Editorial
Understanding the Anterior Leaflet of the Mitral Valve
Paterson SH*
University of Sydney Faculty of Medicine, Australia
*Corresponding author: Hugh S. Paterson, University of Sydney Faculty of Medicine, Australia
Published: 09 Jul, 2016
Cite this article as: Paterson SH. Understanding the Anterior Leaflet of the Mitral Valve. Clin Surg. 2016; 1: 1061.
Editorial
Since the first prosthetic valve became commercially available in 1961, debate has continued over
the best way to manage the dysfunctional native mitral valve. Transcatheter Mitral Valve Insertions
(TMVI) have introduced new controversies which can be better understood by reviewing the old.
In 1991, Waggoner et al. [1] published the outcomes of 7 patients who underwent bioprosthetic
mitral valve insertion over a 5 year period, without resection or any modification of the anterior
leaflet of the mitral valve (AML) and who had post valve insertion echocardiography. Six of the
seven patients died within 2 months of surgery and a retrospective review of the post operative
echocardiography showed left ventricular outflow tract obstruction in all 7 patients. Since then,
there have been very few reports of full retention of the mitral valve at the time of open heart
bioprosthetic valve insertion, but full retention is now a requirement for the catheter deployed mitral
prostheses. Therefore, it is necessary to look at the rationale for performing the procedures reported
by Waggoner et al and understand why the outcomes were so poor, particularly after Cooley et al.
[2] had reported successful outcomes with mechanical valve insertion.
Anterior Mitral Leaflet Function
The rationale for retention of the native mitral valve at the time of prosthetic valve insertion is based on the physiological function of the AML. The anterior leaflet contributes to Left Ventricular
(LV) function by reducing LV work and improving efficiency. It has long been known that the
retention of the annulo-papillary connection through the posterior leaflet [3,4] improves outcomes
for patients undergoing mitral valve replacement for mitral incompetence and that the clinical
extent of this benefit is inversely related to pre-operative left ventricular function. However, AML
support of LV function is greater than that of the posterior leaflet [5] for the following reasons.
Intraventricular baffle
Magnetic Resonance Imaging (MRI) for assessment of blood flow velocities through the
ventricle during diastole has shown that the AML acts as a mid ventricular baffle which provides
laminar blood flow characteristics [6]. Following excision of the AML associated with mitral
mechanical valve insertion, MRI shows turbulence and stasis of blood within the ventricle during
diastole (Figure 1). With the AML baffle, blood flows through the inlet part of the ventricle, around
the apex towards the outflow tract, and this flow is maintained throughout diastole such that systole
provides acceleration of that diastolic flow. Without the AML baffle, greater LV work is required to
re-initiate blood flow from a situation of turbulence and stasis.
AML/papillary muscle apparatus
The mitral valve closes immediately after the onset of systole. The mitral leaflets move from
their diastolic intraventricular positions to the plane of the mitral annulus pulling the papillary
muscles and left ventricular wall towards the mitral and aortic valves (Figure 2). This dynamic action
“turbo-charges” the LV. A diastolic passive action of annulo-papillary continuity prevents excessive
LV dilatation which can be achieved with the posterior leaflet connection alone. The height of
the AML (distance from annulus to free edge chordal attachments) is considerably greater than
that of the posterior leaflet. This has 2 important implications. (a) The excursion of the papillary
muscle movement due to AML support is substantially greater and the turbo-charging effect
is proportionally greater [5]. (b) Fixing the free edge of the AML to the annulus will impair the
diastolic excursion of the papillary muscles away from the mitral annulus, with impaired diastolic
filling of the LV.
Accordingly, the rationale for maintenance of the AML at the time of mitral prosthetic insertion
is the improved ventricular function due to both turbo-charging and
baffle effects. It is of note that the Washington University experience
was with selected patients with poor LV function, on anti-failure
therapy and most with ischaemic mitral incompetence. These
patients are considered to be at high risk with conventional valve
surgery and are the ones to derive greatest benefit from preservation
of LV function by any means possible. It is inappropriate to attribute
poor outcomes of conventional mitral valve replacement to an acute
increase in after load when it is known that the method of mitral
replacement impairs LV function.
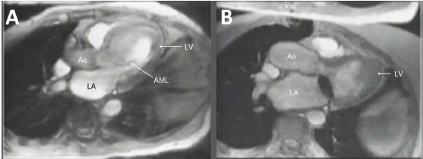
Figure 1
Figure 1
MRIs showing blood flow into the ventricle during early diastole.
