Case Report
Brisk Bleeding during Deployment of the Angio-Seal Vascular Closure Device: What the User Manual Doesn't Tell You
Rasuli P*, Jaganathan S, French JG and Hammond DI
Department of Radiology, the Ottawa Hospital, University of Ottawa, Canada
*Corresponding author: Pasteur Rasuli, Department of Radiology, the Ottawa Hospital, 501 Smyth Road Ottawa ON, K1J 8N5, Canada
Published: 11 Jul, 2016
Cite this article as: Rasuli P, Jaganathan S, French JG, Hammond DI. Brisk Bleeding during Deployment of the Angio-Seal Vascular Closure Device: What the User Manual Doesn't Tell You. Clin Surg. 2016; 1: 1058.
Abstract
Brisk puncture site bleeding during deployment and application of traction to the Angio-Seal footplate indicates that the foot plate is not anchored correctly against the arterial wall. In this situation, the collagen pack should not be deployed. A more vigorous pull should be applied to disengage the mal-positioned footplate, and to bring it to the arteriotomy site. Once the bleeding stops, the collagen plug can be deployed safely. Deploying the collagen plug before the bleeding stops can deliver the plug into the vessel lumen, resulting in arterial thrombosis. We review four patients in our practice that experienced this event.
Introduction
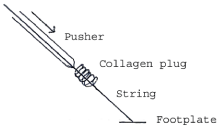
Vascular access closure devices are commonly used to achieve hemostasis following femoral arterial punctures, and to facilitate early ambulation of patients after angiography. The Angio-Seal Vascular Closure Device (St Jude Medical, St Paul, MN) is a widely used such device. It consists (Figure 1) of a footplate or anchor attached to a string that is loaded with a collagen plug. The foot plate is placed inside the artery and pulled by the string against the arterial wall to occlude the arteriotomy site. The collagen plug is then packed by a pusher catheter immediately outside the artery to seal the puncture site and bring about hemostasis. The string is then cut to release the device. The footplate, collagen plug and string are all bio-absorbable. Several authors [1-3] have reported incidents where collagen plugs have been found within the vessel lumen after deployment, leading to lower limb ischemia. The Manufacturer and User Facility Device Experience (MAUDE) database shows over 500 of such incidents. In our practice there were 4 patients in over a 6 year period in whom lower limb ischemia or numbness occurred within several hours after deployment of the 6F STS plus version of Angio-Seal, three of whom required surgical intervention to remove the collagen plug lodged inside the artery. Reports on how this event can be avoided are lacking. The purpose of our report is to elucidate the mechanisms leading to intra-arterial placement of the collagen plug, and steps that can be taken to prevent it. Once aware of this, we were able to avert the complication in a fifth patient. Our institution does not require Research Ethics approval for retrospective case reports.
Case Presentation
Case 1
A 64 year old man presented with a chronically infected wound site following left tarsometatarsal
amputation. Because of increasing ischemia and necrosis, he was referred for possible
percutaneous revascularization. The procedure was performed from a right common femoral
arterial approach. Self-expanding metallic stents were noted in the right common iliac artery and
bilateral distal external iliac arteries. Angioplasty of the distal left superficial femoral artery, tibioperoneal
trunk, proximal peroneal artery and anterior tibial artery were performed. At the end of
the procedure, a 6 F Angio-Seal device was deployed, following which there was brisk bleeding from
the puncture site. This was attributed to device failure, and manual compression was applied for 10
minutes to obtain hemostasis. Three hours later the patient developed features of acute right lower
limb ischemia, for which a MDCT was done, revealing a short segment of occlusion immediately
distal to the external iliac stent and reconstitution of flow in the common femoral artery through the
collaterals (Figure 2). This was suspected to be due to the collagen plug of the Angio-Seal, and the
patient was transferred to the operating room. At surgery the Angio-Seal device was found lodged
at the distal end of the external iliac artery stent. Following removal
of the device there good arterial flow was restored.
