgery
Harji D1*, Watson L1, Gallagher1, Burke D2, Sagar P2 and Griffiths B1
1Department of Colorectal Surgery, Newcastle Upon Tyne Hospitals NHS Foundation Trust, UK
2Department of Colorectal Surgery, St James’s University Hospital, UK
*Corresponding author: Deena Harji, Department of Colorectal Surgery, Newcastle Upon Tyne Hospitals NHS Foundation Trust, Newcastle, NE1 4LP, UK
Published: 07 Jul, 2016
Cite this article as: Harji D, Watson L, Gallagher, Burke D, Sagar P, Griffiths B. Laparoscopic Surgery for Splenic Flexure Cancers: Short and Long-Term Outcomes in Comparison with Conventional Open Surgery. Clin Surg. 2016; 1: 1065.
Abstract
Background: Laparoscopic resection of splenic flexure cancers remains controversial. This study reviews the management of splenic flexure tumours, comparing outcomes between laparoscopic (LR) and open (OR) resections.
Methods: All patients undergoing surgery for a splenic flexure colonic carcinoma at two tertiary
level institutions between January 2000 and July 2011 were identified. Data were collected on patient demographics, operative detail, histological data and follow up status. Data was analysed using SPSS version 19.
Results: A total of 111 patients were included in the study: 40 LR and 71 OR. The overall conversion rate in the LR group was 7.5%. Oncological outcomes between the two groups were similar, with
no statistically significant differences observed with regards to lymph node yield, margin status,
overall survival and recurrence rates. The median length of stay in the laparoscopic group was
10 days compared to 18 days in the open group (p=0.05). No significant differences were seen
between the two groups with regards to post-operative morbidity, with rates of 35.1% and 25.7%
in the laparoscopic and open group respectively, p=0.30. However, the grade of complication was
significantly lower in the laparoscopic group compared to the open group, with grade III ClavienDindo
rates of 7.7% and 42.1% respectively, p=0.05.
Conclusion: Our study adds to the growing evidence base advocating laparoscopic surgery as
technically safe and feasible option in the operative management of splenic flexure tumours, with
comparable oncological and clinical outcomes compared to open surgery.
Keywords: Splenic flexure cancer; Laparoscopic surgery
Introduction
Splenic flexure tumours account for 3-8% of all colonic malignancies, and are traditionally
associated with a high risk of obstruction and poor prognosis [1]. The management of splenic
flexure tumours is challenging, with a range of surgical options available from segmental
resection to subtotal colectomy. The role of laparoscopic surgery has not been fully elucidated in
the management of this group of tumours, as splenic flexure tumours were not included in the
previous randomised controlled trials [2,3]. There are a number of technical considerations when
considering laparoscopic resection in this group, including type of operation, lymph node yield,
high tie evaluation and potential for splenic injury.
This study reviews our experience in managing splenic flexure tumours, comparing outcomes
between laparoscopic and open resections.
Methods
All patients undergoing surgery for a splenic flexure colonic carcinomaat two tertiary level
hospitals between January 2000 and July 2011were identified retrospectively. Local ethical approval
was sought for the study. A splenic flexure carcinoma was defined as a carcinoma located between
the distal third of the transverse colon and the first part of the descending colon [4]. Pre-operative
workup included physical examination, colonoscopy, staging computed tomography of the thorax,
abdomen and pelvis. Definitive diagnosis of a splenic flexure cancer was confirmed intra-operatively
by visualisation of the lesion or a tattoo.
Inclusion criteria for the study included a histologically confirmed
adenocarcinoma located at the splenic flexure in an adult patient.
Exclusion criteria included patients with synchronous colonic cancers
and patients undergoing an elective palliative operation.
Data were collected on patient demographics, presentation of
disease, operative detail, multimodal therapy, histological data and
follow up status. All complications were graded according to the
Clavien-Dindo classification. This is an acceptable and validated
method of documenting surgical complications. The system is
divided into 7 grades, reflecting the varying severity of post-operative
complications (Table 1).
Statistical analysis
Statistical analysis was performed using the Statistical Package
for Social Sciences (SPSS) version 19.0 (SPSS™
, Chicago, Illinois).