A: Normal flow in an adult, showing the AML directing flow posteriorly, away
from the interventricular septum and around the apex. This is followed by
continuing flow towards the outflow tract up to the onset of systole. B: Flow
through a bileaflet mechanical prosthetic valve, showing flow into all parts of
the ventricle towards the apex. This is flowed by turbulence and stasis within
the ventricle. (With permission from Professor Joachim Laas, Bad Bevensen,
Germany).
AML: Anterior Mitral Leaflet; Ao: Aorta; LA: Left Atrium; LV: Left Ventricle
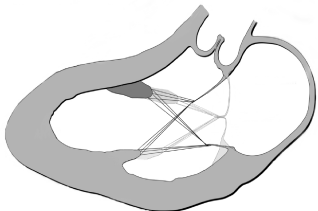
Figure 2
Figure 2
Schematic diagram showing movement of the papillary muscles
towards the mitral annulus with mitral closure. The mitral orifice constricts
and the annulus moves slightly into the ventricle.
The Causes of LV Outflow Tract Obstruction (LVOTO)
As the LVOTO is due to Systolic Anterior Motion (SAM) of the AML (Figure 3), it would be intuitive to use a small mitral bioprosthesis rather than a large one that would likely position the base of the AML closer to the outflow tract. However, the use of a small bioprosthesis appeared to increase the risk of LVOTO in a sheep model reported in 2011 [7]. Although this study was underpowered to achieve significance for the various risk factors, it did demonstrate that reducing the antero-posterior (A-P) diameter of the prosthesis by cinching the prosthesis abolished LVOTO when present, thus confirming the intuitive desire to keep the base of the AML away from the outflow tract. However, small bioprosthesis have short distances between stent posts and this was the likely reason for a trend towards a higher risk of LVOTO with smaller prostheses. The distance between the stent posts should exceed the width of the AML to allow the AML to move freely away from the outflow tract at the onset of systole. All the benefit of the smaller A-P diameter in a small valve is lost by having a stent posts under each side of the AML. Therefore, a bioprosthesis with a large anterior leaflet (wide anterior stent posts) would need to be inserted with the stent posts at the native commissures. The A-P diameter of the valve annulus should be reduced (elliptical shape) and the valve leaflets should be asymmetrical with a large leaflet anteriorly and 2 small equal sized leaflets posteriorly. This design was registered with the US patent office in 2011 by Alain Carpentier and Edwards Life Sciences (Patent no. US 8,034,104 B2). It has not been produced commercially due to the limited knowledge regarding the extent of benefit of AML retention. Accepting a documented hazard of LVOTO for the unproven benefit of AML retention would have little commercial appeal.
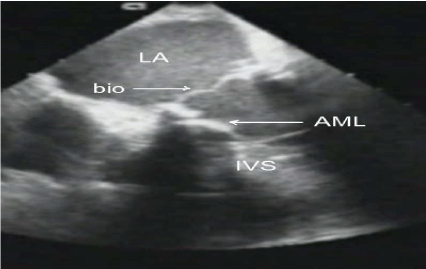
Figure 3
Figure 3
Left ventricular outflow tract obstruction due to systolic anterior
motion of the anterior mitral leaflet (AML) following insertion of a mitral
bioprosthetic valve (bio). The AML is seen abutting the interventricular
septum (IVS) while the bioprosthetic valve is closed during systole.
AML Management with Trans-catheter Mitral Valve Implantation (TMVI)
There are 2 principle methods of AML management at the time of
TMVI, based on the design of the prostheses used.
1. AML entrapment by the prosthetic stent apparatus provides
fixation of the device on the ventricular side and avoids the hazard
of LVOTO. As stated above, reefing the AML at the level of the
mitral annulus will inhibit diastolic filling of the LV. The first human
implant of such a device was in an 86 year old man with severe LV
dysfunction and severe mitral incompetence. The implantation was
successful with minimal residual mitral incompetence but the patient
died 3 days later from multi-organ failure. It is likely that the valve
had an adverse effect on LV function and this may have simply been
due to immobilization of the AML and restriction of diastolic filling.
No devices that use AML entrapment have yet achieved desirable
clinical outcomes in human trials [8]. Use of these devices in humans
is usually based on compassionate grounds where no other form of
therapy can be reasonably offered and the patients’ estimated survival
without treatment is poor. These patients have poor LV function
and are sensitive to interventions with any adverse effect on LV
function. These valves are unlikely be trialed in patients with good
LV function, who might easily tolerate relatively minor disturbances
in LV function. Indeed, many animal studies have been performed
to confirm the function of these valves when implanted into normal
animal hearts.
Valves that capture only the portions of the AML adjacent to
the commissures, along with fixation to the posterior leaflet may
achieve the benefit of retention of the baffle effect of the AML without
diastolic restriction. The restriction of the para-commissural parts of
the AML may be sufficient to prevent SAM.