Case 2
A 72 year old man with a past history of left external iliac artery
stenting presented with painful left buttock claudication. Via a Left
common femoral arterial approach, angioplasty of the left external
iliac artery and stenting of the left common iliac – proximal external
iliac artery were performed. At the end of the procedure, 6 F AngioSeal
was deployed, following which the patient had significant brisk
bleeding at the puncture site. Hemostasis was achieved by 15 minutes
of manual compression. Four hours later the patient developed left
lower limb ischemia and he was operated upon. The Angio-Seal was
found inside the proximal common femoral artery and there was
complete occlusion of distal external iliac artery. Several atheromatous
plaques were seen in both vessels, for which endarterectomy was
performed. Good arterial flow was obtained following device removal
and endarterectomy.
Case 3
A 58 year old woman presented with claudication of the right
leg. An MDCT revealed a severe stenosis in the right distal superficial
femoral artery for which the patient underwent a successful angioplasty
from an antegrade right femoral approach. Following the deployment
of the footplate of a 6F Angio-Seal severe bleeding was encountered
which did not stop after deployment of the collagen plug. Manual
groin compression was applied for 15 minutes and hemostasis was
obtained. Shortly after the deployment of Angio-Seal the patient
developed discoloration right foot and this was attributed to vascular
spasm. But symptoms worsened over the following two hours and she
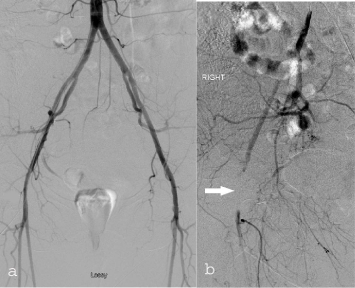
complained of numbness in her foot. An angiogram from the contra
lateral femoral artery showed occlusion of the right femoral artery
which was not present on a diagnostic arteriogram 2 months earlier
(Figure 3A and B). This necessitated surgical exploration disclosing
the collagen plug within the common femoral arterial lumen. After
removal of the plug and thrombectomy the circulation in the right leg
improved and the ischemia resolved.
Case 4
A 45 year old woman presented with cervical bleeding due to
cancer of cervix. Urgent embolization of the anterior trunk of both
internal iliac arteries with Gelfoam torpedoes was performed from
a right femoral approach. A 6 F Angio-Seal was used for hemostasis.
The footplate was deployed, stopping bleeding at the puncture
site. However the patient was severely cachectic and lacking in
subcutaneous fat, such that when the collagen plug was packed
under the skin, it was inadvertently pushed intravascularly. A brisk
non-pulsatile hemorrhage ensued which was controlled by manual
compression. Several hours later, the patient complained of numbness
of the right foot, and MDCT confirmed isolated right common
femoral artery occlusion. Since the symptoms were relatively mild
and the patient’s life expectancy was limited, the attending physician
decided to treat this conservatively.
Case 5
A 75 year old woman presented with severe left lower limb
claudication. After a diagnostic arteriogram via left femoral artery
access, left common iliac artery angioplasty and stenting were
performed. Post procedure, a 6F Angio-Seal was deployed in the
left common femoral artery. Brisk puncture site bleeding was noted
post traction, but prior to packing of the collagen plug. We exposed
the left foot and found it to be cold and discolored. Because of our
earlier experiences we suspected this was the result of inadvertent
entrapment of the footplate by a plaque, causing the obstruction of
the vessel lumen. As the string had not yet been cut, we were able to
pull back the footplate more forcibly, stopping the hemorrhage and
confirming that the foot plate was now in correct position against the
arterial wall. The collagen plug was then deployed and packed. Foot
color returned to normal promptly.
Figure 1
Figure 1
Schematic simplified drawing of Angio-Seal show three main
components of the device: A footplate or anchor attached to a string that
contains a self-tightening suture and is loaded with a collagen sponge and a
pusher to pack the collagen plug outside the vessel wall.