Survival analysis was performed using the Kaplan-Meier method,
with differences between the curves tested using the log-rank test.
Differences between the groups were analysed using the independent
t-test or chi-squared test as appropriate on an intention to treat basis.
A P value of <0.05 was used to denote statistical significance.
Table 1
Table 2
Results
One hundred and eleven patients, including 49 (43.8%) female
underwent surgery with curative intent. Median age at time of surgery
was 68 (IQR 60-77) years. Twenty-five (22.3%) patients underwent
emergency surgery for an obstructing or perforated malignancy. Forty
(35.7%) patients underwent a laparoscopic resection, 3(7.5%) patients
had a laparoscopic procedure converted to an open procedure.
Thirteen (11.6%) patients underwent a multivisceral resection to gain
optimal oncological control. Iatrogenic injury requiring splenectomy
was observed in 7 (6.6%) cases. Patient demographics and operative
details are outlined in (Table 2).
Post-operative outcomes
Thirty-day mortality was 4.5%. Thirty-day morbidity rate was
28.8%, with a total of 32 complications observed. Re-operation rate
was 5 patients (4.5%); 3 for an anastomotic leak, 1 for small bowel
obstruction and 1 for drainage of an intra-abdominal collection.
Median overall length of stay was 12 (IQR 6-20) days. Post-operative
and histological data are outlined in (Table 3).
Survival outcomes
Median overall follow up from time of surgery to death or last
clinical encounter was 26.5 months (IQR 7 – 57), with a mean follow
up of 31.4 months. Mean follow up in the laparoscopic group was
27.2 months compared to 39.4 months in the open group (p=0.05).
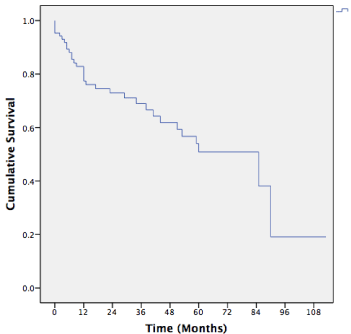
Overall five year survival was 49%, 5 year disease free survival
was 64% with an overall median survival of 85 months (Figure 1).
Locoregional relapse occurred in 22 (15.2%) patients, with local
recurrence in 8 (7.1%) patients, hepatic metastases in 5 (4.5%),
pulmonary metastases in 2 (1.8%) patients, hepatic and pulmonary
metastases in 1 (0.9%) patient and pulmonary and cerebellar
metastases in 1 (0.9%) patients.
Laparoscopic vs. open surgery
There was no statistically significant difference between age and
gender in the laparoscopic and open groups (Table 4). A significantly
higher proportion of patients underwent an open operation when
presenting as an emergency, with rates of 31.1% vs. 5.4% for
laparoscopic surgery, p=0.02. A higher proportion of advanced T4
splenic flexure cancers were observed in the open group compared
to the laparoscopic group, with rates of 44.3% vs. 27.8%, p=0.02.
A higher proportion of patients in the open group underwent a
multivisceral resection compared to the laparoscopic group, with
rates of 17.1% vs. 2.7%, p=0.03. No splenectomies were carried out
in the laparoscopic group compared to 6 in the open group (p=0.05).
Median survival in the laparoscopic group was 27 months vs. 34
months in the open group (p=0.45). The median length of stay in
the laparoscopic group was 10 days compared to 18 days in the open
group (p=0.05). No significant differences were seen between the
two groups with regards to post-operative morbidity, with rates of
35.1% and 25.7% in the laparoscopic and open group respectively,
p=0.30. However, the grade of complication was significantly lower
in the laparoscopic group compared to the open group, with grade III
Clavien-Dindo rates of 7.7% and 42.1% respectively, p=0.05.
Table 3
Figure 1
Table 4
Discussion
There has been much debate around the validity of laparoscopic
surgery in the management of splenic flexure tumours, with the main
controversy surrounding the issue of optimal oncological clearance,
with regards to the correct operation and adequate lymph node yield.
Lymph node status has oncological implications, dictating the need
for further treatment in the form of chemotherapy. Consequently,
the oncological and surgical outcomes of laparoscopic management
of this group have not been examined in previously published
randomised controlled trials [5,6]. Our study is the one of the largest
series documenting outcomes in splenic flexure tumours and drawing
comparisons between open and laparoscopic resections.