2. LV apical tethering of the valve prosthesis effectively fixes
the valve on the ventricular side. As with prostheses that use AML
entrapment, fixation on the atrial side is achieved with a flange.
Apical tethering does not involve attachment to the anterior leaflet
but the nitinol stent supporting the valve extends into the LV cavity
and restricts AML motion. The AML cannot reach the plane of the
mitral annulus during systole and so the turbo-charge effect is largely
lost but the baffle effect is maintained and diastolic LV filling is not
restricted. There is a risk of LVOTO which makes accurate sizing
of the valve very important. Undersizing the valve will likely result
in a paravalvular leak and oversizing increases the risk of LVOTO
by the AML due to SAM. If LVOTO is recognized before the apical
tethering fixation is completed, the prosthesis can be easily retrieved
or repositioned. There are options for management of LVOTO
after completion of the implantation. Stenting of the LVOT can
substantially reduce the gradient [9]. In the sheep model of LVOTO
following open heart implantation of bioprosthesis, volume loading
tended to increase the SAM of the AML which is the opposite of that
seen following mitral valve repair. Where volume loading after repair
increases the cross-sectional area of the LVOT and reduces SAM, it
appears that the valve prosthesis causes a relatively fixed cross sectional
area of the outflow tract so that volume loading simply increases the
cardiac output and blood velocity through the outflow tract, thereby
increasing the risk of SAM. Accordingly, it may be better to reduce
cardiac output with ventricular pacing and or beta blocker therapy.
Urgent alcohol septal ablation has been performed with immediate
resolution of the SAM [10]. This was due to the immediate paralysis
of the sub-aortic septum with onset of paradoxical motion. So far,
the device that uses apical tethering has been the most successful in
human use, presumably due to the preservation of LV function in
patients who are poor candidates for any other form of therapy.
These important advances cannot be achieved without information
from both human and animal experiences. Unfortunately, a lot of
information exists in the industry sector, which is not available to the
broader community. When it is considered that a company with a
single device not yet tested in humans can be worth US$450M, the
risks of industrial espionage are considerable. Even the information
gained within various industry sectors is piecemeal and not shared.
Many theories might be proven incorrect as more information is
gained. There is still much to learn with plenty of room for new ideas.
References
- Waggoner AD, Pérez JE, Barzilai B, Rosenbloom M, Eaton MH, Cox JL. Left ventricular outflow obstruction resulting from insertion of mitral prostheses leaving the native leaflets intact: adverse clinical outcome in seven patients. Am Heart J. 1991; 122: 483-488.
- Cooley DA, Ingram MT. Intravalvular implantation of mitral valve prostheses. Tex Heart Inst J. 1987; 14: 188-193.
- Lillehei CW, Levy MJ, Bonnabeau RC Jr. Mitral valve replacement with preservation of papillary muscles and chordae tendineae. J Thorac Cardiovasc Surg. 1964; 47: 532-543.
- David TE, Ho WC. The effect of preservation of chordae tendineae on mitral valve replacement for postinfarction mitral regurgitation. Circulation. 1986; 74: I116-120.
- Hansen DE, Cahill PD, Derby GC, Miller DC. Relative contributions of the anterior and posterior mitral chordae tendineae to canine global left ventricular systolic function. J Thorac Cardiovasc Surg. 1987; 93: 45-55.
- Kim WY, Walker PG, Pedersen EM, Poulsen JK, Oyre S, Houlind K, et al. Left ventricular blood flow patterns in normal subjects: a quantitative analysis by three-dimensional magnetic resonance velocity mapping. J Am Coll Cardiol. 1995; 26: 224-238.
- Paterson HS, Seitz MJ, Symes MJ, See V, Lu J, Byth K, et al. Bioprosthetic valve modification for full retention of the native mitral valve. Chirurgia. 2011; 24: 263-266.
- De Backer O, Piazza N, Banai S, Lutter G, Maisano F, Herrmann HC, et al. Percutaneous transcatheter mitral valve replacement: an overview of devices in preclinical and early clinical evaluation. Circ Cardiovasc Interv. 2014; 7: 400-409.
- Moat N, Duncan A, Lindsay A, Quarto C, Blanke P, Leipsic J, et al. Transcatheter mitral valve replacement for the treatment of mitral regurgitation: in-hospital outcomes of an apically tethered device. J Am Coll Cardiol. 2015; 65: 2352-2353.
- Deharo P, Urena M, Himbert D, Brochet E, Rouleau F, Pinaud F, et al. Bail-Out Alcohol Septal Ablation for Left Ventricular Outflow Tract Obstruction After Transcatheter Mitral Valve Replacement. JACC Cardiovasc Interv. 2016; 9: e73-76.