Figure 2
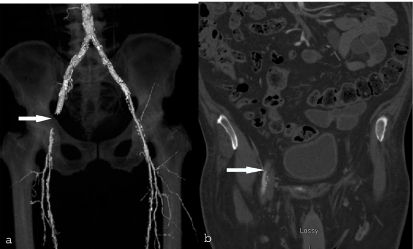
Figure 2
64-year-old with left leg claudication. MDCT obtained 4 hours
post Angio-Seal deployment. (A) Three -dimensional reconstruction shows
thrombus in the distal right external iliac artery (arrow) Note the stent proximal
to the thrombosed segment. (B) Coronal reconstruction shows reconstitution
of the common femoral artery distal to the thrombosed external iliac artery
(arrow).
Figure 3A and B
Figure 3A and B
Technique of repair: the previous anastomosis between the
composite graft and the hemi-arch protheses is open during a short period
of circulatory arrest. A. Then the distal graft is controlled and clamped and
cardiopulmonary bypass restarted. B. Thereafter, the pseudoaneurysm is
fixed from inside the composite graft. C.
Figure 4
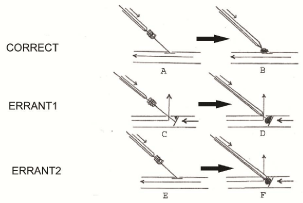
Figure 4
Schematic drawing of correct deployment on Angio-Seal depicted
in 4A and 4B where the foot plate is against the arterial wall at the arteriotomy
site and the collagen plug is deployed while traction is applied to the thread.
There is no bleeding in either phase of the deployment. Errant deployment
type 1 shown in Figure 4C and 4D occurs when the footplate is caught on
an intravascular obstacle and the collagen pack is delivered intravascularly
while traction is applied to the thread. There is bleeding in both phases of
this form of deployment as depicted by vertical arrows in Figure 4C and
4D. Errant deployment type 2 shown in Figure 4E and 4F occurs when the
footplate is pushed intravascularly by the pusher catheter and the collagen
pack is delivered intravascularly due to poor traction applied to the thread.
There is bleeding only on the second phase of this form of deployment as
depicted by vertical arrow in Figure 4F but not in the first phase Figure 4E.
Discussion
When the Angio-Seal device is deployed correctly, a mechanical
seal is created between the anchored footplate on the intimal surface
and the collagen plug on the adventitial surface of the artery (Figure
4A and B), securing hemostasis. If the footplate is not positioned
correctly, the collagen plug can be injected inadvertently into the
vessel lumen.
Dregelid et al. [2] reported that it was not advisable to use an
Angio-Seal if the superficial femoral artery was punctured, as this
could result in intraluminal lodging of the device. However they did
not elaborate upon its mechanism or how this complication might be
anticipated or steps that can be taken to prevent it.
We propose that there are two general situations leading to
vessel occlusion from the mal-positioned closure device. The first
mechanism is deployment of the Angio-Seal in the presence of an
intra-arterial narrowing due to a nearby arterial division, stenotic
plaque, metallic stent, or simple arterial spasm. Each of these
situations can singly or in common, lead to errant lodging of the foot
plate, and subsequent intraluminal lodging of the collagen plug.
With the footplate caught somewhere other than the arteriotomy
site, the arteriotomy access will remain open as shown in (Figure 4C),
resulting in non pulsatile back-bleeding from the artery distal to the
arteriotomy site. Many interventional radiologists would intuitively
rush to deploy the collagen pack to stop the bleeding, and would then
cut the device string. However in doing so they will in fact deploy the
collagen plug inside the vessel as shown in (Figure 4D). Since the intra-
arterial plug does not close the arteriotomy site the back-bleeding
will continue and would require several minutes of manual pressure
until the bleeding stops. The partial thrombosis will then progress to a
complete thrombosis over the following few hours, causing ischemic
symptoms similar to those that occurred in our first three patients.