Tumours located at the splenic flexure pose a range of technical
dilemmas due to its variable blood supply and dual lymphatic
drainage. In 89% of cases the blood supply to the splenic flexure is
carried by the inferior mesenteric artery via the left colic, and by the
superior mesenteric artery via the middle colic artery in 11% [7]. The
middle colic artery is absent in between 5 – 22% of patients [7]. This
has led to ongoing debate in the literature with regards to the optimal
operation, vascular high tie and adequate lymph node yield in this
cohort of patients, with some authors advocating extended resection
in the form of right hemicolectomy [8], whilst others advocate
segmental resection [9,10]. Typically, the operation type undertaken
is left to the discretion of the operating surgeon, depending on
stage of tumour, adjacent organ involvement, patient age and comorbidities.
In this series, a range of operations were undertaken,
with no differences in survival observed based on operation type.
Furthermore, a higher proportion of splenic flexure tumours
requiring multivisceral resection were carried out in the open group
compared to the laparoscopic group (17.1% vs. 2.7%, p-0.03).This is
further reflected by the significantly higher proportion of T4 tumours
observed in the open group, with 44% of T4 tumours in this group,
thus suggesting there is a selection bias towards open surgery in
advanced splenic flexure cancers.
With advancing knowledge and experience in laparoscopic
surgery combined with advances in laparoscopic instrumentation
there is increasing interest in undertaking laparoscopic resections for
transverse colonic and splenic flexure tumours. Kim et al. [11] reported
no statistically significant difference in oncological outcomes between
laparoscopic and open surgery in 87 patients with transverse colonic
cancer, of which 20 were located at the splenic flexure. Interestingly,
this group reported a higher lymph node yield in the laparoscopic
group Vs. the open, with 26.1 and 22.7 nodes obtained respectively
(p>0.05). Schlachta et al. [12] compared laparoscopic outcomes
between transverse colon tumours, including tumours located at the
splenic flexure, and other colonic tumours. This group reported a
statistically significant greater yield of lymph nodes in the transverse
colon group compared to other colonic lesions. We did not observe
this in our study, however we documented a comparable lymph node
yield, with a median of 19 in the laparoscopic group compared to
20 in the open group, p=0.63. However, our study identified lymph
node status to be a statistically significant prognostic factor of overall
survival (p=0.01). These observations have important oncological
implications with regards to further treatment and overall survival,
thus suggesting a laparoscopic approach is oncologically safe, and is a
comparable mode of surgery in this cohort.
Previous literature documenting outcomes in splenic flexure
tumours have drawn comparisons with a heterogeneous control
group, consisting of tumours located in various positions around the
colon [9,12], with potential biological differences effecting outcomes.
Benedix et al support this observation reporting a higher number of
prognostically unfavourable tumours located at the splenic flexure
compared to other colonic sub sites [13]. Our study addresses this by
comparing the mode of surgery in a single cohort of tumours, thus
eliminating any bias secondary to tumour biology based on colonic
location.
The rate of inadvertent splenic injury in splenic flexure tumours
has been reported to be 6%, compared to 2% in descending colon
tumours and 1% in transverse colon tumours. McGory et al. [14]
reported a statistically significant reduction in survival in patients
with colonic cancer and inadvertent splenic injury, with an increased
probability of death by 40% (p=0.001). We were unable to reproduce
a similar statistically significant relationship, between inadvertent
splenic injury and survival, however we observed a similar trend.
Our rate of inadvertent splenic injury is comparable at 6.6%, with no
injuries observed in the laparoscopic group (p=0.05). It postulated
the reduced rate of inadvertent splenic injuries in this group is due
to a combination of factors including: improved views, using angled
scopes and high definition optics, less likelihood of injury due to
reduced tissue traction during laparoscopic dissection and less
advanced tumours.
In keeping with previously published data on colectomy [15],
we observed a statistically significant shorter length of stay in the
laparoscopic group compared to the open surgery. Laparoscopic
colorectal surgery is associated with a shorter length of stay, reduced
post-operative morbidity and reduced blood loss, with comparable
oncological outcomes to open surgery [16], thus making it an
acceptable and attractive mode of surgery. Our data concur with
a smaller study by Ceccarelli et al on laparoscopic splenic flexure
tumour resection, They had acceptable operating times, with a mean
of 183.6 minutes, mean blood loss of 98mls, mean lymph node
harvest of 9.2 nodes and an overall post-operative morbidity rate
of 13.3% [17]. Similar to our study, this group did not observe any
splenic injuries.
There are several important limitations to our study. Firstly,
the use of non-randomisation of patients leads to selection bias
which means the data should be interpreted with caution. Secondly,
differences in the follow up period between the two groups may lead
to survival bias, with the overall follow up period in the laparoscopic
group being too short to currently assess long term outcomes.
Conclusion
Our study adds to the growing evidence base advocating laparoscopic surgery as technically safe and feasible option in the operative management of splenic flexure tumours, with comparable oncological and clinical outcomes compared to open surgery.
References
- Nakagoe T, Sawa T, Tsuji T, Jibiki M, Nanashima A, Yamaguchi H, et al. Carcinoma of the splenic flexure: multivariate analysis of predictive factors for clinicopathological characteristics and outcome after surgery. J Gastroenterol. 2000; 35: 528-5350.
- Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, et al. Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol. 2005; 6: 477-484.
- Hazebroek EJ, Color Study G. COLOR: a randomized clinical trial comparing laparoscopic and open resection for colon cancer. Surg Endosc. 2002; 16: 949-953.
- Steffen C, Bokey EL, Chapuis PH. Carcinoma of the splenic flexure. Dis Colon Rectum. 1987; 30: 872-874.
- Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM, et al. Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre randomised controlled trial. Lancet. 2005; 365: 1718-1726.
- Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, et al. Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol. 2005; 6: 477-484.
- Griffiths JD. Surgical anatomy of the blood supply of the distal colon. Ann R Coll Surg Engl. 1956; 19: 241-256.
- Aldridge MC, Phillips RK, Hittinger R, Fry JS, Fielding LP. Influence of tumour site on presentation, management and subsequent outcome in large bowel cancer. Br J Surg. 1986; 73: 663-670.
- Levien DH, Gibbons S, Begos D, Byrne DW. Survival after resection of carcinoma of the splenic flexure. Dis Colon Rectum. 1991; 34: 401-403.
- Nakagoe T, Sawai T, Tsuji T, Jibiki M, Ohbatake M, Nanashima A. Surgical treatment and subsequent outcome of patients with carcinoma of the splenic flexure. Surg Today. 2001; 31: 204-209.
- Kim HJ, Lee IK, Lee YS, Kang WK, Park JK, Oh ST, et al. A comparative study on the short-term clinicopathologic outcomes of laparoscopic surgery versus conventional open surgery for transverse colon cancer. Surg Endosc. 2009; 23: 1812-1817.
- Schlachta CM, Mamazza J, Poulin EC. Are transverse colon cancers suitable for laparoscopic resection? Surg Endosc. 2007; 21: 396-399.
- Benedix F, Schmidt U, Mroczkowski P, Gastinger I, Lippert H, Kube R, et al. Colon carcinoma--classification into right and left sided cancer or according to colonic subsite?--Analysis of 29,568 patients. Eur J Surg Oncol. 2011; 37: 134-139.
- McGory ML, Zingmond DS, Sekeris E, Ko CY. The significance of inadvertent splenectomy during colorectal cancer resection. Arch Surg. 2007; 142: 668-674.
- Eisenberg DP, Wey J, Bao PQ, Saul M, Watson AR, Schraut WH, et al. Short- and long-term costs of laparoscopic colectomy are significantly less than open colectomy. Surg Endosc. 2010; 24: 2128-2134.
- Buunen M, Veldkamp R, Påhlman L, Cuesta MA, Msika S, Morino M, et al. Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol. 2009; 10: 44-52.
- Ceccarelli G, Biancafarina A, Patriti A, Spaziani A, Bartoli A, Bellochi R, et al. Laparoscopic resection with intracorporeal anastomosis for colon carcinoma located in the splenic flexure. Surg Endosc. 2010; 24: 1784-1788.