A second mechanism which could lead to intra-arterial lodging of
the Angio-Seal plug when the interventional radiologist does not hold
adequate traction on the string during the packing of the collagen. This
permits the footplate to migrate further in the vessel under pressure
from the pusher catheter and the collagen enters the lumen during
the packing stage (Figure 4E and F). This condition, which was seen
in our case 4 and a few other cases reported in the literature [5] occurs
mainly in patients with no atherosclerotic plaques or in situ stents
and in patients with common femoral artery punctures. It differs
from Errant deployment type 1 in that there is no bleeding at the time
of the footplate traction against the arteriotomy site, but rather the
bleeding commences immediately after packing the collagen. Many
of the patients in the latter group may be asymptomatic or mildly
symptomatic for several days to weeks because blood flows around
the plug and the incomplete occlusion. It appears that over time
fibrotic reaction to the existing intraluminal collagen could results in
a complete occlusion or the partial degradation of the collagen plug
may lead to symptoms arising from distal embolization of the parts of
the plug down into the popliteal artery and runoff vessels [4-6].
If the footplate is pulled correctly against the arteriotomy site
there should be no bleeding. It follows that if there is a brisk bleeding
following deployment of the footplate this indicates that the foot
plate is not against the arterial wall (type 1 errant deployment), and
therefore the collagen pack should not be deployed. More vigorous
traction should be applied to the string attached to the footplate in
order to disengage it from the plaque and to bring it to the arteriotomy
site. This maneuver should cause the bleeding to stop as in our patient
described in case 5. The collagen plug can then be safely deployed. If
the bleeding cannot be stopped with the application of due force to
the string, the collagen plug should not be deployed and hemostasis
should be obtained by manual compression. If there are no distal
ischemic symptoms then the string could be cut subcutaneously.
The string should be left accessible to allow easier extraction of the
footplate intraoperatively should the patient subsequently develop
symptoms of ischemia in the affected limb. If there are no ischemic
symptoms in the foot then the string could be subcutaneously cut. It
is logical to cut the string subcutaneously only after confirmation of a
palpable foot pulse or adequate perfusion to the affected foot. Likewise
it is important to keep the traction taught during light packing of the
collagen plug to avoid Type 2 errant deployment.
Conclusion
We would like to stress on the importance of obtaining complete hemostasis before packing the Collagen plug with Angio-Seal to avoid complications. Brisk bleeding following deployment and traction of the Angio-Seal footplate should be given due significance and if needed the footplate has to be pulled harder so that it opposes the arteriotomy site with resultant decrease or stop in the bleeding before packing the collagen plug.
References
- Wille J, Vos JA, Overtoom TT, Suttorp MJ, van de Pavoordt ED, de Vries JP. Acute leg ischemia: the dark side of a percutaneous femoral artery closure device. Ann Vasc Surg. 2006; 2: 278–281.
- Dregelid E, Jensen G, Daryapeyma A. Complications associated with the Angio-Seal arterial puncture closing device: Intra-arterial deployment and occlusion by dissected plaque. Journal of Vascular Surgery. 2006; 44: 1357–1359.
- Cikirikcioglu M, Cherian S, Keil V, Manzano N, Gemayel G, Theologou T, et al. Surgical treatment of complications associated with the Angio-Seal vascular closure device. Ann Vasc Surg. 2011; 25: 557.
- Corley JA, Kasliwal MK, Tan LA, Lopes DK. Delayed Vascular Claudication Following Diagnostic Cerebral Angiography: A Rare Complication of the AngioSeal Arteriotomy Closure Device. J Cerebrovasc Endovasc Neurosurg. 2014; 16: 275-280.
- Chihara S, Matsuo H, Takagi K, Arai S, Morimatsu M. A foot ulcer caused by the use of an angio-seal arterial closure device after percutaneous transluminal angioplasty: a case report. Ann Vasc Dis. 2012; 5: 65-68.
- Ainslie MP, Macdonald J, Smyth J. A pain in the leg following angiography. J Invasive Cardiol. 2011; 23: E58-E60.